Anti-neutrophil cytoplasmic antibody

Anti-neutrophil cytoplasmic antibodies (ANCAs) are a group of
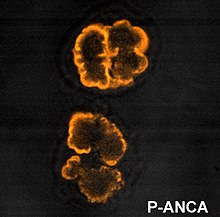
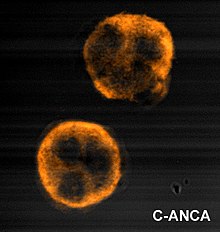
ANCA IF patterns
Immunofluorescence (IF) on ethanol-fixed neutrophils is used to detect ANCA, although formalin-fixed neutrophils may be used to help differentiate ANCA patterns. ANCA can be divided into four patterns when visualised by IF; cytoplasmic ANCA (c-ANCA), C-ANCA (atypical), perinuclear ANCA (p-ANCA) and atypical ANCA (a-ANCA), also known as x-ANCA. c-ANCA shows cytoplasmic granular fluorescence with central interlobular accentuation. C-ANCA (atypical) shows cytoplasmic staining that is usually uniform and has no interlobular accentuation. p-ANCA has three subtypes, classical p-ANCA, p-ANCA without nuclear extension and granulocyte specific-antinuclear antibody (GS-ANA). Classical p-ANCA shows perinuclear staining with nuclear extension, p-ANCA without nuclear extension has perinuclear staining without nuclear extension and GS-ANA shows nuclear staining on granulocytes only. a-ANCA often shows combinations of both cytoplasmic and perinuclear staining.[1]
ANCA antigens
The c-ANCA antigen is specifically
Other less common antigens include
ELISA
Development
It is poorly understood how ANCA are developed, although several hypotheses have been suggested. There is probably a genetic contribution, particularly in genes controlling the level of immune response – although genetic susceptibility is likely to be linked to an environmental factor, some possible factors including vaccination or exposure to silicates. Two possible mechanisms of ANCA development are postulated, although neither of these theories answers the question of how the different ANCA specificities are developed, and there is much research still being undertaken on the development of ANCA.[3]
Theory of molecular mimicry
Microbial
Theory of defective apoptosis
Neutrophil apoptosis, or programmed cell death, is vital in controlling the duration of the early inflammatory response, thus restricting damage to tissues by the neutrophils. ANCA may be developed either via ineffective apoptosis or ineffective removal of apoptotic cell fragments, leading to the exposure of the immune system to molecules normally sequestered inside the cells. This theory solves the paradox of how it could be possible for antibodies to be raised against the intracellular antigenic targets of ANCA.[3]
Role in disease
Disease associations
ANCAs are associated with small vessel vasculitides including granulomatosis with polyangiitis, microscopic polyangiitis, primary pauci-immune necrotizing crescentic glomerulonephritis (a type of renal-limited microscopic polyangiitis), eosinophilic granulomatosis with polyangiitis and drug induced vasculitides. ANCA-associated vasculitides (AAV) have new classification criteria, updated in 2022.[4][5] PR3 directed c-ANCA is present in 80-90% of granulomatosis with polyangiitis, 20-40% of microscopic polyangiitis, 20-40% of pauci-immune crescentic glomerulonephritis and 35% of eosinophilic granulomatosis with polyangiitis. c-ANCA (atypical) is present in 80% of cystic fibrosis (with BPI as the target antigen) and also in inflammatory bowel disease, primary sclerosing cholangitis and rheumatoid arthritis (with antibodies to multiple antigenic targets). p-ANCA with MPO specificity is found in 50% of microscopic polyangiitis, 50% of primary pauci-immune necrotizing crescentic glomerulonephritis and 35% of eosinophilic granulomatosis with polyangiitis. p-ANCA with specificity to other antigens are associated with inflammatory bowel disease, rheumatoid arthritis, drug-induced vasculitis, autoimmune liver disease, drug induced syndromes and parasitic infections. Atypical ANCA is associated with drug-induced systemic vasculitis, inflammatory bowel disease and rheumatoid arthritis.[2][6] The ANCA‐positive rate is much higher in patients with type 1 diabetes mellitus than in healthy individuals.[7]
Levamisole, which is a common adulterant of cocaine, can cause an ANCA positive vasculitis.[8]
The presence or absence of ANCA cannot indicate presence or absence of disease and results are correlated with clinical features. The association of ANCA and disease activity remains controversial; however, the reappearance of ANCA after treatment can indicate a relapse.[9][10]
Pathogenesis
Although the pathogenic role of ANCA is still controversial, in vitro and animal models support the idea that the antibodies have a direct pathological role in the formation of small vessel vasculitides. MPO and PR3 specific ANCA can activate
Treatment
Avacopan was approved for medical use in the United States to treat anti-neutrophil cytoplasmic autoantibody-associated vasculitis in October 2021.[19]
History
ANCAs were originally described in Davies et al. in 1982 in segmental necrotising glomerulonephritis.[16][20] The Second International ANCA Workshop, held in The Netherlands in May 1989, fixed the nomenclature on perinuclear vs. cytoplasmic patterns, and the antigens MPO and PR3 were discovered in 1988 and 1989, respectively.[21] International ANCA Workshops have been carried out every two years.[citation needed]
References
- ^ ISBN 978-0-7044-8510-5.)
{{cite book}}: CS1 maint: multiple names: authors list (link - ^ S2CID 14521707.
- ^ PMID 14700590.
- PMID 35110333. Retrieved 27 September 2023.
- PMID 35110332.
- PMID 16339302.
- S2CID 201845957.
- PMID 22723468.
- S2CID 28849057.
- PMID 16265681.
- PMID 25578468.
- PMID 20395376.
- PMID 15210387.
- PMID 16624929.
- PMID 2161532.
- ^ S2CID 54474335.
- PMID 19565480.
- .
- ^ "ChemoCentryx Announces FDA Approval of Tavneos (avacopan) in ANCA-Associated Vasculitis". ChemoCentryx, Inc. (Press release). 8 October 2021. Archived from the original on 8 October 2021. Retrieved 11 October 2021.
- PMID 6297657.
- PMID 2189509.
External links
- images of pANCA and cANCA Archived 2012-09-27 at the Wayback Machine
- fluorescence images of ANCA Archived 2007-03-26 at the Wayback Machine
- Anti-Neutrophil+Cytoplasmic+Antibody at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
