Absorbed dose
| Absorbed dose of ionizing radiation | |
|---|---|
Common symbols | D |
Rad | |
| In SI base units | J⋅kg−1 |
Absorbed dose is a dose quantity which is the measure of the energy deposited in matter by ionizing radiation per unit mass. Absorbed dose is used in the calculation of dose uptake in living tissue in both radiation protection (reduction of harmful effects), and radiology (potential beneficial effects, for example in cancer treatment). It is also used to directly compare the effect of radiation on inanimate matter such as in radiation hardening.
The
Deterministic effects
Conventionally, in radiation protection, unmodified absorbed dose is only used for indicating the immediate health effects due to high levels of acute dose. These are tissue effects, such as in acute radiation syndrome, which are also known as deterministic effects. These are effects which are certain to happen in a short time.[citation needed] The time between exposure and vomiting may be used as a heuristic for quantifying a dose when more precise means of testing are unavailable. [2]
Effects of acute radiation exposure
| Phase | Symptom | Whole-body absorbed dose (Gy) | ||||
|---|---|---|---|---|---|---|
| 1–2 Gy | 2–6 Gy | 6–8 Gy | 8–30 Gy | > 30 Gy | ||
| Immediate | Nausea and vomiting | 5–50% | 50–100% | 75–100% | 90–100% | 100% |
| Time of onset | 2–6 h | 1–2 h | 10–60 min | < 10 min | Minutes | |
| Duration | < 24 h | 24–48 h | < 48 h | < 48 h | — (patients die in < 48 h) | |
| Diarrhea | None | None to mild (< 10%) | Heavy (> 10%) | Heavy (> 95%) | Heavy (100%) | |
| Time of onset | — | 3–8 h | 1–3 h | < 1 h | < 1 h | |
| Headache | Slight | Mild to moderate (50%) | Moderate (80%) | Severe (80–90%) | Severe (100%) | |
| Time of onset | — | 4–24 h | 3–4 h | 1–2 h | < 1 h | |
| Fever | None | Moderate increase (10–100%) | Moderate to severe (100%) | Severe (100%) | Severe (100%) | |
| Time of onset | — | 1–3 h | < 1 h | < 1 h | < 1 h | |
| CNS function | No impairment | Cognitive impairment 6–20 h | Cognitive impairment > 24 h | Rapid incapacitation | ||
Latent period |
28–31 days | 7–28 days | < 7 days | None | None | |
Illness |
Mild to moderate Fatigue
Weakness |
Moderate to severe | Severe Electrolyte disturbance
|
Nausea Vomiting Severe diarrhea High fever Electrolyte disturbance Shock |
— (patients die in < 48h) | |
| Mortality | Without care | 0–5% | 5–95% | 95–100% | 100% | 100% |
| With care | 0–5% | 5–50% | 50–100% | 99–100% | 100% | |
| Death | 6–8 weeks | 4–6 weeks | 2–4 weeks | 2 days – 2 weeks | 1–2 days | |
| Table source[3] | ||||||
Radiation therapy
The measurement of absorbed dose in tissue is of fundamental importance in radiobiology as it is the measure of the amount of energy the incident radiation is imparting to the target tissue.[citation needed]
Dose computation
The absorbed dose is equal to the radiation exposure (ions or C/kg) of the radiation beam multiplied by the ionization energy of the medium to be ionized.
For example, the ionization energy of dry air at 20 °C and 101.325 kPa of pressure is 33.97±0.05 J/C.[4] (33.97 eV per ion pair) Therefore, an exposure of 2.58×10−4 C/kg (1 roentgen) would deposit an absorbed dose of 8.76×10−3 J/kg (0.00876 Gy or 0.876 rad) in dry air at those conditions.
When the absorbed dose is not uniform, or when it is only applied to a portion of a body or object, an absorbed dose representative of the entire item can be calculated by taking a mass-weighted average of the absorbed doses at each point.
More precisely,[5]
Where
- is the mass-averaged absorbed dose of the entire item ;
- is the item of interest;
- is the absorbed dose as a function of location;
- is the density as a function of location;
- is volume.
Medical considerations
Non-uniform absorbed dose is common for soft radiations such as low energy x-rays or beta radiation. Self-shielding means that the absorbed dose will be higher in the tissues facing the source than deeper in the body.[citation needed]
The mass average can be important in evaluating the risks of radiotherapy treatments, since they are designed to target very specific volumes in the body, typically a tumour. For example, if 10% of a patient's bone marrow mass is irradiated with 10 Gy of radiation locally, then the absorbed dose in bone marrow overall would be 1 Gy. Bone marrow makes up 4% of the body mass, so the whole-body absorbed dose would be 0.04 Gy. The first figure (10 Gy) is indicative of the local effects on the tumour, while the second and third figure (1 Gy and 0.04 Gy) are better indicators of the overall health effects on the whole organism. Additional dosimetry calculations would have to be performed on these figures to arrive at a meaningful effective dose, which is needed to estimate the risk of cancer or other stochastic effects.
When ionizing radiation is used to treat cancer, the doctor will usually prescribe the
Stochastic risk - conversion to equivalent dose
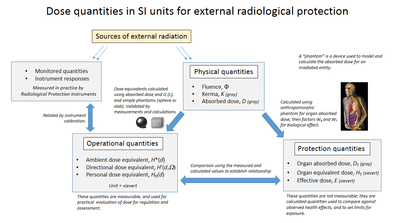
For stochastic radiation risk, defined as the probability of cancer induction and genetic effects occurring over a long time scale, consideration must be given to the type of radiation and the sensitivity of the irradiated tissues, which requires the use of modifying factors to produce a risk factor in sieverts. One sievert carries with it a 5.5% chance of eventually developing cancer based on the linear no-threshold model.[6][7] This calculation starts with the absorbed dose.
To represent stochastic risk the dose quantities
For whole body radiation, with
Development of the absorbed dose concept and the gray

Wilhelm Röntgen first discovered X-rays on November 8, 1895, and their use spread very quickly for medical diagnostics, particularly broken bones and embedded foreign objects where they were a revolutionary improvement over previous techniques.
Due to the wide use of X-rays and the growing realisation of the dangers of ionizing radiation, measurement standards became necessary for radiation intensity and various countries developed their own, but using differing definitions and methods. Eventually, in order to promote international standardisation, the first International Congress of Radiology (ICR) meeting in London in 1925, proposed a separate body to consider units of measure. This was called the International Commission on Radiation Units and Measurements, or ICRU,[a] and came into being at the Second ICR in Stockholm in 1928, under the chairmanship of Manne Siegbahn.[9][10][b]
One of the earliest techniques of measuring the intensity of X-rays was to measure their ionising effect in air by means of an air-filled
In 1940,
In the late 1950s, the CGPM invited the ICRU to join other scientific bodies to work on the development of the
Other uses
Absorbed dose is also used to manage the irradiation and measure the effects of ionising radiation on inanimate matter in a number of fields.
Component survivability
Absorbed dose is used to rate the survivability of devices such as electronic components in ionizing radiation environments.
Radiation hardening
The measurement of absorbed dose absorbed by inanimate matter is vital in the process of radiation hardening which improves the resistance of electronic devices to radiation effects.
Food irradiation
Absorbed dose is the physical dose quantity used to ensure
The following table shows radiation quantities in SI and non-SI units:
| Quantity | Unit | Symbol | Derivation | Year | SI equivalent |
|---|---|---|---|---|---|
| Activity (A) | becquerel | Bq | s−1 | 1974 | SI unit |
| curie | Ci | 3.7 × 1010 s−1 | 1953 | 3.7×1010 Bq | |
| rutherford | Rd | 106 s−1 | 1946 | 1,000,000 Bq | |
| Exposure (X) | coulomb per kilogram | C/kg | C⋅kg−1 of air | 1974 | SI unit |
| röntgen | R | esu / 0.001293 g of air | 1928 | 2.58 × 10−4 C/kg | |
| Absorbed dose (D) | gray | Gy | J⋅kg−1 | 1974 | SI unit |
| erg per gram | erg/g | erg⋅g−1 | 1950 | 1.0 × 10−4 Gy | |
rad
|
rad | 100 erg⋅g−1 | 1953 | 0.010 Gy | |
| Equivalent dose (H) | sievert | Sv | J⋅kg−1 × WR | 1977 | SI unit |
| röntgen equivalent man | rem | 100 erg⋅g−1 × WR | 1971 | 0.010 Sv | |
| Effective dose (E) | sievert | Sv | J⋅kg−1 × WR × WT | 1977 | SI unit |
| röntgen equivalent man | rem | 100 erg⋅g−1 × WR × WT | 1971 | 0.010 Sv |
Although the United States Nuclear Regulatory Commission permits the use of the units
See also
Notes
References
- ^ ICRP 2007, glossary.
- ^ "Radiation Exposure and Contamination - Injuries; Poisoning". Merck Manuals Professional Edition. Retrieved 2023-05-20.
- ^ "Radiation Exposure and Contamination - Injuries; Poisoning - Merck Manuals Professional Edition". Merck Manuals Professional Edition. Retrieved 2017-09-06.
- S2CID 250751778.
- ^ ICRP 2007, p. 1.
- ISBN 978-0-7020-3048-2. Retrieved 17 May 2012.
- ^ The ICRP says, "In the low dose range, below about 100 mSv, it is scientifically plausible to assume that the incidence of cancer or heritable effects will rise in direct proportion to an increase in the equivalent dose in the relevant organs and tissues." ICRP publication 103 paragraph 64
- ^ ICRP 2007, paragraphs 104 and 105.
- S2CID 74656044. Retrieved 2012-05-20.
- ^ "About ICRU - History". International Commission on Radiation Units & Measures. Retrieved 2012-05-20.
- ^ LCCN 60014734. Retrieved 2012-05-15.
- ISBN 0-521-22436-5. Retrieved 2012-05-15.
- ISBN 978-3-642-00737-8. Retrieved 2012-05-14.
- ^ "CCU: Consultative Committee for Units". International Bureau of Weights and Measures (BIPM). Retrieved 2012-05-18.
- ^ 10 CFR 20.1004. US Nuclear Regulatory Commission. 2009.
- ^ The Council of the European Communities (1979-12-21). "Council Directive 80/181/EEC of 20 December 1979 on the approximation of the laws of the Member States relating to Unit of measurement and on the repeal of Directive 71/354/EEC". Retrieved 19 May 2012.
Literature
- ICRP (2007). "The 2007 Recommendations of the International Commission on Radiological Protection". Annals of the ICRP. ICRP publication 103. 37 (2–4). ISBN 978-0-7020-3048-2. Retrieved 17 May 2012.
External links
- Specific Gamma-Ray Dose Constants for Nuclides Important to Dosimetry and Radiological Assessment, Laurie M. Unger and D. K . Trubey, Oak Ridge National Laboratory, May 1982 - contains gamma-ray dose constants (in tissue) for approximately 500 radionuclides.






