Advanced airway management
| Advanced airway management | |
|---|---|
intubate a patient with challenging airway anatomy |
Advanced airway management is the subset of
This is accomplished by clearing or preventing obstructions of airways. There are multiple causes of potential airway obstructions, including the patient's own tongue or other anatomical components of the airway, foreign bodies, excessive amounts of blood and body fluids, or aspiration of food particles.
Unlike
Supraglottic airways in increasing order of invasiveness are nasopharyngeal (NPA), oropharyngeal (OPA), and laryngeal mask airways (LMA). Laryngeal mask airways can even be used to deliver general anesthesia or intubate a patient through the device. These are followed by infraglottic techniques, such as tracheal intubation and finally surgical techniques.
Advanced airway management is a key component in
Pharyngeal airways
Pharyngeal airway devices are used in spontaneously breathing patients to move the tongue away from the back of the throat to restore airway patency.[2][3] Obstruction of the upper airway caused by the tongue most commonly occurs during decreased levels of consciousness.[2][3][4] Pharyngeal airway devices include oropharyngeal airways (OPAs) and nasopharyngeal airways (NPAs). These devices are the simplest artificial airways.[3][4]
Oropharyngeal airways

An
Nasopharyngeal airways
A
Extraglottic airways
Extraglottic airway devices (EGDs) create a patent airway without entering the trachea. These devices are highly effective for providing oxygenation and ventilation.[3][5] They can be used as primary airway devices, such as during CPR, or as rescue devices in situations where securing an airway using other devices has failed.[3][5][4] EGDs are especially effective rescue devices for obese patients and patients with significant facial trauma.[3] EGDs do not protect the trachea from obstruction or aspiration. They may be used for several hours until a definitive airway can be secured.[5][4]
Each type of EGD has different features, including the ability to remove air from the stomach (gastric decompression) and perform tracheal intubation.[5][4] All EGDs can be placed without directly seeing the glottis (also called "blind" placement).[3][4] EGDs can be classified into supraglottic airways and retroglottic airways.[3][5]
Supraglottic airways
Supraglottic airway devices (SGAs) create a seal over the glottic opening to route oxygen directly into the trachea.[3][5] The SGAs consist entirely of laryngeal masks. Several manufacturers produce these devices, the most well known being the laryngeal mask airway (LMA).[3][5][4] Success rates of SGAs in securing airways are similar between the different models, and these devices provide effective ventilation in more than 98% of patients.[3][5] SGAs can be placed in under 30 seconds, making them advantageous for emergency use.[3] Serious complications are rare and usually result from nerve and soft tissue trauma in the pharynx during placement.[4]
Retroglottic airways
Retroglottic airway devices (RGAs) pass behind the glottis and into the
Tracheal intubation


Indications
There are specific indications or guidelines for deciding a more invasive and more secure airway is worth the associated risk:[6]
- respiratory failure
- apnea or the suspension of breathing
- decreased or altered level of consciousness, rapid mental status change, Glasgow Coma Scale score less than 8 (GCS<8).
- major trauma, such as penetrating injury to the abdomen or chest
- direct airway injury or facial burns
- high risk of aspiration
Methods
Direct Laryngoscopy
Classically, tracheal intubation has been performed utilizing direct

Video Laryngoscopy
Multiple intubation tools are now available with built-in video technology, also known as video laryngoscopy.
Fiberoptic Intubation
In patients with known difficult airways, fiberoptic intubation can be considered. This technique involves the use of a flexible fiberoptic bronchoscope for visualization of the vocal cords. The bronchoscope can be passed directly into the trachea and the endotracheal tube can be threaded over the bronchoscope into position. This technique has various advantages over direct laryngoscopy and video laryngoscopy techniques. The fiberoptic scope is flexible and can be directed by the operator, allowing it to traverse the upper airway with minimal manipulation of the patient's neck. The operator can manipulate the device around obstructions in the upper airway, making the technique advantageous for patients with cancer or swelling in the upper airway. The device is relatively small compared to a laryngoscope and can therefore be implemented in patients with small mouth openings. Additionally, the fiberoptic scope can be passed through the nostril to provide visualization for a nasotracheal intubation. Lastly, fiberoptic intubation can be conducted in an awake patient with sufficient use of local anesthetics, which can prove useful in patients who would otherwise be unable to be anesthetized without having a secure airway in place beforehand. [9]
Less Common Methods
There are a variety of less commonly used methods of intubation and ventilating a patient, which even includes methods avoiding tracheal intubation. Some of the more popular techniques include Lightwand intubation that uses an LED lit stylet to transilluminate the soft tissues of the neck if correctly placed in the trachea and then inserting an endotracheal tube through it. The Lightwand was originally developed for use in the military where a blood in the airway may obstruct an effective view of the glottis.[13][14]
Utilization of
Confirming placement
It is necessary to confirm placement of the endotracheal tube to ensure that the tube is properly positioned within the
Surgical airways
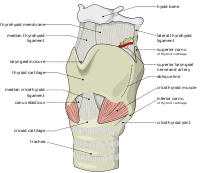
Surgical methods for airway management rely on making a surgical incision below the glottis in order to achieve direct access to the
Cricothyrotomy
A
Tracheotomy
A tracheotomy is a surgical procedure creating an incision in the front of the neck down to the trachea.[20][23] A tracheostomy tube can be placed through the opening created by the incision, which allows breathing through the tube rather than the nose and mouth.[20][24] Although the terms are sometimes used interchangeably, a "tracheotomy" is the surgical procedure creating an incision into the trachea, while "tracheostomy" refers to the opening in the trachea created by the incision.[24] The most common acute complications of a tracheotomy are difficulty speaking or swallowing due to nerve damage, prolonged bleeding at the incision site, and pneumothorax.[19][25] A tracheotomy is rarely indicated in an emergent setting. It more commonly performed in a controlled environment to create an airway that can be used long-term, such as for prolonged mechanical ventilation.[20][25]
Difficult airway algorithm
Various expert societies in airway management, including the American Society of Anesthesiologists, have recommended approaches to difficult airways. The algorithm provides a step-by-step framework to respond to situations where traditional airway management techniques may be inadequate. Current guidelines for airway management when inducing anesthesia where ventilation is inadequate recommend to call for help and limit attempts at
Pediatric considerations
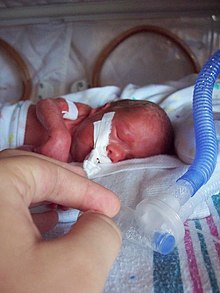
Many advanced airway techniques may be applied to children. In the fields of pediatric anesthesiology, pediatric critical care, and pediatric emergency medicine, a clear passage between the lungs and the environment is essential.[27]
Children have numerous anatomic differences from adults which present unique challenges when implementing advanced airway techniques.
Supraglottic airway devices, direct laryngoscopy, indirect video laryngoscopy, and fiberoptic intubation are all techniques which can be used to secure the pediatric airway. In the event that these techniques cannot adequately ventilate the patient, a surgical airway may be required. Surgical help should be requested for invasive access, however, in scenarios in which a pediatric
See also
References
- PMID 29761867.
- ^ OCLC 1021173545.)
{{cite book}}: CS1 maint: location missing publisher (link - ^ OCLC 1025330199.)
{{cite book}}: CS1 maint: location missing publisher (link) CS1 maint: others (link - ^ OCLC 1124935549.)
{{cite book}}: CS1 maint: location missing publisher (link) CS1 maint: others (link - ^ )
- ^ PMID 29262130, retrieved 2024-01-11
- PMID 32809565, retrieved 2024-01-11
- PMID 29763142, retrieved 2024-01-11
- ^ ISBN 978-1-260-47379-7.
- PMID 30020596, retrieved 2023-11-30
- ^ Lewis SR, Butler AR, Parker J, Cook TM, Smith AF. Videolaryngoscopy versus direct laryngoscopy for adult patients requiring tracheal intubation. Cochrane Database of Systematic Reviews 2016, Issue 11. Art. No: CD011136 DOI: 10.1002/14651858.CD011136.pub2.
- PMID 24741496.
- ISSN 1496-8975.
- ISSN 1496-8975.
- PMID 2683873.
- PMID 3813383.
- PMID 27343673.
- ^ Reichman, Eric F. (2013), "Chapter 12. Confirmation of Endotracheal Intubation", Emergency Medicine Procedures (2 ed.), New York, NY: The McGraw-Hill Companies, retrieved 2024-01-11
- ^ OCLC 1012122640.
- ^ )
- S2CID 219507502.
- PMID 30726035, retrieved 2024-01-12
- PMID 25581416.
- ^ a b Molnar, Heather. "What is a tracheostomy?". www.hopkinsmedicine.org. Retrieved 2022-01-19.
- ^ a b "Tracheostomy - Mayo Clinic". www.mayoclinic.org. Retrieved 2022-01-19.
- ISSN 0003-3022.
- ^ PMID 31073483.
