Alphavirus
This article has multiple issues. Please help improve it or discuss these issues on the talk page. (Learn how and when to remove these template messages)
|
Alphavirus is a genus of
Genome
This section needs additional citations for verification. (May 2023) |
| Alpha_E1_glycop | |||||||||
|---|---|---|---|---|---|---|---|---|---|
TCDB 1.G | | ||||||||
| OPM superfamily | 109 | ||||||||
| OPM protein | 1rer | ||||||||
| |||||||||
| Alpha_E2_glycop | |||||||||
|---|---|---|---|---|---|---|---|---|---|
TCDB 1.G | | ||||||||
| OPM superfamily | 109 | ||||||||
| OPM protein | 2yew | ||||||||
| |||||||||
| Alpha_E3_glycop | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Identifiers | |||||||||
| Symbol | Alpha_E3_glycop | ||||||||
TCDB | 1.G | ||||||||
| OPM superfamily | 109 | ||||||||
| |||||||||
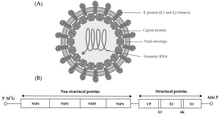
The alphaviruses are small, spherical, enveloped viruses with a genome of a single strand of positive-sense RNA. The total genome length ranges between 11,000 and 12,000 nucleotides, and has a
There are two
Structural proteins
The
Nonstructural proteins
Four nonstructural proteins (nsP1–4) which are produced as a single polyprotein constitute the virus' replication machinery.[5] The processing of the polyprotein occurs in a highly regulated manner, with cleavage at the P2/3 junction influencing RNA template use during genome replication. This site is located at the base of a narrow cleft and is not readily accessible. Before cleavage, nsP3 creates a ring structure that encircles nsP2. These two proteins have an extensive interface.
Mutations in nsP2 that produce noncytopathic viruses or a temperature sensitive phenotypes cluster at the P2/P3 interface region. P3 mutations opposite the location of the nsP2 noncytopathic mutations prevent efficient cleavage of P2/3. This in turn affects RNA infectivity altering viral RNA production levels.
Virology
The virus has a 60–70
The nucleocapsid, 40 nanometers in diameter, contains 240 copies of the capsid protein and has a T = 4 icosahedral symmetry. The E1 and E2 viral glycoproteins are embedded in the lipid bilayer. Single E1 and E2 molecules associate to form heterodimers. The E1–E2 heterodimers form one-to-one contacts between the E2 protein and the nucleocapsid monomers. The E1 and E2 proteins mediate contact between the virus and the host cell.
Several receptors have been identified. These include prohibitin, phosphatidylserine, glycosaminoglycans and ATP synthase β subunit (ref needed).
Replication occurs within the cytoplasm, specifically in areas termed "spherules" separated by plasma membrane invaginations from the rest. Each complex occupies one such area of about 50-nm in inner diameter.[6]
Virions mature by budding through the plasma membrane, where virus-encoded surface glycoproteins E2 and E1 are assimilated. These two glycoproteins are the targets of numerous serologic reactions and tests including neutralization and hemagglutination inhibition. The alphaviruses show various degrees of antigenic cross-reactivity in these reactions and this forms the basis for the seven antigenic complexes, 32 species and many subtypes and varieties. The E2 protein is the site of most neutralizing epitopes, while the E1 protein contains more conserved, cross-reactive epitopes.
Evolution
A study of this taxon suggests that this group of viruses had a marine origin—specifically the Southern Ocean—and that they have subsequently spread to both the Old and New World.[7]
There are three subgroups in this genus: the Semliki Forest virus subgroup (Semliki Forest, O'nyong-nyong and Ross River viruses); the eastern equine encephalitis virus subgroup (eastern equine encephalitis and Venezuelan equine encephalitis viruses) and the Sindbis virus subgroup.[8] Sindbis virus, geographically restricted to the Old World, is more closely related to the eastern equine encephalitis subgroup, which are New World viruses, than it is to the Semliki Forest virus subgroup which is also found in the Old World.
Taxonomy
The following species are assigned to the genus:[9]
- Aura virus
- Barmah Forest virus
- Bebaru virus
- Caaingua virus
- Cabassou virus
- Chikungunya virus
- Eastern equine encephalitis virus
- Eilat virus
- Everglades virus
- Fort Morgan virus
- Getah virus
- Highlands J virus
- Madariaga virus
- Mayaro virus
- Middelburg virus
- Mosso das Pedras virus
- Mucambo virus
- Ndumu virus
- O'nyong'nyong virus
- Pixuna virus
- Rio Negro virus
- Ross River virus
- Salmon pancreas disease virus
- Semliki Forest virus
- Sindbis virus
- Southern elephant seal virus
- Tonate virus
- Trocara virus
- Una virus
- Venezuelan equine encephalitis virus
- Western equine encephalitis virus
- Whataroa virus
The seven complexes are:
- Barmah Forest virus complex
- Eastern equine encephalitis complex
- Eastern equine encephalitis virus(seven antigenic types)
- Middelburg virus complex
- Ndumu virus complex
- Semliki Forest virus complex
- Bebaru virus
- Chikungunya virus
- Getah virus
- Mayaro virus
- Subtype: Una virus
- O'nyong'nyong virus
- Subtype: Igbo-Ora virus
- Ross River virus
- Subtype: Sagiyama virus
- Subtype:
- Semliki Forest virus
- Subtype: Me Tri virus
- Venezuelan equine encephalitis complex
- Cabassou virus
- Everglades virus
- Mosso das Pedras virus
- Mucambo virus
- Paramana virus
- Pixuna virus
- Rio Negro virus
- Trocara virus
- Subtype: Bijou Bridge virus
- Venezuelan equine encephalitis virus
- Western equine encephalitis complex
- Aura virus
- Babanki virus
- Kyzylagach virus
- Sindbis virus
- Ockelbo virus
- Whataroa virus
- Recombinants within this complex
- Buggy Creek virus
- Fort Morgan virus
- Highlands J virus
- Western equine encephalitis virus
- Unclassified
- Eilat virus
- Mwinilunga alphavirus
- Salmonid Alphavirus
- Southern elephant seal virus
- Tonatevirus
- Caaingua virus[10]
Notes
Barmah Forest virus is related to the Semliki Forest virus. Middelburg virus, although classified as a separate complex, may be a member of the Semliki Forest virus group.
It seems likely that the genus evolved in the Old World from an insect-borne plant virus.[11]
Sindbis virus may have originated in South America.[12] The equine encephalitis viruses and the Sindbis virus are related.
The Old World and New World viruses appears to have diverged between 2000 and 3000 years ago.[13] Divergence between the Venezuelan equine encephalitis virus and the eastern equine virus appears to have been ~1400 years ago.[14]
The fish infecting clade appears to be basal to the other species.
The southern elephant seal virus appears to be related to the Sinbis clade.
Pathogenesis and immune response
| Virus | Human Disease | Vertebrate Reservoir | Distribution |
|---|---|---|---|
| Barmah Forest virus |
|
Humans | Australia |
Chikungunya virus
|
Rash, arthritis | Primates, humans | Africa, Latin America, SE Asia
|
Eastern equine encephalitis virus
|
Encephalitis | Birds | Americas |
Mayaro virus
|
Rash, arthritis | Primates, humans | South America |
| O'nyong'nyong virus | Rash, arthritis | Primates, Humans | Africa |
| Ross River virus | Rash, arthritis | Mammals, humans | Australia, South Pacific |
| Semliki Forest virus | Rash, arthritis | Birds | Africa |
| Sindbis virus | Rash, arthritis | Birds | Europe, Africa, Australia |
| Tonate virus | Encephalitis | Humans | South America |
| Una virus | Rash, arthritis | Primates, humans | South America |
| Venezuelan equine encephalitis virus | Encephalitis | Rodents, horses | Americas |
| Western equine encephalitis virus | Encephalitis | Birds, mammals | North America |
There are many alphaviruses distributed around the world with the ability to cause human disease. Infectious
Terrestrial alphavirus infections are spread by insect vectors such as mosquitoes. Once a human is bitten by the infected mosquito, the virus can gain entry into the bloodstream, causing viremia. The alphavirus can also get into the CNS where it is able to grow and multiply within the neurones. This can lead to encephalitis, which can be fatal.
When an individual is infected with this particular virus, its immune system can play a role in clearing away the virus particles. Alphaviruses are able to cause the production of
Diagnosis, prevention, and control
Diagnoses is based on clinical samples from which the virus can be easily isolated and identified. There are no alphavirus vaccines currently available. Vector control with repellents, protective clothing, breeding site destruction, and spraying are the preventive measures of choice.[citation needed]
Research
Alphaviruses are of interest to
History
Initially, the Togaviridae family included what are now called the Flaviviruses, within the Alphavirus genus. The flaviviruses were formed into their own family when sufficient differences with the alphaviruses were noted due to the development of sequencing.[15] Rubella virus was formerly included in the family Togaviridae in its own genus Rubivirus, but is now classified in its own family Matonaviridae.[16] Alphavirus is now the sole genus in the family.
- 1930 – Western equine encephalitis virus is first isolated in the United States (the first alphavirus ever isolated)
- 1933 – Eastern equine encephalitis virusis first isolated in the United States.
- 1938 – Venezuelan equine encephalitis is isolated.
- 1941 – Western equine encephalitis epidemic is seen in the United States. It affects 300,000 horses and 3,336 humans.
- 1941 – cataracts following a rubella outbreak. This and other defects are then categorized under the congenital rubella syndrome.
- 1942 – Semliki Forest virus is isolated in Buliyama, Bwamba County, Uganda.
- 1952 – Sindbis virus is isolated in the Sindbis health district, 40 mi (64 km) north of Cairo, Egypt.
- 1959 – Ross River virus is isolated from Aedes vigilax mosquitoes (now known as Ochlerotatus vigilax)[17] which were trapped at the Ross River in Australia.
- 1963 – Ross River virus, which causes epidemic polyarthritis (mostly seen in Australia), is isolated by Doherty and colleagues.[18]
- 1971 – Last epidemic of Venezuelan equine encephalitis is seen in horses in southern Texas.[19]
- 1986 – Barmah Forest virus is identified as causing human disease in Australia.[20]
- 2001 – Scientists solved the Semliki Forest virus.
- 2005–2006 – Large epidemic of the
- 2006 – Major epidemic of the chikungunya virus in India with over 1.5 million cases reported[22]
See also
Sources
- "Arboviruses". Virology-online.
- "ICTV Sources". ICTV. Archived from the original on 12 February 2006.
- Smerdou, C.; Liljestrom, P. (2000). "Alphavirus vectors: from protein production to gene therapy". Gene Therapy and Regulation. 1 (1): 33–63. ISSN 1568-5586.
- Rayner JO, Dryga SA, Kamrud KI (2002). "Alphavirus vectors and vaccination". Reviews in Medical Virology. 12 (5): 279–96. S2CID 21432844.
- Rhême, Céline; Ehrengruber, Markus U.; Grandgirard, Denis (2005). "Alphaviral cytotoxicity and its implication in vector development". Experimental Physiology. 90 (1): 45–52. PMID 15542620.
- Schmaljohn, Alan L.; McClain, David (1996). "54. Alphaviruses (Togaviridae) and Flaviviruses (Flaviviridae)". In Baron, Samuel (ed.). Medical Microbiology (4th ed.). University of Texas Medical Branch at Galveston. PMID 21413253. NBK7633.
References
- PMID 32878245.
- PMID 29745869.
- PMID 8107141.
- S2CID 16535677.
- PMID 23010928.
- PMID 21389137.
- PMID 22190718.
- PMID 2155505.
- ^ "Virus Taxonomy: 2020 Release". International Committee on Taxonomy of Viruses (ICTV). March 2021. Retrieved 15 May 2021.
- PMID 31237479.
- PMID 11581380.
- PMID 20420530.
- PMID 8105605.
- PMID 1318187.
- ^ "Togaviridae". stanford.edu.
- ^ "ICTV Taxonomy List". Retrieved 5 May 2020.
- ^ "Aedes vigilax". NSW Arbovirus Surveillance & Vector Monitoring Program. The New South Wales Arbovirus Surveillance and Mosquito Monitoring Program. Archived from the original on 19 March 2018. Retrieved 5 June 2010.
Note that 'Ochlerotatus vigilax' prior to 2000, was known as 'Aedes vigilax'
- S2CID 13048176.
- PMID 8118792.
- S2CID 30837260.
- PMID 17187566.
- PMID 17175699.