ALS
| Amyotrophic lateral sclerosis | |
|---|---|
| Other names |
|
| Treatment | Walker (mobility); Wheelchair; Non-invasive ventilation;[5] Feeding tube; Augmentative and alternative communication; symptomatic management |
| Medication | Riluzole, Edaravone, Sodium phenylbutyrate/ursodoxicoltaurine, Tofersen, Dextromethorphan/quinidine |
| Prognosis | Life expectancy highly variable but typically 2–4 years after diagnosis[6] |
| Frequency | |
Amyotrophic lateral sclerosis (ALS), also known as motor neurone disease (MND) or Lou Gehrig's disease in the United States, is a rare but terminal neurodegenerative disorder that results in the progressive loss of both upper and lower motor neurons that normally control voluntary muscle contraction.[3] ALS is the most common form of the motor neuron diseases.[8] ALS often presents in its early stages with gradual muscle stiffness, twitches, weakness, and wasting.[3] Motor neuron loss typically continues until the abilities to eat, speak, move, and, lastly, breathe are all lost.[3] While only 15% of people with ALS also fully develop frontotemporal dementia, an estimated 50% face at least some minor difficulties with thinking and behavior.[9] Depending on which of the aforementioned symptoms develops first, ALS is classified as limb-onset (begins with weakness in the arms or legs) or bulbar-onset (begins with difficulty in speaking or swallowing).[10]
Most cases of ALS (about 90% to 95%) have
There is no known cure for ALS.[3] The goal of treatment is to slow the disease progression, and improve symptoms.[9] Treatments that slow ALS include riluzole (extends life by two to three months) and sodium phenylbutyrate/ursodoxicoltaurine (extends life by around seven months).[15][16] Non-invasive ventilation may result in both improved quality, and length of life.[5] Mechanical ventilation can prolong survival but does not stop disease progression.[17] A feeding tube may help maintain weight and nutrition.[18] Death is usually caused by respiratory failure.[19] The disease can affect people of any age, but usually starts around the age of 60.[19] The average survival from onset to death is two to four years, though this can vary, and about 10% of those affected survive longer than ten years.[20]
Descriptions of the disease date back to at least 1824 by Charles Bell.[21] In 1869, the connection between the symptoms and the underlying neurological problems was first described by French neurologist Jean-Martin Charcot, who in 1874 began using the term amyotrophic lateral sclerosis.[21]
Classification
ALS is a motor neuron disease, which is a group of neurological disorders that selectively affect motor neurons, the cells that control voluntary muscles of the body.[3] Other motor neuron diseases include primary lateral sclerosis (PLS), progressive muscular atrophy (PMA), progressive bulbar palsy, pseudobulbar palsy, and monomelic amyotrophy (MMA).[22]
As a disease, ALS itself can be classified in a few different ways: by which part of the motor neurons are affected; by the parts of the body first affected; whether it is genetic; and the age at which it started. Each individual diagnosed with the condition will sit at a unique place at the intersection of these complex and overlapping subtypes, which presents a challenge to diagnosis, understanding, and prognosis.[23]
Subtypes of motor neuron disease
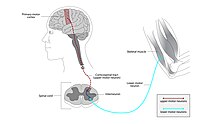
ALS can be classified by the types of motor neurons that are affected.
Classical, or classic ALS, involves degeneration to both the upper motor neurons in the brain and the lower motor neurons in the spinal cord.[6][2] Primary lateral sclerosis (PLS) involves degeneration of only the upper motor neurons, and progressive muscular atrophy (PMA) involves only the lower motor neurons. There is debate over whether PLS and PMA are separate diseases or simply variants of ALS.[9]
| Main ALS Subtypes | Upper motor neuron degeneration | Lower motor neuron degeneration |
|---|---|---|
| Classical ALS | Yes | Yes |
| Primary lateral sclerosis (PLS) | Yes | No |
| Progressive muscular atrophy (PMA) | No | Yes |
Classical ALS accounts for about 70% of all cases of ALS and can be subdivided into where symptoms first appear as these are usually focussed to one region of the body at initial presentation before later spread. Limb-onset ALS (also known as spinal-onset) and bulbar-onset ALS.
Primary lateral sclerosis (PLS) is a subtype of the overall ALS category which accounts for about 5% of all cases and only affects the upper motor neurons in the arms, legs, and bulbar region.[27] However, more than 75% of people with apparent PLS go on to later develop lower motor neuron signs within four years of symptom onset, meaning that a definitive diagnosis of PLS cannot be made until several years have passed.[28] PLS has a better prognosis than classical ALS, as it progresses slower, results in less functional decline, does not affect the ability to breathe, and causes less severe weight loss than classical ALS.[27]
Progressive muscular atrophy (PMA) is another subtype that accounts for about 5% of the overall ALS category and affects lower motor neurons in the arms, legs, and bulbar region.[27] While PMA is associated with longer survival on average than classical ALS, it is still progressive over time, eventually leading to respiratory failure and death.[9] As with PLS developing into classical ALS, PMA can also develop into classical ALS over time if the lower motor neuron involvement progresses to include upper motor neurons, in which case the diagnosis might be changed to classic ALS.[28]
Rare isolated variants of ALS
Isolated variants of ALS have symptoms that are limited to a single region for at least a year; they progress more slowly than classical ALS and are associated with longer survival.[2] These regional variants of ALS can only be considered as a diagnosis should the initial symptoms fail to spread to other spinal cord regions for an extended period of time (at least 12 months).[29] Flail arm syndrome is characterized by lower motor neuron damage affecting the arm muscles, typically starting with the upper arms symmetrically and progressing downwards to the hands.[2] Flail leg syndrome is characterized by lower motor neuron damage leading to asymmetrical weakness and wasting in the legs starting around the feet.[2] Isolated bulbar palsy is characterized by upper or lower motor neuron damage in the bulbar region (in the absence of limb symptoms for at least 20 months),[30] leading to gradual onset of difficulty with speech (dysarthria) and swallowing (dysphagia).

Age of onset
ALS can also be classified based on the age of onset. While the peak age of onset is 58 to 63 for sporadic ALS and 47 to 52 for genetic ALS,
Signs and symptoms
The disorder causes muscle weakness,
Initial symptoms
The start of ALS may be so subtle that the symptoms are overlooked.[3] The earliest symptoms of ALS are muscle weakness or muscle atrophy, typically on one side of the body. Other presenting symptoms include trouble swallowing or breathing, cramping, or stiffness of affected muscles; muscle weakness affecting an arm or a leg; or slurred and nasal speech. The parts of the body affected by early symptoms of ALS depend on which motor neurons in the body are damaged first.[34]
In limb-onset ALS, the first symptoms are in the arms or the legs. If the legs are affected first, people may experience awkwardness, tripping, or stumbling when walking or running; this is often marked by walking with a "dropped foot" that drags gently on the ground. If the arms are affected first, they may experience difficulty with tasks requiring manual dexterity, such as buttoning a shirt, writing, or turning a key in a lock.[35]
In bulbar-onset ALS, the first symptoms are difficulty speaking or swallowing. Speech may become slurred, nasal in character, or quieter. There may be difficulty with swallowing and loss of tongue mobility. A smaller proportion of people experience "respiratory-onset" ALS, where the
Over time, people experience increasing difficulty moving, swallowing (dysphagia), and speaking or forming words (dysarthria). Symptoms of upper motor neuron involvement include tight and stiff muscles (spasticity) and exaggerated reflexes (hyperreflexia), including an overactive gag reflex.[24] While the disease does not cause pain directly, pain is a symptom experienced by most people with ALS caused by reduced mobility.[36] Symptoms of lower motor neuron degeneration include muscle weakness and atrophy, muscle cramps, and fleeting twitches of muscles that can be seen under the skin (fasciculations).[25]
Progression
Although the initial site of symptoms and subsequent rate of disability progression vary from person to person, the initially affected body region is usually the most affected over time, and symptoms usually spread to a neighbouring body region. For example, symptoms starting in one arm usually spread next to either the opposite arm or to the leg on the same side.[24] Bulbar-onset patients most typically get their next symptoms in their arms rather than legs, arm-onset patients typically spreads to the legs before the bulbar region, and leg-onset patients typically spread to the arms rather than the bulbar region.[37] Over time, regardless of where symptoms began, most people eventually lose the ability to walk or use their hands and arms independently. Less consistently, they may lose the ability to speak and to swallow food. It is the eventual development of weakness of the respiratory muscles, with the loss of ability to cough and to breathe without support, that is ultimately life-shortening in ALS.[5]
The rate of progression can be measured using the ALS Functional Rating Scale - Revised (ALSFRS-R), a 12-item instrument survey administered as a clinical interview or self-reported questionnaire that produces a score between 48 (normal function) and 0 (severe disability).[38] The ALSFRS-R is the most frequently used outcome measure in clinical trials[39] and is used by doctors to track disease progression.[40] Though the degree of variability is high and a small percentage of people have a much slower progression, on average people with ALS lose about 1 ALSFRS-R point per month.[41] Brief periods of stabilization ("plateaus") and even small reversals in ALSFRS-R score are not uncommon, due to the fact the tool is subjective, can be affected by medication, and different forms of compensation for changes in function.[42] However, it is rare (<1%) for these improvements to be large (i.e. greater than 4 ALSFRS-R points) or sustained (i.e. greater than 12 months).[42] A survey-based study among clinicians showed that they rated a 20% change in the slope of the ALSFRS-R as being clinically meaningful, which is the most common threshold used to determine whether a new treatment is working in clinical trials.[43]
Late stage disease management
Difficulties with chewing and swallowing make eating very difficult (
Prognosis, staging, and survival
Although respiratory support using non-invasive ventilation can ease problems with breathing and prolong survival,[48] it does not affect the progression rate of ALS. Most people with ALS die between two and four years after the diagnosis.[5] Around 50% of people with ALS die within 30 months of their symptoms beginning, about 20% live between five and ten years,[19] and about 10% survive for 10 years or longer.[20]
The most common cause of death among people with ALS is respiratory failure, often accelerated by pneumonia.[19] Most ALS patients die at home after a period of worsening difficulty breathing, a decline in their nutritional status, or a rapid worsening of symptoms.[49] Sudden death or acute respiratory distress are uncommon.[50] Access to palliative care is recommended from an early stage to explore options, ensure psychosocial support for the patient and caregivers, and to discuss advance healthcare directives.[49]
As with cancer staging, ALS has staging systems numbered between 1 and 4 that are used for research purposes in clinical trials.[6] Two very similar staging systems emerged around a similar time, the King's staging system and Milano-Torino (MiToS) functional staging.[51]
| Stage 1 | Stage 2 | Stage 3 | Stage 4 | |
|---|---|---|---|---|
| Stage description | Symptom onset, involvement of the first region | 2A: Diagnosis
2B: Involvement of the second region |
Involvement of the third region | 4A: Need for a feeding tube
4B: Need for non-invasive ventilation |
| Median time to stage | 13.5 months | 17.7 months | 23.3 months | 4A: 17.7 months
4B: 30.3 months |
| Stage 0 | Stage 1 | Stage 2 | Stage 3 | Stage 4 | Stage 5 | |
|---|---|---|---|---|---|---|
| Stage description | No loss of a functional domain | Loss of 1 domain | Loss of 2 domains | Loss of 3 domains | Loss of 4 domains | Death |
| Probability of death at each stage | 7% | 26% | 33% | 33% | 86% |
Providing individual patients with a precise prognosis is not currently possible, though research is underway to provide statistical models on the basis of prognostic factors including age at onset, progression rate, site of onset, and presence of frontotemporal dementia.[6] Those with a bulbar onset have a worse prognosis than limb-onset ALS; a population-based study found that bulbar-onset ALS patients had a median survival of 2.0 years and a 10-year survival rate of 3%, while limb-onset ALS patients had a median survival of 2.6 years and a 10-year survival rate of 13%.[52] Those with respiratory-onset ALS had a shorter median survival of 1.4 years and 0% survival at 10 years.[52] While astrophysicist Stephen Hawking lived for 55 more years following his diagnosis, his was an unusual case.[53]
Cognitive, emotional, and behavioral symptoms
Cognitive impairment or behavioral dysfunction is present in 30–50% of individuals with ALS,[54] and can appear more frequently in later stages of the disease.[55] Language dysfunction, executive dysfunction, and troubles with social cognition and verbal memory are the most commonly reported cognitive symptoms in ALS.[55] Cognitive impairment is found more frequently in patients with C9orf72 gene repeat expansions, bulbar onset, bulbar symptoms, family history of ALS, and/or a predominantly upper motor neuron phenotype.[56]
Emotional lability is a symptom in which patients cry, smile, yawn, or laugh, either in the absence of emotional stimuli, or when they are feeling the opposite emotion to that being expressed;[57] it is experienced by about half of ALS patients and is more common in those with bulbar-onset ALS.[5] While relatively benign relative to other symptoms, it can cause increased stigma and social isolation as people around the patient struggle to react appropriately to what can be frequent and inappropriate outbursts in public.[58]
In addition to mild changes in cognition that may only emerge during neuropsychological testing, around 10–15% of individuals have signs of frontotemporal dementia (FTD).[5] Repeating phrases or gestures, apathy, and loss of inhibition are the most frequently reported behavioral features of ALS.[59] ALS and FTD are now considered to be part of a common disease spectrum (ALS–FTD) because of genetic, clinical, and pathological similarities.[60] Genetically, repeat expansions in the C9orf72 gene account for about 40% of genetic ALS and 25% of genetic FTD.[61]
Cognitive and behavioral issues are associated with poorer prognosis as they may reduce adherence to medical advice, and deficits in empathy and social cognition which may increase caregiver burden.[62]
Cause
It is not known what causes sporadic ALS, hence it is described as an
Genetics and genetic testing
While they appear identical clinically and pathologically,
There is considerable variation among clinicians on how to approach genetic testing in ALS, and only about half discuss the possibility of genetic inheritance with their patients, particularly if there is no discernible family history of the disease.[68] In the past, genetic counseling and testing was only offered to those with obviously familial ALS.[14] But it is increasingly recognized that cases of sporadic ALS may also be due to disease-causing de novo mutations in SOD1, or C9orf72,[69] an incomplete family history, or incomplete penetrance, meaning that a patient's ancestors carried the gene but did not express the disease in their lifetimes.[14] The lack of positive family history may be caused by lack of historical records, having a smaller family, older generations dying earlier of causes other than ALS, genetic non-paternity, and uncertainty over whether certain neuropsychiatric conditions (e.g. frontotemporal dementia, other forms of dementia, suicide, psychosis, schizophrenia) should be considered significant when determining a family history.[14] There have been calls in the research community to routinely counsel and test all diagnosed ALS patients for familial ALS,[70] particularly as there is now a licensed gene therapy (tofersen) specifically targeted to carriers of SOD-1 ALS. A shortage of genetic counselors and limited clinical capacity to see such at-risk individuals makes this challenging in practice, as does the unequal access to genetic testing around the world.[71]
More than 40 genes have been associated with ALS, of which four account for nearly half of familial cases, and around 5% of sporadic cases:
Environmental and other factors
The multi-step hypothesis suggests the disease is caused by some interaction between an individual's genetic risk factors and their cumulative lifetime of exposures to environmental factors, termed their
Although some personality traits, such as openness,[73] agreeableness[74] and conscientiousness[74] appear remarkably common among patients with ALS, it remains open whether personality can increase susceptibility to ALS directly.[75] Instead, genetic factors giving rise to personality might simultaneously predispose people to developing ALS,[73] or the above personality traits might underlie lifestyle choices which are in turn risk factors for ALS.[74]
Pathophysiology
Neuropathology
Upon examination at autopsy, features of the disease that can be
The defining feature of ALS is the death of both upper motor neurons (located in the
Biochemistry
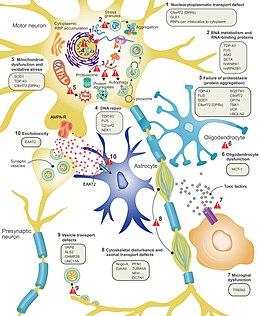
It is still not fully understood why neurons die in ALS, but this
There are a number of ALS genes that encode for RNA-binding proteins. The first to be discovered was TDP-43 protein,[77] a nuclear protein that aggregates in the cytoplasm of motor neurons in almost all cases of ALS; however, mutations in TARDBP, the gene that codes for TDP-43, are a rare cause of ALS.[10] FUS codes for FUS, another RNA-binding protein with a similar function to TDP-43, which can cause ALS when mutated.[61] It is thought that mutations in TARDBP and FUS increase the binding affinity of the low-complexity domain, causing their respective proteins to aggregate in the cytoplasm.[83] Once these mutant RNA-binding proteins are misfolded and aggregated, they may be able to misfold normal proteins both within and between cells in a prion-like manner.[77] This also leads to decreased levels of RNA-binding protein in the nucleus, which may mean that their target RNA transcripts do not undergo normal processing. Other RNA metabolism genes associated with ALS include ANG, SETX, and MATR3.[10]
C9orf72 is the most commonly mutated gene in ALS and causes motor neuron death through a number of mechanisms.
Diagnosis
No single test can provide a definite diagnosis of ALS. Because symptoms of ALS can be similar to those of a wide variety of other, more treatable diseases or disorders, appropriate tests must be conducted to exclude the possibility of other conditions. One of these tests is Differential diagnosis
Based on the person's symptoms and findings from the examination and from these tests, the physician may order tests on blood and urine samples to eliminate the possibility of other diseases, as well as routine laboratory tests. In some cases, for example, if a physician suspects the person may have a myopathy rather than ALS, a muscle biopsy may be performed.[3]
A number of infectious diseases can sometimes cause ALS-like symptoms,
ALS must be differentiated from the "ALS mimic syndromes", which are unrelated disorders that may have a similar presentation and clinical features to ALS or its variants.[89] Because the prognosis of ALS and closely related subtypes of motor neuron disease are generally poor, neurologists may carry out investigations to evaluate and exclude other diagnostic possibilities. Disorders of the neuromuscular junction, such as myasthenia gravis (MG) and Lambert–Eaton myasthenic syndrome, may also mimic ALS, although this rarely presents diagnostic difficulty over time.[90][91] Benign fasciculation syndrome and cramp fasciculation syndrome may also, occasionally, mimic some of the early symptoms of ALS. Nonetheless, the absence of other neurological features that develop inexorably with ALS means that, over time, the distinction will not present any difficulty to the experienced neurologist; where doubt remains, EMG may be helpful.[92]
Management
There is no cure for ALS.[9] Management focuses on treating symptoms and providing supportive care, with the goal of improving quality of life and prolonging survival.[9] This care is best provided by multidisciplinary teams of healthcare professionals; attending a multidisciplinary ALS clinic is associated with longer survival, fewer hospitalizations, and improved quality of life.[5]
Non-invasive ventilation (NIV) is the main treatment for respiratory failure in ALS.[10] In people with normal bulbar function, it prolongs survival by about seven months and improves quality of life. One study found that NIV is ineffective for people with poor bulbar function[93] while another suggested that it may provide a modest survival benefit.[9] Many people with ALS have difficulty tolerating NIV.[94] Invasive ventilation is an option for people with advanced ALS when NIV is not enough to manage their symptoms.[5] While invasive ventilation prolongs survival, disease progression and functional decline continue.[17] It may decrease the quality of life of people with ALS or their caregivers.[18][17] Invasive ventilation is more commonly used in Japan than in North America or Europe.[95]
Physical therapy can promote functional independence[96][97] through an aerobic, range of motion, and stretching exercises.[98] Occupational therapy can assist with activities of daily living through adaptive equipment.[99] Speech therapy can assist people with ALS who have difficulty speaking.[97] Preventing weight loss and malnutrition in people with ALS improves both survival and quality of life.[9] Initially, difficulty swallowing (dysphagia) can be managed by dietary changes and swallowing techniques. A feeding tube should be considered if someone with ALS loses 5% or more of their body weight or if they cannot safely swallow food and water.[10] The feeding tube is usually inserted by percutaneous endoscopic gastrostomy (PEG). There is weak evidence that PEG tubes improve survival.[100] PEG insertion is usually performed with the intent of improving quality of life.[18]
Palliative care should begin shortly after someone is diagnosed with ALS.[101] Discussion of end-of-life issues gives people with ALS time to reflect on their preferences for end-of-life care and can help avoid unwanted interventions or procedures. Hospice care can improve symptom management at the end of life and increases the likelihood of a peaceful death.[18] In the final days of life, opioids can be used to treat pain and dyspnea, while benzodiazepines can be used to treat anxiety.[17]
Medications
Disease-slowing treatments

Edaravone has been shown to modestly slow the decline in function in a small group of people with early-stage ALS.[104][105] It may work by protecting motor neurons from oxidative stress.[106] The most common side effects are bruising and gait disturbance.[105] Edaravone is available as an intravenous infusion or as an oral suspension.[107]
Symptomatic treatments
Other medications may be used to help reduce fatigue, ease muscle cramps, control spasticity, and reduce excess saliva and
Depression can be treated with
A 2017 review concluded that mexiletine is safe and effective for treating cramps in ALS based on a randomized controlled trial from 2016.[105]
Breathing support
Non-invasive ventilation

Non-invasive ventilation (NIV) is the primary treatment for respiratory failure in ALS[10] and was the first treatment shown to improve both survival and quality of life.[5] NIV uses a face or nasal mask connected to a ventilator that provides intermittent positive pressure to support breathing. Continuous positive pressure is not recommended for people with ALS because it makes breathing more difficult.[17] Initially, NIV is used only at night[5] because the first sign of respiratory failure is decreased gas exchange (hypoventilation) during sleep; symptoms associated with this nocturnal hypoventilation include interrupted sleep, anxiety, morning headaches, and daytime fatigue.[94] As the disease progresses, people with ALS develop shortness of breath when lying down, during physical activity or talking, and eventually at rest.[114] Other symptoms include poor concentration, poor memory, confusion, respiratory tract infections, and a weak cough. Respiratory failure is the most common cause of death in ALS.[5]
It is important to monitor the respiratory function of people with ALS every three months because beginning NIV soon after the start of respiratory symptoms is associated with increased survival. This involves asking the person with ALS if they have any respiratory symptoms and measuring their respiratory function.
Non-invasive ventilation prolongs survival longer than riluzole.[115] A 2006 randomized controlled trial found that NIV prolongs survival by about 48 days and improves the quality of life; however, it also found that some people with ALS benefit more from this intervention than others. For those with normal or only moderately impaired bulbar function, NIV prolongs survival by about seven months and significantly improves the quality of life. For those with poor bulbar function, NIV neither prolongs survival nor improves the quality of life, though it does improve some sleep-related symptoms.[93] Despite the clear benefits of NIV, about 25–30% of all people with ALS are unable to tolerate it, especially those with cognitive impairment or bulbar dysfunction.[94] Results from a large 2015 cohort study suggest that NIV may prolong survival in those with bulbar weakness, so NIV should be offered to all people with ALS, even if it is likely that they will have difficulty tolerating it.[9]
Invasive ventilation
Invasive ventilation bypasses the nose and mouth (the upper airways) by making a cut in the trachea (
Therapy

Physical therapy plays a large role in rehabilitation for individuals with ALS. Specifically, physical, occupational, and speech therapists can set goals and promote benefits for individuals with ALS by delaying loss of strength, maintaining endurance, limiting pain, improving speech and swallowing, preventing complications, and promoting functional independence.[96][97]
Occupational therapy and special equipment such as assistive technology can also enhance people's independence and safety throughout the course of ALS.[99] Gentle, low-impact aerobic exercise such as performing activities of daily living, walking, swimming, and stationary bicycling can strengthen unaffected muscles, improve cardiovascular health, and help people fight fatigue and depression. Range of motion and stretching exercises can help prevent painful spasticity and shortening (contracture) of muscles.[116] Physical and occupational therapists can recommend exercises that provide these benefits without overworking muscles because muscle exhaustion can lead to a worsening of symptoms associated with ALS, rather than providing help to people with ALS.[98] They can suggest devices such as ramps, braces, walkers, bathroom equipment (shower chairs, toilet risers, etc.), and wheelchairs that help people remain mobile. Occupational therapists can provide or recommend equipment and adaptations to enable ALS people to retain as much safety and independence in activities of daily living as possible.[99] Since respiratory insufficiency is the primary cause of mortality, physical therapists can help improve respiratory outcomes in people with ALS by implementing pulmonary physical therapy. This includes inspiratory muscle training, lung volume recruitment training, and manual assisted cough therapy aimed at increasing respiratory muscle strength as well as increasing survival rates.[117]
People with ALS who have difficulty speaking or swallowing may benefit from working with a
Nutrition

Preventing weight loss and malnutrition in people with ALS improves both survival and quality of life.[9] Weight loss in ALS is caused by muscle wasting, increased resting energy expenditure, and decreased food intake. Difficulty swallowing (dysphagia) develops in about 85% of people with ALS at some point over the course of their disease, leading to malnutrition and weight loss.[17] It is important to regularly assess the weight and swallowing ability of people with ALS.[5] Initially, dysphagia may be managed by dietary changes and modified swallowing techniques.[10] Difficulty swallowing liquids usually develops first and can be managed by switching to thicker liquids like fruit nectar or smoothies, or by adding fluid thickeners to thin fluids like water and coffee. People with ALS should eat soft, moist foods, which tend to be easier to swallow than dry, crumbly, or chewy foods.[114] They should also be instructed on proper head posture during swallowing, which can make swallowing easier.[10] There is tentative evidence that high-calorie diets may prevent further weight loss and improve survival.[105]
A
There is weak evidence that PEG tubes improve survival.[100] PEG insertion is usually performed with the intent of improving quality of life[18] by sustaining nutrition and medication intake.[5] This makes up for reduced oral food intake,[5] decreases risk of weight loss and dehydration, and can decrease anxiety by shortening what can become extended time taken to eat at mealtimes.[18]
End-of-life care
Epidemiology
ALS is the most common motor neuron disease in adults and the third most common neurodegenerative disease[61] after Alzheimer's disease and Parkinson's disease.[119] Worldwide the number of people who develop ALS yearly is estimated to be 1.9 people per 100,000 per year, while the number of people who have ALS at any given time is estimated to be about 4.5 people per 100,000.[120] In Europe, the number of new cases a year is about 2.6 people per 100,000, while the number affected is 7–9 people per 100,000.[121] The lifetime risk of developing ALS is 1:350 for European men and 1:400 for European women. Men have a higher risk mainly because spinal-onset ALS is more common in men than women.[63] The number of those with ALS in the United States in 2015 was 5.2 people per 100,000, and was higher in whites, males, and people over 60 years old.[122] The number of new cases is about 0.8 people per 100,000 per year in east Asia and about 0.7 people per 100,000 per year in south Asia. About 80% of ALS epidemiology studies have been conducted in Europe and the United States, mostly in people of northern European descent.[10] There is not enough information to determine the rates of ALS in much of the world, including Africa, parts of Asia, India, Russia, and South America.[63] There are several geographic clusters in the Western Pacific where the prevalence of ALS was reported to be 50–100 times higher than the rest of the world, including Guam, the Kii Peninsula of Japan, and Western New Guinea. The incidence in these areas has decreased since the 1960s;[1] the cause remains unknown.[63]

People of all races and ethnic backgrounds may be affected by ALS,[122] but it is more common in whites than in Africans, Asians, or Hispanics.[123] In the United States in 2015, the prevalence of ALS in whites was 5.4 people per 100,000, while the prevalence in blacks was 2.3 people per 100,000. The Midwest had the highest prevalence of the four US Census regions with 5.5 people per 100,000, followed by the Northeast (5.1), the South (4.7), and the West (4.4). The Midwest and Northeast likely had a higher prevalence of ALS because they have a higher proportion of whites than the South and West.[122] Ethnically mixed populations may be at a lower risk of developing ALS; a study in Cuba found that people of mixed ancestry were less likely to die from ALS than whites or blacks.[124] There are also differences in the genetics of ALS between different ethnic groups; the most common ALS gene in Europe is C9orf72, followed by SOD1, TARDBP, and FUS, while the most common ALS gene in Asia is SOD1, followed by FUS, C9orf72, and TARDBP.[125]
ALS can affect people at any age,
History


Descriptions of the disease date back to at least 1824 by Charles Bell.[21] In 1850, François-Amilcar Aran was the first to describe a disorder he named "progressive muscular atrophy", a form of ALS in which only the lower motor neurons are affected.[127] In 1869, the connection between the symptoms and the underlying neurological problems were first described by Jean-Martin Charcot, who initially introduced the term amyotrophic lateral sclerosis in his 1874 paper.[21] Flail arm syndrome, a regional variant of ALS, was first described by Alfred Vulpian in 1886. Flail leg syndrome, another regional variant of ALS, was first described by Pierre Marie and his student Patrikios in 1918.[128]
Diagnostic criteria
In the 1950s,
Name
Amyotrophic comes from Greek: a- means "no", myo- (from mûs) refers to "muscle", and trophḗ means "nourishment". Therefore, amyotrophy means "muscle malnourishment"[134] or the wasting of muscle tissue.[135] Lateral identifies the locations in the spinal cord of the affected motor neurons. Sclerosis means "scarring" or "hardening" and refers to the death of the motor neurons in the spinal cord.[134]
ALS is sometimes referred to as Charcot's disease (not to be confused with
In the United States and continental Europe, the term ALS (as well as Lou Gehrig's disease in the US) refers to all forms of the disease, including "classical" ALS, progressive bulbar palsy, progressive muscular atrophy, and primary lateral sclerosis.[139][33] In the United Kingdom and Australia, the term motor neurone disease refers to all forms of the disease while ALS only refers to "classical" ALS, meaning the form with both upper and lower motor neuron involvement.[139]
Society and culture
In addition to the baseball player Lou Gehrig and the theoretical physicist Stephen Hawking (who notably lived longer than any other known person with the condition) a number of other notable individuals have or have had ALS.[65] People with ALS have been featured in high-profile works such as the memoir Tuesdays with Morrie and the critically acclaimed motion picture The Theory of Everything.
In August 2014 the "Ice Bucket Challenge" to raise money for ALS research went viral online.[140] Participants filmed themselves filling a bucket full of ice water and pouring it onto themselves; they then nominated other individuals to do the same. Many participants donated to ALS research at the ALS Association, the ALS Therapy Development Institute, ALS Society of Canada, or Motor Neurone Disease Association in the UK.[141]
References
![]() This article incorporates text from this source, which is in the public domain: "Amyotrophic Lateral Sclerosis Fact Sheet". Archived from the original on 18 November 2004.
This article incorporates text from this source, which is in the public domain: "Amyotrophic Lateral Sclerosis Fact Sheet". Archived from the original on 18 November 2004.
- ^ PMID 19192301.
- ^ PMID 32526057.
- ^ a b c d e f g h i j k l m n o p q r "Amyotrophic Lateral Sclerosis (ALS) Fact Sheet". National Institute of Neurological Disorders and Stroke. Archived from the original on 5 January 2017. Retrieved 22 October 2020.
- S2CID 249014375.
- ^ (PDF) from the original on 1 December 2020. Retrieved 20 December 2019.
- ^ PMID 35334233.
- PMID 31329211.
- ^ "Motor Neuron Diseases Fact Sheet". www.ninds.nih.gov. National Institute of Neurological Disorders and Stroke. Archived from the original on 10 October 2020. Retrieved 27 October 2020.
- ^ S2CID 24483077.
- ^ (PDF) from the original on 1 December 2020. Retrieved 20 December 2019.
- ^ "Understanding ALS". The ALS Association. Archived from the original on 26 October 2020. Retrieved 28 October 2020.
- ^ PMID 22132186.
- ^ "Amyotrophic lateral sclerosis". MedlinePlus Genetics. Retrieved 7 August 2023.
- ^ PMID 35334234.
- ^ a b "FDA-Approved Drugs for Treating ALS". The ALS Association. Archived from the original on 25 April 2023. Retrieved 25 April 2023.
- S2CID 251162676.
- ^ PMID 28461024.
- ^ S2CID 34109901.
- ^ PMID 21296405.
- ^ S2CID 205345019.
- ^ PMID 11255459.
- ^ "8B60 Motor neuron disease". ICD-11 for Mortality and Morbidity Statistics. World Health Organization. Archived from the original on 1 August 2018. Retrieved 24 January 2019.
- PMID 34942899.
- ^ PMID 28003278.
- ^ PMID 32809609. Retrieved 27 August 2023.
- S2CID 27672209.
- ^ from the original on 31 December 2018. Retrieved 22 August 2018.
- ^ S2CID 45285510.
- PMID 26515621.
- PMID 34686150.
- PMID 34946884.
- PMID 28634552.
- ^ PMID 28477850.
- PMID 23678876.
- ^ "Motor neurone disease". UK: National Health Service. 15 January 2018. Archived from the original on 29 December 2014. Retrieved 24 October 2020.
- ^ S2CID 38905437.
- PMID 32558369.
- S2CID 7057926.
- PMID 34901853.
- S2CID 31734765.
- PMID 25298304.
- ^ PMID 26658909.
- S2CID 207619689.
- ^ PMID 30837936.
- S2CID 7650356.
- PMID 21603029.
- PMID 31391247.
- S2CID 195805546.
- ^ from the original on 28 May 2023. Retrieved 30 April 2023.
- S2CID 40367873.
- PMID 28054828.
- ^ (PDF) from the original on 24 November 2022. Retrieved 4 August 2022.
- ^ Landau E (20 September 2009). "Stephen Hawking serves as role model for ALS patients". CNN. Archived from the original on 15 August 2016.
- ^ PMID 28408982.
- ^ PMID 30209236.
- S2CID 231858696.
- S2CID 12807996.
- S2CID 21066800.
- S2CID 22224140.
- PMID 28449882.
- ^ PMID 24369373.
- S2CID 22082109.
- ^ S2CID 25040863.
- ^ a b "Amyotrophic lateral sclerosis (ALS) - Symptoms and causes". Mayo Clinic. Archived from the original on 6 April 2022. Retrieved 6 April 2022.
- ^ a b c "Who Gets ALS?". The ALS Association. Archived from the original on 6 April 2022. Retrieved 6 April 2022.
- (PDF) from the original on 7 May 2020. Retrieved 20 December 2019.
- PMID 35379930.
- S2CID 254150195.
- PMID 34518333.
- PMID 35379930.
- from the original on 27 May 2023. Retrieved 27 May 2023.
- ^ from the original on 17 November 2022. Retrieved 27 May 2023.
- ^ S2CID 20998807.
- ^ PMID 30239176.
- PMID 28127517.
- S2CID 208941.
- ^ from the original on 25 February 2021. Retrieved 20 December 2019.
- S2CID 34398467.
- PMID 27213408.
- PMID 32819425.
- PMID 28468939.
- PMID 30050368.
- PMID 27033831.
- PMID 29605155.
- PMID 27059391.
- PMID 33398403.
- PMID 31001186.
- PMID 23523708.
- PMID 21412713.
- ^ Stickler DE. Lorenzo N (ed.). "Lambert-Eaton Myasthenic Syndrome (LEMS)". Misc.medscape.com. Archived from the original on 14 May 2013. Retrieved 18 April 2013.
- ^ "Lambert-Eaton Myasthenic Syndrome: About". LEMS.com. BioMarin Pharmaceutical Inc. Archived from the original on 20 January 2013. Retrieved 18 April 2013.
- PMID 20959307.
- ^ PMID 28982219.
- ^ PMID 26166297.
- ^ S2CID 26282198.
- ^ PMID 18198431.
- ^ a b c d e "Amyotrophic Lateral Sclerosis (ALS)". American Speech-Language-Hearing Association, Rockville, MD. Archived from the original on 2 August 2012. Retrieved 30 November 2016.
- ^ PMID 20015852.
- ^ PMID 24367951.
- ^ PMID 37579081.
- ^ S2CID 5746940.
- ^ PMID 22419278.
- PMID 21412722.
- PMID 28522181.
- ^ PMID 29399045.
- PMID 28872907.
- ^ Center for Drug Evaluation and Research (16 June 2022). "FDA Approves Oral Form for the treatment of adults with amyotrophic lateral sclerosis (ALS)". U.S. Food and Drug Administration. Archived from the original on 12 May 2022. Retrieved 25 April 2023.
- ^ "AMX0035 (RELYVRIO)". The ALS Association. Archived from the original on 25 April 2023. Retrieved 25 April 2023.
- ^ "ALS drug will be pulled from US market after study showed patients didn't benefit". AP News. 4 April 2024. Retrieved 4 April 2024.
- ^ Amylyx Pharmaceuticals Inc. (4 January 2023). A Phase III, Randomized, Double-Blind, Placebo-Controlled, Multicenter Trial to Evaluate the Safety and Efficacy of AMX0035 Versus Placebo for 48-week Treatment of Adult Patients With Amyotrophic Lateral Sclerosis (ALS) (Report). clinicaltrials.gov.
- ^ a b "FDA approves treatment of amyotrophic lateral sclerosis associated with a mutation in the SOD1 gene" (Press release). U.S. Food and Drug Administration (FDA). 25 April 2023. Archived from the original on 25 April 2023. Retrieved 25 April 2023.
- S2CID 252438252.
- PMID 25934855.
- ^ PMID 26409693.
- PMID 24640982.
- PMID 24510737.
- S2CID 7279853.
- S2CID 26479278.
- ISBN 978-9283221630.
- PMID 23860588.
- from the original on 21 December 2019. Retrieved 22 August 2018.
- ^ PMID 30462626.
- ^ PMID 27510634.
- ^ PMID 28477849.
- S2CID 41974606.
- ^ PMID 27191240.
- S2CID 22629725.
- PMID 19307543.
- S2CID 32884687.
- S2CID 32678612.
- S2CID 22725949.
- S2CID 14851649.
- S2CID 215823371.
- ^ a b "What is ALS?". The ALS Association. Archived from the original on 21 December 2018. Retrieved 23 December 2018.
- ^ "ALS: Amyotrophic Lateral Sclerosis". Muscular Dystrophy Association. 18 December 2015. Archived from the original on 6 August 2018. Retrieved 23 December 2018.
- S2CID 5917354.
- ISBN 978-0824729240.
- PMID 24124634.
- ^ S2CID 3757685.
- ^ Alexander E (20 August 2014). "George Bush delivers possibly the best ALS ice bucket challenge yet". The Independent. Archived from the original on 21 August 2014. Retrieved 20 August 2014.
- S2CID 207581186.
External links
![]() Media related to Amyotrophic lateral sclerosis at Wikimedia Commons
Media related to Amyotrophic lateral sclerosis at Wikimedia Commons
