Angular cheilitis
| Angular cheilitis | |
|---|---|
| Other names | allergies[2] |
| Treatment | Based on cause, barrier cream[2] |
| Frequency | 0.7% of the population[3] |
Angular cheilitis (AC) is inflammation of one or both corners of the mouth.[4][5] Often the corners are red with skin breakdown and crusting.[2] It can also be itchy or painful.[2] The condition can last for days to years.[2] Angular cheilitis is a type of cheilitis (inflammation of the lips).[6]
Angular cheilitis can be caused by
Treatment for angular cheilitis is typically based on the underlying causes along with the use of a
Signs and symptoms
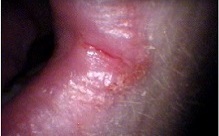

Angular cheilitis is a fairly non specific term which describes the presence of an inflammatory lesion in a particular anatomic site (i.e. the corner of the mouth). As there are different possible causes and contributing factors from one person to the next, the appearance of the lesion is somewhat variable. The lesions are more commonly symmetrically present on both sides of the mouth,
Sometimes contributing factors can be readily seen, such as loss of lower face height from poorly made or worn dentures, which results in mandibular overclosure ("collapse of jaws").
Causes
Angular cheilitis is thought to be a multifactorial disorder of infectious origin,
Infection
The involved organisms are:
- Candida species alone (usually Candida albicans), which accounts for about 20% of cases,[14]
- Bacterial species, either:
- Staphylococcus aureus alone, which accounts for about 20% of cases,[14]
- β-hemolytic streptococci alone. These types of bacteria have been detected in between 8–15% of cases of angular cheilitis,[2] but less commonly are they present in isolation,[10]
- Or a combination of the above organisms, (a polymicrobial infection)[8] with about 60% of cases involving both C. albicans and S. aureus.[14][15]
Candida can be detected in 93% of angular cheilitis lesions.
A lesion caused by recurrence of a latent
Irritation contact dermatitis

22% of cases of angular cheilitis are due to irritants.
Habits or conditions that keep the corners of the mouth moist might include chronic lip licking, thumb sucking (or sucking on other objects such as pens, pipes, lollipops), dental cleaning (e.g. flossing), chewing gum, hypersalivation, drooling and
The sunscreen in some types of lip balm degrades over time into an irritant. Using expired lipbalm can initiate mild angular cheilitis, and when the person applies more lipbalm to alleviate the cracking, it only aggravates it. Because of the delayed onset of contact dermatitis and the recovery period lasting days to weeks, people typically do not make the connection between the causative agent and the symptoms.[medical citation needed]
Nutritional deficiencies
Several different
In general, these nutritional disorders may be caused by
Systemic disorders
Some systemic disorders are involved in angular cheilitis by virtue of their association with malabsorption and the creation of nutritional deficiencies described above. Such examples include people with
Drugs
Several drugs may cause AC as a side effect, by various mechanisms, such as creating drug-induced xerostomia. Various examples include isotretinoin, indinavir, and sorafenib.[5] Isotretinoin (Accutane), an analog of vitamin A, is a medication which dries the skin. Less commonly, angular cheilitis is associated with primary hypervitaminosis A,[20] which can occur when large amounts of liver (including cod liver oil and other fish oils) are regularly consumed or as a result from an excess intake of vitamin A in the form of vitamin supplements. Recreational drug users may develop AC. Examples include cocaine, methamphetamine, heroin, and hallucinogens.[5]
Allergic contact dermatitis
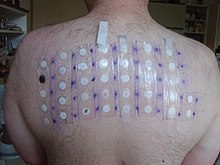
Allergic reactions may account for about 25–34% of cases of generalized cheilitis (i.e., inflammation not confined to the angles of the mouth). It is unknown how frequently allergic reactions are responsible for cases of angular cheilitis, but any substance capable of causing generalized allergic cheilitis may present involving the corners of the mouth alone.[citation needed]
Examples of potential allergens include substances that may be present in some types of lipstick, toothpaste, acne products, cosmetics, chewing gum, mouthwash, foods, dental appliances, and materials from dentures or mercury containing amalgam fillings.[2] It is usually impossible to tell the difference between irritant contact dermatitis and allergic contact dermatitis without a patch test.[citation needed]
Loss of lower facial height
Severe tooth wear or ill fitting dentures may cause wrinkling at the corners of the lip that creates a favorable environment for the condition.[21] This can be corrected with onlays or crowns on the worn teeth to restore height or new dentures with "taller" teeth. The loss of vertical dimension has been associated with angular cheilitis in older individuals with an increase in facial laxity.[22]
Diagnosis
Angular cheilitis is normally a diagnosis made clinically. If the sore is unilateral, rather than bilateral, this suggests a local factor (e.g., trauma) or a split
The lesions are normally swabbed to detect if
Classification
Angular cheilitis could be considered to be a type of cheilitis or
Management
There are four aspects to the treatment of angular cheilitis.[24] Firstly, potential reservoirs of infection inside the mouth are identified and treated.[24] Oral candidiasis, especially denture-related stomatitis is often found to be present where there is angular cheilitis, and if it is not treated, the sores at the corners of the mouth may often recur.[8][13] This involves having dentures properly fitted and disinfected. Commercial preparations are marketed for this purpose, although dentures may be left in dilute (1:10 concentration) household bleach overnight, but only if they are entirely plastic and do not contain any metal parts, and with rinsing under clean water before use.[9] Improved denture hygiene is often required thereafter, including not wearing the denture during sleep and cleaning it daily.[4] For more information, see Denture-related stomatitis.
Secondly, there may be a need to increase the vertical dimension of the lower face to prevent overclosure of the mouth and formation of deep skin folds.
Thirdly, treatment of the infection and inflammation of the lesions themselves is addressed. This is usually with
Finally, if the condition appears resistant to treatment, investigations for underlying causes such as anemia or nutrient deficiencies or HIV infection.[24] Identification of the underlying cause is essential for treating chronic cases. The lesions may resolve when the underlying disease is treated, e.g. with a course of oral iron or B vitamin supplements.[4] Patch testing is recommended by some in cases which are resistant to treatment and where allergic contact dermatitis is suspected.[2]
Prognosis
Most cases of angular cheilitis respond quickly when antifungal treatment is used.[16] In more long standing cases, the severity of the condition often follows a relapsing and remitting course over time.[14] The condition can be difficult to treat and can be prolonged.[4]
Epidemiology
AC is a relatively common condition,[11] accounting for between 0.7 – 3.8% of oral mucosal lesions in adults and between 0.2 – 15.1% in children, though overall it occurs most commonly in adults in the third to sixth decades of life.[2][4] It occurs worldwide, and both males and females are affected.[4] Angular cheilitis is the most common presentation of fungal and bacterial infections of the lips.[14]
Etymology
The term "angular cheilitis" is from Ancient Greek, χείλος meaning lip and -itis meaning inflammation.
References
- ISBN 9780721672649. Archivedfrom the original on 10 September 2017. Retrieved 17 September 2014.
Angular cheilosis: The lateral lip fissures, well known among denture wearers, have been called by a variety of names, such as "rhagades", "perleche", "angular cheilitis", and "angular cheilosis".
- ^ PMID 21838086.
- ^ ISBN 9780826136442. Archivedfrom the original on 2016-08-16.
- ^ ISBN 9780443068188.
- ^ PMID 21877503. Archived from the original(PDF) on 2014-04-19.
- ISBN 9780199687817. Archivedfrom the original on 2016-08-16.
- ^ ISBN 978-0815194323.
- ^ ISBN 9780443068966.
- ^ ISBN 978-1-60327-519-4.
- ^ ISBN 978-0192628947.
- ^ ISBN 978-0192631473.
- ^ MedlinePlus (2005-08-01). "Riboflavin (vitamin B2) deficiency (ariboflavinosis)". National Institutes of Health. Archived from the original on 2010-07-24.
- ^ ISBN 978-0-7817-9378-0. Archivedfrom the original on 2017-09-10.
- ^ ISBN 978-0721690032.
- ISBN 9780199204830.
- ^ ISBN 978-1550091861.
- ^ Gibson, Lawrence E., M.D., "Dry Skin" Archived 2009-09-15 at the Wayback Machine, Mayo Clinic
- PMID 3579131.
- ISBN 978-1-4051-6911-0.
- ^ Kliegman: Nelson Textbook of Pediatrics, 18th ed.
- PMC 1949217.
- ^ "How Do I Manage a Patient with Angular Cheilitis? | jcda". www.jcda.ca. Retrieved 8 June 2018.
- ISBN 9781439863350. Archivedfrom the original on 10 September 2017. Retrieved 17 September 2014.
- ^ ISBN 978-0702041679.
