Arteriovenous malformation
| Arteriovenous malformation | |
|---|---|
| Other names | AVM |
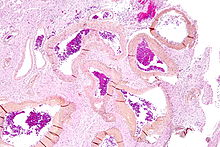 | |
| Micrograph of an arteriovenous malformation in the brain. HPS stain. | |
| Specialty | Neurosurgery |
| Diagnostic method | CT, MRI, MRA |
An arteriovenous malformation (AVM) is an abnormal connection between
Signs and symptoms
Symptoms of AVMs vary according to their location. Most
The most general symptoms of a
- Difficulties with movement coordination, including muscle weakness and even paralysis;
- Vertigo (dizziness);
- Difficulties of speech (dysarthria) and communication, such as aphasia;
- Difficulties with everyday activities, such as apraxia;
- Abnormal sensations (numbness, tingling, or spontaneous pain);
- Memory and thought-related problems, such as confusion, dementia, or hallucinations.
Cerebral AVMs may present themselves in a number of different ways:[citation needed]
- Bleeding (45% of cases)
- "parkinsonism" 4 symptoms in Parkinson's disease.
- Acute onset of severe headache. May be described as the worst headache of the patient's life. Depending on the location of bleeding, may be associated with new fixed neurologic deficit. In unruptured brain AVMs, the risk of spontaneous bleeding may be as low as 1% per year. After a first rupture, the annual bleeding risk may increase to more than 5%.[3]
- Seizure or brain seizure (46%). Depending on the place of the AVM, it can contribute to loss of vision.
- Headache (34%)
- Progressive neurologic deficit (21%)
- May be caused by mass effect or venous dilatations. Presence and nature of the deficit depend on location of lesion and the draining veins.[4]
- Pediatric patients
- Heart failure
- Macrocephaly
- Prominent scalp veins
Pulmonary arteriovenous malformations
Pulmonary arteriovenous malformations are abnormal communications between the veins and arteries of the pulmonary circulation, leading to a right-to-left blood shunt.[5][6]
They have no symptoms in up to 29% of all cases,
Genetics
AVMs are usually
The anomaly can occur due to autosomal dominant diseases, such as hereditary hemorrhagic telangiectasia.[8]
Pathophysiology
In the
As an AVM lacks the dampening effect of capillaries on the blood flow, the AVM can get progressively larger over time as the amount of blood flowing through it increases, forcing the heart to work harder to keep up with the extra blood flow. It also causes the surrounding area to be deprived of the functions of the capillaries. The resulting tangle of blood vessels, often called a nidus (Latin for 'nest'), has no capillaries. It can be extremely fragile and prone to bleeding because of the abnormally direct connections between high-pressure arteries and low-pressure veins.[11] One indicator is a pulsing 'whoosh' sound caused by rapid blood flow through arteries and veins, which has been given the term bruit (French for 'noise'). If the AVM is severe, this may produce an audible symptom which can interfere with hearing and sleep as well as cause psychological distress.[1]
Diagnosis


AVMs are diagnosed primarily by the following imaging methods:[12]
- CT angiography involves the injection of contrastinto the blood stream to view the arteries of the brain. This type of test provides the best pictures of blood vessels through angiography and soft tissues through CT.
- Magnetic resonance imaging (MRI) scan is a noninvasive test, which uses a magnetic field and radio-frequency waves to give a detailed view of the soft tissues of the brain.
- Magnetic resonance angiography (MRA) – scans created using magnetic resonance imaging to specifically image the blood vessels and structures of the brain. A magnetic resonance angiogram can be an invasive procedure, involving the introduction of contrast dyes (e.g., gadolinium MR contrast agents) into the vasculature (circulatory system) of a patient using a catheter inserted into an artery and passed through the blood vessels to the brain. Once the catheter is in place, the contrast dye is injected into the bloodstream and the MR images are taken. Additionally or alternatively, flow-dependent or other contrast-free magnetic resonance imaging techniques can be used to determine the location and other properties of the vasculature.
AVMs can occur in various parts of the body:
- brain (cerebral AV malformation)
- spleen[13]
- kidney[16]
- spinal cord[17]
- liver[18]
- intercostal space[19]
- iris[20]
- spermatic cord[21]
- extremities – arm, shoulder, etc.
AVMs may occur in isolation or as a part of another disease (for example,
AVMs have been shown to be associated with aortic stenosis.[23]
Bleeding from an AVM can be relatively mild or devastating. It can cause severe and less often fatal strokes.[citation needed]
Treatment
Treatment for AVMs in the brain can be symptomatic, and patients should be followed by a neurologist for any seizures, headaches, or focal neurologic deficits. AVM-specific treatment may also involve endovascular embolization, neurosurgery or radiosurgery.[1]
Embolization, that is, cutting off the blood supply to the AVM with coils, particles, acrylates, or polymers introduced by a radiographically guided catheter, may be used in addition to neurosurgery or radiosurgery, but is rarely successful in isolation except in smaller AVMs.
If a cerebral AVM is detected before a stroke occurs, usually the arteries feeding blood into the nidus can be closed off to avert the danger.[26] Interventional therapy may be relatively risky in the short term.[27]
Treatment of lung AVMs is typically performed with endovascular embolization alone, which is considered the standard of care.[15]
Epidemiology
The estimated detection rate of AVM in the US general population is 1.4/100,000 per year.[28] This is approximately one-fifth to one-seventh the incidence of intracranial aneurysms. An estimated 300,000 Americans have AVMs, of whom 12% (approximately 36,000) will exhibit symptoms of greatly varying severity.[1]
History
Hubert von Luschka (1820–1875) and Rudolf Virchow (1821–1902) first described arteriovenous malformations in the mid-1800s. Herbert Olivecrona (1891–1980) performed the first surgical excision of an intracranial AVM in 1932.
Society and culture
Notable cases
- Actor Ricardo Montalbán was born with spinal AVM.[29] During the filming of the 1951 film Across the Wide Missouri, Montalbán was thrown from his horse, knocked unconscious, and trampled by another horse which aggravated his AVM and resulted in a painful back injury that never healed. The pain increased as he aged, and in 1993, Montalbán underwent 9+1⁄2 hours of spinal surgery which left him paralyzed below the waist and using a wheelchair.[30]
- Composer and lyricist Tony Award for best musical, awarded to "Falsettos".[31] Finn wrote the 1998 Off-Broadway musical A New Brainabout the experience.
- AJ Price nearly died from AVM in 2004 while a student at the University of Connecticut.
- On December 13, 2006, Senator Tim Johnson of South Dakota was diagnosed with AVM and treated at George Washington University Hospital.[32]
- Actor/comedian T. J. Miller was diagnosed with AVM in 2010; Miller had a seizure and was unable to sleep for a period. He successfully underwent surgery that had a mortality rate of 10%.[33]
- On August 3, 2011, Mike Patterson of the Philadelphia Eagles collapsed on the field and had a seizure during a practice, leading to him being diagnosed with AVM.[34]
- Former Florida Gators and Oakland Raiders linebacker Florida, but recovered and was cleared to play. On September 16, 2018, Ball was placed in a medically induced coma due to complications of the disease, which lasted until his death on September 10, 2019.[35]
- Indonesian actress Egidia Savitri died from complications of AVM on November 29, 2013.[36]
- Jazz guitarist
- YouTube vlogger 2016 season of Junior Bake Off was born with AVM, which has resulted in some facial disfigurement.[38]
- Country music singer Drake White was diagnosed with AVM in January 2019, and is undergoing treatment.
Cultural depictions
- In the HBO series Nate Fisherdiscovers he has an AVM after being in a car accident and getting a precautionary cat scan at the hospital during Season 1. His AVM becomes a key focus during Season 2 and again in Season 5.
- In season 1 episode 9 of House (2004), titled "DNR", a jazz musician has an AVM and is misdiagnosed with ALS. Two season three episodes also involve AVM - "Top Secret" (episode 16), in which a veteran who believes himself to be suffering from Gulf War syndrome is found to have spinal and pulmonary AVM from hereditary hemorrhagic telangiectasia; and "Resignation" (episode 22), where the patient developed AVM in her intestines after drinking pipe cleaner fluid in a suicide attempt.
- In the 2005 Lifetime film Dawn Anna, the titular character learns she has AVM, and undergoes a serious operation and subsequent rehabilitation, which she recovers from.
See also
References
- ^ a b c d e Arteriovenous Malformation Information Page at NINDS
- Johns Hopkins Medicine. Retrieved October 26, 2022.
- S2CID 22004276.
- PMID 19729171.
- ^ S2CID 22394114.
- ^ S2CID 53144651.
- ISBN 978-0-07-145739-2.
- ^ "Hereditary hemorrhagic telangiectasia: MedlinePlus Genetics". medlineplus.gov. Retrieved July 23, 2022.
- ^ "Circulatory System: Anatomy and Function". Cleveland Clinic. September 21, 2021. Retrieved March 8, 2023.
- ^ PMID 34445743.
- PMID 25407267.
- PMID 24287392. Retrieved February 11, 2023.
- PMID 17145440.
- PMID 18294908.
- ^ S2CID 201675132.
- S2CID 9335750.
- PMID 15730991.
- PMID 7650340.
- PMID 17056881.
- PMID 16534057.
- PMID 17939869.
- NIH. February 22, 2024. Retrieved March 30, 2024.
- PMID 12912718.
- PMID 8416244.
- ^ "Conditions We Treat". Macquarie University Hospital. Archived from the original on June 13, 2013.
- ^ "Arteriovenous Malformations". Neurosurgery. Retrieved June 26, 2023.
- ^ "A Randomized Trial of Unruptured Brain Arteriovenous Malformations (ARUBA)". National Institute of Neurological Disorders and Stroke. January 29, 2014. Archived from the original on July 4, 2016. Retrieved March 6, 2023.
- PMID 12690217.
- ^ "Ricardo Montalban tribute" YouTube, acceptance speech video of Easter Seals Lifetime Achievement Award
- ^ "Inside". mahalo.com. Retrieved March 17, 2018.
- ^ Pall, Ellen (June 14, 1998). "The Long-Running Musical of William Finn's Life". The New York Times. Retrieved March 17, 2018.
- ^ "Sen. Johnson recovering after brain surgery". AP. December 14, 2006.
- You Made It Weird #2: TJ Miller (Podcast). Nerdist Industries. Event occurs at 37:45. Archived from the originalon February 12, 2013. Retrieved December 5, 2012.
- ^ "Mike Patterson's Collapse Reportedly Related To Brain AVM". sbnation.com. August 4, 2011. Retrieved March 17, 2018.
- ^ "Neiron Ball, former Raiders LB, in medically induced coma after aneurysm". ESPN. September 26, 2018.
- ^ Suhendra, Ichsan. "Pesinetron Egidia Savitri Telah Pergi". KOMPAS.com (in Indonesian). Kompas Cyber Media. Retrieved May 15, 2019.
- ^ Vida, Vendela. Confidence, or the Appearance of Confidence: The Best of the Believer Music Interviews. No ed. San Francisco, CA: Believer, a Tiny Division of McSweeney's Which Is Also Tiny, 2014. Print.
- BBC Media Centre. BBC Online. November 25, 2016. Retrieved April 9, 2017.
