Lichen sclerosus
| Lichen sclerosus | |
|---|---|
| Other names | Balanitis xerotica obliterans, lichen sclerosus et atrophicus,[1] Lichen sclerosis et atrophicus,[2] lichen plan atrophique, lichen plan scléreux, Kartenblattförmige Sklerodermie, Weissflecken Dermatose, lichen albus, lichen planus sclerosus et atrophicus, dermatitis lichenoides chronica atrophicans, kraurosis vulvae[3] |
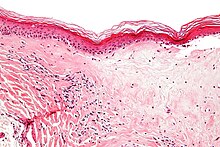 | |
| Micrograph of lichen sclerosus showing the characteristic subepithelial sclerosus (right/bottom of image). H&E stain. | |
| Specialty | Gynaecology |
Lichen sclerosus (LS) is a chronic, inflammatory skin disease of unknown cause which can affect any body part of any person but has a strong preference for the genitals (penis, vulva) and is also known as balanitis xerotica obliterans (BXO) when it affects the penis. Lichen sclerosus is not contagious. There is a well-documented increase of skin cancer risk in LS, potentially improvable with treatment. LS in adult age women is normally incurable, but improvable with treatment, and often gets progressively worse if not treated properly. Most males with mild or intermediate disease restricted to foreskin or glans can be cured by either medical or surgical treatment.[4]
Signs and symptoms
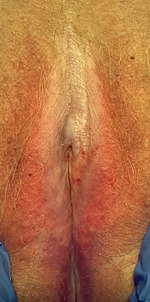

LS can occur without symptoms. White patches on the LS body area, itching, pain, dyspareunia (in genital LS), easier bruising, cracking, tearing and peeling, and hyperkeratosis are common symptoms in both men and women. In women, the condition most commonly occurs on the vulva and around the anus with ivory-white elevations that may be flat and glistening.[citation needed]
In males, the disease may take the form of whitish patches on the foreskin and its narrowing (preputial stenosis), forming an "indurated ring", which can make retraction more difficult or impossible (phimosis). In addition there can be lesions, white patches or reddening on the glans. In contrast to women, anal involvement is less frequent. Meatal stenosis, making it more difficult or even impossible to urinate, may also occur.[citation needed]
On the non-genital skin, the disease may manifest as porcelain-white spots with small visible plugs inside the orifices of
Psychological effect
Distress due to the discomfort and pain of lichen sclerosus is normal, as are concerns with self-esteem and sex. Counseling can help.[citation needed]
According to the National Vulvodynia Association, which also supports women with lichen sclerosus, vulvo-vaginal conditions can cause feelings of isolation, hopelessness, low self-image, and much more. Some women are unable to continue working or have sexual relations and may be limited in other physical activities.[6][7] Depression, anxiety, and even anger are all normal responses to the ongoing pain LS patients experience.
Pathophysiology
Although it is not clear what causes LS, several theories have been postulated. Lichen sclerosus is not contagious; it cannot be caught from another person.[8]
Several risk factors have been proposed, including
Genetic
Lichen sclerosus may have a genetic component. A high correlation of lichen sclerosus has been reported between twins[12][13] and between family members.[14]
Autoimmunity
Infection
Both
are also suspected.A link with Lyme disease is shown by the presence of Borrelia burgdorferi in LSA biopsy tissue.[19]
Hormones
Since LS in females is primarily found in women with a low estrogen state (prepubertal and postmenopausal women), hormonal influences were postulated. To date though, very little evidence has been found to support this theory.[citation needed]
Local skin changes
Some findings suggest that LS can be initiated through scarring[20] or radiation,[21][22] although these findings were sporadic and very uncommon.[citation needed]
Diagnosis

The disease often goes undiagnosed for several years, as it is sometimes not recognized and misdiagnosed as thrush or other problems and not correctly diagnosed until the patient is referred to a specialist when the problem does not clear up.[citation needed]
A biopsy of the affected skin can be done to confirm diagnosis. When a biopsy is done, hyperkeratosis, atrophic epidermis, sclerosis of dermis and lymphocyte activity in dermis are histological findings associated with LS.[24] The biopsies are also checked for signs of dysplasia.[25]
It has been noted that clinical diagnosis of BXO can be "almost unmistakable," though there are other dermatologic conditions such as lichen planus, localized scleroderma, leukoplakia, vitiligo, and the cutaneous rash of Lyme disease can have a similar appearance.[26]
Treatment
Main treatment
There is no definitive cure for LS.[27] Behavior change is part of treatment. The patient should minimize or preferably stop scratching LS-affected skin.[28] Any scratching, stress or damage to the skin can worsen the disease. Scratching has been theorized to increase cancer risks.[29] Furthermore, the patient should wear comfortable clothes and avoid tight clothing, as it is a major factor in the severity of symptoms in some cases.[29][30]
Topically applied corticosteroids to the LS-affected skin are the first-line treatment for lichen sclerosus in women and men, with strong evidence showing that they are "safe and effective" when appropriately applied, even over long courses of treatment, rarely causing serious adverse effects.
Continuous usage of appropriate doses of topical corticosteroids is required to ensure symptoms stay relieved over the patient's life time. If continuously used, corticosteroids have been suggested to minimize the risk of cancer in various studies. In a prospective longitudinal cohort study of 507 women throughout 6 years, cancer occurred for 4.7% of patients who were only "partially compliant" with corticosteroid treatment, while it occurred in 0% of cases where they were "fully compliant".[41] In a second study, of 129 patients, cancer occurred in 11% of patients, none of which were fully compliant with corticosteroid treatment.[37] Both these studies however also said that a corticosteroid as powerful as clobetasol is not necessary in most cases. In a prospective study of 83 patients, throughout 20 years, 8 patients developed cancer. 6 already had cancer at presentation and had not had treatment, while the other 2 were not taking corticosteroids often enough.[36] In all three studies, every single cancer case observed occurred in patients who were not taking corticosteroids as often as the study recommended.[citation needed]
Continuous, abundant usage of emollients topically applied to the LS-affected skin is recommended to improve symptoms. They can supplement but not replace corticosteroid therapy.[32][34][42] They can be used much more frequently than corticosteroids due to the extreme rarity of serious adverse effects. Appropriate lubrication should be used every time before and during sex in genital LS in order to avoid pain and worsening the disease.[43] Some oils such as olive oil and coconut oil can be used to accomplish both the emollient and sexual lubrication function.[citation needed]
In males, it has been reported that circumcision can have positive effects, but does not necessarily prevent further flares of the disease[44] and does not protect against the possibility of cancer.[45] Circumcision does not prevent or cure LS; in fact, "balanitis xerotica obliterans" in men was first reported as a condition affecting a set of circumcised men, by Stühmer in 1928.[3]
Other treatments
Platelet-rich plasma was reported to be effective in one study, producing large improvements in the patients' quality of life, with an average IGA improvement of 2.04 and DLQI improvement of 7.73.[47]
Prognosis
The disease can last for a considerably long time. Occasionally, "spontaneous cure" may ensue,[48] particularly in young girls.
Lichen sclerosus is associated with a higher risk of cancer.
Epidemiology
There is a bimodal age distribution in the incidence of LS in women. It occurs in females with an average age of diagnosis of 7.6 years in girls and 60 years old in women. The average age of diagnosis in boys is 9–11 years old.[59]
In men, the most common age of incidence is 21–30.[60]
History
In 1875, Weir reported what was possible vulvar or oral LS as "ichthyosis." In 1885, Breisky described kraurosis vulvae. In 1887, Hallopeau described a series of extragenital cases of LS. In 1892, Darier formally described the classic histopathology of LS. In 1900 the concept was formed that scleroderma and LS are closely related, which continues to this day. In 1901, pediatric LS was described. From 1913 to present, the concept that scleroderma is not closely related to LS also was formed. In 1920, Taussig established vulvectomy as the treatment of choice for kraurosis vulvae, a premalignant condition. In 1927, Kyrle defined LS ("white spot disease") as an entity sui generis. In 1928, Stühmer described balanitis xerotica obliterans as a postcircumcision phenomenon. In 1936, retinoids (vitamin A) were used in LS. In 1945, testosterone was used in genital LS. In 1961, the use of corticosteroids started. Jeffcoate presented an argument against vulvectomy for simple LS. In 1971, progesterone was used in LS. Wallace defined clinical factors and the epidemiology of LS. In 1976, Friedrich defined LS as a dystrophic, not an atrophic condition; "et atrophicus" was dropped. The
Lichen sclerosus et atrophicus was first described in 1887 by
See also
- Lichen planus
- List of cutaneous conditions
- List of cutaneous conditions associated with increased risk of nonmelanoma skin cancer
- List of human leukocyte antigen alleles associated with cutaneous conditions
References
- ISBN 0-7216-2921-0.
- ^ "Lichen sclerosus". Autoimmune Registry Inc. Retrieved 14 June 2022.
- ^ PMID 7868709.
- ^ European Dermatology Forum Guideline on Lichen Sclerosus (2014)
- PMID 14867888.
- ^ National Vulvodynia Association. "Vulvodynia Fact Sheet". Vulvodynia Media Corner. National Vulvodynia Association. Retrieved 16 June 2012.
- S2CID 204775452.
- ^ National Institute of Health. "Fast Facts About Lichen Sclerosus". Lichen Sclerosus. National Institute of Arthritis and Musculoskeletal and Skin Diseases. Archived from the original on 15 June 2012. Retrieved 16 June 2012.
- S2CID 21471620.
- PMID 15819407.
- PMID 17286064.
- S2CID 11142666.
- S2CID 40455781.
- S2CID 1358288.
- S2CID 37200022.
- PMID 28492056.
- S2CID 10110510.
- S2CID 9261207.
- PMID 18490585.
- PMID 6723373.
- PMID 3208439.
- PMID 4026344.
- ISSN 2081-9390.
- "Figures - available via license: CC BY 4.0" - ^ Lichen Sclerosus et Atrophicus at eMedicine
- S2CID 27778016.
- S2CID 32219826.
- PMID 22483994.
- PMID 18448767.
- ^ PMID 11240748.
- S2CID 29331610.
- S2CID 44975544.
- ^ PMID 10328191.
- PMID 10071317.
- ^ S2CID 16634027.
- S2CID 31834145.
- ^ PMID 15210462.
- ^ S2CID 43273940.
- PMID 24049806.
- PMID 22951124.
- ^ PMID 22161424.
- PMID 26070005.
- PMID 23329078.
- S2CID 22448081.
- S2CID 3416734.
- S2CID 24738069.
- S2CID 36979154.
- S2CID 11499796.
- S2CID 205677253.
- PMID 10570372.
- S2CID 23716949.
- PMID 16515998.
- PMID 37697418.
- PMID 29898214.
- PMID 18406622.
- S2CID 24203150.
- PMID 27223861.
- PMID 28124469.
- PMID 16831147.
- PMID 23329078.
- S2CID 45454913.
- ^ Hallopeau, H (1887). "Du lichen plan et particulièrement de sa forme atrophique: lichen plan scléreux". Annales de Dermatologie et de Syphiligraphie (8): 790–791.
- PMID 135083.
External links
- NIAMS – Questions and Answers About Lichen Sclerosus
- NIAMS – Fast Facts About Lichen Sclerosus
- dermnetnz.org
- better medicine
- Medscape Reference Author: Jeffrey Meffert, MD; Chief Editor: Dirk M Elston, MD
Medical pictures
