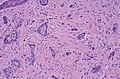
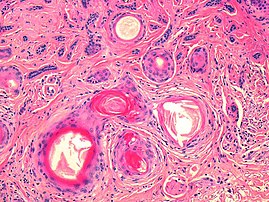
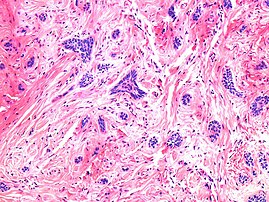
Basal-cell carcinoma
| Basal-cell carcinoma | |
|---|---|
| Other names | Basal-cell skin cancer, basalioma, rodent ulcer |
| Treatment | Surgical removal[2] |
| Prognosis | Good[5] |
| Frequency | ~30% of white people at some point (US)[2] |
| Deaths | Rare[6] |
Basal-cell carcinoma (BCC), also known as basal-cell cancer, basalioma[7] or rodent ulcer,[8] is the most common type of skin cancer.[2] It often appears as a painless raised area of skin, which may be shiny with small blood vessels running over it.[1] It may also present as a raised area with ulceration.[1] Basal-cell cancer grows slowly and can damage the tissue around it, but it is unlikely to spread to distant areas or result in death.[9]
Risk factors include exposure to
It remains unclear whether
Basal-cell cancer accounts for at least 32% of all cancers globally.[9][13] Of skin cancers other than melanoma, about 80% are basal-cell cancers.[2] In the United States, about 35% of white males and 25% of white females are affected by BCC at some point in their lives.[2]
Basal-cell carcinoma is named after the
Signs and symptoms
Individuals with a basal-cell carcinoma typically present with a shiny, pearly skin
-
Basal cell carcinoma on patient's back
-
Basal-cell carcinoma
-
Basal cell carcinoma on the left upper back, nodular and micronodular, marked for biopsy
-
Dermoscopy showing telangiectatic vessels
Cause
The majority of basal-cell carcinomas occur on sun-exposed areas of the body.[15]
Pathophysiology
Basal-cell carcinoma is named after the
Overexposure to sun leads to the formation of
Basal-cell carcinomas can often come in association with other lesions of the skin, such as actinic keratosis, seborrheic keratosis, and squamous cell carcinoma.[21] In a small proportion of cases, basal-cell carcinoma also develops as a result of basal-cell nevus syndrome, or Gorlin Syndrome, which is also characterized by keratocystic odontogenic tumors of the jaw, palmar or plantar (sole of the foot) pits, calcification of the falx cerebri (in the center line of the brain) and rib abnormalities. The cause of this syndrome is a mutation in the PTCH1 tumor suppressor gene located in chromosome 9q22.3, which inhibits the hedgehog signaling pathway. A mutation in the SMO gene, which is also on the hedgehog pathway, also causes basal-cell carcinoma.[22]
Diagnosis

To diagnose basal-cell carcinomas, a
Characteristics

Basal-cell carcinoma cells appear similar to epidermal basal cells, and are usually well differentiated.[25]
In uncertain cases,
Main classes
Basal-cell carcinoma can broadly be divided into three groups, based on the growth patterns.
- Superficial basal-cell carcinoma, formerly referred to in-situ basal-cell carcinoma, is characterized by a superficial proliferation of neoplastic basal-cells. This tumor is generally responsive to topic chemotherapy, such as imiquimod, or fluorouracil, although surgical treatment is better able to ensure complete removal and confirm that there is not an underlying more aggressive subtype that was not sampled in the initial biopsy.
- Infiltrative basal-cell carcinoma, which also encompasses morpheaform and micronodular basal-cell cancer, is more difficult to treat with conservative methods, given its tendency to penetrate into deeper layers of the skin.
- Nodular basal-cell carcinoma includes most of the remaining categories of basal-cell cancer. It is not unusual to encounter heterogeneous morphologic features within the same tumor.
Nodular basal-cell carcinoma

Nodular basal-cell carcinoma (also known as "classic basal-cell carcinoma") accounts for 50% of all BCC.[27] It most commonly occurs on the sun-exposed areas of the head and neck.[28]: 748 [29]: 646 Histopathology shows aggregates of basaloid cells with well-defined borders, showing a peripheral palisading of cells and one or more typical clefts.[27] Such clefts are caused by shrinkage of mucin during tissue fixation and staining.[30] Central necrosis with eosinophilic, granular features may be also present, as well as mucin. The heavy aggregates of mucin determine a cystic structure. Calcification may be also present, especially in long-standing lesions.[27] Mitotic activity is usually not so evident, but a high mitotic rate may be present in more aggressive lesions.[27] Adenoidal BCC can be classified as a variant of NBCC, characterized by basaloid cells with a reticulated configuration extending into the dermis.[27]
-
Cleft.
Other subtypes
Other more specific subtypes of basal-cell carcinoma include:[28][29]: 646–50
| Type | Histopathology | Other characteristics | Image |
|---|---|---|---|
| Cystic basal-cell carcinoma | Morphologically characterized by dome-shaped, blue-gray cystic nodules.[29]: 647 | 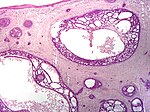
| |
| Morpheaform basal-cell carcinoma (also known as "cicatricial basal-cell carcinoma", and "morphoeic basal-cell carcinoma") | Narrow strands and nests of basaloid cells, surrounded by dense sclerotic stroma.[31] | Aggressive[28]: 748 [29]: 647 | 
|
| Infiltrative basal-cell carcinoma | Deep infiltration.[29]: 647 | Aggressive[29]: 647 | |
| Micronodular basal-cell carcinoma | Small and closely spaced nests. | 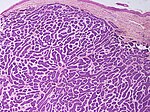
| |
| Superficial basal-cell carcinoma (also known as "superficial multicentric basal-cell carcinoma") | Occurs most commonly on the trunk and appears as an : 647 | 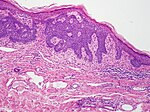
| |
| Pigmented basal-cell carcinoma exhibits increased melanization.[28]: 748 [29]: 647 | About 80% of all basal-cell carcinoma in Chinese are pigmented while this subtype is uncommon in white people. [citation needed] | ||
| Jacob's ulcer | Nodular, with central necrosis.[28]: 748 [29]: 647 | Generally a large : 647 | |
| Fibroepithelioma of Pinkus | Anastomosing epithelial strands in a fenestrated pattern[32] | Most commonly occurs on the lower back.[28]: 748 [29]: 648 | 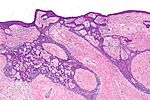
|
| Polypoid basal-cell carcinoma | Exophytic nodules (polyp-like structures) | Generally on head and neck.[29]: 648 | |
| Pore-like basal-cell carcinoma | Resembles an enlarged pore or stellate pit.[29]: 648 | ||
| Aberrant basal-cell carcinoma | Absence of any apparent carcinogenic factor, and occurring in odd sites such as the scrotum, vulva, perineum, nipple, and axilla.[29]: 648 |
Aggressiveness patterns
There are mainly three patterns of aggressiveness, based mainly the cohesion of cancer cells:[33]
| Low-level aggressive pattern | Moderately aggressive pattern | Highly aggressive pattern |
|---|---|---|
|
|
|
Differential diagnoses
| Differential diagnosis | Pathological Features | Image |
|---|---|---|
Hair follicles
|
Peripheral sections may look like nests, but do not display atypia, nuclei are smaller, and serial sections will reveal the rest of the hair follicle. | 
|
Squamous-cell carcinoma of the skin
|
Squamous-cell carcinoma of the skin is generally distinguishable by for example relatively more cytoplasm, horn cyst formation and absence of palisading and cleft formations. Yet, a high prevalence means a relatively high incidence of borderline cases, such as basal-cell carcinoma with squamous cell metaplasia (H&E stain at left in image). BerEP4 staining helps in such cases, staining only basal-cell carcinoma cells (right in image). | 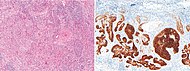
|
| Trichoblastoma | Absence of cleft, rudimentary hair germs, papillary mesenchymal bodies. | 
|
| Adenoid cystic carcinoma | Lack of basaloid cells disposed in peripheral palisades; adenoid-cystic lesion without connection to the epidermis; absence of artefactual clefts | 
|
| Microcystic adnexal carcinoma | Bland keratinocytes, keratin cysts, ductal differentiation. BerEp4- (in 60% of cases),[35] CEA+, EMA+ | |
| Trichoepithelioma[notes 1] | Rims of collagen bundles, calcification, follicular/sebaceous/infundibular differentiation and cut artefacts. Cytokeratin (CK)20+, p75+, Pleckstrin homology-like domain family A member 1 + (PHLDA1+), common acute lymphoblastic leukemiaantigen + (CD10+) in tumor stroma, CK 6-, Ki-67- and Androgen Rceptor- (AR-) | 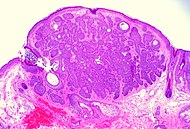
|
Merkel cell carcinoma |
Cells arranged in a diffuse, trabecular and/or nested pattern, involving also the subcutis. Mouse Anti-Cytokeratin (CAM) 5.2+, CK20+, S100-, human leukocyte common antigen- ( LCA-), thyroid transcription factor 1- (TTF1-) | 
|
Radicality

In suspected but uncertain BCC cells close to the resection margins, immunohistochemistry with BerEp4 can highlight the BCC cells.
Prevention
Basal-cell carcinoma is a common skin cancer and occurs mainly in fair-skinned patients with a family history of this cancer. Sunlight is a factor in about two-thirds of these cancers; therefore, doctors recommend
The use of a chemotherapeutic agent such as
Treatment
The following methods are employed in the treatment of basal-cell carcinoma (BCC):
Standard surgical excision

Surgery to remove the basal-cell carcinoma affected area and the surrounding skin is thought to be the most effective treatment.[38] A disadvantage with standard surgical excision is a reported higher recurrence rate of basal-cell cancers of the face,[39] especially around the eyelids,[40] nose, and facial structures.[41] There is no clear approach, nor a clear research comparing the effectiveness of Mohs micrographic surgery versus surgical excision for BCC of the eye.[42]
For basal cell carcinoma excisions on the lower lip the wound can be covered with a keystone flap. A keystone flap is achieved by creating a flap below the defect and pulling it superiorly to cover the wound. This can be performed if there is enough skin laxity to cover the defect and adequate blood supply to the flap.[43]
Mohs surgery
For many new (primary) and all recurrent forms of basal cell carcinoma after previous surgery, especially on the head, neck, hands, feet, genitalia and anterior legs (shins), Mohs surgery should be considered.[44][45]
An essential aspect of Mohs surgery is that the Mohs surgeon performs the surgery and personally reviews the Mohs pathology slides.[45] Most standard excisions done in an office setting are sent to an outside laboratory for standard bread loafing method of processing.[47] With this method, it is likely that less than 5% of the surgical margin is examined, as each slice of tissue is only 6 micrometres thick, about 3 to 4 serial slices are obtained per section, and only about 3 to 4 sections are obtained per specimen.[48]
Cryosurgery
Cryosurgery is an old modality for the treatment of many skin cancers. When accurately utilized with a temperature probe and cryotherapy instruments, it can result in very good cure rate. Disadvantages include lack of margin control, tissue necrosis, over or under treatment of the tumor, and long recovery time. Overall, there are sufficient data to consider cryosurgery as a reasonable treatment for BCC. There are no good studies, however, comparing cryosurgery with other modalities, particularly with Mohs surgery, excision, or electrodesiccation and curettage so that no conclusion can be made whether cryosurgery is as efficacious as other methods. Also, there is no evidence on whether curetting the lesions before cryosurgery affects the efficacy of treatment.[49] Several textbooks are published on the therapy, and a few physicians still apply the treatment to selected patients.[50]
Electrodesiccation and curettage
Electrodesiccation and curettage (EDC, also known as curettage and cautery, simply curettage)[51] is accomplished by using a round knife, or curette, to scrape away the soft cancer. The skin is then burned with an electric current. This further softens the skin, allowing for the knife to cut more deeply with the next layer of curettage. The cycle is repeated, with a safety margin of curettage of normal skin around the visible tumor. This cycle is repeated 3 to 5 times, and the free skin margin treated is usually 4 to 6 mm. Cure rate is very much user-dependent and depends also on the size and type of tumor. Infiltrative or morpheaform BCCs can be difficult to eradicate with EDC. Generally, this method is used on cosmetically unimportant areas like the trunk (torso). Some physicians believe that it is acceptable to utilize EDC on the face of elderly patients over the age of 70. However, with increasing life expectancy, such an objective criterion cannot be supported. The cure rate can vary, depending on the aggressiveness of the EDC and the free margin treated. Some advocate curettage alone without electrodesiccation, and with the same cure rate.[52]
Chemotherapy
Some superficial cancers respond to local therapy with
Removing the residual superficial tumor with surgery alone can result in large and difficult to repair surgical defects. One often waits a month or more after surgery before starting the immunotherapy or chemotherapy to make sure the surgical wound has adequately healed. Some people[who?] advocate the use of curettage (see EDC below) first, followed by chemotherapy. These experimental procedures are not standard care.[51]
Vismodegib and sonidegib are drugs approved for specially treating BCC, but are expensive and cannot be used in pregnant women.
Itraconazole, traditionally an anti-fungal medication, has also garnered recent attention for its potential use in the treatment of BCC, especially those that cannot be removed surgically. Possessing anti-Hedgehog pathway activity, there is clinical evidence that itraconazole has some efficacy either alone or when combined with vismodegib/sonidegib for primary and recurrent BCC. There is one case report of efficacy in metastatic BCC.[54]
Immunotherapy
This technique uses the body's immune system to kill cancer cells. Improvement of the immune system works its way out up to the cancerous cells and treat the skin cancer.
Topical treatment with 5% Imiquimod cream (IMQ), with five applications per week for six weeks has a reported 70–90% success rate at reducing, even removing, the BCC [basal-cell carcinoma]. Imiquimod has received FDA approval, and topical IMQ is approved by the European Medicines Agency for treatment of small superficial basal-cell carcinoma.[51] Off label use of imiquimod on invasive basal-cell carcinoma has been reported. Imiquimod may be used prior to surgery in order to reduce the size of the carcinoma.
Some advocate the use of imiquimod prior to Mohs surgery to remove the superficial component of the cancer.[55]
Research suggests that treatment using Euphorbia peplus, a common garden weed, may be effective.[56] Australian biopharmaceutical company Peplin[57] is developing this as topical treatment for BCC.
Radiation
Usually, recurrent tumors after radiation are treated with surgery, and not with radiation. Further radiation treatment will further damage normal tissue, and the tumor might be resistant to further radiation. Radiation therapy may be contraindicated for treatment of nevoid basal-cell carcinoma syndrome. A 2008 study reported that radiation therapy is appropriate for primary BCCs and recurrent BCCs, but not for BCCs that have recurred following previous radiation treatment.[51]
Photodynamic therapy
Photodynamic therapy (PDT) is a new modality for treatment of basal-cell carcinoma, which is administered by application of photosensitizers to the target area. When these molecules are activated by light, they become toxic, therefore destroying the target cells. Methyl aminolevulinate is approved by EU as a photosensitizer since 2001. This therapy is also used in other skin cancer types.[59] A 2008 study reported that PDT was a good treatment option for primary superficial BCCs and reasonable for primary low-risk nodular BCCs, but was a "relatively poor" option for high-risk lesions.[51]
Prognosis
Prognosis is excellent if the appropriate method of treatment is used in early primary basal-cell cancers. Recurrent cancers are much harder to cure, with a higher recurrence rate with any methods of treatment. Although basal-cell carcinoma rarely metastasizes, it grows locally with invasion and destruction of local tissues. The cancer can impinge on vital structures like nerves and result in loss of sensation or loss of function or rarely death. The vast majority of cases can be successfully treated before serious complications occur. The recurrence rate for the above treatment options ranges from 50 percent to 1 percent or less.
Epidemiology
Basal-cell cancer is a very common skin cancer. It is much more common in fair-skinned individuals with a family history of basal-cell cancer and increases in incidence closer to the equator or at higher altitude. It is very common among elderly people over the age of 80.[60] There are approximately 800,000[61] new cases yearly in the United States alone. Up to 30% of white people develop basal-cell carcinomas in their lifetime.[62] In Canada, the most common skin cancer is basal-cell carcinoma (as much as one third of all cancer diagnoses), affecting 1 in 7 individuals over a lifetime.[63]
In the United States, approximately 3 out of 10 Caucasian people develop a basal-cell carcinoma during their lifetime.[62] This tumor accounts for approximately 70% of non-melanoma skin cancers. In 80 percent of all cases, basal-cell carcinoma affects head or neck skin.[62]
Most sporadic BCC arises in small numbers on sun-exposed skin of people over age 50, although younger people may also be affected. The development of multiple basal-cell cancer at an early age could be indicative of nevoid basal-cell carcinoma syndrome, also known as Gorlin syndrome.[64]
Notes
- ^ Desmoplastic tricoepithelioma is particularly similar to basal-cell carcinoma.
References
- ^ a b c "Skin Cancer Treatment (PDQ®)". NCI. 2013-10-25. Archived from the original on 5 July 2014. Retrieved 30 June 2014.
- ^ PMID 26476255.
- ^ a b "Skin Cancer Treatment". National Cancer Institute. 21 June 2017. Archived from the original on 4 July 2017. Retrieved 2 July 2017.
- ISBN 978-3-642-12264-4. Archivedfrom the original on 2017-09-10.
- ^ ISBN 978-92-832-0429-9.
- PMID 27733281.
- ^ "Basal Cell Carcinoma". dermnetnz.org. Retrieved 12 November 2023.
- ^ "Basal Cell Carcinoma (Rodent Ulcer or BCC)". Newcastle Hospitals NHS Foundation Trust. 31 October 2022. Retrieved 12 November 2023.
- ^ PMID 23084294.
- ] has increased.
- S2CID 44457153.
- ^ a b "Skin Cancer Treatment". National Cancer Institute. 21 June 2017. Archived from the original on 4 July 2017. Retrieved 2 July 2017.
- PMID 23369588.
- ^ "Basal Cell Carcinoma Warning Signs and Images". The Skin Cancer Foundation. Retrieved 2023-03-02.
- ^ a b "Genetics of Skin Cancer". National Cancer Institute. 2009-07-29. Retrieved 2019-05-06.
- ^ a b "Basal Cell Carcinoma - Skin Disorders". MSD Manual Consumer Version.
- S2CID 234598207.
- PMID 22678003.)
{{cite journal}}: CS1 maint: DOI inactive as of March 2024 (link - S2CID 81618758.
- ISBN 978-1-893357-10-5.
- S2CID 206650583.
- ^ PMID 18216361.
- ^ "What Is Basal Cell Cancer". SkinCancerGuide. Archived from the original on 2009-03-01. Retrieved 2009-02-18.
- PMID 30521689.
- ^ Robert S Bader. "Which histologic findings are characteristic of basal cell carcinoma (BCC)?". Medscape. Updated: Feb 21, 2019
- ^ PMID 29464122.
- ^ PMID 29261131.
- ^ ISBN 0-07-138076-0.
- ^ ISBN 978-0-7216-2921-6.
- ^ Robert S Bader. "Which histologic findings are characteristic of basal cell carcinoma (BCC)?". Medscape. Updated: Feb 21, 2019
- S2CID 44948030.
- PMID 27329375.
- S2CID 43844922.
- PMID 31384511. Creative Commons Attribution License
- PMID 25692080.
- PMID 27455163.
- PMID 29299592.
- PMID 33202063.
- ^ Basal Cell and Squamous Cell Skin Cancers (PDF). NCCN Clinical Practice Guidelines in Oncology. National Comprehensive Cancer Network. 2009. p. 38. Archived from the original (PDF) on 2009-02-27.
- PMID 9716337.
- S2CID 19202086.
- PMID 25503105.
- . 290.6.
- PMID 27160235.
- ^ PMID 22959232.
- ^ PMID 28676157.
- PMID 16125611.
- ISBN 978-0-86542-299-5.
- PMID 12786697.
- ^ "Understanding Actinic Keratosis – Treatment". Web MD. Archived from the original on 2007-08-11. Retrieved 2008-12-05.
- ^ S2CID 12365983.
- PMID 16713459.
- ^ [1] Archived 2009-05-20 at the Wayback Machine
- S2CID 235608763.
- S2CID 45091789.
- ^ "Peplin's skin cancer gel trial a success". The Age. Melbourne. 1 May 2006. Archived from the original on 16 June 2006.
- ^ Peplin Archived June 14, 2008, at the Wayback Machine
- PMID 33140131.
- S2CID 119815301.
- S2CID 8964342.
- ^ Skin Cancer Foundation: Basal-Cell Carcinoma Archived 2006-06-19 at the Wayback Machine
- ^ PMID 14525881.
- ^ "Epidemiology of Skin Cancer". BC Cancer Agency. Archived from the original on 2011-05-14. Retrieved 2011-06-25.
- ISBN 978-3-211-21396-4.








![Fibroepitheliomatous pattern (anastomosing basaloid epithelial strands enclosing round islands of fibrous stroma)[34]](http://upload.wikimedia.org/wikipedia/commons/thumb/f/fc/Micrograph_of_basal-cell_carcinoma_with_fibroepitheliomatous_pattern.jpg/120px-Micrograph_of_basal-cell_carcinoma_with_fibroepitheliomatous_pattern.jpg)