Baylisascaris procyonis
| Baylisascaris procyonis | |
|---|---|
| |
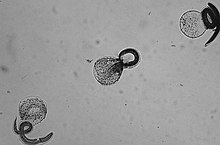
| Freshly hatched B. procyonis larvae | |
| Scientific classification | |
| Domain: | Eukaryota |
| Kingdom: | Animalia |
| Phylum: | Nematoda |
| Class: | Chromadorea |
| Order: | Ascaridida |
| Family: | Ascarididae |
| Genus: | Baylisascaris |
| Species: | B. procyonis
|
| Binomial name | |
| Baylisascaris procyonis (Stefanski & Zarnowski, 1951)
| |
| Synonyms[1] | |
| |
Baylisascaris procyonis, also known by the common name raccoon roundworm, is a
Signs and symptoms
The potential for human infection was noted in 1969 by Paul C. Beaver, who studied infected mice, and the first case was reported 15 years later.
Cause
Transmission
In North America, B. procyonis infection rates in raccoons are very high, being found in around 70% of adult raccoons and 90% of juvenile raccoons.[7] Transmission occurs similarly to other roundworm species, through the fecal-oral route. Eggs are produced by the worm while in the intestine, and the released eggs will mature to an infective state externally in the soil. When an infected egg is ingested, the larvae will hatch and enter the intestine. Transmission of B. procyonis may also occur through the ingestion of larvae found in infected tissue.[7]
Life cycle

An adult worm lives and reproduces in the intestine of its definitive host, the raccoon. The female worm can produce between 115,000–179,000 eggs per day. Eggs are excreted along with feces, and become infective in the soil after 2–4 weeks. If ingested by another raccoon, the life cycle repeats. However, if these eggs are ingested by an intermediate host (small mammals, birds) the larvae of B. procyonis will penetrate the gut wall of the host and migrate into tissues. Larvae tend to migrate to the brain, cause damage, and affect the behaviour of the intermediate host, making it an easier prey for raccoons. Reproduction does not occur in these intermediate hosts; however, if a raccoon preys on an infected paratenic host, the encysted larvae can become adults in the raccoon and the cycle resumes.[3]
Diagnosis
Laboratory and clinical diagnosis can be challenging: there is no commercially available serologic test in the United States, and although identification of larvae in tissue or specimens is confirmatory, this is not always possible or practical.[5]
Diagnosis of B. procyonis is through identification of
Human Baylisascariasis is under-recognized, as the knowledge of the clinical illness is still a bit unclear. This could be because of the difficulty of diagnosing the illness. As small numbers of larvae can cause severe disease, and larvae occur randomly in tissue, a biopsy usually fails to include larvae and therefore leads to negative results. The identification of the morphologic characteristics takes practice and experience and may not be accurately recognized or could be misidentified. The fact that no commercial serologic test exists for the diagnosis of B. procyonis infection makes the diagnosis and treatment more difficult.[7]
Prevention
Educating the public about the dangers of contact with raccoons or their feces is the most important preventive step.[4]
Parents should encourage their children to practice good hygiene; Hand-washing after outdoor play or contact with animals is very important. Fences can be used to prevent raccoons from visiting homes, garbage, or yards for food. Keeping raccoons as pets is strongly discouraged. Raccoon latrines in and around homes should be checked for and cleaned as soon as possible. Boiling water,
Epidemiology
Baylisascaris procyonis is found abundantly in its
The white-footed mouse (Peromyscus leucopus) among other small rodents are considered common intermediate hosts.
Bioterrorism threat
Baylisascaris procyonis has become a concern for its potential use as an agent of bioterrorism. The fact that this parasite's eggs are easy to acquire, able to live for years, extremely resistant to many disinfectants, and cause serious infections in humans with poor treatment options could make it a dangerous weapon.[4] Community water supplies are easily susceptible to contamination due to the lack of filtration and treatment methods to get rid of the eggs.[13]
See also
- List of parasites (human)
References
- ^ "Baylisascaris procyonis (Stefanski & Zarnowski, 1951)". Global Biodiversity Information Facility. Retrieved 24 February 2024.
- PMC 3294543.
- ^ ISBN 978-0-520-25938-6.
- ^ PMID 16223954.
- ^ PMID 27608169.
- ^ PMID 27869612.
- ^ PMID 11971766.
- PMID 28726612.
- ^ Beasley, JC et al., (2013) "Baylisascaris procyonis Infections in White- Footed Mice: Predicting patterns of Infection from landscape Habitat Attributes," Journal of Parasitology, 99(5). , p. 743.
- ^ Beasley, JC et al., (2013). "Baylisascaris procyonis Infections in White- Footed Mice: Predicting patterns of Infection from landscape Habitat Attributes," Journal of Parasitology, 99(5), p. 745.
- ^ "Allegheny Woodrat - NYS Dept. Of Environmental Conservation".
- ^ "Allegheny Woodrat in Alabama". Archived from the original on 2007-12-03. Retrieved 2008-01-14.
- PMID 11971766.
