Behçet's disease
| Behçet's disease | |
|---|---|
| Other names |
|
corticosteroids[1] | |
| Prognosis | Often improves with time[2] |
| Frequency | Rare (US, EU), more common (Middle East, Asia)[2] |
Behçet's disease (BD) is a type of
The cause is unknown.
There is no cure.
While rare in the United States and Europe, it is more common in the Middle East and Asia.[2] In Turkey, for example, about 2 per 1,000 are affected.[2] Onset is usually in a person's twenties or forties.[1][2] The disease was initially described by Turkish dermatologist Hulusi Behçet in 1937.[3]
Signs and symptoms
Skin and mucosa
Nearly all people with Behçet's disease present with some form of painful ulcerations inside the mouth.
Eyes
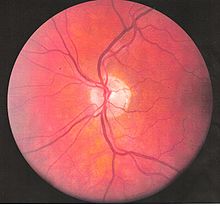
Inflammatory eye disease can develop early in the disease course and lead to permanent vision loss in 20 percent of cases. Ocular involvement can be in the form of
Optic nerve involvement in Behçet's disease is rare, typically presenting as progressive
Signs and symptoms of acute
Episcleritis may occur, which causes eye redness and mild pain, without a significant impact on vision.[10]
Bowels
Gastrointestinal (GI) manifestations include abdominal pain, nausea, and diarrhea with or without blood, and they often involve the terminal ileum and ileocecal valve.[4] Some patients with BD experience abdominal tenderness, bloating, and general abdominal discomfort. When mild this can resemble irritable bowel syndrome; more severe cases bear similarities to inflammatory bowel diseases such as ulcerative colitis or Crohn's. Behçet's disease causes ulcers in the terminal ileum and ileocecal valve. The ulcers may be aphthous or have a classic punched out appearance with undermining. Linear and fissuring ulcers up to 5cm may be present. Biopsies show vasculitis (phlebitis or venulitis) with a neutrophilic inflammatory infiltrate. Involvement of the oesophagus, stomach and large intestine is rare.[citation needed]
Lungs
Lung involvement is typically in the form of
Joints
Arthritis is seen in up to half of people, and is usually a non-erosive poly or oligoarthritis primarily of the large joints of the lower extremities.[4]
Kidneys
Behçet's disease can rarely result in renal involvement. This can manifest in the following:
- Glomerulonephritis
- Renal amyloidosis
- IgA nephropathy
- Vascular disease
- Drug side effects, such as NSAID's (non-steroidal anti-inflammatories), cyclophosphamide, cyclosporine and tacrolimus.
Small vessel vascular disease results in renal vasculitis, whereas large vessel involvement causes aneurysms (bulging) and thrombosis (blockages). Serious kidney problems are more common in men typically with a history of large vessel involvement in other parts of the body. Bladder and urethral involvement is rare in Behçet's disease.
Brain
Central nervous system (CNS) involvement most often occurs as a chronic meningoencephalitis. Lesions tend to occur in the brainstem, the basal ganglia and deep hemispheric white matter and may resemble those of multiple sclerosis (MS). Brainstem atrophy is seen in chronic cases.[citation needed]
Neurological involvements range from
Heart
Chronic aortic regurgitation due to aortic root disease may also be seen.[11] Although infrequent, myocardial infarction (heart attack) with angiographically identified acute coronary artery thrombosis has been reported, including one case with a pathologically demonstrable lesion due to arteritis found at autopsy.[12]
Blood vessels
Blood vessel problems are observed in 7–29% of people with arterial lesions representing 15% of vascular lesions. Arterial lesions pose a greater risk. Most common arterial lesions are occlusions or stenosis and aneurysms or pseudoaneurysms.[13] [citation needed]
Cause
The cause is not well-defined, but it is primarily characterized by auto-inflammation of the blood vessels. Although sometimes erroneously referred to as a diagnosis of exclusion, the diagnosis can sometimes be reached by pathologic examination of the affected areas.[14]
The primary mechanism of the damage is autoimmune, which by definition is an overactive immune system that targets the patient's own body. The involvement of a subset of T cells (
Research suggests that previous infections may provoke the autoimmune responses present in Behçet's disease.
An association with the GIMAP ("GTPase of the immunity-associated protein") family of genes on the long arm of chromosome 7 (7q36.1) has been reported.[18] Gene locations of single-nucleotide polymorphisms associated with Behçet's disease included GIMAP1, GIMAP2 and GIMAP4.[18]
Pathophysiology

Behçet's disease is considered more prevalent in the areas surrounding the old silk trading routes in the Middle East and in Central Asia. Thus, it is sometimes known as Silk Road disease. However, this disease is not restricted to people from these regions. A large number of serological studies show a linkage between the disease and HLA-B51.[20] HLA-B51 is more frequently found from the Middle East to South Eastern Siberia, but the incidence of B51 in some studies was 3 fold higher than the normal population. However, B51 tends not to be found in disease when a certain SUMO4 gene variant is involved,[21] and symptoms appear to be milder when HLA-B27 is present.[22] At the current time, a similar infectious origin has not yet been confirmed that leads to Behçet's disease, but certain strains of S. sanguinis has been found to have a homologous antigenicity.[23]
Vasculitis resulting in occlusion of the vessels supplying the optic nerve may be the cause of acute optic neuropathy and progressive optic atrophy in Behçet's disease. Histological evaluation in a reported case of acute optic neuropathy demonstrated substitution of the axonal portion of the optic nerve with fibrous astrocytes without retinal changes.[8] CNS involvement in Behçet's disease may lead to intracranial hypertension most commonly due to dural venous sinus thrombosis[6] and subsequent secondary optic atrophy.
Diagnosis
There is no specific pathological testing or technique available for the diagnosis of the disease, although the International Study Group criteria for the disease are highly sensitive and specific, involving clinical criteria and a
Visual acuity, or color vision loss with concurrent mucocutaneous lesions or systemic Behçet's disease symptoms should raise suspicion of optic nerve involvement in Behçet's disease and prompt a work-up for Behçet's disease if not previously diagnosed in addition to an ocular work-up. Diagnosis of Behçet's disease is based on clinical findings including oral and genital ulcers, skin lesions such as erythema nodosum, acne, or folliculitis, ocular inflammatory findings and a pathergy reaction. Inflammatory markers such ESR, and CRP may be elevated. A complete ophthalmic examination may include a slit lamp examination, optical coherence tomography to detect nerve loss, visual field examinations, fundoscopic examination to assess optic disc atrophy and retinal disease, fundoscopic angiography, and visual evoked potentials, which may demonstrate increased latency. Optic nerve enhancement may be identified on Magnetic Resonance Imaging (MRI) in some patients with acute optic neuropathy. However, a normal study does not rule out optic neuropathy. Cerebrospinal fluid (CSF) analysis may demonstrate elevated protein level with or without pleocytosis. Imaging including angiography may be indicated to identify dural venous sinus thrombosis as a cause of intracranial hypertension and optic atrophy.[citation needed]
Diagnostic guidelines

According to the International Study Group guidelines, for a patient to be diagnosed with Behçet's disease,
- iritis, uveitis, retinal vasculitis, cells in the vitreous)
- genital ulcers (including anal ulcers and spots in the genital region and swollen testicles or epididymitis in men)
- pathergy reaction (papule >2 mm dia. 24–48 hrs or more after needle-prick). The pathergy test has a specificity of 95 percent to 100 percent, but the results are often negative in American and European patients[4]
- skin lesions (papulo-pustules, folliculitis, erythema nodosum, acne in post-adolescents not on corticosteroids)
Despite the inclusive criteria set forth by the International Study Group, there are cases where not all the criteria can be met and therefore a diagnosis cannot readily be made. There is, however, a set of clinical findings that a physician can rely upon in making a tentative diagnosis of the disease; essentially, Behçet's disease does not always follow the International Study Group guidelines and so a high degree of suspicion for a patient who presents having any number of the following findings is necessary:[citation needed]
- arthritis/arthralgia
- cardio-vascular problems of an inflammatory origin
- changes of psychoses
- deep vein thrombosis
- epididymitis
- extreme exhaustion – chronic fatigue
- inflammatory problems in lungs
- mouth ulcers
- nervous system symptoms
- problems with hearing or balance
- bowelinflammation
- superficial thrombophlebitis
- any other members of the family with a diagnosis of Behçet's disease.
Treatment
Current treatment is aimed at easing the symptoms, reducing inflammation, and controlling the immune system. The quality of the evidence for treating the oral ulcers associated with Behçet's disease, however, is poor.[25]
High-dose corticosteroid therapy is often used for severe disease manifestations.[26] Anti-TNF therapy such as infliximab has shown promise in treating the uveitis associated with the disease.[27][28] Another Anti-TNF agent, etanercept, may be useful in people with mainly skin and mucosal symptoms.[29] Apremilast may also be used to treat oral ulcers associated with Behçet's disease.[30]
Interferon alpha-2a may also be an effective alternative treatment, particularly for the genital and oral ulcers[31] as well as ocular lesions.[32] Azathioprine, when used in combination with interferon alpha-2b also shows promise,[33] and colchicine can be useful for treating some genital ulcers, erythema nodosum, and arthritis.[34] Benzathine‐penicillin may also reduce new arthritic attacks.[35]
Thalidomide has also been used due to its immune-modifying effect.[36] Dapsone and rebamipide have been shown, in small studies, to have beneficial results for mucocutaneous lesions.[37][38]
Given its rarity, the optimal treatment for acute optic neuropathy in Behçet's disease has not been established. Early identification and treatment are essential. Response to
Intravenous immunoglobulin therapy (IVIg) could be a treatment for severe[40] or complicated cases.[41][42]
Surgery
Surgical treatment of arterial manifestations of BD bears many pitfalls since the obliterative endarteritis of vasa vasorum causes thickening of the medial layer and splitting of elastin fibers. Therefore, anastomotic pseudoaneurysms are likely to form, as well as pseudoaneurysms at the site of the puncture in case of angiography or endovascular treatment; furthermore, early graft occlusion may occur.[citation needed]
For these reasons, invasive treatment should not be performed in the acute and active phases of the disease when inflammation is at its peak. The evaluation of disease's activity is usually based on relapsing symptoms, ESR (erythrocyte sedimentation rate), and serum levels of CRP (C‐reactive protein).[citation needed]
Endovascular treatment can be an effective and safe alternative to open surgery, with less postoperative complications, faster recovery time, and reduced need for intensive care, while offering patency rates and procedural success rates comparable with those of surgery. This notwithstanding, long‐term results of endovascular treatment in BD are still to be determined.[citation needed]
Epidemiology
The syndrome is rare in the United States, Africa and South America, but is common in Asia, suggesting a possible cause endemic to those areas.[43] A theory suggested that past exposure to lethal infectious agents might have fixed the genetic susceptibility factors to Behçet's disease in those area.[44] An estimated 15,000 to 20,000 Americans have been diagnosed with this disease. In the UK, it is estimated to have about 1 case for every 100,000 people.[45] Globally, males are affected more frequently than females.[46]
In an epidemiologic study, 56 percent of patients with Behçet's disease developed ocular involvement at a mean age of 30.[47] Ocular involvement was the first manifestation of Behçet's disease in 8.6 percent of patients.[47] Ocular Behçet's disease with involvement of the optic nerve is rarely reported. Among patients with ocular Behçet's disease funduscopic findings of optic atrophy, and optic disc paleness have been identified with a frequency of 17.9 percent and 7.4 percent, respectively. Other fundoscopic findings include vascular sheathing (23.7%),[7] retinal hemorrhage (9%),[7] macular edema (11.3%),[7] branch retinal vein occlusion (5.8%),[7] and retinal edema (6.6%).[7] However, optic atrophy was the most significant cause of visual impairment identified in 54 percent of patients with ocular Behçet's disease and permanent visual impairment.[7]
Pregnancy
With Behçet's disease as a
Behçet's can cause
History
The first modern formal description of the symptoms was made by H. Planner and F. Remenovsky and published in 1922 in the
Some sources use the term "Adamantiades's syndrome" or "Adamantiades–Behçet syndrome", for the work done by Benediktos Adamantiades.[54] However, the current World Health Organization/ICD-10 standard is "Behçet's disease". In 1991, Saudi Arabian medical researchers described neuro-Behçet's disease,[55] a neurological involvement in Behçet's disease, considered one of the most devastating manifestations of the disease.[56] The mechanism can be immune-mediated or thrombotic.[57] The term dates back to at least 1990.[58]
References
- ^ a b c d e f g h i j k l m n o Fleming, Ray (November 2014). "Fast Facts About Behçet's Disease". www.niams.nih.gov. Archived from the original on 13 May 2017. Retrieved 29 May 2017.
- ^ a b c d e f g h i j k l m n o "Behçet's Syndrome". NORD (National Organization for Rare Disorders). 2015. Archived from the original on 11 February 2017. Retrieved 29 May 2017.
- ISBN 9780191667022. Archivedfrom the original on 10 September 2017.
- ^ ISBN 978-1-934465-30-1.
- PMID 21212799.
- ^ PMID 7723211.
- ^ S2CID 13428859.
- ^ PMID 2531168.
- OCLC 1127393738.)
{{cite book}}: CS1 maint: others (link - )
- ISBN 978-1-60913-360-3.
- PMID 7064781.
- PMID 29564347.
- ^ "Behcet Disease: Overview – eMedicine Dermatology". Archived from the original on 16 February 2009. Retrieved 28 March 2009.
- ^ Hatemi G, Seyahi E, Fresko I, Hamuryudan V (2012). "Behçet's syndrome: a critical digest of the recent literature". Clin Exp Rheumatol
- PMID 24490075.
- PMID 10420201.
- ^ S2CID 206848143.
- PMID 6956266.
- S2CID 11695492.
- PMID 18657476.
- PMID 17923546.
- PMID 16514412.
- ^ S2CID 53261546.
- PMID 25254615.
- ^ CMDT (Current Medical Diagnosis & Treatment) 2007, Chapter 20, page 872
- S2CID 23347314.
- PMID 12379622.
- PMID 15630733.
- ^ "Search Orphan Drug Designations and Approvals". www.accessdata.fda.gov. Retrieved 19 November 2019.
- PMID 11939808.
- PMID 12642304.
- PMID 12455182.
- S2CID 19523919.
- PMID 10796413.
- S2CID 12089634.
- S2CID 23711352.
- S2CID 23356719.
- S2CID 45084854.
- PMID 11673289.
- PMID 22727170.
- S2CID 26407172.
- ^ "Behcet's Syndrome: MedlinePlus". nih.gov. Archived from the original on 4 July 2016. Retrieved 19 September 2016.
- PMID 24447390.
- ^ Choices, N. H. S. "Behçet's disease – NHS Choices". www.nhs.uk. Archived from the original on 3 March 2016. Retrieved 19 September 2016.
- PMID 16476027.
- ^ S2CID 23191896.
- ^ S2CID 12860697.
- ^ S2CID 22363654.
- ^ Behçet's disease – Treatment Archived 5 April 2014 at the Wayback Machine from National Health Service. Page last reviewed: 22 August 2012
- ^ Who Named It?
- doi:10.1102/1470-5206.2011.L001. Archived from the originalon 27 January 2012.
- PMID 12928293.
- ^ B. Adamandiades. Sur un cas d'iritis à hypopyon récidivant. Annales d'oculistique, Paris, 1931, 168: 271–278.
- doi:10.1111/j.1474-7766.2004.03-225.x (inactive 8 March 2024).)
{{cite journal}}: CS1 maint: DOI inactive as of March 2024 (link - ^ Saleem S (2005). "Neuro-Behçet's Disease: NBD". Neurographics. 4 (2): 1. Archived from the original on 16 March 2008.
- S2CID 16483117.
- PMID 2188002.
Further reading
- Brissaud P, Laroche L, de Gramont A, Krulik M (March 1985). "Digital angiography for the diagnosis of dural sinus thrombosis in Behçet's disease". Arthritis Rheum. 28 (3): 359–60. PMID 3884020.
- el-Ramahi KM, al-Kawi MZ (September 1991). "Papilloedema in Behçet's disease: value of MRI in diagnosis of dural sinus thrombosis". J. Neurol. Neurosurg. Psychiatry. 54 (9): 826–29. PMID 1955903.
- Yamauchi Y, Cruz JM, Kaplan HJ, Goto H, Sakai J, Usui M (2005). "Suspected simultaneous bilateral anterior ischemic optic neuropathy in a patient with Behçet's disease". Ocul. Immunol. Inflamm. 13 (4): 317–25. S2CID 24830133.
External links
- Behçet's disease at Curlie
- Questions and answers about Behçet's disease – US National Institute of Arthritis and Musculoskeletal and Skin Diseases
