Bronchiolitis
| Bronchiolitis | |
|---|---|
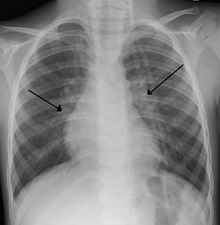 | |
| An X-ray of a child with RSV showing the typical bilateral perihilar fullness of bronchiolitis. | |
| Specialty | Emergency medicine, pediatrics |
| Symptoms | Fever, cough, runny nose, wheezing, breathing problems[1] |
| Complications | Shortness of breath, dehydration[1] |
| Usual onset | Less than 2 years old[2] |
| Causes | Viral disease (respiratory syncytial virus, human rhinovirus)[2] |
| Diagnostic method | Based on symptoms[1] |
| Differential diagnosis | Asthma, pneumonia, heart failure, allergic reaction, cystic fibrosis[1] |
| Treatment | Symptomatic treatment (oxygen, support with feeding, intravenous fluids)[3] |
| Frequency | ~20% (children less than 2)[2][1] |
| Deaths | 1% (among those hospitalized)[4] |
Bronchiolitis is inflammation of the small airways in the lungs. Acute bronchiolitis is due to a viral infection usually affecting children younger than two years of age.[5] Symptoms may include fever, cough, runny nose, wheezing, and breathing problems.[1] More severe cases may be associated with nasal flaring, grunting, or the skin between the ribs pulling in with breathing.[1] If the child has not been able to feed properly, signs of dehydration may be present.[1]
Chronic bronchiolitis is the general term used for
Acute bronchiolitis is usually the result of infection by respiratory syncytial virus (72% of cases) or human rhinovirus (26% of cases).[2] Diagnosis is generally based on symptoms.[1] Tests such as a chest X-ray or viral testing are not routinely needed.[2]
There is no specific treatment.[3][7] Symptomatic treatment at home is generally sufficient.[1] Occasionally, hospital admission for oxygen, support with feeding, or intravenous fluids is required.[1] Tentative evidence supports nebulized hypertonic saline.[8][needs update] Evidence for antibiotics, antivirals, bronchodilators, or nebulized epinephrine is either unclear or not supportive.[9]
About 10% to 30% of children under the age of two years are affected by bronchiolitis at some point in time.[1][2] It commonly occurs in the winter in the Northern Hemisphere.[1] It is the leading cause of hospitalizations in those less than one year of age in the United States.[10][7] The risk of death among those who are admitted to hospital is about 1%.[4] Outbreaks of the condition were first described in the 1940s.[11]
Signs and symptoms
Bronchiolitis typically presents in children under two years old and is characterized by a constellation of respiratory symptoms that consists of fever,
Some signs of severe disease include:[12]
- increased work of breathing (such as use of accessory muscles of respiration, rib & sternal retraction, tracheal tug)
- severe chest wall recession (Hoover's sign)
- presence of nasal flaring and/or grunting
- increased respiratory rate above normal
- hypoxia(low oxygen levels)
- cyanosis (bluish skin)
- lethargy and decreased activity
- poor feeding (less than half of usual fluid intake in preceding 24 hours)
- history of stopping breathing
Causes

The term usually refers to acute viral bronchiolitis, a common disease in infancy. This is most commonly caused by
Risk factors
Children are at an increased risk for progression to severe respiratory disease if they have any of the following additional factors:[7][10][15][16]
- Preterm infant (gestational ageless than 37 weeks)
- Younger age at onset of illness (less than 3 months of age)
- Congenital heart disease
- Immunodeficiency
- Chronic lung disease
- Neurological disorders
- Tobacco smoke exposure
Diagnosis
The diagnosis is typically made by clinical examination.
Testing for the specific viral cause can be done but has little effect on management and thus is not routinely recommended.
Infants with bronchiolitis between the age of two and three months have a second infection by bacteria (usually a urinary tract infection) less than 6% of the time.[19] When further evaluated with a urinalysis, infants with bronchiolitis had a concomitant UTI 0.8% of the time.[20] Preliminary studies have suggested that elevated procalcitonin levels may assist clinicians in determining the presence of bacterial co-infection, which could prevent unnecessary antibiotic use and costs.[21]
Differential diagnosis
There are many childhood illnesses that can present with respiratory symptoms, particularly persistent cough and wheezing.[10][22] Bronchiolitis may be differentiated from some of these by the characteristic pattern of preceding febrile upper respiratory tract symptoms lasting for 1 to 3 days followed by the persistent cough, tachypnea, and wheezing.[22] However, some infants may present without fever (30% of cases) or may present with apnea without other signs or with poor weight gain prior to onset of symptoms.[22] In such cases, additional laboratory testing and radiographic imaging may be useful.[10][22] The following are some other diagnoses to consider in an infant presenting with signs of bronchiolitis:[citation needed]
- Asthma and reactive airway disease
- Bacterial pneumonia
- Congenital heart disease
- Heart failure
- Whooping cough
- Allergic reaction
- Cystic fibrosis
- Chronic pulmonary disease
- Foreign body aspiration
- Vascular ring
Prevention
Prevention of bronchiolitis relies strongly on measures to reduce the spread of the viruses that cause respiratory infections (that is, handwashing, and avoiding exposure to those symptomatic with respiratory infections).[7][10] Guidelines are mixed on the use of gloves, aprons, or personal protective equipment.[7]
One way to improve the immune system is to feed the infant with breast milk, especially during the first month of life.[16][23] Respiratory infections were shown to be significantly less common among breastfed infants and fully breastfed RSV-positive hospitalized infants had shorter hospital stays than non or partially breastfed infants.[10] Guidelines recommend exclusive breastfeeding for infants for the first 6 months of life.[10]
The US Food and Drug Administration (FDA) has currently approved two RSV vaccines for adults ages 60 and older, Arexvy (GSK plc) and Abrysvo (Pfizer).[24] Abrysvo is also approved for "immunization of pregnant individuals at 32 through 36 weeks gestational age for the prevention of lower respiratory tract disease (LRTD) and severe LRTD caused by respiratory syncytial virus (RSV) in infants from birth through 6 months of age."[25]
Nirsevimab, a monoclonal antibody against RSV, is recommended by the CDC for all children younger than 8 months in their first RSV season.[24] Additionally, children aged 8 to 19 months who are at increased risk may be recommended to receive Nirsevimab as they enter their second RSV season.[26][27]
A second monoclonal antibody,
Tobacco smoke exposure has been shown to increase both the rates of lower respiratory disease in infants, as well as the risk and severity of bronchiolitis.[10] Tobacco smoke lingers in the environment for prolonged periods and on clothing even when smoking outside the home.[10] Guidelines recommend that parents be fully educated on the risks of tobacco smoke exposure on children with bronchiolitis.[10][22]
Management
Treatment of bronchiolitis is usually focused on the hydration and symptoms instead of the infection itself since the infection will run its course and complications are typically from the symptoms themselves.[28] Without active treatment, half of cases will go away in 13 days and 90% in three weeks.[29] Children with severe symptoms, especially poor feeding or dehydration, may be considered for hospital admission.[7] Oxygen saturation under 90%-92% as measured with pulse oximetry is also frequently used as an indicator of need for hospitalization.[7] High-risk infants, apnea, cyanosis, malnutrition, and diagnostic uncertainty are additional indications for hospitalization.[7]
Most guidelines recommend sufficient fluids and nutritional support for affected children.
Diet
Maintaining hydration is an important part of management of bronchiolitis.
Oxygen

Inadequate oxygen supply to the tissue is one of the main concerns during severe bronchiolitis and
When choosing to use oxygen therapy for a child with bronchiolitis, there is evidence that home oxygen may reduce hospitalization rate and length of stay although readmission rates and follow-up visits are increased.[10] Also, the use of humidified, heated, high-flow nasal cannula may be a safe initial therapy to decrease work of breathing and need for intubation.[10][37] However, evidence is lacking regarding the use of high-flow nasal cannula compared to standard oxygen therapy or continuous positive airway pressure.[18][37][38][needs update] These practices may still be used in severe cases prior to intubation.[22][39][40][needs update]
Blood gas testing is not recommended for people hospitalized with the disease and is not useful in the routine management of bronchiolitis.[18][22] People with severe worsening respiratory distress or impending respiratory failure may be considered for capillary blood gas testing.[22]
Hypertonic saline
Guidelines recommend against the use of
Bronchodilators
Guidelines recommend against the use of bronchodilators in children with bronchiolitis as evidence does not support a change in outcomes with such use.[10][22][44][45] Additionally, there are adverse effects to the use of bronchodilators in children such as tachycardia and tremors, as well as adding increased financial expenses.[46][44]
Several studies have shown that bronchodilation with β-adrenergic agents such as salbutamol may improve symptoms briefly but do not affect the overall course of the illness or reduce the need for hospitalization.[10] However, there are conflicting recommendations about the use of a trial of a bronchodilator, especially in those with history of previous wheezing, due to the difficulty with assessing an objective improvement in symptoms.[7][10][18] Bronchiolitis-associated wheezing is likely not effectively alleviated by bronchodilators anyway as it is caused by airway obstruction and plugging of the small airway diameters by luminal debris, not bronchospasm as in asthma-associated wheezing that bronchodilators usually treat well.[44]
Anticholinergic inhalers, such as ipratropium bromide, have a modest short-term effect at best and are not recommended for treatment.[22][47][48]
Epinephrine
The current state of evidence suggests that
Epinephrine is an α and β adrenergic agonist that has been used to treat other upper respiratory tract illnesses, such as croup, as a nebulized solution.[49] A Cochrane meta-analysis in 2011 found no benefit to the use of epinephrine in the inpatient setting and suggested that there may be utility in the outpatient setting in reducing the rate of hospitalization.[50][31] However, current guidelines do not support the outpatient use of epinephrine given the lack of substantial sustained benefit.[10]
A 2017 review found inhaled
Fluid therapy
Approximately 50% of infants who are hospitalized due to bronchiolitis require fluid therapy.
Unclear evidence
Currently other medications do not yet have evidence to support their use, although they have been studied for use in bronchiolitis.[10][50] Experimental trials with novel antiviral medications in adults are promising but it remains unclear if the same benefit will be present.[18]
- Surfactant had favorable effects for severely critical infants on duration of mechanical ventilation and ICU stay however studies were few and small.[53][14]
- Chest physiotherapy, such as vibration or percussion, to promote airway clearance may slightly reduce duration of oxygen therapy but there is a lack of evidence that demonstrates any other benefits.[10][54] People with difficulty clearing secretions due to underlying disorders such as spinal muscle atrophy or severe tracheomalacia may be considered for chest physiotherapy.[22]
- Suctioning of the
- Heliox, a mixture of oxygen and the inert gas helium, may be beneficial in infants with severe acute RSV bronchiolitis who require CPAP but overall evidence is lacking.[30]
- DNAse has not been found to be effective but might play a role in severe bronchiolitis complicated by atelectasis.[55]
- There are no systematic reviews or controlled trials on the effectiveness of nasal decongestants, such as xylometazoline, for the treatment of bronchiolitits.[14]
- Overall evidence is insufficient to support the use of alternative medicine.
Non-effective treatments
- Ribavirin is an antiviral drug which does not appear to be effective for bronchiolitis.[14]
- Antibiotics are often given in case of a bacterial infection complicating bronchiolitis, but have no effect on the underlying viral infection and their benefit is not clear.[14][57][58] The risks of bronchiolitis with a concomitant serious bacterial infection among hospitalized febrile infants is minimal and work-up and antibiotics are not justified.[10][20] Azithromycin adjuvant therapy may reduce the duration of wheezing and coughing in children with bronchiolitis but has not effect on length of hospital stay or duration of oxygen therapy.[59]
- Leukotriene inhibitors, such as montelukast, have not been found to be beneficial and may increase adverse effects.[7][63][64][65]
- Immunoglobulins are of unclear benefit.[66]
Epidemiology
Bronchiolitis typically affects infants and children younger than two years, principally during the autumn and winter.[18] It is the leading cause of hospital admission for respiratory disease among infants in the United States and accounts for one out of every 13 primary care visits.[7] Bronchiolitis accounts for 3% of emergency department visits for children under 2 years old.[14] Bronchiolitis is the most frequent lower respiratory tract infection and hospitalization in infants worldwide.[18]
References
- ^ PMID 25414585.
- ^ PMID 24739493.
- ^ S2CID 3454691.
- ^ ISBN 978-1437719840.
- ^ PMID 32551095.
- ISBN 9780323353175.
- ^ PMID 31541233.
- ^ PMID 29265171.
- ^ PMID 27088767.
- ^ PMID 25349312.
- PMID 24362701.
- ISBN 9781905813018. Archived from the originalon 1 November 2012. Retrieved 6 December 2012.
- S2CID 208791826.
- ^ PMID 21486501.
- ^ PMID 14757603.
- ^ S2CID 39990266.
- ^ S2CID 4932917.
- ^ PMID 28859915.
- PMID 21969396.
- ^ PMID 30688987.
- S2CID 11141711.
- ^ a b c d e f g h i j k l m n o p "1 Recommendations | Bronchiolitis in children: diagnosis and management | Guidance | NICE". www.nice.org.uk. June 2015. Retrieved 31 October 2019.
- S2CID 7605378.
- ^ a b "Respiratory Syncytial Virus (RSV)". U.S. Food & Drug Administration. 14 September 2023. Retrieved 27 October 2023.
- ^ "ABRYSVO". U.S. Food & Drug Administration. Retrieved 27 October 2023.
- ^ "FDA Approves New Drug to Prevent RSV in Babies and Toddlers". U.S. Food & Drug Administration. 17 July 2023. Retrieved 27 October 2023.
- ^ "RSV Immunization for Children 19 months and Younger". Centers for Disease Control and Prevention. Retrieved 27 October 2023.
- PMID 19209271.
- PMID 24335668.
- ^ PMID 26384333.
- ^ PMID 21678340.
- PMID 37010196.
- PMID 23733383.
- PMID 35377462.
- PMID 21249676.
- PMID 28212381.
- ^ S2CID 58666508.
- PMID 24442856.
- PMID 28192893.
- PMID 30701528.
- PMID 26416925.
- S2CID 48358175.
- PMID 37014057.
- ^ PMID 24937099.
- ^ "Bronchiolitis - Clinical Practice Guideline". www.aafp.org. Archived from the original on 23 October 2019. Retrieved 23 October 2019.
- PMID 12137663.
- S2CID 25465924.
- PMID 16034861.
- PMID 24114291.
- ^ PMID 21471175.
- PMID 28690542.
- ^ PMID 34852398.
- PMID 26299681.
- S2CID 51680313.
- PMID 23152257.
- ^ PMID 28212381.
- PMID 25300167.
- PMID 28828759.
- PMID 31416508.
- PMID 29750779.
- PMID 29677180.
- PMID 31375615.
- PMID 28032855.
- S2CID 27539127.
- PMID 25773054.
- PMID 37870128.
External links
- Bronchiolitis. Patient information from NHS Choices
- "Bronchiolitis in children – A national clinical guideline" (PDF). Archived from the original (PDF) on 4 March 2016. Retrieved 6 December 2007. (1.74 MB) from the Scottish Intercollegiate Guidelines Network
- Ralston SL, Lieberthal AS, Meissner HC, Alverson BK, Baley JE, Gadomski AM, et al. (November 2014). "Clinical practice guideline: the diagnosis, management, and prevention of bronchiolitis". Pediatrics. 134 (5): e1474–e1502. PMID 25349312.

