Brucellosis
| Brucellosis | |
|---|---|
| Other names | undulant fever, undulating fever, Mediterranean fever, Malta fever, Cyprus fever, rock fever (Micrococcus melitensis) aminoglycosides |
Brucellosis[4] is a zoonosis caused by ingestion of unpasteurized milk from infected animals, or close contact with their secretions.[5] It is also known as undulant fever, Malta fever, and Mediterranean fever.[6]
The bacteria causing this disease,
Signs and symptoms
This section needs additional citations for verification. (January 2023) |

The symptoms are like those associated with many other febrile diseases, but with emphasis on muscular pain and night sweats. The duration of the disease can vary from a few weeks to many months or even years.
In the first stage of the disease,
This complex is, at least in Portugal, Israel, Syria, and Jordan, known as Malta fever. During episodes of Malta fever, melitococcemia (presence of brucellae in the blood) can usually be demonstrated by means of blood culture in tryptose medium or Albini medium. If untreated, the disease can give origin to focalizations[clarification needed] or become chronic. The focalizations of brucellosis occur usually in bones and joints, and osteomyelitis or spondylodiscitis of the lumbar spine accompanied by sacroiliitis is very characteristic of this disease. Orchitis is also common in men.
The consequences of Brucella infection are highly variable and may include arthritis, spondylitis, thrombocytopenia, meningitis, uveitis, optic neuritis, endocarditis, and various neurological disorders collectively known as neurobrucellosis.
Cause

Brucellosis in humans is usually associated with consumption of unpasteurized milk and soft cheeses made from the milk of infected animals—often goats—infected with B. melitensis, and with occupational exposure of laboratory workers, veterinarians, and slaughterhouse workers. These infected animals may be healthy and asymptomatic.
Overall findings support that brucellosis poses an
Diagnosis

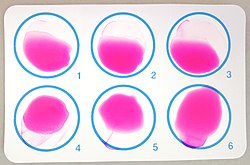
The diagnosis of brucellosis relies on:[citation needed]
- Demonstration of the agent: blood cultures in tryptose broth, bone marrow cultures: The growth of brucellae is extremely slow (they can take up to two months to grow) and the culture poses a risk to laboratory personnel due to high infectivity of brucellae.
- Demonstration of antibodies against the agent either with the classic Huddleson, Wright, and/or Bengal Rose reactions, either with ELISA or the 2-mercaptoethanol assay for IgM antibodies associated with chronic disease
- Histologic evidence of granulomatous hepatitis on hepatic biopsy
- Radiologic alterations in infected vertebrae: the Pedro Pons sign (preferential erosion of the anterosuperior corner of lumbar vertebrae) and marked osteophytosis are suspicious of brucellic spondylitis.
Definite diagnosis of brucellosis requires the isolation of the organism from the blood, body fluids, or tissues, but serological methods may be the only tests available in many settings. Positive blood culture yield ranges between 40 and 70% and is less commonly positive for B. abortus than
Due to the similarity of the O
Dipstick assays are new and promising, based on the binding of Brucella IgM antibodies, and are simple, accurate, and rapid. ELISA typically uses cytoplasmic proteins as antigens. It measures IgM, IgG, and IgA with better sensitivity and specificity than the SAT in most recent comparative studies.[15] The commercial Brucellacapt test, a single-step immunocapture assay for the detection of total anti-Brucella antibodies, is an increasingly used adjunctive test when resources permit. PCR is fast and should be specific. Many varieties of PCR have been developed (e.g. nested PCR, realtime PCR, and PCR-ELISA) and found to have superior specificity and sensitivity in detecting both primary infection and relapse after treatment.[16] Unfortunately, these are not standardized for routine use, and some centres have reported persistent PCR positivity after clinically successful treatment, fuelling the controversy about the existence of prolonged chronic brucellosis.[citation needed]
Other laboratory findings include normal peripheral white cell count, and occasional
Prevention
Surveillance using serological tests, as well as tests on milk such as the milk ring test, can be used for screening and play an important role in campaigns to eliminate the disease. Also, individual animal testing both for trade and for disease-control purposes is practiced. In endemic areas, vaccination is often used to reduce the incidence of infection. An animal vaccine is available that uses modified live bacteria. The World Organisation for Animal Health Manual of Diagnostic Test and Vaccines for Terrestrial Animals provides detailed guidance on the production of vaccines. As the disease is closer to being eliminated, a test and eradication program is required to eliminate it.[citation needed]
The main way of preventing brucellosis is by using fastidious hygiene in producing raw milk products, or by pasteurizing all milk that is to be ingested by human beings, either in its unaltered form or as a derivative, such as cheese.[citation needed]
Another important aspect of Brucellosis prevention is public awareness. People in endemic areas demonstrated a high lack of knowledge and understanding of the disease and its causes.[18] To combat this, the One Health concept has been proposed. One Health is a method for combining disciplines such as public health, veterinary services, and microbiology to bring awareness to the disease. However, the implementation of this method faces many challenges including economic, political, and social barriers.[19]
Treatment
Antibiotics such as tetracyclines, rifampicin, and the aminoglycosides streptomycin and gentamicin are effective against Brucella bacteria. However, the use of more than one antibiotic is needed for several weeks, because the bacteria incubate within cells.[citation needed]
The gold standard treatment for adults is daily
Doxycycline is able to cross the blood–brain barrier, but requires the addition of two other drugs to prevent relapse. Ciprofloxacin and co-trimoxazole therapy is associated with an unacceptably high rate of relapse. In brucellic endocarditis, surgery is required for an optimal outcome. Even with optimal antibrucellic therapy, relapses still occur in 5 to 10% of patients with Malta fever.[citation needed]
Prognosis
The mortality of the disease in 1909, as recorded in the British Army and Navy stationed in Malta, was 2%. The most frequent cause of death was
Epidemiology
Argentina
According to a study published in 2002, an estimated 10–13% of farm animals were infected with Brucella species.
Australia
Australia is free of cattle brucellosis, although it occurred in the past. Brucellosis of sheep or goats has never been reported. Brucellosis of pigs does occur. Feral pigs are the typical source of human infections.[27][28]
Canada
On 19 September 1985, the
China
An outbreak infecting humans took place in Lanzhou in 2019 after the Lanzhou Biopharmaceutical Plant, which was involved in vaccine production, accidentally pumped out the bacteria into the atmosphere in exhaust air due to use of expired disinfectant.[30][31]
According to Georgios Pappas, an infectious-disease specialist and author of a report published in the journal Clinical Infectious Diseases,[32] the result was “possibly the largest laboratory accident in the history of infectious diseases.” According to Pappas, out of nearly 70,000 people tested, more than 10,000 were seropositive, citing figures compiled by the provincial health authorities in Lanzhou’s Gansu province. Pappas also states that Chinese documents show that more than 3,000 people living near the plant applied for compensation, an indication of at least a mild illness.[33]
Europe

Malta
Until the early 20th century, the disease was endemic in Malta to the point of it being referred to as "Maltese fever". Since 2005, due to a strict regimen of certification of milk animals and widespread use of pasteurization, the illness has been eradicated from Malta.[34]
Republic of Ireland
Ireland was declared free of brucellosis on 1 July 2009. The disease had troubled the country's farmers and veterinarians for several decades.[35][36] The Irish government submitted an application to the European Commission, which verified that Ireland had been liberated.[36] Brendan Smith, Ireland's then Minister for Agriculture, Food and the Marine, said the elimination of brucellosis was "a landmark in the history of disease eradication in Ireland".[35][36] Ireland's Department of Agriculture, Food and the Marine intends to reduce its brucellosis eradication programme now that eradication has been confirmed.[35][36]
UK
Mainland Britain has been free of brucellosis since 1979, although there have been episodic re-introductions since.[37] The last outbreak of brucellosis in Great Britain was in cattle in Cornwall in 2004.[37][38] Northern Ireland was declared officially brucellosis-free in 2015.[37]
New Zealand
Brucellosis in New Zealand is limited to sheep (B. ovis). The country is free of all other species of Brucella.[39]
United States
Dairy herds in the U.S. are tested at least once a year to be certified brucellosis-free[40] with the Brucella milk ring test.[41] Cows confirmed to be infected are often killed. In the United States, veterinarians are required [citation needed] to vaccinate all young stock, to further reduce the chance of zoonotic transmission. This vaccination is usually referred to as a "calfhood" vaccination. Most cattle receive a tattoo in one of their ears, serving as proof of their vaccination status. This tattoo also includes the last digit of the year they were born.[42]
The first state–federal cooperative efforts towards eradication of brucellosis caused by B. abortus in the U.S. began in 1934.[citation needed]
Brucellosis was originally imported to North America with non-native domestic cattle (Bos taurus), which transmitted the disease to wild bison (Bison bison) and elk (Cervus canadensis). No records exist of brucellosis in ungulates native to America until the early 19th century.[43]
History


Brucellosis first came to the attention of British medical officers in the 1850s in Malta during the Crimean War, and was referred to as Malta Fever. Jeffery Allen Marston (1831–1911) described his own case of the disease in 1861. The causal relationship between organism and disease was first established in 1887 by David Bruce.[44][45] Bruce considered the agent spherical and classified it as a coccus.[citation needed]
In 1897,
Maltese scientist and archaeologist Themistocles Zammit identified unpasteurized goat milk as the major etiologic factor of undulant fever in June 1905.[47]
In the late 1910s, American bacteriologist Alice C. Evans was studying the Bang bacillus and gradually realized that it was virtually indistinguishable from the Bruce coccus.[48] The short-rod versus oblong-round morphologic borderline explained the leveling of the erstwhile bacillus/coccus distinction (that is, these "two" pathogens were not a coccus versus a bacillus but rather were one coccobacillus).[48] The Bang bacillus was already known to be enzootic in American dairy cattle, which showed itself in the regularity with which herds experienced contagious abortion.[48] Having made the discovery that the bacteria were certainly nearly identical and perhaps totally so, Evans then wondered why Malta fever was not widely diagnosed or reported in the United States.[48] She began to wonder whether many cases of vaguely defined febrile illnesses were in fact caused by the drinking of raw (unpasteurized) milk.[48] During the 1920s, this hypothesis was vindicated. Such illnesses ranged from undiagnosed and untreated gastrointestinal upset to misdiagnosed[48] febrile and painful versions, some even fatal. This advance in bacteriological science sparked extensive changes in the American dairy industry to improve food safety. The changes included making pasteurization standard and greatly tightening the standards of cleanliness in milkhouses on dairy farms. The expense prompted delay and skepticism in the industry,[48] but the new hygiene rules eventually became the norm. Although these measures have sometimes struck people as overdone in the decades since, being unhygienic at milking time or in the milkhouse, or drinking raw milk, are not a safe alternative.[citation needed]
In the decades after Evans's work, this genus, which received the name Brucella in honor of Bruce, was found to contain several species with varying virulence. The name "brucellosis" gradually replaced the 19th-century names Mediterranean fever and Malta fever.[49]
Neurobrucellosis, a neurological involvement in brucellosis, was first described in 1879. In the late 19th century, its symptoms were described in more detail by M. Louis Hughes, a Surgeon-Captain of the
These obsolete names have previously been applied to brucellosis:[49][53]
- Crimean fever
- Cyprus fever
- Gibraltar fever
- Goat fever
- Italian fever
- Neapolitan fever
Biological warfare
Brucella species had been weaponized by several advanced countries by the mid-20th century. In 1954, B. suis became the first agent weaponized by the United States at its Pine Bluff Arsenal near Pine Bluff, Arkansas. Brucella species survive well in aerosols and resist drying. Brucella and all other remaining biological weapons in the U.S. arsenal were destroyed in 1971–72 when the American offensive biological warfare program was discontinued by order of President Richard Nixon.[54]
The experimental American bacteriological warfare program focused on three agents of the Brucella group:[citation needed]
- Porcine brucellosis(agent US)
- Bovine brucellosis (agent AA)
- Caprine brucellosis (agent AM)
Agent US was in advanced development by the end of
The main drawback of using the M114 with Agent US was that it acted mainly as an incapacitating agent, whereas the USAF administration wanted weapons that were deadly. The stability of M114 in storage was too low to allow for storing it at forward air bases, and the logistical requirements to neutralize a target were far higher than originally planned. Ultimately, this would have required too much logistical support to be practical in the field.[citation needed]
Agents US and AA had a median infective dose of 500 organisms/person, and for Agent AM it was 300 organisms/person. The incubation time was believed to be about 2 weeks, with a duration of infection of several months. The lethality estimate was, based on epidemiological information, 1 to 2 per cent. Agent AM was believed to be a somewhat more virulent disease, with a fatality rate of 3 per cent being expected.[citation needed]
Other animals
Species infecting domestic livestock are
Cattle
The two main causes for spontaneous abortion in animals are
]Dogs
The causative agent of brucellosis in dogs, B. canis, is transmitted to other dogs through breeding and contact with aborted fetuses. Brucellosis can occur in humans who come in contact with infected aborted tissue or semen. The bacteria in dogs normally infect the genitals and lymphatic system, but can also spread to the eyes, kidneys, and intervertebral discs. Brucellosis in the intervertebral disc is one possible cause of discospondylitis. Symptoms of brucellosis in dogs include abortion in female dogs and scrotal inflammation and orchitis in males. Fever is uncommon. Infection of the eye can cause uveitis, and infection of the intervertebral disc can cause pain or weakness. Blood testing of the dogs prior to breeding can prevent the spread of this disease. It is treated with antibiotics, as with humans, but it is difficult to cure.[56]
Aquatic wildlife
Brucellosis in cetaceans is caused by the bacterium
Terrestrial wildlife
The disease in its various strains can infect multiple wildlife species, including elk (Cervus canadensis), bison (Bison bison), African buffalo (Syncerus caffer), European wild boar (Sus scrofa), caribou (Rangifer tarandus), moose (Alces alces), and marine mammals (see section on aquatic wildlife above).[58][59] While some regions use vaccines to prevent the spread of brucellosis between infected and uninfected wildlife populations, no suitable brucellosis vaccine for terrestrial wildlife has been developed.[60] This gap in medicinal knowledge creates more pressure for management practices that reduce spread of the disease.[60]
Wild bison and elk in the greater
The National Elk Refuge in Jackson, Wyoming asserts that the intensity of the winter feeding program affects the spread of brucellosis more than the population size of elk and bison.[58] Since concentrating animals around food plots accelerates spread of the disease, management strategies to reduce herd density and increase dispersion could limit its spread.[58]
Effects on hunters
Hunters may be at additional risk for exposure to brucellosis due to increased contact with susceptible wildlife, including predators that may have fed on infected prey. Hunting dogs can also be at risk of infection.[62] Exposure can occur through contact with open wounds or by directly inhaling the bacteria while cleaning game.[63] In some cases, consumption of undercooked game can result in exposure to the disease.[63] Hunters can limit exposure while cleaning game through the use of precautionary barriers, including gloves and masks, and by washing tools rigorously after use.[60][64] By ensuring that game is cooked thoroughly, hunters can protect themselves and others from ingesting the disease.[63] Hunters should refer to local game officials and health departments to determine the risk of brucellosis exposure in their immediate area and to learn more about actions to reduce or avoid exposure.[citation needed]
See also
References
- ^ a b c "Brucellosis". mayoclinic.org. Mayo Clinic. Retrieved June 5, 2022.
- ^ "Brucellosis". mayoclinic.org. Mayo Clinic. Retrieved June 5, 2022.
- ^ "Brucellosis". American Heritage Dictionary. Archived from the original on 2011-06-06.
- ^ "Diagnosis and Management of Acute Brucellosis in Primary Care" (PDF). Brucella Subgroup of the Northern Ireland Regional Zoonoses Group. August 2004. Archived from the original (PDF) on 2007-10-13.
- PMID 21398234.
- ^ Park. K., Park’s textbook of preventive and social medicine, 23 editions. Page 290-91
- ISBN 978-93-5090-187-8, retrieved 2022-11-13
- ^ "Brucellosis: Resources: Surveillance". CDC. 2018-10-09.
- PMID 28722861, retrieved 2023-11-08
- PMID 16199812.
- S2CID 53034163.
- PMID 18045560.
- S2CID 5068325.
- PMID 20682874.
- PMID 20718083.
- PMID 18462106.
- PMID 31048848.
- PMID 37630630.
- PMID 16575723.
- PMID 1420670.
- PMID 23076931.
- PMID 16102304.
- PMID 18199967.
- PMID 12414136.
- ^ "Brucelosis Bovina". SENASA - Argentine Government. 2022. Archived from the original on 2016-02-16.
- ^ "Queensland Health: Brucellosis". State of Queensland (Queensland Health). 2010-11-24. Archived from the original on 2011-04-22. Retrieved 2011-06-06.
- ^
Lehane, Robert (1996) Beating the Odds in a Big Country: The eradication of bovine brucellosis and tuberculosis in Australia, CSIRO Publishing, ISBN 0-643-05814-1
- ^ "Reportable Diseases". Accredited Veterinarian's Manual. Canadian Food Inspection Agency. Archived from the original on 2007-02-08. Retrieved 2007-03-18.
- ^ China reports outbreak of brucellosis disease 'way larger' than originally thought 18 September 2020 www.news.com.au, accessed 18 September 2020
- ^ "兰州药厂泄漏事件布病患者:肿痛无药可吃,有人已转成慢性病_绿政公署_澎湃新闻-The Paper". www.thepaper.cn. Retrieved 2 June 2021.
- PMID 35675697.
- ^ Warwick J, Willman D (April 12, 2023). "China's struggles with lab safety carry danger of another pandemic". The Washington Post. Washington D.C.
- ISBN 978-99909-0-425-3.
- ^ a b c "Ireland free of brucellosis". RTÉ. 2009-07-01. Retrieved 2009-07-01.
- ^ a b c d "Ireland declared free of brucellosis". The Irish Times. 2009-07-01. Archived from the original on 2021-04-03. Retrieved 2009-07-01.
Michael F Sexton, president of Veterinary Ireland, which represents vets in practice, said: "Many vets and farmers in particular suffered significantly with brucellosis in past decades and it is greatly welcomed by the veterinary profession that this debilitating disease is no longer the hazard that it once was."
- ^ a b c Monitoring brucellosis in Great Britain 3 September 2020 veterinary-practice.com, accessed 18 September 2020
- ^ Guidance Brucellosis: how to spot and report the disease 18 October 2018 www.gov.uk, accessed 18 September 2020
- ^ "MAF Biosecurity New Zealand: Brucellosis". Ministry of Agriculture and Forestry of New Zealand. Archived from the original on 2012-03-20. Retrieved 2011-06-06.
- ^ Brucellosis Eradication APHIS 91–45–013. United States Department of Agriculture. October 2003. p. 14.
- PMID 15405523.
- ^ Vermont Beef Producers. "How important is calfhood vaccination?" (PDF). Archived from the original (PDF) on 2008-05-09.
- JSTOR 2386505. Archived from the original(PDF) on 2017-01-08. Retrieved 2017-01-07.
- ^ Wilkinson L (1993). "Brucellosis". In Kiple KF (ed.). The Cambridge World History of Human Disease. Cambridge University Press.
- Who Named It?
- ^ Evans A (1963). Dr. Alice C. Evans Memoir.
- ^ OCLC 11210642.
- ^ PMC 498028.
- ISBN 978-1-4831-9359-5.
- .
- PMID 15037461.
- ISSN 0040-781X. Retrieved 2017-05-01.
- U.S. Army Medical Institute of Infectious Diseases. p. 53. Archived from the original(PDF) on 2007-06-09.
- ISBN 0702027774.
- ISBN 978-0-7216-4679-4.
- PMID 22919595.
- ^ a b c "Brucellosis". www.fws.gov. U.S. Fish &Wildlife Service. 2016. Archived from the original on 2016-10-09. Retrieved 2016-10-03.
- PMID 11974615. Archived from the original(PDF) on 2015-06-06. Retrieved 2016-10-07.
- ^ PMID 23837363. Archived from the original(PDF) on 2015-06-06. Retrieved 2016-10-07.
- PMID 23837367.
- ^ CDC - Hunters Risks - Animals That Can Put Hunters at Risk
- ^ a b c "CDC – Home – Brucellosis". www.cdc.gov. Center for Disease Control. 2016. Retrieved 2016-10-03.
- ^ "Zoonoses – Brucellosis". www.who.int/en/. World Health Organization. 2016. Archived from the original on March 9, 2005. Retrieved 2016-10-03.
Further reading
- WHO fact sheet on brucellosis
- Brucella genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
- Prevention about Brucellosis from Centers for Disease Control
- Capasso L (August 2002). "Bacteria in two-millennia-old cheese, and related epizoonoses in Roman populations". The Journal of Infection. 45 (2): 122–7. PMID 12217720. – re high rate of brucellosis in humans in ancient Pompeii
- Brucellosis, factsheet from European Centre for Disease Prevention and Control
