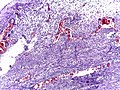
Appendicitis
| Appendicitis | |
|---|---|
| Other names | Epityphlitis |
| Frequency | 11.6 million (2015)[8] |
| Deaths | 50,100 (2015)[9] |
Appendicitis is inflammation of the appendix.[2] Symptoms commonly include right lower abdominal pain, nausea, vomiting, and decreased appetite.[2] However, approximately 40% of people do not have these typical symptoms.[2] Severe complications of a ruptured appendix include widespread, painful inflammation of the inner lining of the abdominal wall and sepsis.[3]
Appendicitis is primarily caused by a blockage of the
The diagnosis of appendicitis is largely based on the person's signs and symptoms.[11] In cases where the diagnosis is unclear, close observation, medical imaging, and laboratory tests can be helpful.[4] The two most commonly used imaging tests for diagnosing appendicitis are ultrasound and computed tomography (CT scan).[4] CT scan is more accurate than ultrasound in detecting acute appendicitis.[14] However, ultrasound may be preferred as the first imaging test in children and pregnant women because of the risks associated with radiation exposure from CT scans.[4] Although ultrasound may aid in diagnosis, its main role in identifying important differentials, such as ovarian pathology in females or mesenteric adenitis in children.
The standard treatment for acute appendicitis involves the surgical removal of the inflamed appendix.[6][11] This procedure can be performed either through an open incision in the abdomen (laparotomy) or using minimally invasive techniques with small incisions and cameras (laparoscopy). Surgery is essential to reduce the risk of complications or potential death associated with the rupture of the appendix.[3] Antibiotics may be equally effective in certain cases of non-ruptured appendicitis.[15][7][16] It is one of the most common and significant causes of sudden abdominal pain. In 2015, approximately 11.6 million cases of appendicitis were reported, resulting in around 50,100 deaths worldwide.[8][9] In the United States, appendicitis is one of the most common causes of sudden abdominal pain requiring surgery.[2] Annually, more than 300,000 individuals in the United States undergo surgical removal of their appendix.[17] Reginald Fitz is credited with being the first person to describe the condition in 1886.[18]
Signs and symptoms

The presentation of acute appendicitis includes acute abdominal pain, nausea, vomiting, and fever. As the appendix becomes more swollen and inflamed, it begins to irritate the adjoining abdominal wall. This leads the pain to localize at the right lower quadrant. This classic migration of pain may not appear in children under three years. This pain can be elicited through signs, which can feel sharp. Pain from appendicitis may begin as dull pain around the navel. After several hours, the pain usually migrates towards the right lower quadrant, where it becomes localized. Symptoms include localized findings in the right iliac fossa. The abdominal wall becomes very sensitive to gentle pressure (palpation). There is pain in the sudden release of deep tension in the lower abdomen (Blumberg's sign). If the appendix is retrocecal (localized behind the cecum), even deep pressure in the right lower quadrant may fail to elicit tenderness (silent appendix). This is because the cecum, distended with gas, protects the inflamed appendix from pressure. Similarly, if the appendix lies entirely within the pelvis, there is typically a complete absence of abdominal rigidity. In such cases, a digital rectal examination elicits tenderness in the rectovesical pouch. Coughing causes point tenderness in this area (McBurney's point), called Dunphy's sign.[medical citation needed]
Causes

Acute appendicitis seems to be the result of a primary obstruction of the appendix.[19][10] Once this obstruction occurs, the appendix becomes filled with mucus and swells. This continued production of mucus leads to increased pressures within the lumen and the walls of the appendix. The increased pressure results in thrombosis and occlusion of the small vessels, and stasis of lymphatic flow. At this point, spontaneous recovery rarely occurs. As the occlusion of blood vessels progresses, the appendix becomes ischemic and then necrotic. As bacteria begin to leak out through the dying walls, pus forms within and around the appendix (suppuration). The result is appendiceal rupture (a 'burst appendix') causing peritonitis, which may lead to sepsis and in rare cases, death. These events are responsible for the slowly evolving abdominal pain and other commonly associated symptoms.[12]
The causative agents include
The occurrence of a fecalith in the appendix was thought to be attributed to a right-sided fecal retention reservoir in the colon and a prolonged transit time. However, a prolonged transit time was not observed in subsequent studies.
Diagnosis

The physician will ask questions to get the
Typical appendicitis is characterized by a migratory
Atypical histories lack this typical progression and may include pain in the right lower quadrant as an initial symptom. Irritation of the peritoneum (inside lining of the abdominal wall) can lead to increased pain on movement, or jolting, for example going over speed bumps.[36] Atypical histories often require imaging with ultrasound or CT scanning.[3]
Signs
During the early stages of appendicitis diagnosis, it is common for physical exams to present inconspicuous findings. Signs of inflammation become noticeable as the disease progresses. These signs may include:[37]
- Aure-Rozanova's sign: Increased pain on palpation with a finger in the right inferior lumbar triangle (can be a positive Blumberg's sign).[38]
- Bartomier-Michelson's sign: Increased pain on palpation at the right iliac region as the person being examined lies on their left side compared to when they lie on their back.[38]
- Dunphy's sign: Increased pain in the right lower quadrant by coughing.[39]
- Hamburger sign: The patient refuses to eat (anorexia is 80% sensitive for appendicitis)[40]
- Kocher's sign (Kosher's sign): From the person's medical history, the start of pain in the umbilical region with a subsequent shift to the right iliac region.[38]
- Massouh's sign: Developed in and popular in southwest England, the examiner performs a firm swish with their index and middle finger across the abdomen from the xiphoid process to the left and the right iliac fossa.[39]
- Obturator sign: The person being evaluated lies on her or his back with the hip and knee both flexed at ninety degrees. The examiner holds the person's ankle with one hand and knee with the other hand. The examiner rotates the hip by moving the person's ankle away from their body while allowing the knee to move only inward. A positive test is pain with internal rotation of the hip.[41]
- Psoas sign, also known as "Obraztsova's sign", is right lower-quadrant pain that is produced with either the passive extension of the right hip or by the active flexion of the person's right hip while supine. The pain that is elicited is due to inflammation of the peritoneum overlying the iliopsoas muscles and inflammation of the psoas muscles themselves. Straightening out the leg causes pain because it stretches these muscles, while flexing the hip activates the iliopsoas and causes pain.[41]
- ileocaecal valve provoking right-sided abdominal pain.[42]
- Rosenstein's sign (Sitkovsky's sign): Increased pain in the right iliac region as the person is being examined lies on their left side.[43]
- Perman's sign: In acute appendicitis palpation in the left iliac fossa may produce pain in the right iliac fossa.[44]
Laboratory tests
While there is no laboratory test specific for appendicitis, a
In children, neutrophil-lymphocyte ratio (NLR) demonstrates a high degree of accuracy in the diagnosis of acute appendicitis and distinguishes complicated appendicitis from the simple one.[47] 75–78 percent of the patients have neutrophilia.[39] Delta-neutrophil index (DNI) is a valuable parameter that helps in the diagnosis of histologically normal appendicitis and distinguishing between simple and complicated appendicitis.[48]
A C-reactive protein (CRP) blood test will be ordered by the doctor to find out if there are any further causes of inflammation.[33] The C-reactive protein/albumin (CRP/ALB) ratio can be a reliable predictor of complicated appendicitis.[49]
The urinalysis is important for ruling out a urinary tract infection as the cause of abdominal pain. The presence of more than 20 WBC per high-power field in the urine is more suggestive of a urinary tract disorder.[45]
If the patient is a woman, a pregnancy test will be ordered.[33]
Imaging
In children, the clinical examination is important to determine which children with abdominal pain should receive immediate surgical consultation and which should receive diagnostic imaging.
Ultrasound

-
Ultrasound showing appendicitis and an appendicolith[58]
-
Ultrasound showing appendicitis and an appendicolith[58]
-
Ultrasound of a normal appendix for comparison
-
A normal appendix without and with compression. Absence of compressibility indicates appendicitis.[55]
Computed tomography


Where it is readily available,
The accurate diagnosis of appendicitis is multi-tiered, with the size of the appendix having the strongest
However, because the appendix can be filled with fecal material, causing intraluminal distention, this criterion has shown limited utility in more recent meta-analyses.[63] This is as opposed to ultrasound, in which the wall of the appendix can be more easily distinguished from intraluminal feces. In such scenarios, ancillary features such as increased wall enhancement as compared to adjacent bowel and inflammation of the surrounding fat, or fat stranding, can be supportive of the diagnosis. However, their absence does not preclude it. In severe cases with perforation, an adjacent phlegmon or abscess can be seen. Dense fluid layering in the pelvis can also result, related to either pus or enteric spillage. When patients are thin or younger, the relative absence of fat can make the appendix and surrounding fat stranding difficult to see.[63]
Magnetic resonance imaging
Magnetic resonance imaging (MRI) use has become increasingly common for diagnosis of appendicitis in children and pregnant patients due to the radiation dosage that, while of nearly negligible risk in healthy adults, can be harmful to children or the developing baby.[64] In pregnancy, it is more useful during the second and third trimester, particularly as the enlargening uterus displaces the appendix, making it difficult to find by ultrasound. The periappendiceal stranding that is reflected on CT by fat stranding on MRI appears as an increased fluid signal on T2 weighted sequences. First trimester pregnancies are usually not candidates for MRI, as the fetus is still undergoing organogenesis, and there are no long-term studies to date regarding its potential risks or side effects.[65]
X-ray

In general, plain abdominal radiography (PAR) is not useful in making the diagnosis of appendicitis and should not be routinely obtained from a person being evaluated for appendicitis.
Scoring systems
Several scoring systems have been developed to try to identify people who are likely to have appendicitis. The performance of scores such as the Alvarado score and the Pediatric Appendicitis Score, however, are variable.[69]
The Alvarado score is the most known scoring system. A score below 5 suggests against a diagnosis of appendicitis, whereas a score of 7 or more is predictive of acute appendicitis. In a person with an equivocal score of 5 or 6, a CT scan or ultrasound exam may be used to reduce the rate of negative appendectomy.
| Migratory right iliac fossa pain | 1 point |
| Anorexia | 1 point |
| Nausea and vomiting | 1 point |
| Right iliac fossa tenderness | 2 points |
| Rebound abdominal tenderness | 1 point |
| Fever | 1 point |
| High white blood cell count (leukocytosis) | 2 points |
| Shift to left (segmented neutrophils )
|
1 point |
| Total score | 10 points |
|---|
Pathology
Even for clinically certain appendicitis, routine histopathology examination of appendectomy specimens is of value for identifying unsuspected pathologies requiring further postoperative management.[70] Notably, appendix cancer is found incidentally in about 1% of appendectomy specimens.[71]
Pathology diagnosis of appendicitis can be made by detecting a
Periappendicitis (inflammation of tissues around the appendix) is often found in conjunction with other abdominal pathology.[72]
-
Micrograph of appendicitis and periappendicitis. H&E stain
-
Micrograph of appendicitis showing neutrophils in the muscularis propria. H&E stain
-
Acute suppurative appendicitis with perforation (at right). H&E stain
| Pattern | Gross pathology | Light microscopy | Image | Clinical significance |
|---|---|---|---|---|
| Acute intraluminal inflammation | None visible |
|

|
Probably none |
| Acuta mucosal inflammation | None visible |
|
May be secondary to enteritis. | |
| Suppurative acute appendicitis | May be inapparent.
|
|

|
Can be presumed to be primary cause of symptoms |
| Gangrenous/necrotizing appendicitis |
|
|

|
Will perforate if untreated |
| Periappendicitis | May be inapparent.
|
|

|
If isolated, probably secondary to other disease |
| Eosinophilic appendicitis | None visible |
|
Possibly parasitic, or eosinophilic enteritis. |
Differential diagnosis

Children:
Women: A pregnancy test is important for all women of childbearing age since an ectopic pregnancy can have signs and symptoms similar to those of appendicitis. Other obstetrical/ gynecological causes of similar abdominal pain in women include pelvic inflammatory disease, ovarian torsion, menarche, dysmenorrhea, endometriosis, and Mittelschmerz (the passing of an egg in the ovaries approximately two weeks before menstruation).[74]
Men: testicular torsion
Adults: new-onset
.Elderly:
The term "pseudoappendicitis" is used to describe a condition mimicking appendicitis.[75] It can be associated with Yersinia enterocolitica.[76]
Management
Acute appendicitis
Using antibiotics to prevent potential postoperative complications in emergency appendectomy procedures is recommended, and the antibiotics are effective when given to a person before, during, or after surgery.[83]
Pain
Pain medications (such as morphine) do not appear to affect the accuracy of the clinical diagnosis of appendicitis and therefore should be given early in the patient's care.[84] Historically there were concerns among some general surgeons that analgesics would affect the clinical exam in children, and some recommended that they not be given until the surgeon was able to examine the person.[84]
Surgery


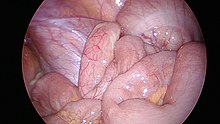
The surgical procedure for the removal of the appendix is called an appendectomy. Appendectomy can be performed through open or laparoscopic surgery. Laparoscopic appendectomy has several advantages over open appendectomy as an intervention for acute appendicitis.[85]
Open appendectomy
For over a century, laparotomy (open appendectomy) was the standard treatment for acute appendicitis.[86] This procedure consists of the removal of the infected appendix through a single large incision in the lower right area of the abdomen.[87] The incision in a laparotomy is usually 2 to 3 inches (51 to 76 mm) long.
During an open appendectomy, the person with suspected appendicitis is placed under general
Laparoscopic appendectomy
Laparoscopic appendectomy was introduced in 1983 and has become an increasingly prevalent intervention for acute appendicitis.
Laparoscopic-assisted transumbilical appendectomy
In pediatric patients, the high mobility of the cecum allows externalization of the appendix through the umbilicus, and the entire procedure can be performed with a single incision. Laparoscopic-assisted transumbilical appendectomy is a relatively recent technique but with long published series and very good surgical and aesthetic results.[91]
Pre-surgery
The treatment begins by
Once the decision to perform an appendectomy has been made, the preparation procedure takes approximately one to two hours. Meanwhile, the surgeon will explain the surgery procedure and will present the risks that must be considered when performing an appendectomy. (With all surgeries there are risks that must be evaluated before performing the procedures.) The risks are different depending on the state of the appendix. If the appendix has not ruptured, the complication rate is only about 3% but if the appendix has ruptured, the complication rate rises to almost 59%.[92] The most usual complications that can occur are pneumonia, hernia of the incision, thrombophlebitis, bleeding and adhesions. Evidence indicates that a delay in obtaining surgery after admission results in no measurable difference in outcomes to the person with appendicitis.[93][94]

The surgeon will explain how long the recovery process should take. Abdomen hair is usually removed to avoid complications that may appear regarding the incision.
In most cases, patients going in for surgery experience nausea or vomiting that require medication before surgery. Antibiotics, along with pain medication, may be administered before appendectomies.
After surgery
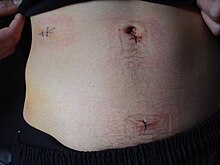
Hospital lengths of stay typically range from a few hours to a few days but can be a few weeks if complications occur. The recovery process may vary depending on the severity of the condition: if the appendix had ruptured or not before surgery. Appendix surgery recovery is generally much faster if the appendix did not rupture.[95] It is important that people undergoing surgery respect their doctor's advice and limit their physical activity so the tissues can heal. Recovery after an appendectomy may not require diet changes or a lifestyle change.
The length of hospital stays for appendicitis varies on the severity of the condition. A study from the United States found that in 2010, the average appendicitis hospital stay was 1.8 days. For stays where the person's appendix had ruptured, the average length of stay was 5.2 days.[13]
After surgery, the patient will be transferred to a
Prognosis
Most people with appendicitis recover quickly after surgical treatment, but complications can occur if treatment is delayed or if peritonitis occurs. Recovery time depends on age, condition, complications, and other circumstances, including the amount of alcohol consumption, but usually is between 10 and 28 days. For young children (around ten years old), the recovery takes three weeks.
The possibility of peritonitis is the reason why acute appendicitis warrants rapid evaluation and treatment. People with suspected appendicitis may have to undergo a medical evacuation. Appendectomies have occasionally been performed in emergency conditions (i.e., not in a proper hospital) when a timely medical evacuation was impossible.
Typical acute appendicitis responds quickly to appendectomy and occasionally will resolve spontaneously. If appendicitis resolves spontaneously, it remains controversial whether an elective interval appendectomy should be performed to prevent a recurrent episode of appendicitis. Atypical appendicitis (associated with suppurative appendicitis) is more challenging to diagnose and is more apt to be complicated even when operated early. In either condition, prompt diagnosis and appendectomy yield the best results with full recovery in two to four weeks usually. Mortality and severe complications are unusual but do occur, especially if peritonitis persists and is untreated.
Another entity known as the appendicular lump is talked about. It happens when the appendix is not removed early during infection, and omentum and intestine adhere to it, forming a palpable lump. During this period, surgery is risky unless there is pus formation evident by fever and toxicity or by ultrasound. Medical management treats the condition.
An unusual complication of an appendectomy is "stump appendicitis": inflammation occurs in the remnant appendiceal stump left after a prior incomplete appendectomy.[96] Stump appendicitis can occur months to years after initial appendectomy and can be identified with imaging modalities such as ultrasound.[97]
Epidemiology


Appendicitis is most common between the ages of 5 and 40.[99] In 2013, it resulted in 72,000 deaths globally, down from 88,000 in 1990.[100]
In the United States, there were nearly 293,000 hospitalizations involving appendicitis in 2010.[13] Appendicitis is one of the most frequent diagnoses for emergency department visits resulting in hospitalization among children ages 5–17 years in the United States.[101]
Adults presenting to the emergency department with a known family history of appendicitis are more likely to have this disease than those without.[102]
See also
References
- ^ "appendicitis". Medical Dictionary. Merriam-Webster. Archived from the original on 2013-12-30.
- ^ PMID 8921763.
- ^ a b c d Hobler K (Spring 1998). "Acute and Suppurative Appendicitis: Disease Duration and its Implications for Quality Improvement" (PDF). Permanente Medical Journal. 2 (2). Archived from the original (PDF) on 2021-03-06. Retrieved 2016-10-26.
- ^ PMID 12529465. Archived from the original(PDF) on 2017-09-22. Retrieved 2017-11-01.
- ISBN 978-0-323-07699-9.
- ^ ISBN 978-0-07-174889-6. Archivedfrom the original on 30 March 2016. Retrieved 6 November 2014.
- ^ PMID 22491789.
- ^ PMID 27733282.
- ^ PMID 27733281.
- ^ PMID 7136413.
- ^ ISBN 978-0-07-174467-6. Archivedfrom the original on 22 December 2016. Retrieved 6 November 2014.
- ^ ISBN 978-0-07-154770-3.
- ^ (PDF) from the original on 2016-10-20.
- ^ PMID 25493136.
- ^ PMID 34476484. Retrieved 8 September 2021.
- ^ "Appendicitis: Surgical vs. Medical Treatment | Science-Based Medicine". sciencebasedmedicine.org. 2020-11-24. Retrieved 2022-11-04.
- PMID 18687030.
- ^ Fitz RH (1886). "Perforating inflammation of the vermiform appendix with special reference to its early diagnosis and treatment". American Journal of the Medical Sciences (92): 321–346.
- .
- PMID 3052484.
- ^ PMID 21805435.
- PMID 2990360.
- PMID 2385810.
- PMID 2992354.
- PMID 17381397.
- PMID 4937032.
- PMID 6813167.
- S2CID 30187238.
- PMID 4118696.
- S2CID 218989618.
- from the original on 2006-08-26.
- PMID 6258626.
- ^ a b c National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (n.d.). Appendicitis – Diagnosis. Retrieved September 21, 2023, from https://www.niddk.nih.gov/health-information/digestive-diseases/appendicitis/diagnosis
- ^ PMID 37143626.
- PMID 22977765.
- PMID 23247977.
- ^ Jones MW, Lopez RA, Deppen JG. Appendicitis. [Updated 2023 Apr 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan. Available from: https://www.ncbi.nlm.nih.gov/books/NBK493193/
- ^ ISBN 978-93-5025-777-7.
- ^ ISBN 978-3-030-29210-2.
- ISBN 978-1-4939-1726-6.
- ^ ISBN 978-1-4698-8948-1. Archivedfrom the original on 10 September 2017. Retrieved 15 June 2016.
Physical signs classically associated with acute appendicitis include Rovsing sign, psoas sign, and obturator sign.
- ^ Rovsing N (1907). "Indirektes Hervorrufen des typischen Schmerzes an McBurney's Punkt. Ein Beitrag zur diagnostik der Appendicitis und Typhlitis". Zentralblatt für Chirurgie (in German). 34. Leipzig: 1257–1259.
- ^ Dunster ES, Hunter JB, Sajous CE, Foster FP, Stragnell G, Klaunberg HJ, Martí-Ibáñez F (1922). International Record of Medicine and General Practice Clinics. New York Medical Journal. p. 663.
- ^ Emil Samuel Perman 1856–1946 "About the indications for surgery in appendicitis and an account of cases of Sabbatsberg Hospital in Hygiea 1904
- ^ a b c Gregory C (2010). "Appendicitis". CDEM Self Study Modules. Clerkship Directors in Emergency Medicine. Archived from the original on 2013-11-30.
- PMID 25541921.
- PMID 31687137.
- PMID 28747992.
- ^ Zhao, X., Yang, J. and Li, J. (2023) The predictive value of the C-reactive protein/albumin ratio in adult patients with complicated appendicitis. Journal of Laboratory Medicine. https://doi.org/10.1515/labmed-2023-0069
- PMID 17652298.
- ABIM Foundation, American College of Radiology, archived(PDF) from the original on April 16, 2012, retrieved August 17, 2012
- PMID 21324843.
- PMID 19098225.
- S2CID 46371675.
- ^ PMID 27087976.
- S2CID 78306243.
- S2CID 51677455.
- ^ a b "UOTW #45 - Ultrasound of the Week". Ultrasound of the Week. 25 April 2015. Archived from the original on 9 May 2017.
- PMID 31743429.
- PMID 25368849.
- PMID 25170393.
- PMID 19188320.
- ^ PMID 16928974.
- PMID 34905621.
- PMID 26215327.
- PMID 10452424.
- S2CID 23733164.
- ^ a b APPENDICITIS from Townsend: Sabiston Textbook of Surgery on MD Consult Archived December 3, 2013, at the Wayback Machine
- PMID 23177898.
- S2CID 202550141.
- S2CID 12566272.
- PMID 2349982.
- PMID 10684382.
- ^ "Pelvic inflammatory disease (PID) Symptoms; Diseases and Conditions". Mayo Clinic. Archived from the original on 2015-05-07. Retrieved 2015-04-23.
- PMID 20633930.
- )
- ^ "appendicitis". health n surgery. 15 June 2020. Archived from the original on 2020-10-25.
- PMID 26990957.
- S2CID 41805607.
- PMID 28346589.
- S2CID 222168573.
- S2CID 2292989.
- PMID 16034862.
- ^ from the original on 2013-05-17.
- PMID 30484855.
- PMID 6385879.
- ^ "Appendicitis". National Institute of Diabetes and Digestive and Kidney Diseases. U.S. Department of Health and Human Services. Archived from the original on 2010-02-01. Retrieved 2010-02-01.
- PMID 34402522.
- S2CID 45763958.
- PMID 14595145.
- S2CID 51941735.
- ^ "Appendicitis". Encyclopedia of Surgery. Archived from the original on 2010-02-09. Retrieved 2010-02-01.
- ^ "'Emergency' appendix surgery can wait: MDs". CBC News. 2010-09-21. Archived from the original on 2016-06-30.
- PMID 20855760.
Delay of appendectomy for acute appendicitis in adults does not appear to adversely affect 30-day outcomes.
- ^ Appendicitis surgery, removal and reco very Retrieved on 2010-02-01 Archived January 11, 2010, at the Wayback Machine
- S2CID 37041386.
- .
- ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 11 November 2020. Retrieved Nov 11, 2009.
- PMID 22411604.
- PMID 25530442.
- ^ Wier LM, Yu H, Owens PL, Washington R (June 2013). Overview of Children in the Emergency Department, 2010. Healthcare Cost and Utilization Project Statistical Brief #157 (Report). Agency for Healthcare Research and Quality. Archived from the original on 2013-12-03.
- PMID 23359540.
External links
- Appendicitis at Curlie
- CT of the abdomen showing acute appendicitis
- Appendicitis, history, diagnosis and treatment by Surgeons Net Education
- Appendicitis: Acute Abdomen and Surgical Gastroenterology from the Merck Manual Professional (content last modified September 2007)
- Appendicitis – Symptoms Causes and Treatment Archived 2021-02-27 at the Wayback Machine at Health N Surgery

![Ultrasound showing appendicitis and an appendicolith[58]](http://upload.wikimedia.org/wikipedia/commons/thumb/e/e0/UOTW_45_-_Ultrasound_of_the_Week_3.jpg/120px-UOTW_45_-_Ultrasound_of_the_Week_3.jpg)

![A normal appendix without and with compression. Absence of compressibility indicates appendicitis.[55]](http://upload.wikimedia.org/wikipedia/commons/thumb/3/3e/Ultrasonography_of_a_normal_appendix_without_and_with_compression.jpg/120px-Ultrasonography_of_a_normal_appendix_without_and_with_compression.jpg)