Cardiac arrest
| Cardiac arrest | |
|---|---|
| Other names | Cardiopulmonary arrest, circulatory arrest, sudden cardiac arrest (SCA) persistent vegetative state, post-cardiac arrest syndrome; if not reversed, death |
| Usual onset | The risk of onset increases with age[3] |
| Causes | Coronary artery disease, congenital heart defect, major blood loss, lack of oxygen, electrical injury, very low potassium, heart failure, myocardial infarction |
| Diagnostic method | Finding no pulse,[1] ECG (EKG)[4] |
| Prevention | Not smoking, physical activity, maintaining a healthy weight, healthy eating[5] |
| Treatment | Cardiopulmonary resuscitation (CPR), defibrillation[6] |
| Prognosis | Overall survival rate ≈10% (outside of hospital) 25% (in hospital);[7][8] depends strongly on type and cause |
| Frequency | 13 per 10,000 people per year (outside hospital in the US)[9] |
| Deaths | > 425,000 per year (U.S.)[10] |
Cardiac arrest, also known as sudden cardiac arrest, is when the heart suddenly and unexpectedly stops beating.
Cardiac arrest and resultant hemodynamic collapse often occur due to arrhythmias (irregular heart rhythms). Ventricular fibrillation and ventricular tachycardia are most commonly recorded.[12] However, as many incidents of cardiac arrest occur out-of-hospital or when a person is not having their cardiac activity monitored, it is difficult to identify the specific mechanism in each case.
Structural heart disease, such as coronary artery disease, is a common underlying condition in people who experience cardiac arrest. The most common risk factors include age and cardiovascular disease.[13] Additional underlying cardiac conditions include heart failure and inherited arrhythmias. Additional factors that may contribute to cardiac arrest include major blood loss, lack of oxygen, electrolyte disturbance (such as very low potassium), electrical injury, and intense physical exercise.[14]
Cardiac arrest is diagnosed by the inability to find a pulse in an unresponsive patient.[4][1] The goal of treatment for cardiac arrest is to rapidly achieve return of spontaneous circulation using a variety of interventions including CPR, defibrillation, and/or cardiac pacing. Two protocols have been established for CPR: basic life support (BLS) and advanced cardiac life support (ACLS).[15]
If return of spontaneous circulation is achieved with these interventions, then sudden cardiac arrest has occurred. By contrast, if the person does not survive the event, this is referred to as sudden cardiac death. Among those whose pulses are re-established, the care team may initiate measures to protect the person from brain injury and preserve neurological function.
Per the 2015 American Heart Association Guidelines, there are approximately 535,000 incidents of cardiac arrest annually (about 13 per 10,000 people).[9] Of these, 326,000 (61%) experience cardiac arrest outside of a hospital setting, while 209,000 (39%) occur within a hospital.[9]
Cardiac arrest becomes more common with age and affects males more often than females.[11] Twice as many black men die from a cardiac arrest as white men. Asian and Hispanic people are not as frequently affected as white people.[11]
Signs and symptoms
Cardiac arrest is not preceded by any warning symptoms in approximately 50 percent of people.
When cardiac arrest is suspected by a layperson (due to signs of unconsciousness, abnormal breathing, and/or no pulse) it should be assumed that the victim is in cardiac arrest. Bystanders should call emergency medical services (such as 911 or 112) and initiate CPR.
Risk factors
Major risk factors for cardiac arrest include age and underlying cardiovascular disease. A prior episode of sudden cardiac arrest increases the likelihood of future episodes.[21] A 2021 meta-analysis assessing the recurrence of cardiac arrest in out-of-hospital cardiac arrest survivors identified that 15% of survivors experienced a second event, most often in the first year.[22] Furthermore, of those who experienced recurrence, 35% had a third episode.[22]
Additional significant risk factors include
Causes and mechanisms
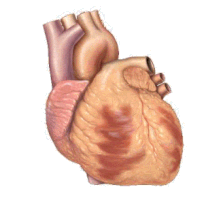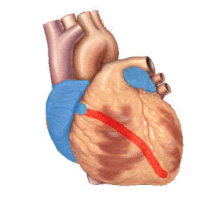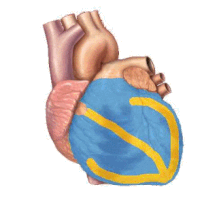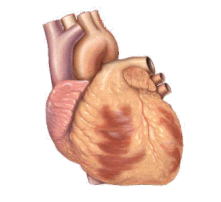
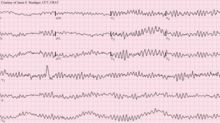
The underlying causes of sudden cardiac arrest can result from cardiac and non-cardiac etiologies. The most common underlying causes are different, depending on the patient's age. Common cardiac causes include coronary artery disease, non-atherosclerotic coronary artery abnormalities, structural heart damage, and inherited arrhythmias. Common non-cardiac causes include respiratory arrest, diabetes, medications, and trauma.
The most common mechanism underlying sudden cardiac arrest is an arrhythmia (an irregular rhythm).
There are many different types of arrhythmias, but the ones most frequently recorded in sudden cardiac arrest are ventricular tachycardia and ventricular fibrillation.[30][31] Both ventricular tachycardia and ventricular fibrillation can prevent the heart from generating coordinated ventricular contractions, thereby failing to sustain adequate blood circulation.
Less common types of arrhythmias occurring in cardiac arrest include pulseless electrical activity, bradycardia, and asystole.[28] These rhythms are seen when there is prolonged cardiac arrest, progression of ventricular fibrillation, or efforts like defibrillation executed to resuscitate the person.[28]
Cardiac causes
Coronary artery disease
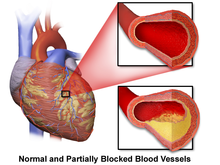
Coronary artery disease (CAD), also known as atherosclerotic cardiovascular disease, involves the deposition of cholesterol and subsequent inflammation-driven formation of atherosclerotic plaques in the arteries. CAD involves the accumulation and remodeling of the coronary vessels along with other systemic blood vessels.[32] When an atherosclerotic plaque dislodges, it can block the flow of blood and oxygen through small arteries, such as the coronary arteries, resulting in ischemic injury. In the heart, this results in myocardial tissue damage which can lead to structural and functional changes that disrupt normal conduction patterns and alter heart rate and contraction.[27]
CAD underlies 68 percent of sudden cardiac deaths in the United States.[33] Indeed, postmortem examinations have shown that the most common finding in cases of sudden cardiac death is chronic, high-grade stenosis of at least one segment of a major coronary artery.[34]
While CAD is a leading contributing factor, this is an age-dependent factor, with CAD being a less common cause of sudden cardiac death in people under the age of 40.[35]
Non-atherosclerotic coronary artery abnormalities
Abnormalities of the coronary arteries not related to atherosclerosis include inflammation (known as coronary arteritis), embolism, vasospasm, mechanical abnormalities related to connective tissue diseases or trauma, and congenital coronary artery anomalies (most commonly anomalous origin of the left coronary artery from the pulmonary artery). These conditions account for 10-15% of cardiac arrest and sudden cardiac death.[27]
- Coronary arteritis commonly results from a pediatric febrile inflammatory condition known as Kawasaki disease. Other types of vasculitis can also contribute to an increased risk of sudden cardiac death.
- Embolism, or clotting, of the coronary arteries most commonly occurs from septic emboli secondary to endocarditis with involvement of the aortic valve, tricuspid valve, or prosthetic valves.
- Coronary vasospasm may result in cardiac arrhythmias, altering the heart's electrical conduction with a risk of complete cardiac arrest from severe or prolonged rhythm changes.
- Mechanical abnormalities with an associated risk of cardiac arrest may arise from coronary artery dissection, which can be attributed to Marfan Syndrome or trauma.[27]
Structural heart disease

Examples of structural heart diseases include:
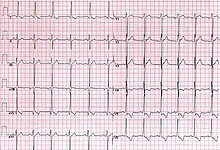
Left ventricular hypertrophy is a leading cause of sudden cardiac deaths in the adult population.[37][28] This is most commonly the result of longstanding high blood pressure, or hypertension, which has led to maladaptive overgrowth of muscular tissue of the left ventricle, the heart's main pumping chamber.[38] This is because elevated blood pressure over the course of several years requires the heart to adapt to the requirement of pumping harder to adequately circulate blood throughout the body. If the heart does this for a prolonged period of time, the left ventricle can experience hypertrophy (grow larger) in a way that decreases the heart's effectiveness.[39] Left ventricular hypertrophy can be demonstrated on an echocardiogram and electrocardiogram (EKG).[38]
Abnormalities of the cardiac conduction system (notably the Atrioventricular Node and His-Purkinje system) may predispose an individual to arrhythmias with a risk of progressing to sudden cardiac arrest, albeit this risk remains low. Many of these conduction blocks can be treated with internal cardiac defibrillators for those determined to be at high risk due to severity of fibrosis or severe electrophysiologic disturbances.[27]
Structural heart diseases unrelated to coronary artery disease account for 10% of all sudden cardiac deaths.[29][33] A 1999 review of sudden cardiac deaths in the United States found that structural heart diseases accounted for over 30% of sudden cardiac arrests for those under 30 years.[35][33]
Inherited arrhythmia syndromes
Arrhythmias not due to structural heart disease account for 5 to 10% of sudden cardiac arrests.
LQTS, a condition often mentioned in young people's deaths, occurs in one of every 5000 to 7000 newborns and is estimated to be responsible for 3000 deaths annually compared to the approximately 300,000 cardiac arrests seen by emergency services.[43] These conditions are a fraction of the overall deaths related to cardiac arrest but represent conditions that may be detected prior to arrest and may be treatable. The symptomatic expression of LQTS is quite broad and more often presents with syncope rather than cardiac arrest. The risk of cardiac arrest is still present, and people with family histories of sudden cardiac arrests should be screened for LQTS and other treatable causes of lethal arrhythmia. Higher levels of risk for cardiac arrest are associated with female sex, more significant QT prolongation, history of unexplained syncope (fainting spells), or premature sudden cardiac death.[27] Additionally, individuals with LQTS should avoid certain medications that carry the risk of increasing the severity of this conduction abnormality, such as certain anti-arrhythmics, anti-depressants, and quinolone or macrolide antibiotics.[44]
Another condition that promotes arrhythmias is Wolff-Parkinson-White syndrome, in which an accessory conduction pathway bypassing the atrioventricular node is present and can cause abnormal conduction patterns leading to supraventricular tachycardia and cardiac arrest.[29]
Non-cardiac causes
Non-cardiac causes account for 15 to 25% of cardiac arrests.[42][45] Common non-cardiac causes include respiratory arrest, diabetes, certain medications, and blunt trauma (especially to the chest).[3][46][47]
- Respiratory arrest will be followed by cardiac arrest unless promptly treated.[47] Respiratory arrest can be caused by pulmonary embolus, choking, drowning, trauma, drug overdose, and poisoning.[3] Pulmonary embolus carries a high mortality rate and may be the triggering cause for up to 5% of cardiac arrests, according to a retrospective study from an urban tertiary care emergency department.[48]
- Diabetes-related factors contributing to cardiac arrest include silent myocardial ischemia, nervous system dysfunction, and electrolyte disturbances leading to abnormal cardiac repolarization.[49]
- Certain medications can worsen an existing arrhythmia. Some examples include antibiotics like macrolides, diuretics, and heart medications such as anti-arrhythmic medications.[3]
Additional non-cardiac causes include hemorrhage, aortic rupture, hypovolemic shock, pulmonary embolism, poisoning such as from the stings of certain jellyfish, and electrical injury.[28][50][51][52]
Circadian patterns are also recognized as triggering factors in cardiac arrest.[53] Per a 2021 systematic review, throughout the day there are two main peak times in which cardiac arrest occurs. The first is in the morning hours and the second is in the afternoon.[54] Moreover, survival rates following cardiac arrest were lowest when occurring between midnight and 6am.[55]
Many of these non-cardiac causes of cardiac arrest are reversible. A common mnemonic used to recall the reversible causes of cardiac arrest is referred to as the Hs and Ts. The Hs are hypovolemia, hypoxia, hydrogen cation excess (acidosis), hyperkalemia, hypokalemia, hypothermia, and hypoglycemia. The Ts are toxins, (cardiac) tamponade, tension pneumothorax, thrombosis (myocardial infarction), thromboembolism, and trauma.
Mechanism
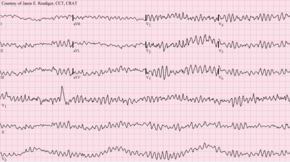
The definitive electrical mechanisms of cardiac arrest, which may arise from any of the functional, structural, or physiologic abnormalities mentioned above, are characterized by arrhythmias.[27] Ventricular fibrillation and pulseless or sustained ventricular tachycardia are the most commonly recorded arrhythmias preceding cardiac arrest. These are rapid and erratic arrhythmias that alter the circulatory pathway such that adequate blood flow cannot be sustained and is inadequate to meet the body's needs.[27]
The mechanism responsible for the majority of sudden cardiac deaths is ventricular fibrillation. Ventricular fibrillation is a tachyarrhythmia characterized by turbulent electrical activity in the ventricular myocardium leading to a heart rate too disorganized and rapid to produce any meaningful cardiac output, thus resulting in insufficient perfusion of the brain and essential organs.[56] Some of the electrophysiologic mechanisms underpinning ventricular fibrillations include ectopic automaticity, re-entry, and triggered activity.[57] However, structural changes in the diseased heart as a result of inherited factors (mutations in ion-channel coding genes, for example) cannot explain the sudden onset of cardiac arrest.[58]
In ventricular tachycardia, the heart also beats faster than normal, which may prevent the heart chambers from properly filling with blood.[59] Ventricular tachycardia is characterized by an altered QRS complex and a heart rate greater than 100 beats per minute.[60] When V-tach is sustained (lasts for at least 30 seconds), inadequate blood flow to heart tissue can lead to cardiac arrest.[61]
Bradyarrhythmias occur following dissociation of spontaneous electrical conduction and the mechanical function of the heart resulting in pulseless electrical activity (PEA) or through complete absence of electrical activity of the heart resulting in asystole. Similar to the result of tachyarrhythmias, these conditions lead to an inability to sustain adequate blood flow as well, though in the case of bradyarrhythmias, the underlying cause is an absence of mechanical activity rather than rapid beats leading to disorganization.[27]
Diagnosis

Cardiac arrest is synonymous with
Obtaining a thorough history can help inform the potential cause and prognosis.[28] The provider taking the person's clinical history should try to learn whether the episode was observed by anyone else, when it happened, what the patient was doing (in particular whether there was any trauma), and whether drugs were involved.[28]
During resuscitation efforts, continuous monitoring equipment including EKG leads should be attached to the patient so that providers can analyze the electrical activity of the cardiac cycle and use this information to guide the management efforts. EKG readings will help to identify the arrhythmia present and allow the team to monitor any changes that occur with the administration of CPR and defibrillation. Clinicians classify cardiac arrest into "shockable" versus "non-shockable", as determined by the
Point-of-care ultrasound (POCUS) is a tool that can be used to examine the movement of the heart and its force of contraction at the patient's bedside.[64] POCUS can accurately diagnose cardiac arrest in hospital settings, as well as visualize cardiac wall motion contractions.[64] Using POCUS, clinicians can have limited, two-dimensional views of different parts of the heart during arrest.[65] These images can help clinicians determine whether electrical activity within the heart is pulseless or pseudo-pulseless, as well as help them diagnose the potentially reversible causes of an arrest.[65] Published guidelines from the American Society of Echocardiography, American College of Emergency Physicians, European Resuscitation Council, and the American Heart Association, as well as the 2018 preoperative Advanced Cardiac Life Support guidelines, have recognized the potential benefits of using POCUS in diagnosing and managing cardiac arrest.[65]
POCUS can help predict outcomes in resuscitation efforts. Specifically, use of transthoracic ultrasound can be a helpful tool in predicting mortality in cases of cardiac arrest, with a systematic review from 2020 finding that there is a significant positive correlation between presence of cardiac motion and short term survival with CPR.[66]
Owing to the inaccuracy diagnosis solely based off central pulse detection, some bodies like the European Resuscitation Council have de-emphasized its importance. Instead, the current guidelines prompt individuals to begin CPR on any unconscious person with absent or abnormal breathing.[62] The Resuscitation Council in the United Kingdom stands in line with the European Resuscitation Council's recommendations and those of the American Heart Association.[15] They have suggested that the technique to check carotid pulses should be used only by healthcare professionals with specific training and expertise, and even then that it should be viewed in conjunction with other indicators like agonal respiration.[62]
Various other methods for detecting circulation and therefore diagnosing cardiac arrest have been proposed. Guidelines following the 2000 International Liaison Committee on Resuscitation recommendations were for rescuers to look for "signs of circulation" but not specifically the pulse.[15] These signs included coughing, gasping, color, twitching, and movement.[67] Per evidence that these guidelines were ineffective, the current International Liaison Committee on Resuscitation recommendation is that cardiac arrest should be diagnosed in all casualties who are unconscious and not breathing normally, a similar protocol to that which the European Resuscitation Council has adopted.[15] In a non-acute setting where the patient is expired, diagnosis of cardiac arrest can be done via molecular autopsy or postmortem molecular testing, which uses a set of molecular techniques to find the ion channels that are cardiac defective.[68] This could help elucidate the cause of death in the patient.
Other physical signs or symptoms can help determine the potential cause of the cardiac arrest.[28] Below is a chart of the clinical findings and signs/symptoms a person may have and potential causes associated with them.
| Location | Findings | Possible Causes |
|---|---|---|
| General | Pale skin | Hemorrhage |
| Decreased body temperature | Hypothermia | |
| Airway | Presence of secretions, vomit, blood | Aspiration |
| Inability to provide positive pressure ventilation | Tension pneumothorax | |
| Neck | Distension of the neck veins | Tension pneumothorax |
| Trachea shifted to one side | Tension pneumothorax | |
| Chest | Scar in the middle of the sternum | Cardiac disease |
| Lungs | Breath sounds only on one side | Tension pneumothorax
Aspiration |
| No breath sounds or distant breath sounds | Esophageal intubation
Airway obstruction | |
| Wheezing | Aspiration | |
| Rales | Aspiration
Pulmonary edema Pneumonia | |
| Heart | Decreased heart sounds | Hypovolemia
Cardiac tamponade Tension pneumothorax Pulmonary embolus |
| Abdomen | Distended and dull | Ruptured abdominal aortic aneurysm
Ruptured ectopic pregnancy |
| Distended and tympanic | Esophageal intubation | |
| Rectal | Blood present | Gastrointestinal hemorrhage |
| Extremities | Asymmetrical pulses | Aortic dissection |
| Skin | Needle tracks | Drug abuse |
Prevention
Primary prevention
With the lack of positive outcomes following cardiac arrest, efforts have been spent finding effective strategies to prevent cardiac arrest events. The approach to primary prevention promotes a healthy diet, exercise, limited alcohol consumption, and smoking cessation.[5]
Exercise is an effective preventative measure for cardiac arrest in the general population but may be risky for those with pre-existing conditions.[69] The risk of a transient catastrophic cardiac event increases in individuals with heart disease during and immediately after exercise.[69] The lifetime and acute risks of cardiac arrest are decreased in people with heart disease who perform regular exercise, perhaps suggesting the benefits of exercise outweigh the risks.[69]
A 2021 study found that diet may be a modifiable risk factor for a lower incidence of sudden cardiac death.[70] The study found that those who fell under the category of having "Southern diets" representing those of "added fats, fried food, eggs, organ and processed meats, and sugar‐sweetened beverages" had a positive association with an increased risk of cardiac arrest, while those deemed following the "Mediterranean diets" had an inverse relationship regarding the risk of cardiac arrest.[70] According to a 2012 review published, omega-3 PUFA supplementation is not associated with a lower risk of sudden cardiac death.[71]
A
Secondary prevention
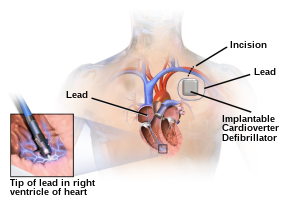
An implantable cardioverter-defibrillator (ICD) is a battery-powered device that monitors electrical activity in the heart, and when an arrhythmia is detected, can deliver an electrical shock to terminate the abnormal rhythm. ICDs are used to prevent sudden cardiac death (SCD) in those who have survived a prior episode of sudden cardiac arrest (SCA) due to ventricular fibrillation or ventricular tachycardia.[73]
Numerous studies have been conducted on the use of ICDs for the secondary prevention of SCD. These studies have shown improved survival with ICDs compared to the use of anti-arrhythmic drugs.[73] ICD therapy is associated with a 50% relative risk reduction in death caused by an arrhythmia and a 25% relative risk reduction in all-cause mortality.[74]
Prevention of SCD with ICD therapy for high-risk patient populations has similarly shown improved survival rates in several large studies. The high-risk patient populations in these studies were defined as those with severe ischemic cardiomyopathy (determined by a reduced left ventricular ejection fraction (LVEF)). The LVEF criteria used in these trials ranged from less than or equal to 30% in MADIT-II to less than or equal to 40% in MUSTT.[73][75]
In certain high-risk patient populations (such as patients with LQTS), ICDs are also used to prevent sudden cardiac death (primary prevention).[75]
Crash teams
In hospital, a cardiac arrest is referred to as a "crash", or a "code". This typically refers to
Patients in general wards often deteriorate for several hours or even days before a cardiac arrest occurs.[62][76] This has been attributed to a lack of knowledge and skill amongst ward-based staff, in particular, a failure to measure the respiratory rate, which is often the major predictor of a deterioration[62] and can often change up to 48 hours prior to a cardiac arrest. In response, many hospitals now have increased training for ward-based staff. A number of "early warning" systems also exist that aim to quantify the person's risk of deterioration based on their vital signs and thus provide a guide to staff. In addition, specialist staff are being used more effectively to augment the work already being done at the ward level. These include:
- Crash teams (or code teams) – These are designated staff members with particular expertise in resuscitation who are called to the scene of all arrests within the hospital. This usually involves a specialized cart of equipment (including a defibrillator) and drugs called a "crash cart" or "crash trolley".
- Medical emergency teams – These teams respond to all emergencies with the aim of treating people in the acute phase of their illness in order to prevent a cardiac arrest. These teams have been found to decrease the rates of in-hospital cardiac arrest (IHCA) and improve survival.[9]
- Critical care outreach – In addition to providing the services of the other two types of teams, these teams are responsible for educating non-specialist staff. In addition, they help to facilitate transfers between intensive care/high dependency units and the general hospital wards. This is particularly important as many studies have shown that a significant percentage of patients discharged from critical care environments quickly deteriorate and are re-admitted; the outreach team offers support to ward staff to prevent this from happening.[citation needed]
Management
Sudden cardiac arrest may be treated via attempts at

Cardiopulmonary resuscitation
Early
Correctly performed bystander CPR has been shown to increase survival, however it is performed in fewer than 30% of out-of-hospital cardiac arrests (OHCAs) as of 2007[update].[82] A 2019 meta-analysis found that use of dispatcher-assisted CPR improved outcomes, including survival, when compared with undirected bystander CPR.[83] Likewise, a 2022 systematic review on exercise-related cardiac arrests supported early intervention of bystander CPR and AED use (for shockable rhythms) as they improve survival outcomes.[84]
If high-quality CPR has not resulted in return of spontaneous circulation and the person's heart rhythm is in
If cardiac arrest occurs after 20 weeks of pregnancy, the uterus should be pulled or pushed to the left during CPR.
Airway management
High levels of oxygen are generally given during CPR.[80] Either a bag valve mask or an advanced airway may be used to help with breathing particularly since vomiting and regurgitation are common, especially in OHCA.[80][87][88] If this occurs, then modification to existing oropharyngeal suction may be required, such as using suction-assisted airway management.[89]
Mouth-to-mouth as a means of providing respirations to the person has been phased out due to the risk of contracting infectious diseases from the affected person.[92]
When done by emergency medical personnel, 30 compressions followed by two breaths appear to be better than continuous chest compressions and breaths being given while compressions are ongoing.[93] For bystanders, CPR that involves only chest compressions results in better outcomes as compared to standard CPR for those who have gone into cardiac arrest due to heart issues.[93]
Defibrillation

Defibrillation is indicated if an electric-shockable heart rhythm is present. The two shockable rhythms are
Ventricular fibrillation involves the ventricles of the heart (lower chambers responsible for pumping blood) rapidly contracting in an disorganized pattern, and thereby limiting blood flow from the heart. This can be due to uncoordinated electrical activity.[95] The electrocardiogram (ECG) generally shows irregular QRS complexes without P-waves.[96] By contrast, the ECG for ventricular tachycardia will generally show a wide complex QRS with more than 100 beats occurring per minute.[97] If sustained, ventricular tachycardia can also lead hemodynamic instability and compromise, resulting in pulselessness and poor perfusion to vital organs.
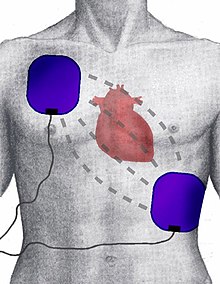
A defibrillator will deliver an electrical current through a pair of electrodes placed on the person's chest. This is thought to depolarize myocardial tissue thereby stopping the arrhythmia.[98] Defibrillators can deliver energy as monophasic or biphasic waveforms, although biphasic defibrillators are the most common.[99][100]
For ventricular fibrillation, defibrillation techniques may utilized either monophasic or biphasic waveforms. Prior studies suggest that biphasic shock is more likely to produce successful defibrillation after a single shock, however rate of survival is comparable between the methods.[100]
In out-of-hospital arrests, the defibrillation is made by an automated external defibrillator (AED), a portable machine that can be used by any user. The AED provides voice instructions that guide the process, automatically checks the person's condition, and applies the appropriate electric shocks. Some defibrillators even provide feedback on the quality of CPR compressions, encouraging the lay rescuer to press the person's chest hard enough to circulate blood.[101]
In addition, there is increasing use of public access defibrillation. This involves placing AEDs in public places and training staff in these areas on how to use them. This allows defibrillation to occur prior to the arrival of emergency services, which has been shown to increase chances of survival. People who have cardiac arrests in remote locations have worse outcomes following cardiac arrest.[102]
Defibrillation is applied to certain arrhythmias such as ventricular fibrillation and pulseless ventricular tachycardia. Defibrillation cannot be applied to asystole, and CPR must be initiated first in this case. Moreover, defibrillation is different than synchronized cardioversion. In synchronized cardioversion, a similar approach is utilized in that electrical current is applied to correct an arrhythmia, however this is used in cases where a pulse is present but the patient is hemodynamically unstable, such as supraventricular tachycardia.
Defibrillators may also be used as part of post-cardiac arrest management. These defibrillators include wearable defibrillator (such as LifeVest), subcutaneous cardiac defibrillator, and implantable cardiac defibrillator.[103]
Medications
Medications recommended in the ACLS protocol include epinephrine, amiodarone, and lidocaine.[9] The timing and administration of these medications depends on the underlying arrhythmia of the arrest.
Epinephrine acts on the alpha-1 receptor, which in turn increases the blood flow that supplies the heart.[104] Epinephrine in adults improves survival[105] but does not appear to improve neurologically normal survival.[106] In ventricular fibrillation and pulseless ventricular tachycardia, 1 mg of epinephrine is given every 3–5 minutes, following an initial round of CPR and defibrillation.[80] Doses higher than 1 mg of epinephrine are not recommended for routine use in cardiac arrest. If the person has a non-shockable rhythm, such as asystole, following an initial round of CPR, 1 mg of epinephrine should be given every 3–5 minutes, with the goal of obtaining a shockable rhythm.[107]
Additional medications
Bicarbonate, given as sodium bicarbonate, works to stabilize acidosis and hyperkalemia, both of which can contribute to and exacerbate cardiac arrest. If acid-base or electrolyte disturbance is evident, bicarbonate may be used. However, if there is little suspicion that these imbalances are occurring and contributing to the arrest, routine use of bicarbonate is not recommended as it does not provide additional benefit.[111]
Vasopressin overall does not improve or worsen outcomes compared to epinephrine.[80] The combination of epinephrine, vasopressin, and methylprednisolone appears to improve outcomes.[113]
The use of atropine, lidocaine, and amiodarone have not been shown to improve survival from cardiac arrest.[114][115][79]
Atropine is used for symptomatic bradycardia. It is given at a does of 1 mg (iv), and additional 1 mg (iv) doses can be given every 3–5 minutes for a total of 3 mg. However, the 2010 guidelines from the American Heart Association removed the recommendation for atropine use in pulseless electrical activity and asystole for lack of evidence supporting its use.[116][79]
Special considerations
Hemodialysis patients carry a greater risk of cardiac arrest events. Multiple factors contribute including increased cardiovascular risk factors, electrolyte disturbances (calcium and potassium, caused by accumulation and aggressive removal), and acid-base disturbances.[117] Calcium levels are considered a key factor contributing to cardiac arrests in this population.[118]
Tricyclic antidepressant (TCA) overdose can lead to cardiac arrest with typical ECG findings including wide QRS and prolonged QTc. Treatment for this condition includes activated charcoal and sodium bicarbonate.[119]
Magnesium can be given at a does of 2 g (iv or oral bolus) to manage
Targeted temperature management
Current international guidelines suggest cooling adults after cardiac arrest using targeted temperature management (TTM) with the goal of improving neurological outcomes.[122] The process involves cooling for a 24-hour period, with a target temperature of 32–36 °C (90–97 °F), followed by gradual rewarming over the next 12 to 24 hrs.[123][124] There are several methods used to lower the body temperature, such as applying ice packs or cold-water circulating pads directly to the body or infusing cold saline.
The effectiveness of TTM after OHCA is an area of ongoing study. Several recent reviews have found that patients treated with TTM have more favorable neurological outcomes.
Do not resuscitate
Some people choose to avoid aggressive measures at the end of life. A
Chain of survival
Several organizations promote the idea of a chain of survival. The chain consists of the following "links":
- Early recognition. If possible, recognition of illness before the person develops a cardiac arrest will allow the rescuer to prevent its occurrence. Early recognition that a cardiac arrest has occurred is key to survival, for every minute a patient stays in cardiac arrest, their chances of survival drop by roughly 10%.[62]
- Early CPR improves the flow of blood and of oxygen to vital organs, an essential component of treating a cardiac arrest. In particular, by keeping the brain supplied with oxygenated blood, the chances of neurological damage are decreased.
- Early defibrillation is effective for the management of ventricular fibrillation and pulseless ventricular tachycardia.[62]
- Early advanced care.
- Early post-resuscitation care, which may include percutaneous coronary intervention.[129]
If one or more links in the chain are missing or delayed, then the chances of survival drop significantly.
These protocols are often initiated by a
Other
Resuscitation with extracorporeal membrane oxygenation devices has been attempted with better results for in-hospital cardiac arrest (29% survival) than OHCA (4% survival) in populations selected to benefit most.[131]
Cardiac catheterization in those who have survived an OHCA appears to improve outcomes, although high-quality evidence is lacking.[132] It is recommended to be done as soon as possible in those who have had a cardiac arrest with ST elevation due to underlying heart problems.[80]
The precordial thump may be considered in those with witnessed, monitored, unstable ventricular tachycardia (including pulseless VT) if a defibrillator is not immediately ready for use, but it should not delay CPR and shock delivery or be used in those with unwitnessed OHCA.[133]
Prognosis
The overall rate of survival among those who have OHCA is 10%.
A 1997 review found rates of survival to discharge of 14%, although different studies varied from 0 to 28%.[140] In those over the age of 70 who have a cardiac arrest while in hospital, survival to hospital discharge is less than 20%.[141] How well these individuals manage after leaving the hospital is not clear.[141]
The global rate of people who were able to recover from OHCA after receiving CPR has been found to be approximately 30%, and the rate of survival to discharge from the hospital has been estimated at 9%.[142] Survival to discharge from the hospital is more likely among people whose cardiac arrest was witnessed by a bystander or emergency medical services, who received bystander CPR, and who live in Europe and North America.[142] Relatively lower survival to hospital discharge rates have been observed in Asian countries.[142]
Prognosis is typically assessed 72 hours or more after cardiac arrest.[143] Rates of survival are better in those who had someone witness their collapse, received bystander CPR, and/or had either V-fib or V-tach when assessed.[144] Survival among those with V-fib or V-tach is 15 to 23%.[144] Women are more likely to survive cardiac arrest and leave the hospital than men.[145] Hypoxic ischemic brain injury is a concerning outcome for people suffering a cardiac arrest.[146] Most improvements in cognition occur during the first three months following cardiac arrest, with some individuals reporting improvement up to one year post-cardiac arrest.[146] 50 – 70% of cardiac arrest survivors report fatigue as a symptom.[146]
Epidemiology
North America
The risk of cardiac arrest varies with geographical region, age, and gender. The lifetime risk is three times greater in men (12.3%) than women (4.2%) based on analysis of the Framingham Heart Study.[147] This gender difference disappeared beyond 85 years of age.[148] Around half of these individuals are younger than 65 years of age.[149]
Based on death certificates, sudden cardiac death accounts for about 20% of all deaths in the United States.[150][151] In the United States, approximately 326,000 cases of out-of-hospital and 209,000 cases of IHCA occur among adults annually, which works out to be an incidence of approximately 110.8 per 100,000 adults per year.[9][79][150]
In the United States, during-pregnancy cardiac arrest occurs in about one in twelve-thousand deliveries or 1.8 per 10,000 live births.[86] Rates are lower in Canada.[86]
Other regions
Non-Western regions of the world have differing incidences. The incidence of sudden cardiac death in China is 41.8 per 100,000 and in South India is 39.7 per 100,000.[150]
Society and culture
Names
In many publications, the stated or implicit meaning of "sudden cardiac death" is sudden death from cardiac causes.[152] Some physicians call cardiac arrest "sudden cardiac death" even if the person survives. Thus one can hear mentions of "prior episodes of sudden cardiac death" in a living person.[153]
In 2021, the American Heart Association clarified that "heart attack" is often mistakenly used to describe cardiac arrest. While a heart attack refers to death of heart muscle tissue as a result of blood supply loss, cardiac arrest is caused when the
Slow code
A "slow code" is a slang term for the practice of deceptively delivering sub-optimal CPR to a person in cardiac arrest, when CPR is considered to have no medical benefit.[155] A "show code" is the practice of faking the response altogether for the sake of the person's family.[156]
Such practices are ethically controversial[157] and are banned in some jurisdictions. The European Resuscitation Council Guidelines released a statement in 2021 that clinicians are not suggested to participate/take part in "slow codes".[155] According to the American College of Physicians, half-hearted resuscitation efforts are deceptive and should not be performed by physicians or nurses.[158]
Children
In children, the most common cause of cardiac arrest is shock or respiratory failure that has not been treated.[28] Cardiac arrhythmias are another possible cause. Arrhythmias such as asystole or bradycardia are more likely in children, in contrast to ventricular fibrillation or tachycardia as seen in adults.[28]
Additional causes of sudden unexplained cardiac arrest in children include hypertrophic cardiomyopathy and coronary artery abnormalities.[159] In childhood hypertrophic cardiomyopathy, previous adverse cardiac events, non-sustained ventricular tachycardia, syncope, and left ventricular hypertrophy have been shown to predict sudden cardiac death.[160] Other causes can include drugs, such as cocaine and methamphetamine, or overdose of medications, such as antidepressants.[28]
For management of pediatric cardiac arrest, CPR should be initiated if suspected. Guidelines provide algorithms for pediatric cardiac arrest management. Recommended medications during pediatric resuscitation include epinephrine, lidocaine, and amiodarone.[161][79][80] However, the use of sodium bicarbonate or calcium is not recommended.[80][162] The use of calcium in children has been associated with poor neurological function as well as decreased survival.[28] Correct dosing of medications in children is dependent on weight, and to minimize time spent calculating medication doses, the use of a Broselow tape is recommended.[28]
Rates of survival in children with cardiac arrest are 3 to 16% in North America.[161]
See also
References
- ^ ISBN 9780781788991. Archivedfrom the original on 2017-09-05.
- ^ "Cardiac Arrest - Symptoms | NHLBI, NIH". www.nhlbi.nih.gov. 27 May 2022. Retrieved 20 September 2023.
- ^ a b c d "Cardiac Arrest - Causes and Risk Factors | NHLBI, NIH". www.nhlbi.nih.gov. 19 May 2022. Retrieved 30 September 2023.
- ^ a b "Cardiac Arrest - Diagnosis | NHLBI, NIH". National Heart, Lung, and Blood Institute, US National Institutes of Health. 19 May 2022. Retrieved 3 October 2022.
- ^ a b c "How Can Death Due to Sudden Cardiac Arrest Be Prevented?". NHLBI. June 22, 2016. Archived from the original on 27 August 2016. Retrieved 16 August 2016.
- ^ "Cardiac Arrest - Treatment". National Heart, Lung, and Blood Institute, US National Institutes of Health. 19 May 2022. Retrieved 24 July 2022.
- ISBN 978-1455733941. Archivedfrom the original on 2017-09-05.
- PMID 30912843.
- ^ S2CID 10073267.
- PMID 23801105.
- ^ a b c d "Cardiac Arrest - What Is Cardiac Arrest? | NHLBI, NIH". www.nhlbi.nih.gov. 19 May 2022. Retrieved 20 September 2023.
- PMID 2911968.
- ^ PMID 14581249.
- PMID 11684624.
- ^ PMID 16314375.
- PMID 18948368.
- ^ PMID 27521472.
- ^ PMID 37217440.
- ^ OCLC 890409638.
- ^ a b "What Are the Signs and Symptoms of Sudden Cardiac Arrest?". National Heart, Lung and Blood Institute. 1 April 2011. Archived from the original on 21 June 2015. Retrieved 2015-06-21.
- OCLC 893557976.
- ^ S2CID 248569642.
- PMID 9445167.
- PMID 35041932.
- PMID 9270951.
- S2CID 245422237.
- ^ OCLC 881838985.
- ^ OCLC 989157341.
- ^ a b c Podrid PJ (2016-08-22). "Pathophysiology and etiology of sudden cardiac arrest". www.uptodate.com. Retrieved 2017-12-03.
- PMID 16935995.
- PMID 33385322.
- PMID 29939576. Retrieved 2021-11-05.
- ^ PMID 11684624.
- ISBN 9780781735834. Archivedfrom the original on 2016-06-03.
- ^ PMID 11898927.
- PMID 9704680.
- PMID 23424223.
- ^ PMID 21755036.
- PMID 32491466. Retrieved 2021-11-05.
- PMID 10931805.
- PMID 8994445.
- ^ PMID 1951130.
- ^ "Sudden Cardiac Death". American Heart Association. Archived from the original on 2010-03-25.
- PMID 23675554.
- PMID 9243146.
- PMID 25572990.
- ^ PMID 29940296.
- PMID 10826469.
- PMID 20544609.
- PMID 20449913.
- PMID 10960389.
- PMID 28444167.
- PMID 3661393.
- S2CID 233349757.
- S2CID 233349757.
- ^ "Ventricular tachycardia - Symptoms and causes". Mayo Clinic. Retrieved 2021-11-29.
- PMID 32140103.
- PMID 16138184.
- ^ "Ventricular fibrillation - Symptoms and causes". Mayo Clinic. Retrieved 2021-11-29.
- S2CID 199437558.
- PMID 27484660.
- ^ a b c d e f g "Resuscitation Council (UK) Guidelines 2005". Archived from the original on 2009-12-15.
- ISBN 9781118474853. Archivedfrom the original on 2017-09-05.
- ^ S2CID 3874849.
- ^ S2CID 234486749.
- PMID 31931808.
- ISBN 978-1-4053-1573-9.
- ISBN 978-1-84628-026-9
- ^ PMID 31308007.
- ^ PMID 34189926.
- PMID 22968891.
- PMID 26961575.
- ^ PMID 18483207.
- PMID 11102258.
- ^ PMID 28329280.
- PMID 15325446.
- S2CID 46720891.
- ^ "AHA Releases 2015 Heart and Stroke Statistics | Sudden Cardiac Arrest Foundation". www.sca-aware.org. Retrieved 21 September 2019.
- ^ OCLC 957505642.
- ^ PMID 26472989.
- PMID 25212112.
- ^ PMID 17200636.
- S2CID 73727100.
- S2CID 244800392.
- ^ a b Resuscitation Council (UK). "Pre-hospital cardiac arrest" (PDF). www.resus.org.uk. p. 41. Archived (PDF) from the original on 13 May 2015. Retrieved 3 September 2014.
- ^ PMID 26472998.
- PMID 17433526.
- ^
Voss S, Rhys M, Coates D, Greenwood R, Nolan JP, Thomas M, Benger J (December 2014). "How do paramedics manage the airway during out of hospital cardiac arrest?". Resuscitation. 85 (12): 1662–1666. PMID 25260723.
- ^
Root CW, Mitchell OJ, Brown R, Evers CB, Boyle J, Griffin C, et al. (2020-03-01). "Suction Assisted Laryngoscopy and Airway Decontamination (SALAD): A technique for improved emergency airway management". Resuscitation Plus. 1–2: 100005. PMID 34223292.
- ^ S2CID 52931036.
- PMID 20836771.
- PMID 10824072.
- ^ PMID 28349529.
- PMID 32504821.
- ^ "Arrhythmias - What Is an Arrhythmia? | NHLBI, NIH". www.nhlbi.nih.gov. 2022-03-24. Retrieved 2024-01-31.
- PMID 30725805. Retrieved 2024-01-31.
- PMID 30422549. Retrieved 2024-01-31.
- ^ Knight BP (23 January 2023). Page RL, Dardas TF (eds.). "Basic principles and technique of external electrical cardioversion and defibrillation". UpToDate. Retrieved 2024-01-18.
- PMID 10869271.
- ^ PMID 11023932.
- ^ "Zoll Automated External Defibrillator (AED) Plus". Life Assistance Training. Archived from the original on 2011-06-21.
- PMID 15333549.
- S2CID 53272603.
- ^ "Deep Dive into the Evidence: Epinephrine in Cardiac Arrest". www.emra.org. Retrieved 2021-11-12.
- S2CID 207940828.
- S2CID 208537959.
- S2CID 208019248.
- PMID 29489285. Retrieved 2024-01-31.
- PMID 30969703. Retrieved 2024-01-31.
- PMID 27496262.
- S2CID 260893519.
- PMID 36238582.
- (PDF) from the original on 5 March 2020.
- PMID 29037886.
- (PDF) from the original on 5 March 2020.
- PMID 20956224.
- PMID 28223004.
- S2CID 5503149.
- PMID 17453872.
- ISSN 2543-5957.
- S2CID 11006778.
- ^ PMID 29534742.
- PMID 26472989.
- OCLC 802346256.
- PMID 29239942.
- ^ S2CID 19236851.
- PMID 20102982.
- PMID 16308044.
- PMID 27640933.
- PMID 25215142.
- PMID 22930866.
- S2CID 207517242.
- PMID 20956223.
- PMID 28122885.
- PMID 29084732.
- PMID 26225413.
- PMID 27994023.
- ^ S2CID 52270938.
- S2CID 10073267.
- PMID 9167565.
- ^ PMID 24760957.
- ^ PMID 32087741.
- PMID 26472989.
- ^ PMID 20123673.
- PMID 26143159.
- ^ S2CID 232408830.
- doi:10.1161/circ.120.suppl_18.S416-c (inactive 31 January 2024).)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - PMID 11684624.
- OCLC 957505642.
- ^ S2CID 53744984.
- S2CID 238581415.
- OCLC 1134470998.
- PMID 18513397.
- S2CID 231762900.
- ^ OCLC 1258336024.
- ^ "Slow Codes, Show Codes and Death". The New York Times. 22 August 1987. Archived from the original on 18 May 2013. Retrieved 2013-04-06.
- PMID 10646457. Archived from the originalon 2013-03-28. Retrieved 2013-04-07.
- S2CID 58004782.
- S2CID 224826594.
- S2CID 206821305.
- ^ PMID 26473000.
- PMID 26985247.
