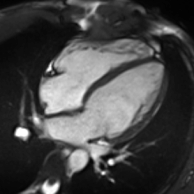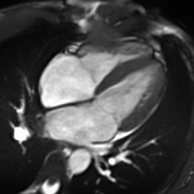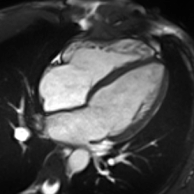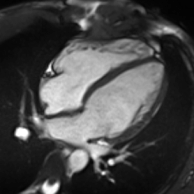
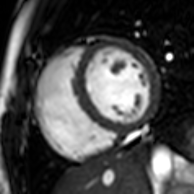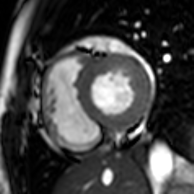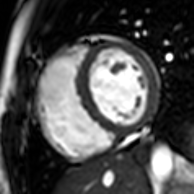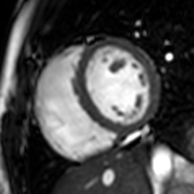
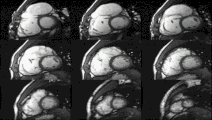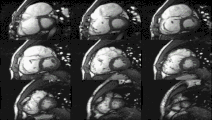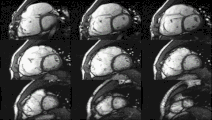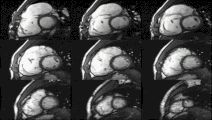
Cardiac magnetic resonance imaging
| Cardiac magnetic resonance imaging | |
|---|---|
| ICD-10-PCS | B23 |
| ICD-9-CM | 88.92 |
| OPS-301 code | 3-803, 3-824 |
Cardiac magnetic resonance imaging (cardiac MRI, CMR), also known as cardiovascular MRI, is a
.It is contraindicated if there are some implanted metal or electronic devices such as some intracerebral clips or claustrophobia.[3] These can be looked up to see if they are MRI conditional. For pacemaker or defibrillator patients, almost all can be scanned but special protocols are needed.
Conventional
Uses
Cardiovascular MRI is complementary to other imaging techniques, such as
Combined with
Obstacles to its wider application include limited access to scanners, lack of technologists and skilled clinicians, relatively high costs, and competing diagnostic modalities.[4] Some organizations are working on solutions to reduce these obstacles so that more clinics can adopt CMR into their practices. These solutions are often software platforms that provide clinical decision support and improve the efficiency of the procedures.[10]
Risks
Cardiac MRI does not pose any specific risks compared to other indications for imaging.
Physics
CMR uses the same basic principles as other
Techniques
A CMR study typically comprises a set of sequences in a protocol tailored to the specific indication for the exam.[21] A study begins with localisers to assist with image planning, and then a set of retrospectively-gated cine sequences to assess biventricular function in standard orientations. Contrast medium is given intravenously to assess myocardial perfusion and LGE. Phase contrast imaging may be used to quantify valvular regurgitant fraction and shunt volume. Additional sequences may include T1 and T2-weighted imaging and MR angiography. Examples are below:
Heart function using cine imaging
Functional and structural information is acquired using bSSFP cine sequences. These are usually retrospectively-gated and have intrinsically high contrast in cardiac imaging due to the relatively high T2:T1 ratio of blood compared to myocardium. Images are typically planned sequentially to achieve the standard cardiac planes used for assessment. Turbulent flow causes dephasing and signal loss allowing valvular disease to be qualitatively appreciated. The left ventricular short axis cines are acquired from base to apex and are used for quantifying end-diastolic and end-systolic volumes, as well as myocardial mass. Tagging sequences excite a grid pattern that deforms with cardiac contraction allowing strain to be assessed.
Late gadolinium enhancement
Gadolinium-based contrast agents are administered intravenously and delayed imaging is performed at least 10 minutes later to achieve optimum contrast between normal and infarcted myocardium. An inversion recovery (IR) sequence is used to null the signal from normal myocardium. Myocardial viability can be assessed by the degree of transmural enhancement. Cardiomyopathic, inflammatory and infiltrative diseases may also have distinctive patterns of non-ischemic LGE.[22][23]
Perfusion
Adenosine is used as a vasodilator, via the A2A receptor, to increase the difference in perfusion between myocardial territories supplied by normal and stenosed coronary arteries. A continuous intravenous infusion is administered for a few minutes until there are hemodynamic signs of vasodilatation, then a bolus of contrast medium is administered while acquiring saturation recovery images of the heart with a high temporal resolution readout. A positive result is evident from an inducible myocardial perfusion defect. Cost and availability mean that its use is often confined to patients with intermediate pre-test probability,[24] but it has been shown to reduce unnecessary angiography compared with guidelines-directed care.[25]

4D flow CMR
Conventional phase contrast imaging can be extended by applying flow-sensitive gradients in 3 orthogonal planes within a 3D volume throughout the cardiac cycle. Such 4D imaging encodes the velocity of flowing blood at each voxel in the volume enabling fluid dynamics to be visualised using specialist software. Applications are in complex congenital heart disease and for research into cardiovascular flow characteristics - however it is not in routine clinical use due to the complexity of post-processing and relatively long acquisition times.[26]
Children and congenital heart disease
Rather, it is typically used in concert with other diagnostic techniques. In general, the clinical reasons for a CMR examination fall into one or more of the following categories: (1) when
Atrial septal defect with dilation of the right ventricle by CMR
Partial Anomalous Pulmonary Venous Drainage by CMR
CMR examinations in children typically last 15 to 60 minutes. In order to avoid blurry images the child must remain very still during the examination. Different institutions have different protocols for pediatric CMR, but most children 7 years of age and older can cooperate sufficiently for a good quality examination. Providing an age-appropriate explanation of the procedure to the child in advance will increase the likelihood of a successful study. After proper safety screening, parents can be allowed into the MRI scanner room to help their child complete the examination. Some centers allow children to listen to music or watch movies through a specialized MRI-compatible audiovisual system to reduce anxiety and improve cooperation. However, the presence of a calm, encouraging, supportive parent generally produces better results in terms of pediatric cooperation than any distraction or entertainment strategy short of sedation. If the child cannot cooperate sufficiently, sedation with intravenous medications or general anesthesia may be necessary. In very young babies, it may be possible to perform the examination while they are in a natural sleep. New image capture techniques such as 4D flow require a shorter scan and can lead to reduced needs for sedation.
Enlarged right ventricle with poor function in a patient with repaired tetralogy of Fallot by CMR
Different cardiac-capable magnet types
The majority of CMR is performed on conventional superconducting MRI systems at either 1.5T or 3T.[27] Imaging at 3T field strength offers greater signal to noise ratio which can be traded for improved temporal or spatial resolution – which is of greatest utility in first-pass perfusion studies.[28] However, greater capital costs and effects of off-resonance artefact on image quality mean that many studies are routinely performed at 1.5T.[29] Imaging at 7T field strength is a growing area of research, but is not widely available.[30]
Current manufacturers of cardiac-capable MRI scanners include Philips, Siemens, Hitachi, Toshiba, GE.
History
The phenomenon of
As MRI became more complex and application to cardiovascular imaging became more sophisticated, the Society for Cardiovascular Magnetic Resonance (SCMR) was set up (1996) with an academic journal, Journal of Cardiovascular Magnetic Resonance (JCMR) in 1999. In a move analogous to the development of 'echocardiography' from cardiac ultrasound, the term 'cardiovascular magnetic resonance' (CMR) was proposed and has gained acceptance as the name for the field.
CMR is increasingly recognized as a quantitative imaging modality for evaluation of the heart. The reporting of CMR exams involves manual work and visual assessment. In recent years, with the development of artificial intelligence techniques, the reporting and analysis of cardiac MRI are expected to be more efficient, facilitated by automatic deep learning tools.[32]
Training
Certification of competency in CMR can be obtained at three levels, with different requirements for each. Level 3 requires 50 hours of approved courses, at least 300 studies performed, sitting a written examination and recommendation by a supervisor.[33]
References
- ^ "Case of the Week Number 06-01. Left Atrial Myxoma". Society for Cardiovascular Magnetic Resonance. 2016-10-21. Archived from the original on 2009-01-16. Retrieved 2016-12-02.
- ^ PMID 29386064.
- ^ ISBN 978-0-7020-7870-5.
- ^ PMID 28942735.
- PMID 26800662.
- PMID 28178995.
- PMID 26424866.
- S2CID 23647168.
- OCLC 1019592102.[page needed]
- ^ "Cohesic cardioDI MR".
- PMID 28267552.
- S2CID 44818510.
- PMID 23793096.
- S2CID 205467617.
- PMID 18804118.
- PMID 11682641.
- PMID 29165554.
- PMID 29281062.
- PMID 22033762.
- PMID 27899132.
- PMID 24103764.
- PMID 23909638.
- PMID 31585768.
- ^ "Chest pain of recent onset: assessment and diagnosis". National Institute for Care and Health Excellence. 24 March 2010. Retrieved 2018-02-25.
- S2CID 205073777.
- PMID 26257141.
- ^ "Magnetic Resonance Imaging (MRI) Equipment, Operations and Planning in the NHS" (PDF). Royal College of Radiologists. 2017-04-01. Retrieved 2018-02-25.
- PMID 25497243.
- PMID 25310420.
- PMID 20676653.
- PMID 5110317.
- S2CID 204974611.
- PMID 24855220.
External links
- The Society for Cardiovascular Magnetic Resonance Archived 2020-11-04 at the Wayback Machine
- The Journal for Cardiovascular Magnetic Resonance
- An Atlas of normal cardiac structure and function by CMR
- Having a CMR scan Archived 2021-02-27 at the Wayback Machine
- Cardiac MRI, Technical Aspects Primer at eMedicine
- the basics of MRI
- MRI tutor