Cerebral arteriovenous malformation
| Cerebral arteriovenous malformation | |
|---|---|
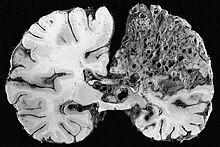 | |
| Large arteriovenous malformation of the parietal lobe | |
| Specialty | Medical genetics |
A cerebral arteriovenous malformation (cerebral AVM, CAVM, cAVM, brain AVM, or BAVM) is an abnormal connection between the
Signs and symptoms
The most frequently observed problems related to a cerebral
In serious cases,
AVMs in certain critical locations may stop the circulation of the cerebrospinal fluid, causing it to accumulate within the skull and giving rise to a clinical condition called hydrocephalus.[5] A stiff neck can occur as the result of increased pressure within the skull and irritation of the meninges.[9]
Pathophysiology
A cerebral AVM is an abnormal
Diagnosis

A cerebral AVM diagnosis is established by
Grading
Spetzler-Martin (SM) Grade
A common method of grading cerebral AVMs is the Spetzler-Martin (SM) grade.[13] This system was designed to assess the patient's risk of neurological deficit after open surgical resection (surgical morbidity), based on characteristics of the AVM itself. Based on this system, AVMs may be classified as grades 1–5. This system was not intended to characterize risk of hemorrhage.[14]
| AVM size | Adjacent eloquent cortex | Draining veins |
|---|---|---|
| < 3 cm = 1 | Non-eloquent = 0 | Superficial only = 0 |
| 3 – 6 cm = 2 | Eloquent* = 1 | Deep veins = 1 |
| > 6 cm = 3 |
"Eloquent" is defined as areas within the brain that, if removed will result in loss of sensory processing or linguistic ability, minor paralysis, or paralysis. These include the basal ganglia, language cortices, sensorimotor regions, and white matter tracts.[15] Importantly, eloquent areas are often defined differently across studies[16] where deep cerebellar nuclei, cerebral peduncles, thalamus, hypothalamus, internal capsule, brainstem, and the visual cortex could be included.
The risk of post-surgical neurological deficit (difficulty with language, motor weakness, vision loss) increases with increasing Spetzler-Martin grade.[17]
Supplemented Spetzler-Martin (SM-supp, Lawton-Young) Grade
A limitation of the Spetzler-Martin Grading system is that it does not include the following factors: Patient age, hemorrhage, diffuseness of nidus, and arterial supply. In 2010 a new supplemented Spetzler-Martin system (SM-supp, Lawton-Young) was devised adding these variables to the SM system. Under this new system AVMs are classified from grades 1–10. It has since been determined to have greater predictive accuracy than SM grades alone.[18]
| Variable | Spetzler-Martin Grading Scale | Supplemental Grading Scale | ||
|---|---|---|---|---|
| Definition | Points | Definition | Points | |
| AVM size | < 3 cm | 1 | ||
| 3 – 6 cm | 2 | |||
| > 6 cm | 3 | |||
| Deep venous drainage | No | 0 | ||
| Yes | 1 | |||
| Eloquence | No | 0 | ||
| Yes | 1 | |||
| SM Grade Subtotal | (1 - 5) | |||
| Age | < 20 years | 1 | ||
| 20 – 40 years | 2 | |||
| > 40 years | 3 | |||
| Unruptured presentation | No | 0 | ||
| Yes | 1 | |||
| Diffuse | No | 0 | ||
| Yes | 1 | |||
| SM-Supp Grade Subtotal | (1 – 5) | |||
| SM-Supp Total | (1 – 10) | |||
Treatment
Treatment depends on the location and size of the AVM and whether there is bleeding or not.[19]
The treatment in the case of sudden bleeding is focused on restoration of
Medical
Anticonvulsant medications such as phenytoin are often used to control seizure; medications or procedures may be employed to relieve intracranial pressure. Eventually, curative treatment may be required to prevent recurrent hemorrhage. However, any type of intervention may also carry a risk of creating a neurological deficit.[21]
Surgical
Surgical elimination of the blood vessels involved is the preferred curative treatment for many types of AVM.
Radiosurgical
Neuroendovascular therapy
Risks
A first-of-its-kind controlled clinical trial by the National Institutes of Health and National Institute of Neurological Disorders and Stroke focuses on the risk of stroke or death in patients with an AVM who either did or did not undergo interventional eradication.[26] Early results suggest that the invasive treatment of unruptured AVMs tends to yield worse results than the therapeutic (medical) management of symptoms.[27][b] Because of the higher-than-expected experimental event rate (e.g. stroke or death), patient enrollment was halted by May 2013, while the study intended to follow participants (over a planned 5 to 10 years) to determine which approach seems to produce better long-term results.[27]
Prognosis
The main risk is intracranial hemorrhage. This risk is difficult to quantify since many patients with asymptomatic AVMs will never come to medical attention. Small AVMs tend to bleed more often than do larger ones, the opposite of
Epidemiology
The annual new detection rate
References
Footnotes
Citations
- ^ "Brain AVM (arteriovenous malformation) - Symptoms and causes". Mayo Clinic. Retrieved April 23, 2022.
- ^ Al-Saiegh, Fadi; et al. (June 28, 2019). "Oculomotor neuropathy from an unruptured arteriovenous malformation in the frontal operculum: A case report". Surgical Neurology International. Retrieved July 31, 2019.
- ^ PMID 11571210.
- ^ a b c Mayo Clinic staff (February 2009). "Brain AVM (arteriovenous malformation)-Symptoms". Mayo Clinic. Retrieved May 18, 2010.
- ^ a b c David C. Dugdale; Daniel B. Hoch (October 2008). "Arteriovenous malformation - cerebral". ADAM. Retrieved May 18, 2010.
- ^ a b c d e Greenberg, Mark (2006) [1990]. Handbook of Neurosurgery (6th ed.). Thieme. pp. 835–837.
- PMID 5925721.
- ^ ISBN 978-0-323-35637-4.
- ^ "Meningitis and stiff neck: Causes, treatment, and more". Medical News Today. September 21, 2021. Retrieved November 6, 2021.
- ^ a b c d e Mayo Clinic staff (February 2009). "Brain AVM (arteriovenous malformation)-Causes". Mayo Clinic. Retrieved May 30, 2010.
- PMID 25407267.
- ^ a b c d e Mayo Clinic staff (February 2009). "Brain AVM (arteriovenous malformation)-Tests and diagnosis". Mayo Clinic. Retrieved May 18, 2010.
- S2CID 21796375.
- ^ "Spetzler Martin Grading Scale". Boston Medical Center. Retrieved April 23, 2022.
- PMID 23251537.
- PMID 26566782.
- ^ "Brain arteriovenous malformations". UpToDate. Wolters Kluwer. Retrieved April 22, 2022.
A higher Spetzler-Martin grading scale score correlates with increased risk of surgical morbidity and neurologic deficits.
- PMID 25251197.
- ^ a b c d e f Mayo Clinic staff (February 2009). "Brain AVM (arteriovenous malformation)-Treatments and drugs". Mayo Clinic. Retrieved May 18, 2010.
- ^ "Arteriovenous Malformation - Conditions - For Patients - UR Neurosurgery". University of Rochester Medical Center. Retrieved April 22, 2022.
- ^ "AANS | Arteriovenous Malformations". www.aans.org. Retrieved February 3, 2018.
- S2CID 26286536.
- PMID 9457809.
- PMID 25624978.
- ^ Huded V. Endovascular balloon-assisted glue embolization of intranidal high flow fistula in brain AVM. J Neurosci Rural Pract 2013;4, Suppl S1:148-9
- ^ Mohr, Jay Preston (June 4, 2015). "A Randomized Trial of Unruptured Brain Arteriovenous Malformations". ClinicalTrials.gov. Columbia University. Retrieved March 6, 2023.
- ^ a b "A Randomized Trial of Unruptured Brain Arteriovenous Malformations (ARUBA)". National Institute of Neurological Disorders and Stroke. January 29, 2014. Archived from the original on July 4, 2016. Retrieved March 6, 2023.
- PMID 3958721.
- PMID 2384776.
- ^ Mayo Clinic staff (February 2009). "Brain AVM (arteriovenous malformation)-Risk factors". Mayo Clinic. Retrieved May 30, 2010.
