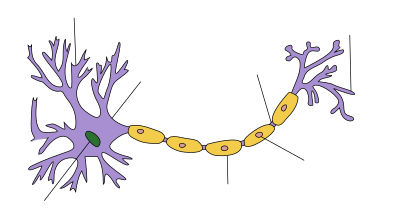
Chronic inflammatory demyelinating polyneuropathy
| Chronic inflammatory demyelinating polyneuropathy | |
|---|---|
| Other names | CIDP, chronic relapsing polyneuropathy, chronic inflammatory demyelinating polyradiculoneuropathy |
 | |
| Histopathology of Chronic inflammatory demyelinating polyneuropathy. Teased single fiber with segmental demyelination. | |
| Specialty | Neurology |
Chronic inflammatory demyelinating polyneuropathy (CIDP) is an acquired
Signs and symptoms
In its traditional manifestation, chronic inflammatory demyelinating polyneuropathy is characterized by symmetric, progressive limb weakness and sensory loss, which typically starts in the legs. Patients report having trouble getting out of a chair, walking, climbing stairs, and falling. Problems with gripping objects, tying shoe laces, and using utensils can all be brought on by upper limb involvement. Proximal limb weakness is a fundamental clinical characteristic that sets apart chronic inflammatory demyelinating polyneuropathy from the vast majority of distal polyneuropathies, which are far more common. Proprioception impairment, distal paresthesias, loss of feeling, and poor balance are all brought on by sensory involvement. Only a small percentage of cases involve neuropathic pain.[4]
Fatigue has been identified as common in CIDP patients, but it is unclear how much this is due to primary (due to the disease action on the body) or secondary effects (impacts on the whole person of being ill with CIDP).[5][6][7]
Numerous reports have outlined a range of clinical patterns that are thought to be chronic inflammatory demyelinating polyneuropathy variations. Different variations include ataxic, pure motor, and pure sensory patterns; additionally, there are multifocal patterns in which the distributions of specific nerve territories experience weakness and sensory loss.[4]
Causes
Chronic inflammatory demyelinating polyneuropathy (or polyradiculoneuropathy) is considered an
There is a lack of awareness and treatment of CIDP. Although there are stringent research criteria for selecting patients for clinical trials, there are no generally agreed-upon clinical diagnostic criteria for CIDP due to its different presentations in symptoms and objective data. Application of the present research criteria to routine clinical practice often misses the diagnosis in a majority of patients, and patients are often left untreated despite progression of their disease.[11]
Risk factors
HIV infection is a factor in the occurrence of CIDP. At every stage of HIV infection, distinct patterns of CIDP, whether progressive or relapsing, have been noted. Increased protein content is linked to CSF pleocytosis in the majority of HIV-CIDP cases.[12] Pregnancy has been linked to a significantly greater risk of relapse.[13]
Triggers
In one study, 32% of 92 CIDP patients had a history of vaccination or infection within 6 weeks of the onset of neurological symptoms, with the majority of these infections being non-specific upper respiratory tract or gastrointestinal infections.[13] A different study showed that out of 100 patients, 16% had an infectious event six weeks or less prior to the onset of neurological symptoms: seven patients had CIDP that was related to or followed viral hepatitis, and six had a chronic infection with the hepatitis B virus. The other nine patients had vague symptoms similar to the flu.[14]
Genetics
There isn't any known genetic predisposition to chronic inflammatory demyelinating polyneuropathy.[15]
Variants with paranodal autoantibodies
Some variants of CIDP present autoimmunity against proteins of the
These cases are special not only because of their pathology, but also because they are non-responsive to the standard treatment. They are responsive to Rituximab instead.[16]
Also some cases of combined central and peripheral demyelination (CCPD) could be produced by neurofascins.[17]
Autoantibodies of the IgG3 Subclass in CIDP
Autoantibodies to components of the Ranvier nodes, specially autoantibodies the Contactin-associated protein 1 (
Mechanism
In the local tissue compartment of
Individuals with chronic inflammatory demyelinating polyneuropathy have evidence of activation of T cells in the systemic immune compartment; however, antigen specificity is still largely unknown.[21][22]
It was proposed more than 20 years ago that
Target antigens may also include gangliosides and related glycolipids. There is serologic evidence of recent Campylobacter jejuni infection in a small number of individuals with chronic inflammatory demyelinating polyneuropathy. Because carbohydrate epitopes are expressed in both microbial lipopolysaccharides and nerve glycolipids, this discovery may, in rare cases, point to molecular mimicry as the root cause of chronic inflammatory demyelinating polyneuropathy.[25]
Apart from myelin-directed antibodies, other serum components that can cause
Diagnosis
When a patient presents with a non-length-dependent demyelinating polyneuropathy which either develops chronically over several months or progresses over more than a month, CIDP may be diagnosed. There may be a secondary progressive course along with a progressive course that follows, or it may be relapsing and remitting. Pathological investigations and electrophysiological studies, if necessary, show the underlying demyelinating process.[26]
The primary basis for diagnosing CIDP is the electrophysiological studies that depict an asymmetric demyelinating process. Comparison of the proximal and distal latencies of equivalent segments of two nerves in the same limb reveals that these patients with acquired demyelinating neuropathy frequently have a differential slowing of conduction velocity. There is always a noticeable difference in the compound muscle action potential's dispersion, and conduction block is commonly experienced.[26]
An MRI can show proximal nerve or root enlargement and gadolinium enhancement, which indicate active inflammation as well as demyelination in the brachial plexus[27] or cauda equina.[28]
Classification
Clinically, CIDP is divided into "typical" and "atypical" cases. A typical case of CIDP is a symmetrical polyneuropathy that affects the proximal and distal muscles equally. Atypical cases of CIDP include multifocal acquired demyelinating sensory and motor neuropathy (MADSAM), Lewis-Sumner syndrome (LSS), and distal acquired demyelinating symmetric (DADS). DADS is a sensory or sensorimotor neuropathy that is symmetrical and length-dependent. It is frequently linked to an IgM paraprotein and noticeably longer distal motor latencies. The characteristics are typical of demyelinating neuropathy with antimyelin-associated glycoprotein (MAG) antibodies; however, anti-MAG neuropathy is not included in the CIDP criteria according to the EFNS/PNS criteria, primarily due to the presence of a particular antibody and a different response to treatment. LSS exhibits a multifocal distribution, with conduction block serving as the disease's electrophysiological hallmark. Furthermore, there have been reports of pure motor and sensory CIDP variants, with the latter occasionally limited to sensory nerve roots (chronic immune sensory polyradiculopathy). The acronym CANOMAD refers to a rare chronic ataxic neuropathy linked to disialosyl (
Differential diagnosis
CIDP variants are among several types of immune-mediated neuropathies recognised.[30][31] These include:
- Chronic inflammatory demyelinating polyneuropathy (CIDP) with subtypes:
- Classical CIDP
- CIDP with diabetes
- CIDP/monoclonal gammopathy of undetermined significance
- Sensory CIDP
- Multifocal motor neuropathy
- Multifocal acquired demyelinating sensory and motor neuropathy (Lewis-Sumner syndrome)
- Multifocal acquired sensory and motor neuropathy
- Distal acquired demyelinating sensory neuropathy
- Guillain–Barré syndrome with subtypes:
- Acute inflammatory demyelinating polyradiculoneuropathy
- Acute motor axonal neuropathy
- Acute motor and sensory axonal neuropathy
- Acute pandysautonomia
- Miller Fisher syndrome
- IgM monoclonal gammopathies with subtypes:
- Waldenström's macroglobulinemia
- Mixed gait ataxia, late-onset polyneuropathysyndrome
- Myelin-associated glycoprotein-associated gammopathy, polyneuropathy, organomegaly, endocrinopathy, M-protein and skin changes syndrome (POEMS)
Other possible diagnoses are
- Bickerstaff brainstem encephalitis
- Fisher syndrome
- Guillain–Barré syndrome
For this reason a diagnosis of chronic inflammatory demyelinating polyneuropathy needs further investigations. The diagnosis is usually provisionally made through a clinical neurological examination.
Tests
Typical diagnostic tests include:
- Electrodiagnostics – demyelination. These findings include:[citation needed]
- a reduction in nerve conduction velocities;
- the presence of conduction block or abnormal temporal dispersion in at least one motor nerve;
- prolonged distal latencies in at least two nerves;
- absent F waves or prolonged minimum F wave latencies in at least two motor nerves. (In some case EMG/NCV can be normal).
- Serum test to exclude other autoimmunediseases.
- anti-ganglioside antibodies. These antibodies are present in the branch of CIDP diseases comprised by anti-GM1, anti-GD1a, and anti-GQ1b.
- axonalinvolvement is observed on EMG.
- Ultrasound of the peripheral nerves may show swelling of the affected nerves.[32][33][34]
- Magnetic resonance imaging can also be used in the diagnostic workup.[35][36]
In some cases electrophysiological studies fail to show any evidence of demyelination. Though conventional
Treatment
First-line treatment for CIDP is currently
Intravenous immunoglobulin and plasmapheresis have proven benefit in randomized, double-blind, placebo-controlled trials. Despite less definitive published evidence of efficacy, corticosteroids are considered standard therapies because of their long history of use and cost effectiveness. Intravenous immunoglobulin is probably the first-line CIDP treatment, but is extremely expensive. For example, in the U.S., a single 65 g dose of Gamunex brand in 2010 might be billed at the rate of $8,000 just for the immunoglobulin—not including other charges such as nurse administration.[citation needed]
Immunosuppressive drugs are often of the
Non-cytotoxic immunosuppressive treatments usually include the anti-rejection transplant drugs
Anti-thymocyte globulin, an immunosuppressive agent that selectively destroys T lymphocytes is being studied for use in CIDP. Anti-thymocyte globulin is the gamma globulin fraction of antiserum from animals that have been immunized against human thymocytes. It is a polyclonal antibody. Although chemotherapeutic and immunosuppressive agents have shown to be effective in treating CIDP, significant evidence is lacking, mostly due to the heterogeneous nature of the disease in the patient population in addition to the lack of controlled trials.[citation needed]
A review of several treatments found that azathioprine,
In severe cases of CIDP, when second-line immunomodulatory drugs are not efficient, autologous hematopoietic stem cell transplantation (HSCT) is sometimes performed. The treatment may induce long-term remission even in severe treatment-refractory cases of CIDP. To improve outcome, it has been suggested that it should be initiated before irreversible axonal damage has occurred. However, a precise estimation of its clinical efficacy for CIDP is not available, as randomized controlled trials (RCT) have not been performed.[42] (In MS, the ASTIMS RCT provides evidence for superior effect of HSCT to the then-best practice for treatment of aggressive MS.[42] The more recent MIST RCT confirmed its superiority in MS.[43])
Physical therapy and occupational therapy may improve muscle strength, activities of daily living, mobility, and minimize the shrinkage of muscles and tendons and distortions of the joints.[citation needed]
Prognosis
As in multiple sclerosis, another demyelinating condition, it is not possible to predict with certainty how CIDP will affect patients over time. The pattern of relapses and remissions varies greatly with each patient. A period of relapse can be very disturbing, but many patients make significant recoveries.[citation needed]
If diagnosed early, initiation of early treatment to prevent loss of nerve axons is recommended. However, many individuals are left with residual numbness, weakness, tremors, fatigue and other symptoms which can lead to long-term
It is important to build a good relationship with doctors, both primary care and specialist. Because of the rarity of the illness, many doctors will not have encountered it before. Each case of CIDP is different, and relapses, if they occur, may bring new symptoms and problems. Because of the variability in severity and progression of the disease, doctors will not be able to give a definite prognosis. A period of experimentation with different treatment regimens is likely to be necessary in order to discover the most appropriate treatment regimen for a given patient.[citation needed]
Epidemiology
In 1982 Lewis et al. reported a group of patients with a chronic asymmetrical sensorimotor neuropathy mostly affecting the arms with multifocal involvement of peripheral nerves.[44] Also in 1982 Dyck et al reported a response to prednisolone to a condition they referred to as chronic inflammatory demyelinating polyradiculoneuropathy.[45] Parry and Clarke in 1988 described a neuropathy which was later found to be associated with IgM autoantibodies directed against GM1 gangliosides.[46][47] This latter condition was later termed multifocal motor neuropathy[48] This distinction is important because multifocal motor neuropathy responds to intravenous immunoglobulin alone, while chronic inflammatory demyelinating polyneuropathy responds to intravenous immunoglobulin, steroids and plasma exchange.[49] It has been suggested that multifocal motor neuropathy is distinct from chronic inflammatory demyelinating polyneuropathy and that Lewis-Sumner syndrome is a distinct variant type of chronic inflammatory demyelinating polyneuropathy.[50]
The Lewis-Sumner form of this condition is considered a rare disease with only 50 cases reported up to 2004.[51] A total of 90 cases had been reported by 2009.[52]
Vaccine injury compensation for CIDP
The
See also
References
- ^ "Chronic Inflammatory Demyelinating Polyneuropathy (CIDP) Information Page". ninds.nih.gov. Retrieved 2020-12-31.
- ^ S2CID 20396024.
- ^ "GBS (Guillain-Barré Syndrome) - CIDP Neuropathy". cidpneuropathysupport.com. Retrieved 2017-12-14.
- ^ PMID 23642722.
- S2CID 225480334.
- S2CID 24896124.
- S2CID 9884101.
- ^ "C.I.D.P. Log". cidplog.com. Retrieved 2018-09-27.
- S2CID 23639113.
- S2CID 46426663.
- S2CID 25742148.
- ISBN 978-0-7020-1836-7. Retrieved December 13, 2023.
- ^ PMID 3427403. Retrieved 13 December 2023.
- S2CID 31543851.
- ISBN 978-0-7216-9491-7. Retrieved 13 December 2023.
- ^ .
- S2CID 53292167.
- S2CID 201980461.
- PMID 14513861.
- ^ PMID 15800230.
- PMID 10555828.
- S2CID 24212928.
- S2CID 20573608.
- PMID 6252877.
- S2CID 23264775.
- ^ S2CID 23226032.
- PMID 10388803.
- S2CID 20762613.
- PMID 30992333.
- S2CID 10651959.
- PMID 11345010.
- S2CID 24416887.
- S2CID 5466514.
- S2CID 37585666.
- S2CID 39436370.
- S2CID 44981467.
- PMID 17151528.
- PMID 12090400.
- PMID 25584070.
- PMID 16024890.
- PMID 29043889.
- ^ PMID 28866625.
- ^ "MS patients could be offered stem cell transplants as a first-line treatment in new world-first trial". www.sheffield.ac.uk. 2022-11-29. Retrieved 2023-08-16.
- S2CID 40027684.
- S2CID 24567176.
- S2CID 21481288.
- S2CID 44845902.
- PMID 11282149.
- S2CID 29950514.
- S2CID 32166227.
- PMID 15289267.
- S2CID 43478826.
- ^ "Riley v. Secretary of Health and Human Services, Case No. 16-262V". United States Court of Federal Claims. July 30, 2019.
- ^ "United States Court of Federal Claims Opinions/Orders". United States Court of Federal Claims. October 24, 2019. Retrieved October 24, 2019.