Psoriasis
| Psoriasis | |
|---|---|
biologics[5] | |
| Frequency | 79.7 million[6] / 2–4%[7] |
Psoriasis is a long-lasting, noncontagious
The five main types of psoriasis are plaque, guttate, inverse, pustular, and erythrodermic.[5] Plaque psoriasis, also known as psoriasis vulgaris, makes up about 90% of cases.[4] It typically presents as red patches with white scales on top.[4] Areas of the body most commonly affected are the back of the forearms, shins, navel area, and scalp.[4] Guttate psoriasis has drop-shaped lesions.[5] Pustular psoriasis presents as small, noninfectious, pus-filled blisters.[10] Inverse psoriasis forms red patches in skin folds.[5] Erythrodermic psoriasis occurs when the rash becomes very widespread, and can develop from any of the other types.[4] Fingernails and toenails are affected in most people with psoriasis at some point in time.[4] This may include pits in the nails or changes in nail color.[4]
Psoriasis is generally thought to be a
There is no known cure for psoriasis, but various treatments can help control the symptoms.
The word "psoriasis" is from Greek ψωρίασις, meaning "itching condition" or "being itchy"[11] from psora, "itch", and -iasis, "action, condition".
Signs and symptoms
Plaque psoriasis

Psoriasis vulgaris (also known as chronic stationary psoriasis or plaque-like psoriasis) is the most common form and affects 85–90% of people with psoriasis.[12] Plaque psoriasis typically appears as raised areas of inflamed skin covered with silvery-white, scaly skin. These areas are called plaques and are most commonly found on the elbows, knees, scalp, and back.[12][13]
-
Plaques of psoriasis
-
A person's arm covered with plaque psoriasis
-
Psoriasis of the palms
Other forms
Additional types of psoriasis comprise about 10% of cases. They include pustular, inverse, napkin, guttate, oral, and seborrheic-like forms.[14]
Pustular psoriasis

Inverse psoriasis
Napkin psoriasis
Guttate psoriasis

There is no firm evidence regarding best management for guttate psoriasis; however, first line therapy for mild guttate psoriasis typically includes topical corticosteroids.[23][24] Phototherapy can be used for moderate or severe guttate psoriasis. Biologic treatments have not been well studied in the treatment of guttate psoriasis.[23]
Guttate psoriasis has a better prognosis than plaque psoriasis and typically resolves within 1–3 weeks; however, up to 40% of patients with guttate psoriasis eventually convert to plaque psoriasis.[23][18]
Erythrodermic psoriasis
Psoriatic erythroderma (erythrodermic psoriasis) involves widespread inflammation and exfoliation of the skin over most of the body surface, often involving greater than 90% of the body surface area.[17] It may be accompanied by severe dryness, itching, swelling, and pain. It can develop from any type of psoriasis.[17] It is often the result of an exacerbation of unstable plaque psoriasis, particularly following the abrupt withdrawal of systemic glucocorticoids.[25] This form of psoriasis can be fatal as the extreme inflammation and exfoliation disrupt the body's ability to regulate temperature and perform barrier functions.[26]
Mouth
Psoriasis in the mouth is very rare, in contrast to lichen planus, another common papulosquamous disorder that commonly involves both the skin and mouth.[27] When psoriasis involves the oral mucosa (the lining of the mouth), it may be asymptomatic,[27] but it may appear as white or grey-yellow plaques.[27] Fissured tongue is the most common finding in those with oral psoriasis and has been reported to occur in 6.5–20% of people with psoriasis affecting the skin. The microscopic appearance of oral mucosa affected by geographic tongue (migratory stomatitis) is very similar to the appearance of psoriasis.[28] A recent study just found an association between the two conditions and it suggests that geographic tounge might be a predictor to psoriasis.[29]
Seborrheic-like psoriasis
Psoriatic arthritis
Psoriatic arthritis is a form of chronic inflammatory arthritis that has a highly variable clinical presentation and frequently occurs in association with skin and nail psoriasis.[30][31] It typically involves painful inflammation of the joints and surrounding connective tissue, and can occur in any joint, but most commonly affects the joints of the fingers and toes. This can result in a sausage-shaped swelling of the fingers and toes known as dactylitis.[30] Psoriatic arthritis can also affect the hips, knees, spine (spondylitis), and sacroiliac joint (sacroiliitis).[32] About 30% of individuals with psoriasis will develop psoriatic arthritis.[12] Skin manifestations of psoriasis tend to occur before arthritic manifestations in about 75% of cases.[31]
Nail changes
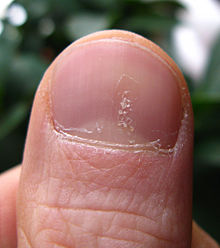

Medical signs
In addition to the appearance and distribution of the rash, specific
Causes
The cause of psoriasis is not fully understood. Genetics, seasonal changes, skin damage, climate, immunocompromised state, specific infections, and the use of some medications have been connected with different types of psoriasis.[34][35]
Genetics
Around one-third of people with psoriasis report a family history of the disease, and researchers have identified genetic loci associated with the condition. Identical twin studies suggest a 70% chance of a twin developing psoriasis if the other twin has the disorder. The risk is around 20% for fraternal twins. These findings suggest both a genetic susceptibility and an environmental response in developing psoriasis.[36]
Psoriasis has a strong hereditary component, and many genes are associated with it, but how those genes work together is unclear. Most of the identified genes relate to the immune system, particularly the
Classic genome-wide
The major determinant is PSORS1, which probably accounts for 35–50% of psoriasis heritability.
Two major immune system genes under investigation are interleukin-12 subunit beta (IL12B) on
Lifestyle
Conditions reported as worsening the disease include chronic infections, stress, and changes in season and
HIV
The rate of psoriasis in
Microbes
Psoriasis has been described as occurring after
Medications
Drug-induced psoriasis may occur with
Pathophysiology
Psoriasis is characterized by an abnormally excessive and rapid growth of the
Gene mutations of proteins involved in the skin's ability to function as a barrier have been identified as markers of susceptibility for the development of psoriasis.[54][55]
Diagnosis

A diagnosis of psoriasis is usually based on the appearance of the skin. Skin characteristics typical for psoriasis are scaly, erythematous plaques, papules, or patches of skin that may be painful and itch.[18] No special blood tests or diagnostic procedures are usually required to make the diagnosis.[16][59]
The
If the clinical diagnosis is uncertain, a skin
Classification
Morphological
| Psoriasis Type | ICD-10 Code |
|---|---|
| Psoriasis Vulgaris | L40.0 |
| Generalized pustular psoriasis | L40.1 |
Acrodermatitis continua
|
L40.2 |
| Pustulosis palmaris et plantaris | L40.3 |
| Guttate psoriasis | L40.4 |
| Psoriatic arthritis | L40.50 |
| Psoriatic spondylitis | L40.53 |
| Inverse psoriasis | L40.8 |
Psoriasis is classified as a
Pathogenetic
Another classification scheme considers genetic and demographic factors. Type 1 has a positive family history, starts before the age of 40, and is associated with the human leukocyte antigen, HLA-Cw6. Conversely, type 2 does not show a family history, presents after age 40, and is not associated with HLA-Cw6.[63] Type 1 accounts for about 75% of persons with psoriasis.[64]
The classification of psoriasis as an autoimmune disease has sparked considerable debate. Researchers have proposed differing descriptions of psoriasis and psoriatic arthritis; some authors have classified them as autoimmune diseases[16][34][65] while others have classified them as distinct from autoimmune diseases and referred to them as immune-mediated inflammatory diseases.[37][66][67]
Severity

No consensus exists about how to classify the severity of psoriasis. Mild psoriasis has been defined as a percentage of body surface area (BSA)≤10, a Psoriasis Area and Severity Index (PASI) score ≤10, and a Dermatology Life Quality Index (DLQI) score ≤10.[68] Moderate to severe psoriasis was defined by the same group as BSA >10 or PASI score >10 and a DLQI score >10.[68]
The DLQI is a 10-question tool used to measure the impact of several dermatologic diseases on daily functioning. The DLQI score ranges from 0 (minimal impairment) to 30 (maximal impairment) and is calculated with each answer being assigned 0–3 points with higher scores indicating greater social or occupational impairment.[69]
The PASI is the most widely used measurement tool for psoriasis. It assesses the severity of lesions and the area affected and combines these two factors into a single score from 0 (no disease) to 72 (maximal disease).[70] Nevertheless, the PASI can be too unwieldy to use outside of research settings, which has led to attempts to simplify the index for clinical use.[71]
Co-morbidities
Psoriasis is not just a skin disease. The symptoms of psoriasis can sometimes go beyond the skin and can have a negative impact on the quality of life of the affected individuals.[72] Additionally, the co-morbidities increase the treatment and financial burden of psoriasis and should be considered when managing this condition.[72]
Cardiovascular complications
There is 2.2 times increased risk of cardiovascular complications in people with psoriasis.[73] Also, people with psoriasis are more susceptible to myocardial infarction (heart attack) and stroke.[73] It has been speculated that there is systemic inflammation in psoriasis, which drives “psoriatic march” and can cause other inflammatory complications including cardiovascular complications.[73] A study used fluorodeoxyglucose F-18 positron emission tomography computed tomography (FDG PET/CT) to measure aortic vascular inflammation in psoriasis patients, and found increased coronary artery disease indices, including total plaque burden, luminal stenosis, and high-risk plaques in people with psoriasis. Similarly, it was found that there is 11% reduction in aortic vascular inflammation when there is 75% reduction in PASI score.[74]
Depression
Depression or depressive symptoms are present in 28–55% of people with psoriasis.[75] People with psoriasis are often stigmatized due to visible disfigurement of the skin. Social stigmatization is a risk factor for depression, however, other immune system factors may also be related to this observed increased incidence of depression in people with psoriasis.[75] There is some evidence that increased inflammatory signals in the body could also contribute to depression in people with chronic inflammatory diseases, including psoriasis.[75]
Type 2 diabetes
People with psoriasis are at increased risk of developing type 2 diabetes (~1.5 odds ratio).[76] A genome-wide based genetic study found that psoriasis and type 2 diabetes share four loci, namely, ACTR2, ERLIN1, TRMT112, and BECN1, which are connected via inflammatory NF-κB pathway.[76]
Management

While no cure is available for psoriasis,[50] many treatment options exist. Topical agents are typically used for mild disease, phototherapy for moderate disease, and systemic agents for severe disease.[77] There is no evidence to support the effectiveness of conventional topical and systemic drugs, biological therapy, or phototherapy for acute guttate psoriasis or an acute guttate flare of chronic psoriasis.[78]
Topical agents
Topical corticosteroid preparations are the most effective agents when used continuously for eight weeks; retinoids and coal tar were found to be of limited benefit and may be no better than placebo.[79] Very potent topical corticosteroids may be helpful in some cases, however, it is suggested to only use them for four weeks at a time and only if other less potent topical treatment options are not working.[80]
For psoriasis of the scalp, a 2016 review found dual therapy (vitamin D analogues and topical corticosteroids) or corticosteroid monotherapy to be more effective and safer than topical vitamin D analogues alone.[82] Due to their similar safety profiles and minimal benefit of dual therapy over monotherapy, corticosteroid monotherapy appears to be an acceptable treatment for short-term treatment.[82]
Moisturizers and emollients such as
Vitamin D analogues may be useful with steroids; steroids alone have a higher rate of side effects.[81] Vitamin D analogues may allow less steroids to be used.[85]
Another topical therapy used to treat psoriasis is a form of
UV phototherapy
One of the problems with clinical phototherapy is the difficulty many people have gaining access to a facility. Indoor tanning resources are almost ubiquitous today and could be considered as a means for people to get UV exposure when dermatologist-provided phototherapy is not available. Indoor tanning is already used by many people as a treatment for psoriasis; one indoor facility reported that 50% of its clients were using the center for psoriasis treatment; another reported 36% were doing the same thing. However, a concern with the use of commercial tanning is that tanning beds that primarily emit UVA might not effectively treat psoriasis. One study found that plaque psoriasis is responsive to erythemogenic doses of either UVA or UVB, as exposure to either can cause dissipation of psoriatic plaques. It does require more energy to reach erythemogenic dosing with UVA.[92]
UV light therapies all have risks; tanning beds are no exception, being listed by the World Health Organization as carcinogens.[93] Exposure to UV light is known to increase the risks of melanoma and squamous cell and basal cell carcinomas; younger people with psoriasis, particularly those under age 35, are at increased risk from melanoma from UV light treatment. A review of studies recommends that people who are susceptible to skin cancers exercise caution when using UV light therapy as a treatment.[92]
A major mechanism of NB-UVB is the induction of
PUVA combines the oral or topical administration of psoralen with exposure to ultraviolet A (UVA) light. The
Systemic agents

Psoriasis resistant to
Non-biologic systemic treatments frequently used for psoriasis include
Guidelines regard biologics as third-line treatment for plaque psoriasis following inadequate response to topical treatment, phototherapy, and non-biologic systemic treatments.[100] The safety of biologics during pregnancy has not been assessed. European guidelines recommend avoiding biologics if a pregnancy is planned; anti-TNF therapies such as infliximab are not recommended for use in chronic carriers of the hepatitis B virus or individuals infected with HIV.[98]
Several monoclonal antibodies target cytokines, the molecules that cells use to send inflammatory signals to each other.
Two medications that target T cells are
Individuals with psoriasis may develop
There is strong evidence to indicate that infliximab,
Another set of treatments for moderate to severe psoriasis are
Apremilast (Otezla, Celgene) is an oral small-molecule inhibitor of the enzyme phosphodiesterase 4, which plays an important role in chronic inflammation associated with psoriasis.[medical citation needed]
It has been theorized that antistreptococcal medications may improve guttate and chronic plaque psoriasis; however, the limited studies do not show that antibiotics are effective.[109]
Surgery
Limited evidence suggests removal of the tonsils may benefit people with chronic plaque psoriasis, guttate psoriasis, and palmoplantar pustulosis.[110][111]
Diet
Uncontrolled studies have suggested that individuals with psoriasis or psoriatic arthritis may benefit from a diet supplemented with fish oil rich in eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA).[112] A low-calorie diet appears to reduce the severity of psoriasis.[43] Diet recommendations include consumption of cold water fish (preferably wild fish, not farmed) such as salmon, herring, and mackerel; extra virgin olive oil; legumes; vegetables; fruits; and whole grains; and avoid consumption of alcohol, red meat, and dairy products (due to their saturated fat). The effect of consumption of caffeine (including coffee, black tea, mate, and dark chocolate) remains to be determined.[113]
Many patients report improvements after consuming less tobacco, caffeine, sugar,
There is a higher rate of
Prognosis
Most people with psoriasis experience nothing more than mild skin lesions that can be treated effectively with topical therapies.[79] Depending on the severity and location of outbreaks, people may experience significant physical discomfort and some disability, affecting the person's quality of life.[34] Itching and pain can interfere with basic functions, such as self-care and sleep.[52] Participation in sporting activities, certain occupations, and caring for family members can become difficult activities for those with plaques located on their hands and feet.[52] Plaques on the scalp can be particularly embarrassing, as flaky plaque in the hair can be mistaken for dandruff.[118]

Individuals with psoriasis may feel self-conscious about their appearance and have a poor self-image that stems from fear of public rejection and psychosexual concerns. Psoriasis has been associated with low self-esteem and
Several conditions are associated with psoriasis including obesity, cardiovascular, and metabolic disturbances. These occur more frequently in older people. Nearly half of individuals with psoriasis over the age of 65 have at least three comorbidities (concurrent conditions), and two-thirds have at least two comorbidities.[121]
Cardiovascular disease
Psoriasis has been associated with obesity[3] and several other cardiovascular and metabolic disturbances. The number of new cases per year of diabetes is 27% higher in people affected by psoriasis than in those without the condition.[122] Severe psoriasis may be even more strongly associated with the development of diabetes than mild psoriasis.[122] Younger people with psoriasis may also be at increased risk for developing diabetes.[121][123] Individuals with psoriasis or psoriatic arthritis have a slightly higher risk of heart disease and heart attacks when compared to the general population. Cardiovascular disease risk appeared to be correlated with the severity of psoriasis and its duration. There is no strong evidence to suggest that psoriasis is associated with an increased risk of death from cardiovascular events. Methotrexate may provide a degree of protection for the heart.[42][121]
The odds of having hypertension are 1.58 times ( i.e. 58%) higher in people with psoriasis than those without the condition; these odds are even higher with severe cases of psoriasis. A similar association was noted in people who have psoriatic arthritis—the odds of having hypertension were found to be 2.07 times ( i.e. 107%) greater when compared to odds of the general population. The link between psoriasis and hypertension is not currently[
Other diseases
The rates of
Epidemiology
Psoriasis is estimated to affect 2–4% of the population of the western world.[7] The rate of psoriasis varies according to age, region and ethnicity; a combination of environmental and genetic factors is thought to be responsible for these differences.[7] Psoriasis is about five times more common in people of European descent than in people of Asian descent,[130] more common in countries farther from the equator,[49] relatively uncommon in African Americans, and extremely uncommon in Native Americans.[50] Psoriasis has been estimated to affect about 6.7 million Americans.[5]
Psoriasis can occur at any age, although it is more frequent in adults and commonly appears for the first time between the ages of 15 and 25 years.[5] Approximately one third of people with psoriasis report being diagnosed before age 20.[131] Psoriasis affects both sexes equally.[63]
People with inflammatory bowel disease such as Crohn disease or ulcerative colitis are at an increased risk of developing psoriasis.[49]
History
Scholars believe psoriasis to have been included among the various skin conditions called
Psoriasis is thought to have first been described in
The history of psoriasis is littered with treatments of dubious effectiveness and high toxicity. In the 18th and 19th centuries,
Society and culture
The International Federation of Psoriasis Associations (IFPA) is the global umbrella organization for national and regional psoriasis associations and also gathers the leading experts in psoriasis and psoriatic arthritis research for scientific conferences every three years.
Cost
The annual cost for treating psoriasis in the United States is estimated as high as $32.5 billion, including $12.2 billion in direct costs. Pharmacy costs are the main source of direct expense, with biologic therapy the most prevalent. These costs increase significantly when co-morbid conditions such as heart disease, hypertension, diabetes, lung disease and psychiatric disorders are factored in. Expenses linked to co-morbidities are estimated at an additional $23,000 per person per year.[137]
Research
The role of insulin resistance in the pathogenesis of psoriasis is under investigation. Preliminary research has suggested that antioxidants such as polyphenols may have beneficial effects on the inflammation characteristic of psoriasis.[138]
Many novel medications being researched during the 2010s target the
References
- ISBN 978-3-12-539683-8.
- ^ "Psoriasis". Merriam-Webster.com Dictionary.
- ^ PMID 18423260.
- ^ S2CID 208793879.
- ^ a b c d e f g h i j k l "Questions and Answers About Psoriasis". National Institute of Arthritis and Musculoskeletal and Skin Diseases. 12 April 2017. Archived from the original on 22 April 2017. Retrieved 22 April 2017.
- PMID 27733282.
- ^ PMID 23014338.
- ISBN 978-1-4860-1440-8. Archivedfrom the original on 14 January 2023. Retrieved 8 May 2020.
- from the original on 2 February 2014.
- ^ ISBN 978-1-4419-0524-6. Archivedfrom the original on 8 September 2017.
- ISBN 978-0-323-03622-1. Archivedfrom the original on 8 January 2017.
- ^ PMID 23569359.
- ISBN 978-0-7020-3084-0.
- ^ ISBN 978-0-7216-2921-6.
- PMID 22609220.
- ^ PMID 24434359.
- ^ PMID 30909615.
- ^ PMID 23668525.[permanent dead link]
- ^ ISBN 978-0-07-166904-7.
- PMID 27103532.
- ^ S2CID 9513914.
- PMID 27900946.
- ^ PMID 29494104.
- S2CID 27381477.
- ^ PMID 22321651.
- ^ Stanway A. "Erythrodermic psoriasis". DermNet NZ. Archived from the original on 2 February 2014. Retrieved 16 March 2014.
- ^ S2CID 33434341.
- ISBN 978-1-55009-345-2.
- PMID 30739339.
- ^ PMID 23620660.
- ^ PMID 22286649.
- PMID 24278057.
- ^ S2CID 8561015.
- ^ PMID 24069534.
- ^ PMID 18021899.
- PMID 15968269.
- ^ S2CID 203791161.
- PMID 16916825.
- PMID 22521419.
- PMID 22521418.
- ^ (PDF) from the original on 27 June 2019. Retrieved 4 March 2014.
- ^ S2CID 2766931.
- ^ PMID 31309536. CD011972.
- ^ PMID 21261982.
- from the original on 21 April 2008.
- ^ PMID 23364144.
- PMID 22673731.
- ^ "Images of Memorable Cases: Case 34". Connexions. Rice University. Archived from the original on 10 July 2012. Retrieved 21 December 2009.
This AIDS patient presented with a pruritic eruption over most of his body
- ^ S2CID 207210831.
- ^ ISBN 978-1-4443-0009-3. Archivedfrom the original on 24 February 2024. Retrieved 19 November 2020.
- ^ PMID 21106435.
- ^ PMID 23124421.
- PMID 25585875.
- PMID 20692714.
- PMID 22507041.
- ^ S2CID 24119451.
- ^ PMID 23122008.
- PMID 29713318.
- S2CID 42148834.
- PMID 19884985.
- ^ "Application to Dermatology of International Classification of Disease (ICD-10)". The International League of Dermatological Societies. Archived from the original on 9 July 2006.
- ISBN 978-0-07-138076-8.
- ^ PMID 24204077.
- S2CID 45917573.
- ^ PMID 24101875.
- PMID 22348323.
- PMID 22754278.
- ^ PMID 20857129.
- PMID 22588772.
- ^ "Psoriasis Update". Skin & Aging. 14 (3): 46–50. 2006. Archived from the original on 2 March 2011.
- PMID 15530297.
- ^ S2CID 21793052.
- ^ PMID 32314303.
- PMID 31971602.
- ^ PMID 34806760.
- ^ PMID 33385400.
- ^ S2CID 7907468.
- PMID 30958563.
- ^ S2CID 21979785.
- S2CID 169036303.
- ^ (PDF) from the original on 28 April 2021. Retrieved 6 November 2019.
- ^ PMID 26915340. CD009687.
- ^ (PDF) from the original on 29 August 2021. Retrieved 30 June 2019.
- PMID 19217694.
- S2CID 1688553.
- ^ PMID 18755374.
- ^ PMID 22503590.
- PMID 32368795.
- ^ Medical College of Georgia at Augusta University. "Glycerin is safe, effective in psoriasis model." ScienceDaily. [www.sciencedaily.com/releases/2021/10/211004104229.htm] (accessed 9 July 2023).
- ^ PMID 21079308.
- PMID 24151011.
- ^ PMID 25735439.
- ISBN 978-92-4-151259-6.
- PMID 21412260.
- PMID 21429620.
- PMID 21720660.
- ^ S2CID 11207097.
- ^ S2CID 22462278.
- ^ "Learning module: Psoriasis | American Academy of Dermatology". www.aad.org. Archived from the original on 27 March 2017. Retrieved 26 March 2017.
- ^ S2CID 42598571.
- PMID 26910853.
- S2CID 10132276.
- ^ Novel Drug Approvals for 2017 Archived 29 June 2017 at the Wayback Machine
- PMID 26598969.
- PMID 20400861.
- ^ PMID 37436070.
- PMID 26714681.
- PMID 26258748.
- PMID 30835819.
- PMID 24283892.
- from the original on 29 August 2021. Retrieved 3 September 2019.
- ^ PMID 20228538.
- ^ PMID 27455297.
- PMID 28526915.
- PMID 24790463.
- S2CID 15561525.
- ^ PMID 24780176.
- PMID 23806151.
- PMID 16756666.
- PMID 23245976.
- ^ ISBN 978-0-323-08037-8. Archivedfrom the original on 14 January 2023. Retrieved 8 May 2020.
- ^ PMID 25149424.
- ^ PMID 23407990.
- S2CID 23724435.
- ^ S2CID 207482092.
- ^ "Psoriasis Linked to Stroke Risk". BBC. August 2011. Archived from the original on 28 August 2011.
- ^ S2CID 12519829.
- PMID 23062896.
- PMID 31617868.
- Lay summary in: Bakalar N (16 October 2019). "Psoriasis Tied to Increased Cancer Risk". The New York Times.
- ^ "Psoriasis affects more than 8 million people in the U.S." National Psoriasis Foundation. Archived from the original on 24 February 2024. Retrieved 12 July 2021.
- PMID 18021892.
- ^ PMID 15072746.
- S2CID 27467338.
- ^ S2CID 5813486.
- ^ S2CID 199596315.
- ^ International Federation of Psoriasis Associations Archived 21 November 2008 at the Wayback Machine. Ifpa-pso.org. Retrieved on 8 June 2013.
- from the original on 2 February 2017.
- ^ PMID 23935446.
- ^ PMID 23205338.
Further reading
- Baker BS (2008). From Arsenic to Biologicals: A 200 Year History of Psoriasis. Beckenham UK: Garner. ISBN 978-0-9551603-2-5.
- "Guidelines for the assessment and management of psoriasis". U.S. National Guideline Clearinghouse. Archived from the original on 27 September 2013. Retrieved 26 July 2013.
- World Health Organization (2016). Global report on psoriasis. ISBN 978-92-4-156518-9. Archived from the originalon 29 February 2016.
External links
- "Psoriatic arthritis". Genetics Home Reference.
- "Psoriasis". MedlinePlus. U.S. National Library of Medicine.



