Cutaneous T-cell lymphoma
| Cutaneous T-cell lymphoma | |
|---|---|
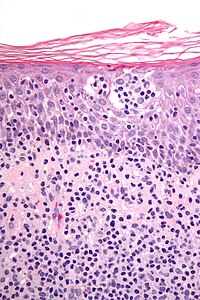 | |
| Micrograph showing cutaneous T-cell lymphoma. H&E stain | |
| Specialty | Hematology and oncology |
Cutaneous T-cell lymphoma (CTCL) is a class of
Signs and symptoms
The presentation depends if it is
Cause
The cause of CTCL remains largely unknown, but several external risk factors have been proposed as potential triggers and promoters of the disease. These include the use of
Diagnosis
A point-based algorithm for the diagnosis for early forms of cutaneous T-cell lymphoma was proposed by the International Society for Cutaneous Lymphomas in 2005.[3]
Classification
Cutaneous T-cell lymphoma may be divided into the several subtypes.
- Pagetoid reticulosis
- Sézary syndrome
- Granulomatous slack skin
- Lymphomatoid papulosis
- Pityriasis lichenoides chronica
- Pityriasis lichenoides et varioliformis acuta
- CD30+ cutaneous T-cell lymphoma
- Secondary cutaneous CD30+ large cell lymphoma
- Non-mycosis fungoides CD30− cutaneous large T-cell lymphoma
- Pleomorphic T-cell lymphoma
- Lennert lymphoma
- Subcutaneous T-cell lymphoma
- Angiocentric lymphoma
- Blastic NK-cell lymphoma
- Primary cutaneous anaplastic large-cell lymphoma
Treatment

There is no cure for CTCL, but there are a variety of treatment options available and some CTCL patients are able to live normal lives with this cancer, although symptoms can be debilitating and painful, even in earlier stages. FDA approved treatments include the following:[9]
- (1999) Denileukin diftitox (Ontak)
- (2000) Bexarotene (Targretin) a retinoid
- (2006) Vorinostat (Zolinza) a hydroxymate histone deacetylase (HDAC) inhibitor
- (2009) Romidepsin (Istodax) a cyclic peptide histone deacetylase (HDAC) inhibitor
- (2018) Poteligeo(mogamulizumab-kpkc)
Histone deacetylase (HDAC) inhibitors are shown to have antiproliferative and cytotoxic properties against CTCL.[10] Other (off label) treatments include:
- Topical and oral corticosteroids
- Bexarotene (Targretin) gel and capsules
- Carmustine (BCNU, a nitrosourea)
- Mechlorethamine(nitrogen mustard)
- Phototherapy(broad and narrow band UVB or PUVA)
- Electron therapy
- Conventional radiation therapy
- Photopheresis
- Interferons
- Alemtuzumab (Campath-1H)
- Methotrexate
- Pentostatin and other purine analogues (Fludarabine, 2-deoxychloroadenosine)
- Liposomal doxorubicin (Doxil)
- Gemcitabine (Gemzar)
- Cyclophosphamide
- Bone marrow / stem cells
- Allogenic transplantation
- Forodesine (inhibits purine nucleoside phosphorylase)
In 2010, the U.S. Food and Drug Administration granted orphan drug designation for naloxone lotion as a treatment for pruritus in cutaneous T-cell lymphoma to a pharmaceutical company called Elorac.[11]
Epidemiology
Of all
There is some evidence of a relationship with
See also
- Cutaneous B-cell lymphoma
- List of cutaneous conditions
References
- ^ "Cutaneous T-Cell Lymphoma: Practice Essentials, Background, Pathophysiology". 2016-06-02.
{{cite journal}}: Cite journal requires|journal=(help) - PMID 31106143.
- PMID 16310068.
- ISBN 978-0-7216-2921-6.
- S2CID 44407772.
- PMID 15692063.
- S2CID 13571836.
- S2CID 213450901.
- ^ S2CID 28520647.
- ISBN 9783319479064.
- ^ Elorac, Inc. Announces Orphan Drug Designation for Novel Topical Treatment for Pruritus in Cutaneous T-cell Lymphoma (CTCL) Archived 2010-12-30 at the Wayback Machine website
- ISBN 978-0-7817-5007-3.
Frequency of lymphoid neoplasms. (Source: Modified from WHO Blue Book on Tumour of Hematopoietic and Lymphoid Tissues. 2001, p. 2001.)
External links
