Dermatitis herpetiformis
| Dermatitis herpetiformis | |
|---|---|
| Other names | Duhring's disease[1][2] |
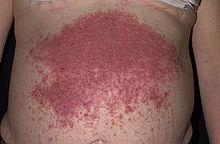 | |
| Characteristic rash of dermatitis herpetiformis | |
| Specialty | Dermatology |
Dermatitis herpetiformis (DH) is a
The age of onset is usually about 15 to 40, but DH also may affect children and the elderly. Men are slightly more affected than women.
Dermatitis herpetiformis was first described by Louis Adolphus Duhring in 1884.[12] A connection between DH and coeliac disease was recognized in 1967.[12][13]
Signs and symptoms

Dermatitis herpetiformis is characterized by intensely
The signs and symptoms of DH typically appear around 30 to 40 years of age, although all ages may be affected.
Dermatitis herpetiformis symptoms are
The rash caused by dermatitis herpetiformis forms and disappears in three stages. In the first stage, the patient may notice a slight discoloration of the
Pathophysiology

In terms of pathology, the first signs of the condition may be observed within the
When looked at under the
Direct IMF studies of uninvolved skin show IgA in the dermal papillae and patchy granular IgA along the basement membrane. The jejunal mucosa may show partial villous atrophy, but the changes tend to be milder than in coeliac disease.[18]
Immunological studies revealed findings that are similar to those of coeliac disease in terms of
Various research studies have pointed out different potential factors that may play a larger or smaller role in the development of dermatitis herpetiformis. The fact that eTG has been found in precipitates of skin-bound IgA from skin affected by this condition has been used to conclude that dermatitis herpetiformis may be caused by a deposition of both IgA and eTG within the dermis. It is estimated that these deposits may resorb after ten years of following a gluten-free diet. Moreover, it is suggested that this condition is closely linked to
Dermatitis herpetiformis may be characterised based on inflammation in the skin and gut. Inflammation in the gut is similar to, and linked to,
The purportedly cross-reactive autoantibodies may migrate to the skin in dermatitis herpetiformis. IgA deposits may form if the antibodies cross-react with epidermal transglutanimase (eTG). Some patients have eTG-specific antibodies instead of tTG-specific cross-reactive antibodies and the relationship between dermatitis herpetiformis and celiac disease in these patients is not fully understood. Macrophages may be stimulated to secrete IL-8 by the same process as is seen in the gut, causing neutrophils to accumulate at sites of high eTG concentrations in the
Diagnosis
Dermatitis herpetiformis often is misdiagnosed, being confused with drug eruptions, contact dermatitis, dishydrotic eczema (dyshidrosis), and even scabies.[22] Other diagnoses in the differential diagnosis include bug bites and other blistering conditions such as bullous pemphigoid, linear IgA bullous dermatosis, and bullous systemic lupus erythematosus.

The diagnosis may be confirmed by a simple
As with ordinary celiac disease, IgA against transglutaminase disappears (often within months) when patients eliminate gluten from their diet. Thus, for both groups of patients, it may be necessary to restart gluten for several weeks before testing may be done reliably. In 2010, Cutis reported an eruption labelled gluten-sensitive dermatitis which is clinically indistinguishable from dermatitis herpetiformis, but lacks the IgA connection,[27] similar to gastrointestinal symptoms mimicking coeliac disease but without the diagnostic immunological markers.[28]
Treatment
First-line therapy
A strict gluten-free diet must be followed,[25] and usually, this treatment will be a lifelong requirement. Avoidance of gluten will reduce any associated intestinal damage[15][25] and the risk of other complications. It can be very difficult to maintain a strict gluten-free diet, however, as contamination with gluten is common in many supposedly gluten-free foods and restaurants.
Alternative treatment options
For individuals with DH unable to tolerate dapsone for any reason, alternative treatment options may include the following:
Combination therapy with nicotinamide and tetracyclines has been shown to be effective and well tolerated in some individuals who cannot tolerate dapsone or live in places where dapsone is not readily available.[31][32][33] While the mechanism of action of tetracyclines and nicotinamide in DH is unknown, it is speculated to be due to their immune-modulating effects.[32]
Topical steroid medications are also sometimes used in combination with dapsone and a gluten-free diet to alleviate the itchiness associated with the rash.[26]
Prognosis
Dermatitis herpetiformis generally responds well to
Dermatitis herpetiformis does not usually cause complications on its own, without being associated with another condition. Complications from this condition, however, arise from the autoimmune character of the disease, as an overreacting immune system is a sign that something does not work well and might cause problems to other parts of the body that do not necessarily involve the
Gluten intolerance and the body's reaction to it make the disease more worrying in what concerns the possible complications. This means that complications that may arise from dermatitis herpetiformis are the same as those resulting from coeliac disease, which include osteoporosis, certain kinds of gut cancer, and an increased risk of other autoimmune diseases such as thyroid disease.
The risks of developing complications from dermatitis herpetiformis decrease significantly if the affected individuals follow a gluten-free diet.
Epidemiology
Global estimates of the prevalence of dermatitis herpetiformis range from 1 in 400 to 1 in 10,000 people. Individuals of Northern European descent are most likely to be affected and estimates of the rates of DH in British and Finnish populations range from 30 in 100,000 to 75 in 100,000 people, respectively. The annual incidence rate of DH in these populations range from 0.8 to 2.7 per 100,000.[37]
People of all ages may be affected, although the mean age at diagnosis varies between 30 and 40 years of age.[6] There is a slight male predominance in DH for unknown reasons and it is associated with celiac disease and the haplotypes HLA-DQ2 and, less commonly, HLA-DQ8.[11]
Notable cases
It has been suggested that French revolutionary Jean-Paul Marat had DH. Marat was known to have a painful skin disease, from which he could only achieve relief by immersing himself in a bathtub filled with an herbal mixture; it was in this tub that he was famously assassinated, as portrayed in The Death of Marat. A researcher suggested in 1979 that the mysterious skin disease was DH based on these symptoms and this regimen of self-treatment.[37]
See also
References
- ^ ISBN 0-07-138076-0.
- ISBN 978-1-4160-2999-1.
- PMID 17656946.
- ^ a b c d e "Dermatitis Herpetiformis". American Osteopathic College of Dermatology.
- ^ "Dermatitis Herpetiformis". Retrieved 2015-04-20.[permanent dead link]
- ^ S2CID 23165241.
- ^ a b c Miller JL, Collins K, Sams HH, Boyd A (2007-05-18). "Dermatitis Herpetiformis". emedicine from WebMD.
{{cite journal}}: Cite journal requires|journal=(help) - ^ PMID 18319038.
- ^ "Dermatitis Herpetiformis". Patient UK. Archived from the original on 2013-07-06. Retrieved 2009-07-22.
- ^ a b c "Dermatitis Herpetiformis". National Digestive Diseases Information Clearinghouse. Archived from the original on 2009-07-20. Retrieved 2009-07-22.
- ^ PMID 9027962.
- ^ a b "What Is Dermatitis Herpetiformis?".
- PMID 17762854.
- PMID 15748547.
- ^ a b c d e "Dermatitis Herpetiformis". The HealthScout Network. Archived from the original on 2009-02-25. Retrieved 2009-07-22.
- ^ PMID 9518950. Archived from the originalon 2011-10-20. Retrieved 2009-07-22.
- ^ "Dermatitis Herpetiformis". Celiac Disease Foundation. Retrieved 2019-03-11.
- ^ "Perioral Dermatitis". Archived from the original on 2010-07-03. Retrieved 2010-06-23.
- ISBN 978-0815342434.
- PMID 25387490.
- PMID 21571167.
- ^ "What's The Diagnosis #9". Emergency Physicians Monthly. 15 April 2010. Retrieved 27 September 2011.
- PMID 25999753.
- PMID 29630215.) Last Update: July 11, 2019.
{{cite journal}}: CS1 maint: multiple names: authors list (link - ^ a b c d "Dermatitis herpetiformis". DermNet NZ.
- ^ a b "Dermatitis herpetiformis". www.uptodate.com. Retrieved 11 March 2019.
- PMID 21284279.
- S2CID 7329242.)
{{cite journal}}: CS1 maint: multiple names: authors list (link - PMID 12165212.
- PMID 25922672.
- PMID 30390734.
- ^ PMID 8445075.
- PMID 15412276.
- PMID 9115907.
- PMID 8949426.
- ^ "Herpetiformis Dermatitis Effects And Complications". Archived from the original on 2010-06-26. Retrieved 2010-06-23.
- ^ PMID 396805.
Further reading
- Kárpáti S (2012). "Dermatitis herpetiformis". Clinics in Dermatology (Review). 30 (1): 56–9. S2CID 206774423.
