Dermatomyositis
| Dermatomyositis | |
|---|---|
| Frequency | ~ 1 per 100,000 people per year[3] |
Dermatomyositis (DM) is a
The cause is unknown.
Eighty percent of adults with adult-onset dermatomyositis have a myositis-specific antibody (MSA).[5]
Sixty percent of children with juvenile dermatomyositis have a myositis-specific antibody (MSA).[6]
Although no cure for the condition is known, treatments generally improve symptoms.
About one per 100,000 people per year are newly affected.[3] The condition usually occurs in those in their 40s and 50s with women being affected more often than men.[3] People of any age, however, may be affected.[3] The condition was first described in the 1800s.[7]
Signs and symptoms
The main symptoms include several kinds of skin rash along with muscle weakness in both upper arms or thighs.[2]
Skin
One form the rashes take is called "
If a person exhibits only skin findings characteristic of DM, without weakness or abnormal muscle enzymes, then he or she may be experiencing amyopathic dermatomyositis (ADM), formerly known as "dermatomyositis sine myositis".[10]
Muscles
People with DM experience progressively worsening muscle weakness in the
Other
Around 30% of people have swollen, painful joints, but this is generally mild.[12]
In some people, the condition affects the lungs, and they may have a cough or difficulty breathing. If the disease affects the heart,
There are further complications possible with dermatomyositis. These complications include difficulty swallowing due to the muscles in the esophagus being affected which can result in malnutrition and can cause the breathing of food or liquids, into the lungs.
- Examples of dermatomyositis
-
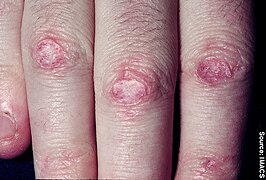
Gottron's papules on finger joints
-
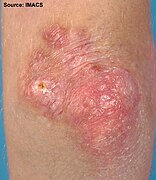
Gottron's papules on the elbows of a person with juvenile DM
-
Gottron's papules
-
Gottron's bumps on a person with juvenile DM
-
Gottron's papules in a severe case of juvenile dermatomyositis
-
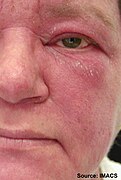
Heliotrope with swelling around the eyes
-
Heliotrope
-
Facial rash
-
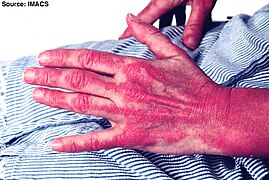
Severe rash on the hands, extending up the forearm
-
Forearm rash
Causes
The cause is unknown, but it may result from an initial viral infection or cancer, either of which could raise an
Between 7 and 30% of dermatomyositis cases
Some cases are inherited, and HLA subtypes HLA-DR3, HLA-DR52, and HLA-DR6 seem to create a disposition to autoimmune dermatomyositis.[12]
Diagnosis



The diagnosis of dermatomyositis is based on five criteria, which are also used to differentially diagnose with respect to polymyositis:[10]
- Muscle weakness in both thighs or both upper arms
- Using a
- Using motor neurons that have multiple phases; and sharp activity when a needle is inserted into the muscle
- Examining a muscle biopsy under a microscope and finding mononuclear white blood cells between the muscle cells, and finding abnormal muscle cell degeneration and regeneration, dying muscle cells, and muscle cells being consumed by other cells (phagocytosis)
- Rashes typical of dermatomyositis, which include heliotrope rash, Gottron sign, and Gottron papules
The fifth criterion is what differentiates dermatomyositis from polymyositis; the diagnosis is considered definite for dermatomyositis if three of items 1 through 4 are present in addition to 5, probable with any two in addition to 5, and possible if just one is present in addition to 5.[10]
Dermatomyositis is associated with
Magnetic resonance imaging may be useful to guide muscle biopsy and to investigate involvement of internal organs;[14] X-ray may be used to investigate joint involvement and calcifications.[15]
A given case of dermatomyositis may be classified as amyopathic dermatomyositis if only skin is affected and no muscle weakness for longer than 6 months is seen according to one 2016 review,[10] or two years according to another.[9]
Classification
Dermatomyositis is a form of systemic
It has also been classified as an idiopathic inflammatory myopathy, along with polymyositis, necrotizing autoimmune myositis, cancer-associated myositis, and sporadic inclusion body myositis.[17]
A form of this disorder that occurs prior to adulthood is known as juvenile dermatomyositis.[18]
Treatment
No cure for dermatomyositis is known, but the symptoms can be treated. Options include medication, physical therapy, exercise, heat therapy (including microwave and ultrasound), orthotics and assistive devices, and rest. The standard treatment for dermatomyositis is a
Physical therapy is usually recommended to prevent muscle atrophy and to regain muscle strength and range of motion. Many individuals with dermatomyositis may need a topical ointment, such as topical corticosteroids, for their skin disorder. They should wear high-protection sunscreen and protective clothing. Surgery may be required to remove calcium deposits that cause nerve pain and recurrent infections.[20]
Rituximab is used when people do not respond to other treatments.[21][22]
As of 2016, treatments for amyopathic dermatomyositis in adults did not have a strong evidence base; published treatments included antimalarial medications,
Prognosis
Before the advent of modern treatments such as prednisone, intravenous immunoglobulin,
The cutaneous manifestations of dermatomyositis may or may not improve with therapy in parallel with the improvement of the myositis. In some people, the weakness and rash resolve together. In others, the two are not linked, with one or the other being more challenging to control. Often, cutaneous disease persists after adequate control of the muscle disease.[24][25]
The risk of death from the condition is much higher if the heart or lungs are affected.[17][20]
Epidemiology
Incidence of DM peaks at ages 40–50, but the disease can affect people of all ages.[26][3] It tends to affect more women than men.[3] The prevalence of DM ranges from one to 22 per 100,000 people.[27][28][29]
History
The diagnostic criteria were proposed in 1975 and became widely adopted.[9][30] Amyopathic DM, also called DM sine myositis, was named in 2002.[9]
People who were affected with dermatomyositis
- Opera singer Maria Callas (1923–1977) allegedly had dermatomyositis from 1975 until her death.[31]
- Actor Laurence Olivier (1907–1989) had dermatomyositis from 1974 until his death.[32]
- American football running back Ricky Bell (1955–1984), the runner-up for the Heisman Trophy in 1976, and the number-one pick in the NFL draft in 1977, died at the age of 29 from heart failure caused by this disease.[33]
- Rob Buckman (1948–2011) a doctor, comedian, author, and the president of the Humanist Association of Canada.[34]
- Samantha, Indian actress diagnosed in 2022
- Suhani Bhatnagar (2005-2024), Indian actress[35]
Research
As of 2016, research was ongoing into causes for DM, as well as
References
- ^ a b c d e f g h i j k l m n o p q r s "Dermatomyositis". GARD. 2017. Archived from the original on 5 July 2017. Retrieved 13 July 2017.
- ^ PMID 16966018.
- ^ a b c d e f g h i j "Dermatomyositis". NORD (National Organization for Rare Disorders). 2015. Archived from the original on 19 February 2017. Retrieved 13 July 2017.
- PMID 35003769.
- PMID 23566358.
Myositis-specific autoantibodies (MSAs) can now be identified in 80% of adults.
- PMID 37188756.
Approximately 60% of patients with JDM are positive for a myositis-specific antibody (MSA).
- ISBN 978-3-540-79312-0.
- ^ S2CID 29083422.
- ^ PMID 27481041.
- ^ S2CID 45638288.
- ^ S2CID 37761391.
- ^ a b c d e f g Hajj-ali RA (June 2013). "Polymyositis and Dermatomyositis – Musculoskeletal and Connective Tissue Disorders". Merck Manuals Professional Edition. Archived from the original on 12 October 2015.
- ^ PMID 24975953.
- PMID 27379096.
- PMID 27871347.
- ^ "ICD-10 Systemic connective tissue disorders (M30-M36)". WHO. Archived from the original on 8 February 2017. Retrieved 9 December 2016.
- ^ PMID 26826433.
- S2CID 205951454.
- ^ "Dermatomyositis (DM)". The Lecturio Medical Concept Library. Retrieved 11 July 2021.
- ^ a b "Dermatomyositis Information". National Institute of Neurological Disorders and Stroke. 27 July 2015. Archived from the original on 2 December 2016.
- PMID 27242652.
- S2CID 7104535.
- ^ Page 285 in: Thomson and Cotton Lecture Notes in Pathology, Blackwell Scientific. Third Edition
- ^ "Dermatomyositis". Genetic and Rare Diseases Information Center (GARD). Retrieved 11 July 2021.
- ^ "Dermatomyositis". Johns Hopkins Medicine. 19 November 2019. Retrieved 11 July 2021.
- PMID 4093921.
- PMID 12848952.
- S2CID 21500536.
- PMID 20083689.
- PMID 1089199.
- ^ "Greek Reporter: 'Maria Callas did not kill herself from grief for Onassis, a rare disease cost her career and life'". GR Reporter. 28 December 2010. Archived from the original on 4 January 2015. Retrieved 1 January 2015.
- ^ "Laurence Olivier Dies: 'The Rest Is Silence'". People Magazine. 24 July 1989. Archived from the original on 10 March 2011. Retrieved 16 July 2012.
- ^ "Forgotten: Ricky Bell". Pro Football Weekly. 8 January 2010. Archived from the original on 11 January 2010. Retrieved 26 January 2010.
- ^ Jones T (12 October 2011). "Rob Buckman obituary". The Guardian. Archived from the original on 1 October 2013. Retrieved 16 July 2012.
- ^ "'Dangal' actor Suhani Bhatnagar succumbs to dermatomyositis: Know about this rare condition". The Times of India. 18 February 2024.
- PMID 27784516.
![]() This article incorporates public domain material from NINDS Dermatomyositis Information Page. United States Department of Health and Human Services. Retrieved 12 December 2016.
This article incorporates public domain material from NINDS Dermatomyositis Information Page. United States Department of Health and Human Services. Retrieved 12 December 2016.