Diagnosis of malaria
The mainstay of
Blood films
| Species | Appearance | Periodicity | Liver persistent |
|---|---|---|---|
| Plasmodium vivax |  |
tertian | yes |
| Plasmodium ovale |  |
tertian | no |
| Plasmodium falciparum |  |
tertian | no |
| Plasmodium malariae | 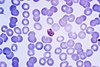 |
quartan | no |
The most economic, preferred, and reliable diagnosis of malaria is microscopic examination of
From the thick film, an experienced microscopist can detect parasite levels (or parasitemia) as few as 5 parasites/µL blood.[6] Diagnosis of species can be difficult because the early trophozoites ("ring form") of all four species look similar and it is never possible to diagnose species on the basis of a single ring form; species identification is always based on several trophozoites.[citation needed]
As malaria becomes less prevalent due to interventions such as bed nets, the importance of accurate diagnosis increases. This is because the assumption that any patient with a fever has malaria becomes less accurate. As such, significant research is being put into developing low cost microscopy solutions for the
Plasmodium malariae and P. knowlesi (which is the most common cause of malaria in Southeast Asia) look very similar under the microscope. However, P. knowlesi parasitemia increases very fast and causes more severe disease than P. malariae, so it is important to identify and treat infections quickly. Therefore, modern methods such as PCR (see "Molecular methods" below) or monoclonal antibody panels that can distinguish between the two should be used in this part of the world.[8]
Antigen tests
For areas where microscopy is not available, or where laboratory staff are not experienced at malaria diagnosis, there are commercial antigen detection tests that require only a drop of blood.
The first rapid diagnostic tests were using Plasmodium glutamate dehydrogenase as antigen.[3] PGluDH was soon replaced by Plasmodium
Modern rapid diagnostic tests for malaria often include a combination of two antigens such as a P. falciparum. specific antigen e.g. histidine-rich protein II (HRP II) and either a P. vivax specific antigen e.g. P. vivax LDH or an antigen sensitive to all plasmodium species which affect humans e.g. pLDH. Such tests do not have a sensitivity of 100% and where possible, microscopic examination of blood films should also be performed.[citation needed]
Molecular methods
Molecular methods are available in some clinical laboratories and rapid real-time assays (for example, QT-NASBA based on the polymerase chain reaction)[4] are being developed with the hope of being able to deploy them in endemic areas.[citation needed]
PCR (and other molecular methods) is more accurate than microscopy. However, it is expensive, and requires a specialized laboratory. Moreover, levels of parasitemia are not necessarily correlative with the progression of disease, particularly when the parasite is able to adhere to blood vessel walls. Therefore, more sensitive, low-tech diagnosis tools need to be developed in order to detect low levels of parasitemia in the field.[10]
Another approach is to detect the iron crystal byproduct of hemoglobin that is found in malaria parasites feasting on red blood cells, but not found in normal blood cells. It can be faster, simpler and precise than any other method. Researchers at Rice University have published a preclinical study of their new tech that can detect even a single malaria-infected cell among a million normal cells.[11][12] They claim it can be operated by nonmedical personal, produce zero false-positive readings, and it doesn't need a needle or any damage done.
Over- and misdiagnosis
Multiple recent studies have documented malaria overdiagnosis as a persistent issue globally, but especially in African countries.[13][14] Overdiagnosis results in over-inflation of actual malaria rates reported at the local and national levels.[15] Health facilities tend to over-diagnose malaria in patients presenting with symptoms such as fever, due to traditional perceptions such as "any fever being equivalent to malaria"[15] and issues related to laboratory testing (for example high false positivity rates of diagnosis by unqualified personnel [16]). Malaria overdiagnosis leads to under management of other fever-inducing conditions, over-prescription of antimalarial drugs [17][15] and exaggerated perception of high malaria endemicity in regions which are no longer endemic for this infection.[15]
Subjective diagnosis
Areas that cannot afford laboratory diagnostic tests often use only a history of subjective fever as the indication to treat for malaria. Using Giemsa-stained blood smears from children in Malawi, one study showed that when clinical predictors (rectal temperature, nailbed pallor, and splenomegaly) were used as treatment indications, rather than using only a history of subjective fevers, a correct diagnosis increased from 2% to 41% of cases, and unnecessary treatment for malaria was significantly decreased.[10]
Differential
Fever and septic shock are commonly misdiagnosed as severe malaria in Africa, leading to a failure to treat other life-threatening illnesses. In malaria-endemic areas, parasitemia does not ensure a diagnosis of severe malaria, because parasitemia can be incidental to other concurrent disease. Recent investigations suggest that malarial retinopathy is better (collective sensitivity of 95% and specificity of 90%) than any other clinical or laboratory feature in distinguishing malarial from non-malarial coma.[18]
Quantitative buffy coat
Quantitative buffy coat (QBC) is a laboratory test to detect infection with malaria or other blood parasites. The blood is taken in a QBC capillary tube which is coated with acridine orange (a fluorescent dye) and centrifuged; the fluorescing parasites can then be observed under ultraviolet light at the interface between red blood cells and buffy coat. This test is more sensitive than the conventional thick smear, however it is unreliable for the differential diagnosis of species of parasite.[19]
In cases of extremely low white blood cell count, it may be difficult to perform a manual differential of the various types of white cells, and it may be virtually impossible to obtain an automated differential. In such cases the medical technologist may obtain a buffy coat, from which a blood smear is made. This smear contains a much higher number of white blood cells than whole blood.[citation needed]
References
- S2CID 19829220.
- PMID 19432543.
- ^ S2CID 16953840.
- ^ PMID 17018138.
- PMID 8813948.
- ISBN 978-0-443-06668-9. Retrieved 22 June 2011.
- PMID 32637243.
- PMID 18976561.
- PMID 16117960.
- ^ S2CID 10931276.
- ^ "Vapor nanobubbles rapidly detect malaria through the skin Archived 2014-01-08 at the Wayback Machine", news.rice.edu
- ^ "Hemozoin-generated vapor nanobubbles for transdermal reagent- and needle-free detection of malaria", Ekaterina Y. L., et al. DOI:10.1073/pnas.1316253111
- PMID 27604542.
- PMID 15542534.
- ^ PMID 18986520.
- PMID 27842555.
- PMID 26628068.
- PMID 17123967.
- PMID 17683979.
