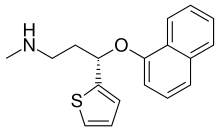
Duloxetine
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Cymbalta, Ariclaim, Yentreve, others[1] |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a604030 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth |
| Drug class | Serotonin–norepinephrine reuptake inhibitor |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | ~ 50% (32% to 80%) |
| Protein binding | ~ 95% |
| Metabolism | Liver, two P450 isozymes, CYP2D6 and CYP1A2 |
| Elimination half-life | 12 hours |
| Excretion | 70% in urine, 20% in feces |
| Identifiers | |
| |
JSmol) | |
| |
| |
| | |
Duloxetine, sold under the brand name Cymbalta among others,
Duloxetine is a serotonin–norepinephrine reuptake inhibitor (SNRI).[9] Similarly to SSRIs and other SNRIs, the precise mechanism for its antidepressant and anxiolytic effects is not known.[7]
Common side effects include
Duloxetine was approved for medical use in the United States and in the European Union in 2004.
Medical uses
The main uses of duloxetine are in
Duloxetine is recommended as a first-line agent for the treatment of chemotherapy-induced neuropathy by the American Society of Clinical Oncology,[14] as a first-line therapy for fibromyalgia in the presence of mood disorders by the German Interdisciplinary Association for Pain Therapy,[15] as a Grade B recommendation for the treatment of diabetic neuropathy by the American Association for Neurology[16] and as a level A recommendation in certain neuropathic states by the European Federation of Neurological Societies.[17]
A 2014 Cochrane review concluded that duloxetine is beneficial in the treatment of diabetic neuropathy and fibromyalgia but that more comparative studies with other medicines are needed.[18] The French medical journal Prescrire concluded that duloxetine is no better than other available agents and has a greater risk of side effects.[19]
Major depressive disorder
Duloxetine was approved for the treatment of major depression in 2004.[4][5] While duloxetine has demonstrated improvement in depression-related symptoms compared to placebo, comparisons of duloxetine to other antidepressant medications have been less successful. A 2012 Cochrane Review did not find greater efficacy of duloxetine compared to SSRIs and newer antidepressants. Additionally, the review found evidence that duloxetine has increased side effects and reduced tolerability compared to other antidepressants. It thus did not recommend duloxetine as a first line treatment for major depressive disorder, given the (then) high cost of duloxetine compared to inexpensive off-patent antidepressants and lack of increased efficacy.[20] Duloxetine appears less tolerable than some other antidepressants.[21] Generic duloxetine became available in 2013.[22]
Generalized anxiety disorder
Duloxetine is more effective than placebo in the treatment of generalized anxiety disorder (GAD).[23] A review from the Annals of Internal Medicine lists duloxetine among the first line drug treatments along with citalopram, escitalopram, sertraline, paroxetine, and venlafaxine.[24]
Neuropathic pain
Duloxetine was approved for the pain associated with diabetic
The comparative efficacy of duloxetine and established pain-relief medications for DPN is unclear. A systematic review noted that
Duloxetine is also an option for the management of neuropathic pain in multiple sclerosis patients.[34]
Fibromyalgia and chronic pain
A review of duloxetine found that it reduced pain and fatigue, and improved physical and mental performance compared to placebo.[35]
The U.S. Food and Drug Administration (FDA) approved the drug for the treatment of fibromyalgia in June 2008.[36][37]
It may be useful for chronic pain from osteoarthritis.[38][39]
On 4 November 2010, the U.S. Food and Drug Administration (FDA) approved duloxetine to treat chronic musculoskeletal pain, including discomfort from osteoarthritis and chronic lower back pain.[40][41]
Stress urinary incontinence
Duloxetine failed to receive US approval for stress urinary incontinence amid concerns over liver toxicity and suicidal events; it was approved for this use in the UK, however, where it is recommended as an add-on medication in stress urinary incontinence instead of surgery.[42]
The safety and utility of duloxetine in the treatment of incontinence has been evaluated in a series of meta analyses and practice guidelines.
- A 2017 meta-analysis found that harms are at least as great if not greater than the benefits.[43]
- A 2013 meta-analysis concluded that duloxetine decreased incontinence episodes more than placebo with people about 56% more likely than placebo to experience a 50% decrease in episodes. Adverse effects were experienced by 83% of duloxetine-treated subjects and by 45% of placebo-treated subjects.[44]
- A 2012 review and practice guideline published by the European Association of Urology concluded that the clinical trial data provides Grade 1a evidence that duloxetine improves but does not cure urinary incontinence, and that it causes a high rate of gastrointestinal side effects (mainly nausea and vomiting) leading to a high rate of treatment discontinuation.[45]
- The National Institute for Clinical and Health Excellence recommends (as of September 2013) that duloxetine not be routinely offered as first line treatment, and that it only be offered as second line therapy in women wishing to avoid therapy. The guideline further states that women should be counseled regarding the drug's side effects.[46]
Contraindications
The following contraindications are listed by the manufacturer:[47]
- Hypersensitivity: duloxetine is contraindicated in patients with a known hypersensitivity to duloxetine or any of the inactive ingredients.
- Monoamine oxidase inhibitors (MAOIs): concomitant use in patients taking MAOIs is contraindicated.
- Uncontrolled narrow-angle , in which mydriasis can cause sudden worsening.
- Central nervous system (CNS) acting drugs: given the primary CNS effects of duloxetine, it should be used with caution when it is taken in combination with or substituted for other centrally acting drugs, including those with a similar mechanism of action.
- Duloxetine and thioridazine should not be co-administered.[note 1]
In addition, the FDA has reported on life-threatening drug interactions that may be possible when co-administered with triptans and other drugs acting on serotonin pathways leading to increased risk for serotonin syndrome.[49]
Duloxetine should also be avoided in hepatic impairment such as cirrhosis.[50]
Adverse effects
In a trial for major depressive disorder (MDD), the most commonly reported treatment-emergent adverse events among duloxetine-treated patients were
Sexual dysfunction
In four clinical trials of duloxetine for the treatment of MDD, sexual dysfunction occurred significantly more frequently in patients treated with duloxetine than those treated with placebo, and this difference occurred only in men.[55][54] Specifically, common side effects include difficulty becoming aroused, lack of interest in sex, and anorgasmia (trouble achieving orgasm). Loss of or decreased response to sexual stimuli and ejaculatory anhedonia are also reported.[56] Frequency of treatment-emergent sexual dysfunction were similar for duloxetine and SSRIs when compared in a 6-month observational study in depressed patients.[57] Rates of sexual dysfunction in MDD patients treated with duloxetine vs escitalopram did not differ significantly at 4, 8, and 12 weeks of treatment, although the trend favored duloxetine (33.3% of duloxetine patients experienced sexual side effects compared to 43.6% of those receiving escitalopram and 25% of those receiving placebo).[56]
Increased sweating
Duloxetine may also cause sweating more than usual (hyperhidrosis).[58][59] The exact mechanism behind why duloxetine increases sweating is still not fully understood. However, a possible explanation is in duloxetine's action on the sympathetic nervous system. Sympathetic nerves control thermoregulation and sweating in humans; when increased levels of noradrenaline are present (as seen with SNRIs), this can stimulate sweat gland activity, leading to an increase in perspiration. Noradrenaline release may also cause increased serotonin availability that results from inhibiting reuptake enhances and further facilitates the activation of post-synaptic α-adrenoceptors by noradrenaline, which can stimulate sweat gland activity, leading to more significant amounts of copious liquid secretion mainly at higher duloxetine dosages above certain thresholds. The degree of noradrenergic "tone" determined by the interaction between noradrenergic and serotonergic neurons may determine the amount of sweating experienced; therefore, at higher doses or concentrations, serum resulting from therapeutic antidepressant treatment patients may show excess perspiration than usual as compared to low doses.[60]
Discontinuation syndrome
During marketing of other
When discontinuing treatment with duloxetine, the manufacturer recommends a gradual reduction in the dose, rather than abrupt cessation, whenever possible. If intolerable symptoms occur following a decrease in the dose or upon discontinuation of treatment, then resuming the previously prescribed dose may be considered. Subsequently, the physician may continue decreasing the dose but at a more gradual rate.
In placebo-controlled clinical trials of up to nine weeks' duration of patients with MDD, a systematic evaluation of discontinuation symptoms in patients taking duloxetine following abrupt discontinuation found the following symptoms occurring at a rate greater than or equal to 2% and at a significantly higher rate in duloxetine-treated patients compared to those discontinuing from placebo: dizziness, nausea, headache, paresthesia, vomiting, irritability, and nightmare.[61]
In 2012 The Institute for Safe Medical Practices (ISMP) published a report: "Duloxetine and Serious Withdrawal Symptoms". The report highlights early clinical studies which found "abrupt discontinuation showed that withdrawal effects occurred in 40-50% of patients, that 10% of those were severe and approximately half were not resolved when side effects monitoring had ended after one or two weeks".
Withdrawal symptoms listed in 48 case reports (in the first quarter of 2012) included anger, crying, dizziness and suicidal ideation.
The report concluded there was insufficient information and a lack of clear warnings about the effects of discontinuing Duloxetine and that in many cases withdrawal symptoms may be "severe, persistent, or both", adding "the prescribing information for physicians and pharmacists does not provide realistic schedules for tapering or a clear picture of the likely incidence of these reactions".
Suicidality
In the United States all antidepressants, including duloxetine carry a
In 2005, the United States FDA released a public health advisory noting that there had been eleven reports of suicide attempts and three reports of suicidality within the mostly middle-aged women participating in the open label extension trials of duloxetine for the treatment of stress urinary incontinence (SUI). The FDA described the potential role of confounding social stressors "unclear". The suicide attempt rate in the SUI study population (based on 9,400 patients) was calculated to be 400 per 100,000 person years. This rate is greater than the suicide attempt rate among middle-aged U.S. women that has been reported in published studies, i.e., 150 to 160 per 100,000 person years. In addition, one death from suicide was reported in a Cymbalta clinical pharmacology study in a healthy female volunteer without SUI. No increase in suicidality was reported in controlled trials of Cymbalta for depression or diabetic neuropathic pain.[65]
Postmarketing reports
Reported adverse events that were temporally correlated to duloxetine therapy include rash, reported rarely, and the following adverse events, reported very rarely:
Pharmacology
Mechanism of action
| Receptor | Ki (nM) |
|---|---|
| SERT | 0.7~0.8 |
| NET | 7.5 |
| DAT | 240 |
| 5-HT2A | 504 |
| 5-HT2C | 916 |
| 5-HT6 | 419 |
Duloxetine inhibits the reuptake of serotonin and norepinephrine (NE) in the central nervous system. Duloxetine increases dopamine (DA) specifically in the prefrontal cortex, where there are few DA reuptake pumps, via the inhibition of NE reuptake pumps (NET), which is believed to mediate reuptake of DA and NE.[69] Duloxetine has no significant affinity for dopaminergic, cholinergic, histaminergic, opioid, glutamate, and GABA reuptake transporters, however, and can therefore be considered to be a selective reuptake inhibitor at the 5-HT and NE transporters. Duloxetine undergoes extensive metabolism, but the major circulating metabolites do not contribute significantly to the pharmacologic activity.[70][71]
In vitro binding studies using synaptosomal preparations isolated from rat cerebral cortex indicated that duloxetine was approximately 3 fold more potent at inhibiting
Pharmacokinetics
Absorption: Duloxetine is acid labile, and is formulated with enteric coating to prevent degradation in the stomach. Duloxetine has good oral bioavailability, averaging 50% after one 60 mg dose. There is an average 2-hour lag until absorption begins with maximum plasma concentrations occurring about 6 hours post dose. Food does not affect the Cmax of duloxetine, but delays the time to reach peak concentration from 6 to 10 hours.[71]
Distribution: Duloxetine is highly bound (>90%) to proteins in human plasma, binding primarily to albumin and α1-acid glycoprotein. Volume of distribution is 1640L.[73]
Metabolism: Duloxetine undergoes predominately hepatic metabolism via two cytochrome P450 isozymes, CYP2D6 and CYP1A2. Circulating metabolites are pharmacologically inactive. Duloxetine is a moderate CYP2D6 inhibitor.[73]
Elimination: Administered in healthy young male subjects at doses between 20 and 40 mg twice a day, had a half-life of 12.5 hours and its pharmacokinetics are dose proportional over the therapeutic range. Steady-state is usually achieved after 3 days. Only trace amounts (<1%) of unchanged duloxetine are present in the urine and most of the dose (approx. 70%) appears in the urine as metabolites of duloxetine with about 20% excreted in the feces.[73]
Smoking is associated with a decrease in duloxetine concentration.[74][75][76]
Research directions
Major depressive disorder is believed to be due in part to an increase in pro-inflammatory cytokines within the central nervous system.[77][78] Antidepressants including ones with a similar mechanism of action as duloxetine, i.e., serotonin metabolism inhibition, cause a decrease in proinflammatory cytokine activity and an increase in anti-inflammatory cytokines;[79] this mechanism may apply to duloxetine in its effect on depression but research on cytokines specific to duloxetine therapy is insufficient.[80][81] Cytokines are immunoregulatory molecules that play a key role in the human immune response. Some cytokines are proinflammatory and contribute to the development of inflammation, while others are anti-inflammatory and help to control the proinflammatory response.[82] Duloxetine can reduce the production of pro-inflammatory cytokines such as interleukin-1 beta (IL-1β), tumor necrosis factor-alpha (TNF-α), and interleukin 6 (IL-6) and may increase the production of anti-inflammatory cytokines such as interleukin 10 (IL-10), however, mechanisms behind these effects are not well elucidated, there have been mixed findings regarding duloxetine's impact on cytokine production in different contexts, and the results are inconclusive.[83][84][85][86]
Duloxetine is being investigated for its potential to decrease opioid use in the perioperative period because duloxetine administration can help reduce opioid consumption and mitigate the risk of opioid-related side effects and dependence. In total hip arthroplasty (THA) or total knee arthroplasty (TKA), duloxetine is researched to provide pain relief; studies demonstrated that it can reduce pain for several weeks post-surgery without an increased risk of adverse drug events, suggesting that duloxetine could be a valuable component of a multimodal management regimen for patients undergoing THA or TKA.[87] Also, duloxetine can reduce postoperative nausea and vomiting after THA or TKA, which are common side effects of anesthesia and opioids: this additional benefit could improve patient comfort and satisfaction, potentially enhancing recovery outcomes.[87]
History

Duloxetine was created by
In 2001, Lilly filed a
After the manufacturing issues were resolved, the liver toxicity warning included in the prescribing information, and the follow-up studies showed that duloxetine does not cause QTc interval prolongation, duloxetine was approved by the FDA for depression and diabetic neuropathy in 2004.[93] In 2007, Health Canada approved duloxetine for the treatment of depression and diabetic peripheral neuropathic pain.[94]
Duloxetine was approved for use of stress urinary incontinence (SUI) in the EU in 2004.[6] In 2005, Lilly withdrew the duloxetine application for stress urinary incontinence (SUI) in the U.S., stating that discussions with the FDA indicated "the agency is not prepared at this time to grant approval ... based on the data package submitted." A year later Lilly abandoned the pursuit of this indication in the U.S. market.[95][96]
The FDA approved duloxetine for the treatment of generalized anxiety disorder in February 2007.[97]
Cymbalta generated sales of nearly US$5 billion in 2012, with US$4 billion of that in the U.S., but its patent protection terminated 1 January 2014. Lilly received a six-month extension beyond 30 June 2013, after testing for the treatment of depression in adolescents, which may produce US$1.5 billion in added sales.[98][99]
The first generic duloxetine was marketed by Indian pharmaceutical company Dr. Reddy's Laboratories.[100]
See also
Explanatory notes
References
- ^ a b "Duloxetine". Drugs.com. Archived from the original on 29 September 2018. Retrieved 24 December 2018.
- FDA. Retrieved 22 October 2023.
- ^ "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 4 April 2023). 31 March 2023. Archived from the original on 3 August 2023. Retrieved 16 August 2023.
- ^ a b c "Cymbalta- duloxetine hydrochloride capsule, delayed release". DailyMed. Archived from the original on 13 August 2020. Retrieved 29 September 2020.
- ^ a b c "Cymbalta EPAR". European Medicines Agency (EMA). 17 September 2018. Archived from the original on 20 October 2020. Retrieved 30 September 2020.
- ^ a b c "Yentreve EPAR". European Medicines Agency (EMA). 17 September 2018. Archived from the original on 24 September 2020. Retrieved 30 September 2020.
- ^ a b c d e f g h i "Duloxetine". Monograph. The American Society of Health-System Pharmacists. Archived from the original on 26 November 2018. Retrieved 24 December 2018.
- ^ "Medications for OCD". International OCD Foundation. Archived from the original on 27 January 2024. Retrieved 25 February 2024.
- ^ ISBN 9780857113382.
- ^ "The Top 300 of 2021". ClinCalc. Archived from the original on 15 January 2024. Retrieved 14 January 2024.
- ^ "Duloxetine - Drug Usage Statistics". ClinCalc. Archived from the original on 12 April 2020. Retrieved 14 January 2024.
- National Institute for Health and Clinical Excellence. Clinical guideline 96: Neuropathic pain – pharmacological management. London, 2010.
- PMID 21482920.
- S2CID 11183183.
- S2CID 1348989.
- S2CID 15020212.
- S2CID 14236933.
- ^ PMID 24385423.
- from the original on 14 July 2014. Retrieved 28 June 2014.
- PMID 23076926.
- PMID 29477251.
- ^ Swiatek J (13 October 2013). "Loss of Cymbalta patent a major blow for Eli Lilly". Indianapolis Star. Archived from the original on 15 January 2014. Retrieved 27 February 2015.
- S2CID 30897102.
- S2CID 42889106.
- PMID 37670573.
- S2CID 10291281.
- PMID 16266355.
- ^ "Application number 21-733. Medical review(s)" (PDF). U.S. Food and Drug Administration (FDA). 3 September 2004. Retrieved 14 April 2009. [dead link]
- PMID 17562735.
- PMID 17121211.
- PMID 18673529.
- from the original on 28 April 2023. Retrieved 28 April 2023.
- PMID 36007534.
- PMID 38421578.
- PMID 19137126.
- ^ "FDA Approves Cymbalta for the Management of Fibromyalgia". Eli Lilly Co. (Press release). 16 June 2008. Archived from the original on 30 July 2008. Retrieved 17 June 2008.
- ^ "Drug Approval Package: Cymbalta (duloxetine hydrochloride) NDA #022148". U.S. Food and Drug Administration (FDA). Archived from the original on 31 October 2020. Retrieved 30 September 2020.
- S2CID 20599116.
- PMID 24618328.
- ^ "FDA clears Cymbalta to treat chronic musculoskeletal pain". U.S. Food and Drug Administration (FDA) (Press release). Food and Drug Administration. 4 November 2010. Archived from the original on 7 August 2013. Retrieved 19 August 2013.
- ^ "Drug Approval Package: Cymbalta (duloxetine hydrochloride) NDA #022516". U.S. Food and Drug Administration (FDA). 16 September 2011. Archived from the original on 5 April 2021. Retrieved 29 September 2020.
- National Institute for Health and Clinical Excellence. Clinical guideline 40: Urinary incontinence. London, 2006.
- PMID 28246265.
- S2CID 10788312.
- ^ "www.uroweb.org" (PDF). Archived from the original (PDF) on 4 May 2014.
- ^ "Urinary incontinence Introduction CG171". Archived from the original on 4 May 2014.
- ^ "Eli Lilly and Company". Archived from the original on 13 April 2010. Retrieved 15 May 2010.
- S2CID 2356196.
- ^ "Information for Healthcare Professionals: Duloxetine (marketed as Cymbalta) – Selective Serotonin Reuptake Inhibitors (SSRIs) or Selective Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs) and 5-Hydroxytryptamine Receptor Agonists (Triptans)". U.S. Food and Drug Administration (FDA). 14 August 2013. Archived from the original on 7 March 2013. Retrieved 18 September 2013.
- S2CID 264888110.
- ^ Cymbalta package insert. Indianapolis, IN: Eli Lilly Pharmaceuticals; 2004, September.
- PMID 16700869.
- S2CID 12208795.
- ^ a b "Cymbalta - FDA prescribing information, side effects and uses". Drugs.com. Archived from the original on 14 September 2018. Retrieved 14 September 2018.
- PMID 16964316.
- ^ PMID 17627739.
- S2CID 23153099.
- ^ "Duloxetine (Oral Route) Side Effects - Mayo Clinic". Mayo Clinic. Archived from the original on 19 October 2023. Retrieved 1 October 2023.
- S2CID 184484229.
- PMID 19664885.
- PMID 16266753.
- ^ Levenson M, Holland C. "Antidepressants and Suicidality in Adults: Statistical Evaluation. (Presentation at Psychopharmacologic Drugs Advisory Committee; December 13, 2006)". Food and Drug Administration. Archived from the original on 27 September 2007. Retrieved 13 May 2007.
- ^ Stone MB, Jones ML (17 November 2006). "Clinical review: relationship between antidepressant drugs and suicidality in adults" (PDF). Overview for December 13 Meeting of Psychopharmacologic Drugs Advisory Committee (PDAC). U.S. Food and Drug Administration (FDA). pp. 11–74. Archived (PDF) from the original on 16 March 2007. Retrieved 22 September 2007.
- ^ Levenson M, Holland C (17 November 2006). "Statistical Evaluation of Suicidality in Adults Treated with Antidepressants" (PDF). Overview for December 13 Meeting of Psychopharmacologic Drugs Advisory Committee (PDAC). U.S. Food and Drug Administration (FDA). pp. 75–140. Archived (PDF) from the original on 16 March 2007. Retrieved 22 September 2007.
- ^ "Historical Information on Duloxetine hydrochloride (marketed as Cymbalta)". U.S. Food and Drug Administration (FDA). Archived from the original on 22 July 2017. Retrieved 16 December 2019.
- ^ "Duloxetine Side Effects, and Drug Interactions". RxList Monographs. Archived from the original on 12 September 2008.
- PMID 11750180.

- ISBN 978-0-19-936258-5. Archivedfrom the original on 25 February 2024. Retrieved 20 October 2020.
- ^ Stahl S (2013). Stahl's Essential Pharmacology (4th ed.). New York: Cambridge University Press. pp. 305, 308, 309.
- S2CID 40022100.
- ^ PMID 15892657.
- PMID 28913467.
- ^ a b c "Cymbalta product insert" (PDF). Archived (PDF) from the original on 31 October 2005. Retrieved 1 November 2005.
- S2CID 207299455.
- S2CID 22045964.
- ^ "Duloxetine 60mg gastro-resistant capsules - Summary of Product Characteristics (SmPC) - (emc)". www.medicines.org.uk. Archived from the original on 21 March 2020. Retrieved 21 March 2020.
- PMID 25003554.
- S2CID 22275879.
- PMID 22981313.
- S2CID 656023.
- PMID 21796103.
- S2CID 2267250.
- PMID 35791513.
- PMID 26556688.
- S2CID 163168228.
- S2CID 235620244.
- ^ PMID 38481321.
- ^ Robertson DW, Wong DT, Krushinski JH (11 September 1990). "United States Patent 4,956,388: 3-Aryloxy-3-substituted propanamines". USPTO. Archived from the original on 7 January 2016. Retrieved 17 May 2008.
- PMID 2850421.
- PMID 14643350.
- ^ Approval package for: application number NDA 721-427. Administrative/Correspondence #2 (PDF) (Report). U.S. Food and Drug Administration (FDA). 2003. Archived (PDF) from the original on 12 February 2017. Retrieved 18 May 2008.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "Drug Approval Package: Cymbalta (Duloxetine Hydrochloride) NDA #021427". U.S. Food and Drug Administration (FDA). 24 December 1999. Archived from the original on 24 September 2020. Retrieved 29 September 2020.
- ^ "FDA news". Food and Drug Administration. Archived from the original on 13 May 2009. Retrieved 16 December 2019.
- ^ "Summary Basis of Decision (SBD): Cymbalta". Health Canada. 5 May 2008. Archived from the original on 1 March 2015. Retrieved 27 February 2015.
- ^ "Lilly Won't Pursue Yentreve for U.S." TheStreet.com. 15 February 2006. Archived from the original on 2 February 2009. Retrieved 18 May 2008.
- PMID 16002878.
- ^ "FDA approves antidepressant Cymbalta (duloxetine HCl) for treatment of generalized anxiety disorder". News-Medical. 26 February 2007. Archived from the original on 15 January 2009. Retrieved 25 December 2013.
- ^ Staton T (9 July 2012). "Lilly could net $1.5B-plus from Cymbalta extension". FiercePharma. Archived from the original on 30 October 2013. Retrieved 25 December 2013.
- ^ Palmer E (11 April 2013). "Eli Lilly to lay off hundreds in sales as Cymbalta nears edge of patent cliff". FiercePharma. Archived from the original on 11 December 2013. Retrieved 25 December 2013.
- ^ Anson P (12 December 2013). "Generic Cheaper Versions of Cymbalta Approved". National Pain Report. Archived from the original on 2 January 2014. Retrieved 2 January 2014.
