Seizure
| Epileptic seizure | |
|---|---|
| Other names | Epileptic fit, |
| Treatment | Less than 5 min: Place person on their side, remove nearby dangerous objects[8] More than 5 min: Treat as per status epilepticus[8] |
| Frequency | ~10% of people (overall worldwide lifetime risk)[5][9] |
A seizure is a period of
Seizures may be provoked and unprovoked.
A seizure that lasts for more than a brief period is a
Up to 10% of people have had at least one epileptic seizure in their lifetime.[5][9] Provoked seizures occur in about 3.5 per 10,000 people a year while unprovoked seizures occur in about 4.2 per 10,000 people a year.[5] After one seizure, the chance of experiencing a second one is about 40%.[12][13] Epilepsy affects about 1% of the population at any given time.[9]
Signs and symptoms
The signs and symptoms of seizures vary depending on the type.
Focal seizures
In a
Jerking activity may start in a specific muscle group and spread to surrounding muscle groups—known as a
Generalized seizures
There are six main types of generalized seizures: tonic-clonic, tonic, clonic, myoclonic, absence, and atonic seizures.[20] They all involve a loss of consciousness and typically happen without warning.[21]
- Tonic-clonic seizures present with a contraction of the limbs followed by their extension, along with arching of the back for 10–30 seconds.[21] A cry may be heard due to contraction of the chest muscles.[21] The limbs then begin to shake in unison.[21] After the shaking has stopped it may take 10–30 minutes for the person to return to normal.[21]
- Tonic seizures produce constant contractions of the muscles.[21] The person may turn blue if breathing is impaired.[21]
- Clonic seizures involve shaking of the limbs in unison.[21]
- Myoclonic seizures involve spasms of muscles in either a few areas or generalized through the body.[21]
- Absence seizures can be subtle, with only a slight turn of the head or eye blinking.[18] The person often does not fall over and may return to normal right after the seizure ends, though there may also be a period of post-ictal disorientation.[18]
- Atonic seizures involve the loss of muscle activity for greater than one second.[19] This typically occurs bilaterally (on both sides of the body).[19]
Duration
A seizure can last from a few seconds to more than five minutes, at which point it is known as status epilepticus.[22] Most tonic-clonic seizures last less than two or three minutes.[22] Absence seizures are usually around 10 seconds in duration.[16]
Postictal
After the active portion of a seizure, there is typically a period of confusion called the
Causes
Seizures have a number of causes. Of those who have a seizure, about 25% have
Different causes of seizures are common in certain age groups.
- metabolic disorders.
- The most frequent cause of seizures in children is febrile seizures, which happen in 2–5% of children between the ages of six months and five years.[28]
- During childhood, well-defined epilepsy syndromes are generally seen.
- In adolescence and young adulthood, non-compliance with the medication regimen and sleep deprivation are potential triggers.
- Pregnancy and labor and childbirth, and the post-partum, or post-natal period (after birth) can be at-risk times, especially if there are certain complications like pre-eclampsia.
- During adulthood, the likely causes are alcohol related, strokes, trauma, CNS infections, and brain tumors.[29]
- In older adults, cerebrovascular disease is a very common cause. Other causes are CNS tumors, head trauma, and other degenerative diseases that are common in the older age group, such as dementia.[30]
Metabolic
Structural
- cavernous malformationis a treatable medical condition that can cause seizures, headaches, and brain hemorrhages.
- Arteriovenous malformation (AVM) is a treatable medical condition that can cause seizures, headaches, and brain hemorrhages.
- Space-occupying lesions in the brain (brain tumours, the frequency of epilepsy depends on the location of the tumor in the cortical region.[32]
Medications
Both medication and
Infections
- Infection with the pork tapeworm, which can cause neurocysticercosis, is the cause of up to half of epilepsy cases in areas of the world where the parasite is common.[34]
- Parasitic infections such as cerebral malaria. In Nigeria this is one of the most common causes of seizures among children under five years of age.[35]
- Infection, such as encephalitis or meningitis[36]
Stress
Stress can induce seizures in people with epilepsy, and is a risk factor for developing epilepsy. Severity, duration, and time at which stress occurs during development all contribute to frequency and susceptibility to developing epilepsy. It is one of the most frequently self-reported triggers in patients with epilepsy.[37][38]
Stress exposure results in hormone release that mediates its effects in the brain. These hormones act on both excitatory and inhibitory neural synapses, resulting in hyper-excitability of neurons in the brain. The hippocampus is known to be a region that is highly sensitive to stress and prone to seizures. This is where mediators of stress interact with their target receptors to produce effects.[39]
Other
Seizures may occur as a result of
- Head injury may cause non-epileptic post-traumatic seizures or post-traumatic epilepsy
- About 3.5 to 5.5% of people with celiac disease also have seizures.[40]
- Seizures in a person with a shunt may indicate failure
- Hemorrhagic embolic strokes generally do not (though epilepsy is a common later complication); cerebral venous sinus thrombosis, a rare type of stroke, is more likely to be accompanied by seizures than other types of stroke
- Multiple sclerosis may cause seizures
- Electroconvulsive therapy (ECT) deliberately sets out to induce a seizure for the treatment of major depression.
- Reflex seizure induced by a specific stimulus or trigger (extrinsic or intrinsic stimuli)
- For people with photosensitive epilepsy, exposure to flashing lights or rapid blinking may cause a seizure.[41][42][43]
Mechanism
Normally, brain electrical activity is non-synchronous.[18] In epileptic seizures, due to problems within the brain,[44] a group of neurons begin firing in an abnormal, excessive,[15] and synchronized manner.[18] This results in a wave of depolarization known as a paroxysmal depolarizing shift.[45]
Normally after an
Focal seizures begin in one hemisphere of the brain while generalized seizures begin in both hemispheres.[20] Some types of seizures may change brain structure, while others appear to have little effect.[54] Gliosis, neuronal loss, and atrophy of specific areas of the brain are linked to epilepsy but it is unclear if epilepsy causes these changes or if these changes result in epilepsy.[54]
Seizure activity may be propagated through the brain's endogenous electrical fields.[55] Proposed mechanisms that may cause the spread and recruitment of neurons include an increase in K+ from outside the cell,[56][unreliable medical source] and increase of Ca2+ in the presynaptic terminals.[48] These mechanisms blunt hyperpolarization and depolarizes nearby neurons, as well as increasing neurotransmitter release.[48]
Diagnosis

Seizures may be divided into provoked and unprovoked.
Classification
Focal seizures (previously called partial seizures)
The classification of seizures can also be made according to dynamical criteria, observable in electrophysiological measurements. It is a classification according to their type of onset and offset.[59][60]
Physical examination
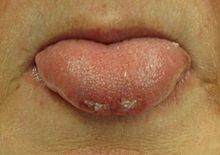
Most people are in a postictal state (drowsy or confused) following a seizure. They may show signs of other injuries. A bite mark on the side of the tongue helps confirm a seizure when present, but only a third of people who have had a seizure have such a bite.[61] When present in people thought to have had a seizure, this physical sign tentatively increases the likelihood that a seizure was the cause.[62]
Tests
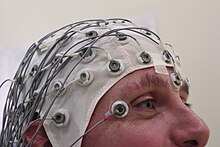
An electroencephalography is only recommended in those who likely had an epileptic seizure and may help determine the type of seizure or syndrome present. In children it is typically only needed after a second seizure. It cannot be used to rule out the diagnosis and may be falsely positive in those without the disease. In certain situations it may be useful to prefer the EEG while sleeping or sleep deprived.[63]
Diagnostic imaging by
In adults, testing electrolytes,
A high blood prolactin level within the first 20 minutes following a seizure may be useful to confirm an epileptic seizure as opposed to psychogenic non-epileptic seizure.[64][65] Serum prolactin level is less useful for detecting partial seizures.[66] If it is normal an epileptic seizure is still possible[65] and a serum prolactin does not separate epileptic seizures from syncope.[67] It is not recommended as a routine part of diagnosis epilepsy.[63]
Differential diagnosis
Differentiating an epileptic seizure from other conditions such as
Prevention
A number of measures have been attempted to prevent seizures in those at risk. Following traumatic brain injury anticonvulsants decrease the risk of early seizures but not late seizures.[69]
In those with a history of
There is no clear evidence that antiepileptic drugs are effective or not effective at preventing seizures following a
Management
Potentially sharp or dangerous objects should be moved from the area around a person experiencing a seizure so that the individual is not hurt. After the seizure, if the person is not fully conscious and alert, they should be placed in the recovery position. A seizure longer than five minutes, or two or more seizures occurring within the time of five minutes is a medical emergency known as status epilepticus.[22][76] Contrary to a common misconception, bystanders should not attempt to force objects into the mouth of the person having a seizure, as doing so may cause injury to the teeth and gums.[77]
Treatments of a person that is actively seizing follows a progression from initial response, through first line, second line, and third line treatments.[78] The initial response involves ensuring the person is protected from potential harms (such as nearby objects) and managing their airway, breathing, and circulation.[78] Airway management should include placing the person on their side, known as the recovery position, to prevent them from choking.[78] If they are unable to breathe because something is blocking their airway, they may require treatments to open their airway.[78]
Medication
The first line medication for an actively seizing person is a benzodiazepine, with most guidelines recommending lorazepam.[57][79] Diazepam and midazolam are alternatives. This may be repeated if there is no effect after 10 minutes.[57] If there is no effect after two doses, barbiturates or propofol may be used.[57]
Second-line therapy for adults is phenytoin or fosphenytoin and phenobarbital for children.[80][page needed] Third-line medications include phenytoin for children and phenobarbital for adults.[80][page needed]
Ongoing anti-epileptic medications are not typically recommended after a first seizure except in those with structural lesions in the brain.[57] They are generally recommended after a second one has occurred.[57] Approximately 70% of people can obtain full control with continuous use of medication.[44] Typically one type of anticonvulsant is preferred. Following a first seizure, while immediate treatment with an anti-seizure drug lowers the probability of seizure recurrence up to five years it does not change the risk of death and there are potential side effects.[81]
In seizures related to toxins, up to two doses of benzodiazepines should be used.[82] If this is not effective pyridoxine is recommended.[82] Phenytoin should generally not be used.[82]
There is a lack of evidence for preventive anti-epileptic medications in the management of seizures related to
Other
Helmets may be used to provide protection to the head during a seizure. Some claim that
Prognosis
Following a first seizure, the risk of more seizures in the next two years is around 40%.[12][13] The greatest predictors of more seizures are problems either on the electroencephalogram or on imaging of the brain.[7] In adults, after 6 months of being seizure-free after a first seizure, the risk of a subsequent seizure in the next year is less than 20% regardless of treatment.[87] Up to 7% of seizures that present to the emergency department (ER) are in status epilepticus.[57] In those with a status epilepticus, mortality is between 10% and 40%.[14] Those who have a seizure that is provoked (occurring close in time to an acute brain event or toxic exposure) have a low risk of re-occurrence, but have a higher risk of death compared to those with epilepsy.[88]
Epidemiology
Approximately 8–10% of people will experience an epileptic seizure during their lifetime.[89] In adults, the risk of seizure recurrence within the five years following a new-onset seizure is 35%; the risk rises to 75% in persons who have had a second seizure.[89] In children, the risk of seizure recurrence within the five years following a single unprovoked seizure is about 50%; the risk rises to about 80% after two unprovoked seizures.[90] In the United States in 2011, seizures resulted in an estimated 1.6 million emergency department visits; approximately 400,000 of these visits were for new-onset seizures.[89] The exact incidence of epileptic seizures in low-income and middle-income countries is unknown, however it probably exceeds that in high-income countries.[91] This may be due to increased risks of traffic accidents, birth injuries, and malaria and other parasitic infections.[91]
History
Epileptic seizures were first described in an Akkadian text from 2000 B.C.
Early surgical treatment of epilepsy was primitive in Ancient Greek, Roman and Egyptian medicine.[94] The 19th century saw the rise of targeted surgery for the treatment of epileptic seizures, beginning in 1886 with localized resections performed by Sir Victor Horsley, a neurosurgeon in London.[93] Another advancement was that of the development by the Montreal procedure by Canadian neurosurgeon Wilder Penfield, which involved use of electrical stimulation among conscious patients to more accurately identify and resect the epileptic areas in the brain.[93]
Society and culture
Economics
Seizures result in direct economic costs of about one billion dollars in the United States.[7] Epilepsy results in economic costs in Europe of around €15.5 billion in 2004.[15] In India, epilepsy is estimated to result in costs of US$1.7 billion or 0.5% of the GDP.[44] They make up about 1% of emergency department visits (2% for emergency departments for children) in the United States.[29]
Driving
Many areas of the world require a minimum of six months from the last seizure before people can drive a vehicle.[7]
Research
Scientific work into the prediction of epileptic seizures began in the 1970s. Several techniques and methods have been proposed, but evidence regarding their usefulness is still lacking.[95]
Two promising areas include
Gene therapy for epilepsy consists of employing vectors to deliver pieces of genetic material to areas of the brain involved in seizure onset.[96]
Seizure prediction is a special case of seizure detection in which the developed systems is able to issue a warning before the clinical onset of the epileptic seizure.[95][97]
Computational neuroscience has been able to bring a new point of view on the seizures by considering the dynamical aspects.[60]
References
- ISBN 9780199560042.
- ^ "Epileptic Seizures - National Library of Medicine". PubMed Health. Retrieved 16 October 2018.
- ^ ISBN 9780190259433.
- ^ Mayo Clinic Staff. "Seizures – Symptoms and causes". Mayo Clinic.
- ^ ISBN 9780323550765.
- ^ S2CID 35958237.
- ^ PMID 22963022.
- ^ a b c d "The Epilepsies and Seizures: Hope Through Research". National Institute of Neurological Disorders and Stroke. Retrieved 16 October 2018.
- ^ a b c "Epilepsy". World Health Organization. 9 February 2023. Retrieved 4 June 2023.
- ^ Schachter SC, Shafer PL, Sirven JI (5 November 2013). "What Is A Seizure Emergency". epilepsy.com.
- S2CID 31709502.
- ^ PMID 36688481.
- ^ S2CID 260965684.
- ^ a b c d e f Shearer P. "Seizures and Status Epilepticus: Diagnosis and Management in the Emergency Department". Emergency Medicine Practice. Archived from the original on 30 December 2010.
- ^ a b c d e National Institute for Health and Clinical Excellence (January 2012). "Chapter 1: Introduction" (PDF). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care. National Clinical Guideline Centre. pp. 21–28. Archived (PDF) from the original on 16 December 2013.
- ^ S2CID 22023692.
- PMID 10933986.
- ^ ISBN 978-0-07-162167-0.
- ^ ISBN 978-1-4377-0434-1.
- ^ a b c d e f g National Institute for Health and Clinical Excellence (January 2012). "Chapter 9: Classification of seizures and epilepsy syndromes" (PDF). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care. National Clinical Guideline Centre. pp. 119–129. Archived (PDF) from the original on 16 December 2013.
- ^ ISBN 978-0-07-175905-2.
- ^ S2CID 5294771.
- ISBN 978-0-7817-7397-3.
- ^ ISBN 978-1-84628-644-5.
- ISBN 978-1-60795-004-2.
- PMID 19605972.
- ^ S2CID 8505004.
- PMID 22335215.
- ^ PMID 21109099.
- ^ Harrison's Principles of Medicine. 15th edition
- ^ "diet and nutrition". 8 May 2013. Archived from the original on 29 June 2015.
- S2CID 12828909.
- S2CID 85563793.
- S2CID 21190601.
- ^ "Management of Convulsion in Children, a Health concern in Nigeria". Public Health Nigeria. October 2018. Archived from the original on 18 October 2018. Retrieved 18 October 2018.
- ISBN 978-0-205-23939-9.
- S2CID 36696690.
- S2CID 27433395.
- PMID 28916130.
- PMID 15825133.
- ^ "Photosensitive epilepsy | Epilepsy Society". epilepsysociety.org.uk. 23 February 2020. Retrieved 8 June 2023.
- ^ "Photosensitivity and Seizures". Epilepsy Foundation. Retrieved 8 June 2023.
- PMID 36467468.
- ^ a b c "Epilepsy". Fact Sheets. World Health Organization. October 2012. Archived from the original on 11 March 2016. Retrieved 24 January 2013.
- ISBN 978-0-19-803459-9.
- PMID 28488083.
- ^ Ropper A (2014). Adams and Victor's Principles of Neurology (10th ed., p. Chapter 16. Epilepsy and Other Seizure Disorders). New York: McGraw-Hill.
- ^ a b c d Lowenstein DH. Seizures and Epilepsy. In: Jameson J, Fauci AS, Kasper DL, Hauser SL, Longo DL, Loscalzo J. eds. (2018) Harrison's Principles of Internal Medicine, 20e New York, NY: McGraw-Hill.
- PMID 25370443.
- ^ PMID 23595016.
- S2CID 15074513.
- ^ PMID 25444846.
- PMID 26093166.
- ^ ISBN 978-0-7817-5777-5.
- PMID 26631463.
electric fields can be solely responsible for spike propagation at ... This phenomenon could be important to explain the slow propagation of epileptic activity and other normal propagations at similar speeds.
- )
- ^ a b c d e f g "Current Guidelines For Management of Seizures in the Emergency Department" (PDF). Archived from the original on 30 December 2010.
- ISBN 978-0-632-06046-7.
- PMID 32691734.
- ^ S2CID 235468072.
- PMID 25105200.
- PMID 22770819.
- ^ a b c d e f g National Institute for Health and Clinical Excellence (January 2012). "4" (PDF). The Epilepsies: The diagnosis and management of the epilepsies in adults and children in primary and secondary care. National Clinical Guideline Centre. pp. 57–83.
- S2CID 945952.
- ^ PMID 14988379.
- S2CID 2381873.
- PMID 16157897.
- PMID 12963568.
- PMID 32343399.
- PMID 34131913.
- PMID 32343399.
- PMID 23744552.
- PMID 35129214.
- ^ PMID 27098266.
- PMID 23740537.
- PMID 25257739.
- ^ O'connor A (22 April 2008). "The Claim: During a Seizure, You Can Swallow Your Tongue". The New York Times. Archived from the original on 6 March 2017.
- ^ PMID 26595862.
- S2CID 17641491.
- ^ a b Marx, J. A., Hockberger, R. S., Walls, R. M., Adams, J., & Rosen, P. (Eds.). (2013). Rosen's emergency medicine: concepts and clinical practice (8th ed). Philadelphia: Mosby/Elsevier.
- PMID 33942281.
- ^ PMID 21109109.
- ^ S2CID 33328776.
- PMID 24595491.
- PMID 25896576.
- PMID 32588435.
- PMID 21147743.
- PMID 8965090.
- ^ PMID 28027373.
- S2CID 20719640.
- ^ PMID 25231525.
- ^ S2CID 26340115.
- ^ PMID 26709155.
- ISSN 0896-6974.
- ^ S2CID 10109539.
- ^ S2CID 13942394.
- ^ PMID 17008335.
External links
- Seizure at Curlie
