Eumycetoma
| Eumycetoma | |
|---|---|
| Other names | Madura foot Curvularia lunata, Pseudallescheria spp., Neotestudina spp., Acremonium spp., Scedosporium spp. and Fusarium spp.
Surgical debridement, antifungal medicines[3] |
| Medication | Itraconazole, posaconazole, voriconazole[4] |
| Prognosis | Recurrence is common[5] |
| Frequency | Endemic in Africa, India and South America[3] |
Eumycetoma, also known as Madura foot,
Several fungi can cause eumycetoma,
Treatment includes
The infection occurs generally in the tropics,
Signs and symptoms

The initial lesion is a small swelling under the skin following minor trauma which breaches the skin.[11][12] It appears as a painless wet nodule, which may be present for years before ulceration, swelling and weeping from sinuses, followed by bone deformity.[3][7] The sinuses discharge a grainy liquid of fungal colonies.[11] These grains are usually black or white.[13] Destruction of deeper tissues, and deformity and loss of function in the affected limbs may occur in later stages.[14] It tends to occur in one foot.[13] Mycetoma due to bacteria has similar clinical features.[15]
Causes
Eumycetoma is a type of
The most common fungi causing white discharge is Scedosporium (ex. Pseudoalleschia) boydii.[13][16] Other causative agents of non-black grain eumycetoma include Acremonium and Fusarium species.[13]
Black discharge tends to be caused by species from the genera Madurella, Pyrenochaeta, Exophiala, Leptosphaeria and Curvularia.[13] The most common species are Madurella mycetomatis[13][17] and Trematospheria grisea (previously called Madurella grisea).[13][18]
Other fungal causative agents include:
- Acremonium falciform[5][19]
- Acremonium kiliense[5][19]
- Acremonium recifei[5][19]
- Aspergillus flavus[5][19]
- Aspergillus nidulans[5][19]
- Cladophialophora bantiana[5][19]
- Cladophialophora mycetomatis[5][19]
- Curvularia geniculata[5][19]
- Cylindrocarpon cyanescens[5][19]
- Exophiala jeanselmei[5][19]
- Falciformispora senegalensis[20]
- Fusarium solani[5][19]
- Glenospora clapieri[19]
- Leptosphaeria senegalensis[5][19][2]
- Leptosphaeria tompkinsii[5][19]
- Madurella grisea[5][19][2]
- Madurella mycetomatis[5][19][2]
- Microsporum audouinii[5][19]
- Microsporum canis[5][19]
- Neotestudina rosatii[5][19][2]
- Phaeoacremonium parasiticum[19]
- Phialophora cyanescens[19]
- Phialophora verrucosa[5][19]
- Scedosporium (ex. Pseudoalleschia) boydii[5][19][2]
- Pyrenochaeta mackinonii[5][19]
- Pyrenochaeta romeroi[5][19]
- Trichophyton rubrum[5][19]
- Zopfia rosatii[20]
Mechanism
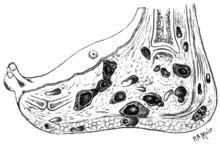
The disease is acquired by entry of the fungal spores from the soil through a breach in the skin produced by minor trauma like a thorn prick.[21] The disease then spreads to deeper tissues and also forms sinus tracts leading to skin surface.[12] Mature lesions are characterised by a grainy discharge from these sinuses. These discharges contain fungal colonies and are infective. Spread of infection internally through blood or lymph is uncommon.[citation needed]
Infections that produce a black discharge mainly spread subcutaneously. In the red and yellow varieties deep spread occurs early, infiltrating muscles and bones but sparing nerves and tendons, which are highly resistant to the invasion.[22]
Botryomycosis, also known as bacterial pseudomycosis, produces a similar clinical picture and is caused usually by Staphylococcus aureus.[23] Other bacteria may also cause botryomycosis.[24]
Diagnosis
Diagnosis is by

Differential diagnosis
The following clinical conditions may be considered before diagnosing a patient with mycetoma:[citation needed]
- Tuberculous ulcer
- Kaposi's sarcoma, a vascular tumour of skin usually seen in AIDS.
- Leprosy
- Syphilis
- Malignant neoplasm
- Tropical ulcer[22]
- Botryomycosis,[12] a skin infection usually caused by the bacteria Staphylococcus aureus.
Prevention
No vaccine is available. Simple hygienic precautions like wearing shoes or sandals while working in fields, and washing hands and feet at regular intervals may help prevent the disease.[citation needed]
Treatment
Surgery combined with itraconazole may be given for up to year when the grains are black.[4] Posaconazole is another option.[4] Voriconazole can be used for infections caused by Fusarium species.[4]
Ketoconazole has been used to treat eumycetoma but has many side effects.[25] Actinomycetes usually respond well to medical treatment, but eukaryotic infections are generally resistant and may require surgical interventions including salvage procedures as bone resection or even the more radical amputation.[26][12][14]
Oral fosravuconazole, which is much cheaper than itraconazole, an important factor as eumycetoma mainly affects young adults in poorer, rural areas, was found in 2023 in Phase II clinical trials to be safe, patient-friendly, and effective in treating eumycetoma.[27][28]
Epidemiology
The disease is more common in males aged 20–40 years who work as labourers, farmers and herders, and in travellers to tropical regions, where the condition is endemic.[4]
History
Madura foot or maduromycosis or maduramycosis[29] is described in ancient writings of India as Padavalmika, which, translated means Foot anthill.[12] The first modern description of Madura foot was made in 1842 from Madurai (the city after which the disease was named Madura-mycosis) in India, by Gill.[12] The fungal cause of the disease was established in 1860 by Carter.[12]
Society and culture
In 2016, the
References
- ^ ISBN 978-1-119-64706-5. Archivedfrom the original on 10 June 2021. Retrieved 9 June 2021.
- ^ a b c d e f g h i "ICD-11 – ICD-11 for Mortality and Morbidity Statistics". icd.who.int. Archived from the original on 1 August 2018. Retrieved 9 June 2021.
- ^ ISBN 978-0-7020-6830-0. Archivedfrom the original on 25 May 2021. Retrieved 13 June 2021.
- ^ from the original on 27 August 2021. Retrieved 30 August 2021.
- ^ PMID 22682186.
- ISBN 978-0-7020-7870-5. Archivedfrom the original on 13 June 2021. Retrieved 13 June 2021.
- ^ PMID 32970667.
- PMID 20734597.
- PMID 31918687.
- PMID 36084235.
- ^ ISBN 9780443101335.
- ^ ISBN 978-8125028086.
- ^ ISBN 978-3-030-35819-8. Archivedfrom the original on 11 June 2021. Retrieved 11 June 2021.
- ^ PMID 26483983.
- ^ a b "Mycetoma | DermNet NZ". dermnetnz.org. Archived from the original on 13 June 2021. Retrieved 11 June 2021.
- ^ "Filamentous Fungi". Archived from the original on 18 June 2012. Retrieved 23 July 2008.
- PMID 14662990.
- S2CID 35337823. [permanent dead link]
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa ab J. Alexandro Bonifaz Trujillo, Micología médica básica. México: McGraw Hill; 2010. ISBN 978-607-15-0744-0
- ^ ISBN 978-92-4-006024-1. Archivedfrom the original on 26 October 2022. Retrieved 27 October 2022.
- from the original on 7 July 2020. Retrieved 30 August 2021.
- ^ ISBN 0-7506-0625-8
- ^ "Dorlands Medical Dictionary:botryomycosis". 5 September 2008. Archived from the original on 5 September 2008. Retrieved 10 July 2018.
- ^ "Skin-nontumor Infectious disorders Botryomycosis". PathologyOutlines.com, Inc. Archived from the original on 24 July 2012. Retrieved 31 July 2013.
- PMID 17582190.
- PMID 28167862.
- ^ "World's first clinical trial for devastating fungal disease mycetoma shows efficacy of new, promising treatment" (Press release). Drugs for Neglected Diseases initiative (DNDi). 23 November 2023.
- ^ Johnson S (23 November 2023). "Cheap over-the-counter nail drug found to work on crippling flesh-eating disease". The Guardian.
The head of mycetoma at the DNDi labelled the discovery 'momentous', and said 'We were all very excited, it's going to be a gamechanger'.
- ^ "Infectious Disorders (Specific Agent) Madura foot/Mycetoma/Maduramycosis". MedTech USA, Inc. Archived from the original on 22 March 2014. Retrieved 1 August 2013.
