Fibromyalgia
| Fibromyalgia | |
|---|---|
| Other names | Fibromyalgia syndrome |
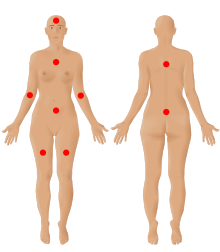 | |
| The nine possible pain sites of fibromyalgia according to the American Pain Society. | |
| Pronunciation | |
| Specialty | Rheumatology, neurology[2] |
| Symptoms | Widespread pain, feeling tired, sleep problems[3][4] |
| Usual onset | Early-Middle age[5] |
| Duration | Long term[3] |
| Causes | Unknown[4][5] |
| Diagnostic method | Based on symptoms after ruling out other potential causes[4][5] |
| Differential diagnosis | Anemia, autoimmune disorders (such as ankylosing spondylitis, polymyalgia rheumatica, rheumatoid arthritis, scleroderma, or multiple sclerosis), Lyme disease, osteoarthritis, thyroid disease[6][7] |
| Treatment | Sufficient sleep and exercise[5] |
| Medication | Duloxetine, milnacipran, pregabalin, gabapentin[5][8] |
| Prognosis | Normal life expectancy[5] |
| Frequency | 2%[4] |
Fibromyalgia is a medical condition which causes chronic widespread
The cause of fibromyalgia is unknown, but is believed to involve a combination of genetic and environmental factors.
The treatment of fibromyalgia is symptomatic
Fibromyalgia is estimated to affect 2–4% of the population.
Classification
Fibromyalgia is classed as a disorder of pain processing due to abnormalities in how pain signals are processed in the central nervous system.[23] The International Classification of Diseases (ICD-11) includes fibromyalgia in the category of "Chronic widespread pain," code MG30.01.[24]
Signs and symptoms
The defining symptoms of fibromyalgia are chronic widespread pain, fatigue, and sleep disturbance.[12] Other symptoms may include heightened pain in response to tactile pressure (allodynia),[12] cognitive problems,[12] musculoskeletal stiffness,[12] environmental sensitivity,[12] hypervigilance,[12] sexual dysfunction,[25] and visual symptoms.[26] Some people with fibromyalgia experience post-exertional malaise, in which symptoms flare up a day or longer after physical exercise.[27]
Pain
Fibromyalgia is predominantly a chronic pain disorder.[12] According to the NHS, widespread pain is one major symptom, which could feel like an ache, a burning sensation, or a sharp, stabbing pain.[28] Patients are also highly sensitive to pain, and the slightest touch can cause pain. Pain also tends to linger for longer when a patient experiences pain.[29]
Fatigue
Fatigue is one of the defining symptoms of fibromyalgia.[12] Patients may experience physical or mental fatigue. Physical fatigue can be demonstrated by a feeling of exhaustion after exercise or by a limitation in daily activities.[12]
Sleep problems
Sleep problems are a core symptom in fibromyalgia.
Cognitive problems
Many people with fibromyalgia experience
Hypersensitivity
In addition to a hypersensitivity to pain, patients with fibromyalgia show hypersensitivity to other stimuli,
Comorbidity
Fibromyalgia as a stand-alone diagnosis is uncommon, as most fibromyalgia patients often have other chronic overlapping pain problems or
Fibromyalgia and numerous chronic pain conditions frequently coexist.[39] These include chronic tension headaches,[37] myofascial pain syndrome,[37] and temporomandibular disorders.[37] Multiple sclerosis, post-polio syndrome, neuropathic pain, and Parkinson's disease are four neurological disorders that have been linked to pain or fibromyalgia.[39] Fibromyalgia largely overlaps with myalgic encephalomyelitis/chronic fatigue syndrome[43][44] and may share the same pathogenetic mechanisms.[44]
Comorbid fibromyalgia has been reported to occur in 20–30% of individuals with rheumatic diseases.[39] It has been reported in people with noninflammatory musculoskeletal diseases.[39]
The prevalence of fibromyalgia in gastrointestinal disease has been described mostly for celiac disease[39] and irritable bowel syndrome (IBS).[39][37] IBS and fibromyalgia share similar pathogenic mechanisms, involving immune system mast cells, inflammatory biomarkers, hormones, and neurotransmitters such as serotonin. Changes in the gut biome alter serotonin levels, leading to autonomic nervous system hyperstimulation.[45]
Fibromyalgia has also been linked with obesity.[46] Other conditions that are associated with fibromyalgia include connective tissue disorders,[47] cardiovascular autonomic abnormalities,[48] restless leg syndrome[49] and an overactive bladder.[50]
Risk factors
The cause of fibromyalgia is unknown. However, several risk factors, genetic and environmental, have been identified.
Genetics
Genetics play a major role in fibromyalgia, and may explain up to 50% of the disease susceptibility.[51] Fibromyalgia is potentially associated with polymorphisms of genes in the serotoninergic,[52] dopaminergic[52] and catecholaminergic systems.[52] Several genes have been suggested as candidates for susceptibility to fibromyalgia. These include SLC6A4,[51] TRPV2,[51] MYT1L,[51] NRXN3,[51] and the 5-HT2A receptor 102T/C polymorphism.[53] The heritability of fibromyalgia is estimated to be higher in patients younger than 50.[54]
Nearly all the genes suggested as potential risk factors for fibromyalgia are associated with neurotransmitters and their receptors.
Stress
Some authors have proposed that, because exposure to stressful conditions can alter the function of the
Personality
Although some have suggested that fibromyalgia patients are more likely to have specific personality traits, when depression is statistically controlled for, it appears that their personality is no different than that of people in the general population.[62]
Other risk markers
Other risk markers for fibromyalgia include premature birth, female sex, cognitive influences, primary pain disorders, multiregional pain, infectious illness, hypermobility of joints, iron deficiency and small-fiber polyneuropathy.[63] Metal-induced allergic inflammation has also been linked with fibromyalgia, especially in response to nickel but also inorganic mercury, cadmium, and lead.[64] Following the COVID-19 pandemic, some have suggested that the SARS-CoV-2 virus may trigger fibromyalgia.[65]
Pathophysiology
As of 2022, the pathophysiology of fibromyalgia has not yet been elucidated[66] and several theories have been suggested. The prevailing perspective considers fibromyalgia as a condition resulting from an amplification of pain by the central nervous system.[55] Substantial biological evidence backs up this notion, leading to the term of nociplastic pain.[55]
Nervous system
Pain processing abnormalities
Chronic pain can be divided into three categories. Nociceptive pain is pain caused by inflammation or damage to tissues. Neuropathic pain is pain caused by nerve damage. Nociplastic pain (or central sensitization) is less understood and is the common explanation of the pain experienced in fibromyalgia.[13][21][67] Because the three forms of pain can overlap, fibromyalgia patients may experience nociceptive (e.g., rheumatic illnesses) and neuropathic (e.g., small fiber neuropathy) pain, in addition to nociplastic pain.[21]
Nociplastic pain (central sensitization)
Fibromyalgia can be viewed as a condition of nociplastic pain.[68] Nociplastic pain is caused by an altered function of pain-related sensory pathways in the periphery and the central nervous system, resulting in hypersensitivity.[69]
Nociplastic pain is commonly referred to as "Nociplastic pain syndrome" because it is coupled with other symptoms.
Neuropathic pain
An alternative hypothesis to nociplastic pain views fibromyalgia as a stress-related dysautonomia with neuropathic pain features.[70] This view highlights the role of autonomic and peripheral nociceptive nervous systems in the generation of widespread pain, fatigue, and insomnia.[71] The description of small fiber neuropathy in a subgroup of fibromyalgia patients supports the disease neuropathic-autonomic underpinning.[70] However, others claim that small fiber neuropathy occurs only in small groups of those with fibromyalgia.[16]
Autonomic nervous system
Some suggest that fibromyalgia is caused or maintained by a decreased vagal tone, which is indicated by low levels of heart rate variability,[57] signaling a heightened sympathetic response.[72] Accordingly, several studies show that clinical improvement is associated with an increase in heart rate variability.[73][72][74] Some examples of interventions that increase the heart rate variability and vagal tone are meditation, yoga, mindfulness and exercise.[57] In 2023 the Fibromyalgia: Imbalance of Threat and Soothing Systems (FITSS) model was suggested as a working hypothesis.[75] According to the FITSS model, the salience network (also known as the midcingulo-insular network) may remain continuously hyperactive due to an imbalance in emotion regulation, which is reflected by an overactive "threat" system and an underactive "soothing" system. This hyperactivation, along with other mechanisms, may contribute to fibromyalgia.[75]
Neurotransmitters
Some neurochemical abnormalities that occur in fibromyalgia also regulate mood, sleep, and energy, thus explaining why mood, sleep, and fatigue problems are commonly co-morbid with fibromyalgia.[23] Serotonin is the most widely studied neurotransmitter in fibromyalgia. It is hypothesized that an imbalance in the serotoninergic system may lead to the development of fibromyalgia.[76] There is also some data that suggests altered dopaminergic and noradrenergic signaling in fibromyalgia.[77] Supporting the monoamine related theories is the efficacy of monoaminergic antidepressants in fibromyalgia.[17] Glutamate/creatine ratios within the bilateral ventrolateral prefrontal cortex were found to be significantly higher in fibromyalgia patients than in controls, and may disrupt glutamate neurotransmission.[59][78]
Neurophysiology
Neuroimaging studies have observed that fibromyalgia patients have increased grey matter in the right postcentral gyrus and left angular gyrus, and decreased grey matter in the right cingulate gyrus, right paracingulate gyrus, left cerebellum, and left gyrus rectus.[79] These regions are associated with affective and cognitive functions and with motor adaptations to pain processing.[79] Other studies have documented decreased grey matter of the default mode network in people with fibromyalgia.[80] These deficits are associated with pain processing.[80]
Neuroendocrine system
Studies on the neuroendocrine system and
One study found fibromyalgia patients exhibited higher plasma
Oxidative stress
Pro-oxidative processes correlate with pain in fibromyalgia patients.[81] Decreased mitochondrial membrane potential, increased superoxide activity, and increased lipid peroxidation production are observed.[81] The high proportion of lipids in the central nervous system (CNS) makes the CNS especially vulnerable to free radical damage. Levels of lipid peroxidation products correlate with fibromyalgia symptoms.[81]
Immune system
A repeated observation shows that autoimmunity triggers such as traumas and infections are among the most frequent events preceding the onset of fibromyalgia.[86] Neurogenic inflammation has been proposed as a contributing factor to fibromyalgia.[87]
Digestive system
Gut microbiome
Though there is a lack of evidence in this area, it is hypothesized that gut bacteria may play a role in fibromyalgia.[88] People with fibromyalgia are more likely to show dysbiosis, a decrease in microbiota diversity.[89] There is a bidirectional interplay between the gut and the nervous system. Therefore, the gut can affect the nervous system, but the nervous system can also affect the gut. Neurological effects mediated via the autonomic nervous system as well as the hypothalamic pituitary adrenal axis are directed to intestinal functional effector cells, which in turn are under the influence of the gut microbiota.[90]
Gut-brain axis
The gut-brain axis, which connects the gut microbiome to the brain via the enteric nervous system, is another area of research. Fibromyalgia patients have less varied gut flora and altered serum metabolome levels of glutamate and serine,[91] implying abnormalities in neurotransmitter metabolism.[86]
Energy metabolism
Low ATP in skeletal muscle
Patients with fibromyalgia experience exercise intolerance. Primary fibromyalgia is idiopathic (cause unknown), whereas secondary fibromyalgia is in association with a known underlying disorder (such as Ankylosing spondylitis).[92][non-primary source needed] In patients with primary fibromyalgia, studies have found disruptions in energy metabolism within skeletal muscle, including: decreased levels of ATP, ADP, and phosphocreatine, and increased levels of AMP and creatine (use of creatine kinase and myokinase in the phosphagen system due to low ATP);[93][non-primary source needed] increased pyruvate;[94][non-primary source needed] as well as reduced capillary density impairing oxygen delivery to the muscle cells for oxidative phosphorylation.[95][96][non-primary source needed]
Low ATP in brain
Despite being a small percentage of the body's total mass, the brain consumes approximately 20% of the energy produced by the body.
Low phosphocreatine levels may disrupt glutamate neurotransmission within the brains of those with fibromyalgia. Glutamate/creatine ratios within the bilateral ventrolateral prefrontal cortex were found to be significantly higher than in controls.[59][78][non-primary source needed]
Diagnosis

There is no single pathological feature, laboratory finding, or biomarker that can diagnose fibromyalgia and there is debate over what should be considered diagnostic criteria and whether an objective diagnosis is possible.[63] In most cases, people with fibromyalgia symptoms may have laboratory test results that appear normal and many of their symptoms may mimic those of other rheumatic conditions such as arthritis or osteoporosis. The specific diagnostic criteria for fibromyalgia have evolved over time.[97]
American College of Rheumatology 1990
The first widely accepted set of classification criteria for research purposes was elaborated in 1990 by the Multicenter Criteria Committee of the American College of Rheumatology. These criteria, which are known informally as "the ACR 1990", defined fibromyalgia according to the presence of the following criteria:
- A history of widespread pain lasting more than three months – affecting all four quadrants of the body, i.e., both sides, and above and below the waist.
- Tender points – there are 18 designated possible tender points (although a person with the disorder may feel pain in other areas as well).
The ACR criteria for the classification of patients were originally established as inclusion criteria for research purposes and were not intended for clinical diagnosis but have later become the de facto diagnostic criteria in the clinical setting. A controversial study was done by a legal team looking to prove their client's disability based primarily on tender points and their widespread presence in non-litigious communities prompted the lead author of the ACR criteria to question now the useful validity of tender points in diagnosis.[98] Use of control points has been used to cast doubt on whether a person has fibromyalgia, and to claim the person is malingering.[99]
American College of Rheumatology 2010 provisional criteria

In 2010, the American College of Rheumatology approved provisional revised diagnostic criteria for fibromyalgia that eliminated the 1990 criteria's reliance on tender point testing.[100] The revised criteria used a widespread pain index (WPI) and symptom severity scale (SSS) in place of tender point testing under the 1990 criteria. The WPI counts up to 19 general body areas[a] in which the person has experienced pain in the preceding week.[9] The SSS rates the severity of the person's fatigue, unrefreshed waking, cognitive symptoms, and general somatic symptoms,[b] each on a scale from 0 to 3, for a composite score ranging from 0 to 12.[9] The revised criteria for diagnosis were:
- WPI ≥ 7 and SSS ≥ 5 OR WPI 3–6 and SSS ≥ 9,
- Symptoms have been present at a similar level for at least three months, and
- No other diagnosable disorder otherwise explains the pain.[100]: 607
American College of Rheumatology 2016 revisions
In 2016, the provisional criteria of the American College of Rheumatology from 2010 were revised.[9] The new diagnosis required all of the following criteria:
- "Generalized pain, defined as pain in at least 4 of 5 regions, is present."
- "Symptoms have been present at a similar level for at least 3 months."
- "Widespread pain index (WPI) ≥ 7 and symptom severity scale (SSS) score ≥ 5 OR WPI of 4–6 and SSS score ≥ 9."
- "A diagnosis of fibromyalgia is valid irrespective of other diagnoses. A diagnosis of fibromyalgia does not exclude the presence of other clinically important illnesses."[9]
American Pain Society 2019

In 2019, the American Pain Society in collaboration with the U.S. Food and Drug Administration developed a new diagnostic system using two dimensions.[12] The first dimension included core diagnostic criteria and the second included common features. In accordance to the 2016 diagnosis guidelines, the presence of another medical condition or pain disorder does not rule out the diagnosis of fibromyalgia. Nonetheless, other conditions should be ruled out as the main explaining reason for the patient's symptoms. The core diagnostic criteria are:[101]
- Multisite pain defined as six or more pain sites from a total of nine possible sites (head, arms, chest, abdomen, upper back, lower back, and legs), for at least three months
- Moderate to severe sleep problems or fatigue, for at least three months
Common features found in fibromyalgia patients can assist the diagnosis process. These are tenderness (sensitivity to light pressure), dyscognition (difficulty to think), musculoskeletal stiffness, and environmental sensitivity or hypervigilance.[12]
Self-report questionnaires
Some research has suggested using a multidimensional approach taking into consideration somatic symptoms, psychological factors, psychosocial stressors and subjective belief regarding fibromyalgia.[102] These symptoms can be assessed by several self-report questionnaires.[9]
Widespread Pain Index (WPI)
The Widespread Pain Index (WPI) measures the number of painful body regions.[100]
Symptom Severity Scale (SSS)
The Symptom Severity Scale (SSS) assesses the severity of the fibromyalgia symptoms.
Fibromyalgia Impact Questionnaire (FIQ)
The Fibromyalgia Impact Questionnaire (FIQ)[103] and the Revised Fibromyalgia Impact Questionnaire (FIQR)[104] assess three domains: function, overall impact and symptoms.[104] It is considered a useful measure of disease impact.[105]
Other questionnaires
Other measures include the Hospital Anxiety and Depression Scale, Multiple Ability Self-Report Questionnaire,[106] Multidimensional Fatigue Inventory, and Medical Outcomes Study Sleep Scale.
Differential diagnosis
As of 2009, as many as two out of every three people who are told that they have fibromyalgia by a
The differential diagnosis is made during the evaluation on the basis of the person's medical history, physical examination, and laboratory investigations.[109][107][110][111] The patient's history can provide some hints to a fibromyalgia diagnosis. A family history of early chronic pain, a childhood history of pain, an emergence of broad pain following physical and/or psychosocial stress, a general hypersensitivity to touch, smell, noise, taste, hypervigilance, and various somatic symptoms (gastrointestinal, urology, gynecology, neurology), are all examples of these signals [11]
Extensive laboratory tests are usually unnecessary in the differential diagnosis of fibromyalgia.[12] Common tests that are conducted include complete blood count, comprehensive metabolic panel, erythrocyte sedimentation rate, C-reactive protein, and thyroid function test.[12]
Management
There is no universally accepted treatment or cure for fibromyalgia, and treatment typically consists of symptom management and improving patient quality of life.[14] A personalized, multidisciplinary approach to treatment that includes both non-pharmacologic and pharmacologic therapy and begins with effective patient education is most beneficial.[14] Developments in the understanding of the pathophysiology of the disorder have led to improvements in treatment, which include prescription medication, behavioral intervention, and exercise.
A number of associations have published guidelines for the diagnosis and management of fibromyalgia. The
The guidelines published by the
Exercise
Exercise is the only fibromyalgia treatment which has been given a strong recommendation by the European Alliance of Associations for Rheumatology (
Exercise may diminish fibromyalgia symptoms through a number of hypothesized biological mechanisms.[117] Exercise may improve pain modulation[118][119] through serotoninergic pathways.[119] It may reduce pain by altering the hypothalamic-pituitary-adrenal axis and reducing cortisol levels.[120] It also has anti-inflammatory effects that may improve fibromyalgia symptoms.[121][122] Aerobic exercise can improve muscle metabolism and pain through mitochondrial pathways.[121]
When comparing different exercise programs, aerobic exercise is capable of modulating the autonomic nervous function of fibromyalgia patients, whereas resistance exercise does not show such effects.[123] A 2022 meta-analysis found that aerobic training showed a high effect size while strength interventions showed moderate effects.[124] Meditative exercise seems preferable for improving sleep,[125][126] with no differences between resistance, flexibility and aquatic exercise in their favorable effects on fatigue.[125]
Despite its benefits, exercise is a challenge for patients with fibromyalgia, due to the chronic fatigue and pain they experience.[127] They perceive it as more effortful than healthy adults.[128] Exercise may intimidate them, in fear that they will be asked to do more than they are capable of.[129] They may also feel that those who recommend or deliver exercise interventions do not fully understand the possible negative impact of exercise on fatigue and pain.[129] This is especially true for non-personalized exercise programs.[129] Adherence is higher when the exercise program is recommended by doctors or supervised by nurses.[130] Depression and higher pain intensity serve as barriers to physical activity.[131] A recommended approach to a graded exercise program begins with small, frequent exercise periods and builds up from there.[124][132] In order to reduce pain, it is recommended to use an exercise program of 13 to 24 weeks, with each session lasting 30 to 60 minutes.[124]
Aerobic
Aerobic exercise for fibromyalgia patients is the most investigated type of exercise.[116] It includes activities such as walking, jogging, spinning, cycling, dancing and exercising in water,[121][123] with walking being named as one of the best methods.[133] A 2017 cochrane summary concluded that aerobic exercise probably improves quality of life, slightly decreases pain and improves physical function and makes no difference in fatigue and stiffness.[134] A 2019 meta-analysis showed that exercising aerobically can reduce autonomic dysfunction and increase heart rate variability.[123] This happens when patients exercise at least twice a week, for 45–60 minutes at about 60%-80% of the maximum heart rate.[123] Aerobic exercise also decreases anxiety and depression and improves the quality of life.[123]
Flexibility
Combinations of different exercises such as flexibility and aerobic training may improve stiffness.[135] However, the evidence is of low-quality.[135] It is not clear if flexibility training alone compared to aerobic training is effective at reducing symptoms or has any adverse effects.[136]
Resistance
In resistance exercise, participants apply a load to their body using weights, elastic band, body weight or other measures.
Two meta-analyses on fibromyalgia have shown that resistance training can reduce anxiety and depression,[123][137] one found that it decreases pain and disease severity[138] and one found that it improves quality of life.[123] Resistance training may also improve sleep, with a greater effect than that of flexibility training and a similar effect to that of aerobic exercise.[139]
The dosage of resistance exercise for women with fibromyalgia was studied in a 2022 meta-analysis.[140] Effective dosages were found when exercising twice a week, for at least eight weeks. Symptom improvement was found for even low dosages such as 1–2 sets of 4–20 repetitions.[140] Most studies use moderate exercise intensity of 40% to 85% one-repetition maximum. This level of intensity was effective in reducing pain.[140] Some treatment regimes increase the intensity over time (from 40% to 80%), whereas others increase it when the participant is able to perform 12 repetitions.[140] High-intensity exercises may cause lower treatment adherence.
Meditative
A 2021 meta-analysis found that meditative exercise programs (tai chi, yoga, qigong) were superior to other forms of exercise (aerobic, flexibility, resistance) in improving sleep quality.[125] Other meta-analyses also found positive effects of tai chi for sleep,[141] fibromyalgia symptoms,[142] and pain, fatigue, depression and quality of life.[143] These tai chi interventions frequently included 1-hour sessions practiced 1-3 times a week for 12 weeks. Meditative exercises, as a whole, may achieve desired outcomes through biological mechanisms such as antioxidation, anti-inflammation, reduction in sympathetic activity and modulation of glucocorticoid receptor sensitivity.[121]
Aquatic
Several reviews and meta-analyses suggest that aquatic training can improve symptoms and wellness in people with fibromyalgia.[144][145][146][147][148][149] It is recommended to practice aquatic therapy at least twice a week using a low to moderate intensity.[148] However, aquatic therapy does not appear to be superior to other types of exercise.[150]
Other
Limited evidence suggests
Medications
A few countries have published guidelines for the management and treatment of fibromyalgia. As of 2018, all of them emphasize that medications are not required. However, medications, though imperfect, continue to be a component of treatment strategy for fibromyalgia patients. The German guidelines outlined parameters for drug therapy termination and recommended considering drug holidays after six months.[16]
Health Canada and the US Food and Drug Administration (FDA) have approved pregabalin[152] (an anticonvulsant) and duloxetine (a serotonin–norepinephrine reuptake inhibitor) for the management of fibromyalgia. The FDA also approved milnacipran (another serotonin–norepinephrine reuptake inhibitor), but the European Medicines Agency refused marketing authority.[153]
Antidepressants
Antidepressants are one of the common drugs for fibromyalgia. A 2021 meta-analysis concluded that antidepressants can improve the quality of life for fibromyalgia patients in the medium-term.[17] For most people with fibromyalgia, the potential benefits of treatment with the serotonin and norepinephrine reuptake inhibitors duloxetine and milnacipran and the tricyclic antidepressants, such as amitriptyline, are outweighed by significant adverse effects (more adverse effects than benefits), however, a small number of people may experience relief from symptoms with these medications.[154][155][156]
The length of time that antidepressant medications take to be effective at reducing symptoms can vary. Any potential benefits from the antidepressant amitriptyline may take up to three months to take effect and it may take between three and six months for duloxetine, milnacipran, and pregabalin to be effective at improving symptoms.[157] Some medications have the potential to cause withdrawal symptoms when stopping so gradual discontinuation may be warranted particularly for antidepressants and pregabalin.[99]
Serotonin and norepinephrine reuptake inhibitors
A 2023 meta analysis found that duloxetine improved fibromyalgia symptoms, regardless of the dosage.[158] SSRIs may be also be used to treat depression in people diagnosed with fibromyalgia.[159]
Tricyclic antidepressants
While amitriptyline has been used as a first line treatment, the quality of evidence to support this use and comparison between different medications is poor.[160][156] Very weak evidence indicates that a very small number of people may benefit from treatment with the tetracyclic antidepressant mirtazapine, however, for most, the potential benefits are not great and the risk of adverse effects and potential harm outweighs any potential for benefit.[161] As of 2018, the only tricyclic antidepressant that has sufficient evidence is amitriptyline.[16][160]
Monoamine oxidase inhibitors
Tentative evidence suggests that monoamine oxidase inhibitors (MAOIs) such as pirlindole and moclobemide are moderately effective for reducing pain.[162] Very low-quality evidence suggests pirlindole as more effective at treating pain than moclobemide.[162] Side effects of MAOIs may include nausea and vomiting.[162]
Central nervous system depressants
Central nervous system depressants include drug categories such as sedatives, tranquilizers, and hypnotics. A 2021 meta-analysis concluded that such drugs can improve the quality of life for fibromyalgia patients in the medium-term.[17]
Anti-seizure medication
The anti-convulsant medications gabapentin and pregabalin may be used to reduce pain.[8] There is tentative evidence that gabapentin may be of benefit for pain in about 18% of people with fibromyalgia.[8] It is not possible to predict who will benefit, and a short trial may be recommended to test the effectiveness of this type of medication. Approximately 6/10 people who take gabapentin to treat pain related to fibromyalgia experience unpleasant side effects such as dizziness, abnormal walking, or swelling from fluid accumulation.[163] Pregabalin demonstrates a benefit in about 9% of people.[164] Pregabalin reduced time off work by 0.2 days per week.[165]
Cannabinoids
Cannabinoids may have some benefits for people with fibromyalgia. However, as of 2022, the data on the topic is still limited.[166][167][168] Cannabinoids may also have adverse effects and may negatively interact with common rheumatological drugs.[169]
Opioids
The use of opioids is controversial. As of 2015, no opioid is approved for use in this condition by the FDA.
A 2015 review found fair evidence to support tramadol use if other medications do not work.[170] A 2018 review found little evidence to support the combination of paracetamol (acetaminophen) and tramadol over a single medication.[172] Goldenberg et al suggest that tramadol works via its serotonin and norepinephrine reuptake inhibition, rather than via its action as a weak opioid receptor agonist.[173]
A large study of US people with fibromyalgia found that between 2005 and 2007 37.4% were prescribed short-acting opioids and 8.3% were prescribed long-acting opioids,[3] with around 10% of those prescribed short-acting opioids using tramadol;[174] and a 2011 Canadian study of 457 people with fibromyalgia found 32% used opioids and two-thirds of those used strong opioids.[114]
Topical treatment
Capsaicin has been suggested as a topical pain reliever. Preliminary results suggest that it may improve sleep quality and fatigue, but there are not enough studies to support this claim.[175]
Unapproved or unfounded
Sodium oxybate increases growth hormone production levels through increased slow-wave sleep patterns. However, this medication was not approved by the FDA for the indication for use in people with fibromyalgia due to the concern for abuse.[176]
The muscle relaxants cyclobenzaprine, carisoprodol with acetaminophen and caffeine, and tizanidine are sometimes used to treat fibromyalgia; however, as of 2015 they are not approved for this use in the United States.[177][178] The use of nonsteroidal anti-inflammatory drugs is not recommended as first-line therapy.[179] Moreover, nonsteroidal anti-inflammatory drugs cannot be considered as useful in the management of fibromyalgia.[180]
Very low-quality evidence suggests quetiapine may be effective in fibromyalgia.[181]
No high-quality evidence exists that suggests synthetic THC (nabilone) helps with fibromyalgia.[182]
Nutrition and dietary supplements
Nutrition is related to fibromyalgia in several ways. Some nutritional risk factors for fibromyalgia complications are obesity, nutritional deficiencies, food allergies and consuming food additives.[183] The consumption of fruits and vegetables, low-processed foods, high-quality proteins, and healthy fats may have some benefits.[183] Low-quality evidence found some benefits of a vegetarian or vegan diet.[184]
Although dietary supplements have been widely investigated in relation to fibromyalgia, most of the evidence, as of 2021, is of poor quality. It is therefore difficult to reach conclusive recommendations.[185] It appears that Q10 coenzyme and vitamin D supplements can reduce pain and improve quality of life for fibromyalgia patients.[20][186] Q10 coenzyme has beneficial effects on fatigue in fibromyalgia patients, with most studies using doses of 300 mg per day for three months.[187] Q10 coenzyme is hypothesized to improve mitochondrial activity and decrease inflammation.[188] Vitamin D has been shown to improve some fibromyalgia measures, but not others.[186][189]
Two review articles found that melatonin treatment has several positive effects on fibromyalgia patients, including the improvement of sleep quality, pain, and disease impact.[190][191] No major adverse events were reported.[190]
Psychotherapy
Due to the uncertainty about the pathogenesis of fibromyalgia, current treatment approaches focus on management of symptoms to improve quality of life,[192] using integrated pharmacological and non-pharmacological approaches.[4] There is no single intervention shown to be effective for all patients.[193] In a 2020 Cochrane review, cognitive behavioral therapy was found to have a small but beneficial effect for reducing pain and distress but adverse events were not well evaluated.[194] Cognitive behavioral therapy and related psychological and behavioural therapies have a small to moderate effect in reducing symptoms of fibromyalgia.[195][196] Effect sizes tend to be small when cognitive behavioral therapy is used as a stand-alone treatment for patients with fibromyalgia, but these improve significantly when it is part of a wider multidisciplinary treatment program.[196]
A 2010 systematic review of 14 studies reported that cognitive behavioral therapy improves self-efficacy or coping with pain and reduces the number of physician visits at post-treatment, but has no significant effect on pain, fatigue, sleep, or health-related quality of life at post-treatment or follow-up. Depressed mood was also improved but this could not be distinguished from some risks of bias.[197] A 2022 meta-analysis found that cognitive behavioral therapy reduces insomnia in people with chronic pain, including people with fibromyalgia.[198] Acceptance and commitment therapy, a type of cognitive behavioral therapy, has also proven effective.[199]
Patient education
Patient education is recommended by the
Sleep hygiene interventions show low effectiveness in improving insomnia in people with chronic pain.[198]
Manual therapy
A 2021 meta-analysis concluded that massage and myofascial release diminish pain in the medium-term.[17] As of 2015, there was no good evidence for the benefit of other mind-body therapies.[202]
Acupuncture
A 2013 review found moderate-level evidence on the usage of acupuncture with electrical stimulation for improvement of the overall well-being. Acupuncture alone will not have the same effects, but will enhance the influence of exercise and medication in pain and stiffness.[203]
Electrical neuromodulation
Several forms of electrical neuromodulation, including transcutaneous electrical nerve stimulation (TENS) and transcranial direct current stimulation (tDCS), have been used to treat fibromyalgia. In general, they have been found to be helpful in reducing pain and depression and improving functioning.[204][205]
Transcutaneous electrical nerve stimulation (TENS)
Transcutaneous electrical nerve stimulation (TENS) is the delivery of pulsed electrical currents to the skin to stimulate peripheral nerves. TENS is widely used to treat pain and is considered to be a low-cost, safe, and self-administered treatment.[206] As such, it is commonly recommended by clinicians to people suffering from pain.[207] On 2019, an overview of eight Cochrane reviews was conducted, covering 51 TENS-related randomized controlled trials.[207] The review concluded that the quality of the available evidence was insufficient to make any recommendations.[207] A later review concluded that transcutaneous electrical nerve stimulation may diminish pain in the short-term, but there was uncertainty about the relevance of the results.[17]
Preliminary findings suggest that electrically stimulating the vagus nerve through an implanted device can potentially reduce fibromyalgia symptoms.[208] However, there may be adverse reactions to the procedure.[208]
Noninvasive brain stimulation
Noninvasive brain stimulation includes methods such as transcranial direct current stimulation and high-frequency repetitive transcranial magnetic stimulation (TMS). Both methods have been found to improve pain scores in neuropathic pain and fibromyalgia.[209]
A 2023 meta analysis of 16 RCTs found that transcranial direct current stimulation (tDCS) of over 4 weeks can decrease pain in patients with fibromyalgia.[210]
A 2021 meta-analysis of multiple intervention types concluded that magnetic field therapy and transcranial magnetic stimulation may diminish pain in the short-term, but conveyed an uncertainty about the relevance of the result.[17] Several 2022 meta-analyses focusing on transcranial magnetic stimulation found positive effects on fibromyalgia.[211][212][213] Repetitive transcranial magnetic stimulation improved pain in the short-term[212][213] and quality of life after 5–12 weeks.[212][213] Repetitive transcranial magnetic stimulation did not improve anxiety, depression, and fatigue.[213] Transcranial magnetic stimulation to the left dorsolateral prefrontal cortex was also ineffective.[212]
EEG neurofeedback
A systematic review of EEG neurofeedback for treatment of fibromyalgia found most treatments showed significant improvements of the main symptoms of the disease.[214] However, the protocols were so different, and the lack of controls or randomization impede drawing conclusive results.[214]
Hyperbaric oxygen therapy
Hyperbaric oxygen therapy (HBOT) has shown beneficial effects in treating chronic pain by reducing inflammation and oxidative stress.[81] However, treating fibromyalgia with hyperbaric oxygen therapy is still controversial, in light of the scarcity of large-scale clinical trials.[121] In addition, hyperbaric oxygen therapy raises safety concerns due to the oxidative damage that may follow it.[121] An evaluation of nine trials with 288 patients in total found that HBOT was more effective at relieving fibromyalgia patients' pain than the control intervention. In most of the trials HBOT improved sleep disturbance, multidimensional function, patient satisfaction, and tender spots. 24% of the patients experienced negative outcomes.[215]
Prognosis
Although in itself fibromyalgia is neither degenerative nor fatal, the chronic pain of fibromyalgia is pervasive and persistent. Most people with fibromyalgia report that their symptoms do not improve over time. However, most patients learn to adapt to the symptoms over time. The German guidelines for patients explain that:
- The symptoms of fibromyalgia are persistent in nearly all patients.
- Total relief of symptoms is seldom achieved.
- The symptoms do not lead to disablement and do not shorten life expectancy.[113]
An 11-year
A study of 97 adolescents diagnosed with fibromyalgia followed them for eight years.[non-primary source needed] After eight years, the majority of youth still experienced pain and disability in physical, social, and psychological areas. At the last follow-up, all participants reported experiencing one or more fibromyalgia symptoms such as pain, fatigue, and/or sleep problems, with 58% matching the complete ACR 2010 criteria for fibromyalgia. Based on the WPI and SS score cut-points, the remaining 42% exhibited subclinical symptoms. Pain and emotional symptom trajectories, on the other hand, displayed a variety of longitudinal patterns. The study concluded that while most patient's fibromyalgia symptoms endure, the severity of their pain tends to reduce over time.[217]
Baseline depressive symptoms in adolescents appear to predict worse pain at follow-up periods.[218][219]
A meta-analysis based on close to 200,000 fibromyalgia patients found that they were at a higher risk for all-cause mortality. Specific mortality causes that were suggested were accidents, infections and suicide.[220]
Epidemiology
Fibromyalgia is estimated to affect 1.8% of the population.[221]
Despite the fact that more than 90% of fibromyalgia patients are women, only 60% of people with fibromyalgia symptoms are female in the general population.[222]
History
Chronic widespread pain had already been described in the literature in the 19th century but the term fibromyalgia was not used until 1976 when Dr P.K. Hench used it to describe these symptoms.[99] Many names, including "muscular rheumatism", "fibrositis", "psychogenic rheumatism", and "neurasthenia" were applied historically to symptoms resembling those of fibromyalgia.[223] The term fibromyalgia was coined by researcher Mohammed Yunus as a synonym for fibrositis and was first used in a scientific publication in 1981.[224] Fibromyalgia is from the Latin fibra (fiber)[225] and the Greek words myo (muscle)[226] and algos (pain).[227]
Historical perspectives on the development of the fibromyalgia concept note the "central importance" of a 1977 paper by Smythe and Moldofsky on fibrositis.[228][229] The first clinical, controlled study of the characteristics of fibromyalgia syndrome was published in 1981,[230] providing support for symptom associations. In 1984, an interconnection between fibromyalgia syndrome and other similar conditions was proposed,[231] and in 1986, trials of the first proposed medications for fibromyalgia were published.[231]
A 1987 article in the
Society and culture
Economics
People with fibromyalgia generally have higher healthcare costs and utilization rates. A review of 36 studies found that fibromyalgia causes a significant economic burden on health care systems.[234] Annual costs per patient were estimated to be up to $35,920 in the US and $8,504 in Europe.[234]
Controversies
Fibromyalgia was defined relatively recently. In the past, it was a disputed diagnosis. Frederick Wolfe, lead author of the 1990 paper that first defined the diagnostic guidelines for fibromyalgia, stated in 2008 that he believed it "clearly" not to be a disease but instead a physical response to depression and stress.[235] In 2013, Wolfe added that its causes "are controversial in a sense" and "there are many factors that produce these symptoms – some are psychological and some are physical and it does exist on a continuum".[236] Some members of the medical community do not consider fibromyalgia a disease because of a lack of abnormalities on physical examination and the absence of objective diagnostic tests.[228][237]
In the past, some psychiatrists have viewed fibromyalgia as a type of
As of 2022,
Notes
- ^ Shoulder girdle (left & right), upper arm (left & right), lower arm (left & right), hip/buttock/trochanter (left & right), upper leg (left & right), lower leg (left & right), jaw (left & right), chest, abdomen, back (upper & lower), and neck.[100]: 607
- ^ Somatic symptoms include, but are not limited to: muscle pain, irritable bowel syndrome, fatigue or tiredness, problems thinking or remembering, muscle weakness, headache, pain or cramps in the abdomen, numbness or tingling, dizziness, insomnia, depression, constipation, pain in the upper abdomen, nausea, nervousness, chest pain, blurred vision, fever, diarrhea, dry mouth, itching, wheezing, Raynaud's phenomenon, hives or welts, ringing in the ears, vomiting, heartburn, oral ulcers, loss of or changes in taste, seizures, dry eyes, shortness of breath, loss of appetite, rash, sun sensitivity, hearing difficulties, easy bruising, hair loss, frequent or painful urination, and bladder spasms.[100]: 607
References
- ^ "fibromyalgia". Collins Dictionaries. Archived from the original on 4 October 2015. Retrieved 16 March 2016.
- ^ "Neurology Now: Fibromyalgia: Is Fibromyalgia Real? | American Academy of Neurology". tools.aan.com. October 2009. Retrieved 1 June 2018.[permanent dead link]
- ^ S2CID 29000267.
- ^ S2CID 43693607.
- ^ a b c d e f g "Questions and Answers about Fibromyalgia". NIAMS. July 2014. Archived from the original on 15 March 2016. Retrieved 15 March 2016.
- ISBN 978-0-323-07699-9.
- PMID 16904498.
- ^ PMID 28045473.
- ^ PMID 27916278.
- ^ PMID 28545798.
- ^ PMID 30747096.
- ^ S2CID 53872511.
- ^ S2CID 235471910.
- ^ S2CID 73482737.
- ^ (PDF) from the original on 8 February 2023. Retrieved 4 March 2023.
- ^ PMID 29946212.
- ^ PMID 33104162.
- PMID 38355316.
- PMID 28536363.
- ^ .
- ^ S2CID 235245552.
- ISBN 978-0-8261-0938-5.
- ^ PMID 21878603.
- ^ "ICD-11 for Mortality and Morbidity Statistics". icd.who.int. Archived from the original on 1 August 2018. Retrieved 9 April 2022.
- S2CID 53717513.
- S2CID 219548664.
- ^ "Archived copy". academic.oup.com. Archived from the original on 21 May 2023. Retrieved 11 February 2024.
{{cite web}}: CS1 maint: archived copy as title (link) - ^ "Fibromyalgia – Symptoms". nhs.uk. 20 October 2017. Archived from the original on 23 March 2018. Retrieved 21 October 2020.
- ^ "Fibromyalgia - Symptoms". nhs.uk. 20 October 2017. Retrieved 11 April 2024.
- PMID 32876042.
- PMID 22094198.
- ^ PMID 19962493.
- PMID 35036191.
- ^ PMID 29388512.
- S2CID 231437516.
- S2CID 232066286.
- ^ S2CID 229948862.
- S2CID 254273680.
- ^ S2CID 44068037.
- PMID 35698706.
- S2CID 73411416.
- ^ Bruce DF, PhD. "Fibromyalgia and Depression". WebMD. Retrieved 1 April 2024.
- S2CID 219104988.
- ^ PMID 35690247.
- PMID 36381861.
- S2CID 232136088.
- (PDF) from the original on 7 January 2024. Retrieved 7 January 2024.
- S2CID 252496799.
- from the original on 28 July 2023. Retrieved 28 July 2023.
- S2CID 249236213.
- ^ PMID 30486733.
- ^ PMID 26266996.
- S2CID 6239018.
- PMID 31736264.
- ^ S2CID 258745974.
- PMID 19482616.
- ^ S2CID 239772451.
- ^ S2CID 231955641.
- ^ PMID 33940974.
- S2CID 20678671.
- from the original on 9 April 2022. Retrieved 9 April 2022.
- PMID 30294356.
- ^ PMID 31191788.
- S2CID 251623384.
- PMID 36849853.
- S2CID 245909381.
- S2CID 58565532.
- S2CID 249650477.
- PMID 34361986.
- ^ S2CID 52306843.
- PMID 33409721.
- ^ S2CID 237375381.
- S2CID 40592827.
- PMID 32045515.
- ^ S2CID 254273384.
- ^ S2CID 123945497.
- ^ PMID 23213512.
- ^ PMID 21799042.
- ^ PMID 37229427.
- ^ PMID 28105430.
- ^ PMID 36246401.
- S2CID 131775636.
- ^ PMID 22034969.
- ^ PMID 24462815.
- PMID 25786052.
- ^ PMID 32116216.
- S2CID 4368913.
- PMID 32192466.
- PMID 35594658.
- PMID 32116215.
- PMID 31327695.
- S2CID 30837539.
- PMID 3741498.
- PMID 33142767.
- PMID 23124535.
- PMID 23116302.
- PMID 29946212.
- from the original on 14 October 2011.
- ^ PMID 19623319.
- ^ S2CID 17154205.
- PMID 32340369.
- S2CID 2412984.
- from the original on 16 May 2022. Retrieved 18 June 2022.
- ^ PMID 19664287.
- ^ "Fibromyalgia Impact Questionnaire (FIQ)". American College of Rheumatology. Archived from the original on 1 July 2022. Retrieved 18 June 2022.
- PMID 8150893.
- ^ PMID 19962492.
- ^ PMID 29392213.
- ^ PMID 25786053.
- ^ S2CID 205309871.
- ^ PMID 26819509.
- ^ S2CID 1348989. Archived from the original(PDF) on 16 February 2013.
- ^ PMID 24379886.
- ^ a b c "Management | Canadian Guidelines for the Diagnosis and Management of Fibromyalgia". Archived from the original on 11 June 2013.
- PMID 17943797.
- ^ S2CID 212638860.
- PMID 33962033.
- PMID 21330218.
- ^ PMID 24477734.
- PMID 26311959.
- ^ S2CID 53240356.
- S2CID 46879701.
- ^ S2CID 85448644.
- ^ S2CID 248970279.
- ^ S2CID 220847961.
- S2CID 258597720.
- PMID 20217670.
- S2CID 219918068.
- ^ S2CID 3395036.
- S2CID 9032840.
- S2CID 253627372.
- PMID 24279570.
- S2CID 256696861.
- PMID 28636204.
- ^ PMID 31124142.
- PMID 31476271.
- S2CID 234489153.
- S2CID 259949000.
- from the original on 28 July 2023. Retrieved 28 July 2023.
- ^ S2CID 238991065.
- S2CID 219743962.
- S2CID 250317143.
- S2CID 199039433.
- PMID 25350761.
- S2CID 25701866.
- PMID 21197303.
- S2CID 222167851.
- ^ S2CID 255217819.
- S2CID 252079586.
- S2CID 259580881.
- PMID 28950401.
- ^ "FDA Approves First Drug for Treating Fibromyalgia" (Press release). U.S. Food and Drug Administration. 21 June 2007. Archived from the original on 21 February 2008. Retrieved 14 January 2008.
- ^ European Medicines Agency. "Questions and answers on the recommendati on for the refusal of the marketing authorisation for Milnacipran Pierre Fabre Médicament/Impulsor" (PDF). European Medicines Agency. Archived (PDF) from the original on 22 February 2014. Retrieved 30 May 2013.
- S2CID 207301478.
- PMID 26482422.
- ^ PMID 29489029.
- PMID 35658166.
- PMID 37461044.
- PMID 26046493.
- ^ PMID 26146793.
- PMID 30080242.
- ^ PMID 22513976.
- PMID 28597471.
- PMID 27684492.
- PMID 21639874.
- S2CID 248423563.
- PMID 35503198.
- S2CID 248973512.
- PMID 35476898.
- ^ S2CID 26613022.
- PMID 27582266.
- PMID 29457627.
- S2CID 20228209.
- ^ Berger A. Patterns of use of opioids in patients with fibromyalgia In: EULAR; 2009:SAT0461
- S2CID 248389141.
- S2CID 33026097.
- from the original on 1 April 2016.
- from the original on 6 August 2020. Retrieved 20 February 2017.
- PMID 21125141.
- PMID 28349517.
- PMID 27251337.
- PMID 27428009.
- ^ PMID 35674686.
- PMID 34066603.
- PMID 33909266.
- ^ S2CID 248948241.
- S2CID 86467031.
- (PDF) from the original on 30 May 2023. Retrieved 17 May 2023.
- S2CID 255471623.
- ^ S2CID 208497324.
- from the original on 5 January 2024. Retrieved 28 July 2023.
- PMID 26817567.
- PMID 25135147.
- PMID 32794606.
- PMID 24018611.
- ^ S2CID 10513179.
- S2CID 11357808.
- ^ PMID 35546397.
- ISSN 2049-4637.
- PMID 35587171.
- from the original on 28 July 2023. Retrieved 28 July 2023.
- PMID 25856658.
- PMID 23728665.
- S2CID 256461558.
- from the original on 28 July 2023. Retrieved 28 July 2023.
- PMID 28990665.
- ^ PMID 30941745.
- ^ PMID 21812908.
- S2CID 248715312.
- S2CID 253933442.
- S2CID 249208885.
- ^ PMID 34983056.
- ^ PMID 34542624.
- ^ PMID 37179502.
- PMID 36690401.
- ^ S2CID 207672626.
- PMID 30335681.
- S2CID 22164186.
- S2CID 25457728.
- S2CID 259502501.
- S2CID 5043754.
- PMID 30212526.
- ^ Health Information Team (February 2004). "Fibromyalgia". BUPA insurance. Archived from the original on 22 June 2006. Retrieved 24 August 2006.
- PMID 6944796.
- ^ "Fibro-". Dictionary.com. Archived from the original on 13 December 2009. Retrieved 21 May 2008.
- ^ "Meaning of myo". 12 April 2009. Archived from the original on 12 April 2009. Retrieved 26 August 2012.
- ^ "Meaning of algos". 12 April 2009. Archived from the original on 12 April 2009. Retrieved 26 August 2012.
- ^ S2CID 2091976.
- PMID 199304.
- PMID 17303220.
- ^ S2CID 42573740.
- PMID 3553636.
- PMID 2306288.
- ^ S2CID 250271053.
- ^ Berenson A (14 January 2008). "Drug Approved. Is Disease Real?". The New York Times. Archived from the original on 10 May 2015. Retrieved 26 March 2014.
- ^ "Fibromyalgia: An interview with Dr Frederick Wolfe, University of Kansas School of Medicine". 22 March 2013. Archived from the original on 29 May 2014. Retrieved 28 May 2014.
- PMID 7880118.
- PMID 29076404.
- PMID 17350675.
