Gastric varices
| Gastric varices | |
|---|---|
gastroscopy in a patient with portal hypertension | |
| Specialty | Gastroenterology Hematology |
| Symptoms | vomiting blood passing black stool |
| Complications | Internal bleeding, hypovolemic shock, cardiac arrest |
Gastric varices are dilated submucosal
Patients with bleeding gastric varices can present with bloody vomiting (hematemesis), dark, tarry stools (melena), or rectal bleeding. The bleeding may be brisk, and patients may soon develop shock. Treatment of gastric varices can include injection of the varices with cyanoacrylate glue, or a radiological procedure to decrease the pressure in the portal vein, termed transjugular intrahepatic portosystemic shunt or TIPS. Treatment with intravenous octreotide is also useful to shunt blood flow away from the stomach's circulation. More aggressive treatment, including splenectomy (surgical removal of the spleen) or liver transplantation, may be required in some cases.
Signs and symptoms

Gastric varices can present in two major ways. First, patients with
Secondly, patients with
Laboratory testing usually shows low red blood cell count and often a low platelet count. If cirrhosis is present, there may be coagulopathy manifested by a prolonged INR; both of these may worsen the bleeding from gastric varices.[2]
In rare cases, gastric varices are caused by splenic vein occlusion as a result of the mass effect of slow-growing pancreatic neuroendocrine tumors.[citation needed]
Diagnosis
The diagnosis of gastric varices is often made at the time of upper endoscopy.[1]
Classification

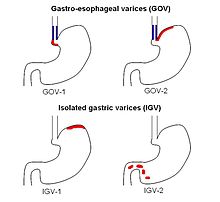
The Sarin classification of gastric varices identifies four different anatomical types of gastric varices, which differ in terms of treatment modalities:[1]
- Type 1 Gastroesophageal Varices: Esophagus extending to lesser curvature of stomach
- Type 2 Gastroesophageal Varices: Esophagus extending to greater curvature of stomach
- Type 1 Gastric Varices: Isolated to the fundus
- Type 2 Gastric Varices: Anywhere in the stomach, or duodenum
Type 1 isolated gastric varices were seen only in primary cases (i.e. without prior sclerotherapy) in the original study of Sarin et al. (1992), while type 1 gastroesophageal varices were the most common overall.[3]
Other classification systems include Hashizume's classification and Arakawa's classification.[1]
Treatment
Initial treatment of bleeding from gastric varices focuses on resuscitation, much as with esophageal varices. This includes administration of fluids, blood products, and antibiotics.[4][5]
Another treatment for gastric varices is injection of the varices with cyanoacrylate, first described by German surgeon Nib Soehendra and colleagues in 1986.[6] The results from two randomized trials comparing band ligation vs cyanoacrylate suggests that endoscopic injection of cyanoacrylate, known as gastric variceal obliteration or GVO is superior to band ligation in preventing rebleeding rates. Cyanoacrylate, a common component in 'super glue' is often mixed 1:1 with lipiodol to prevent polymerization in the endoscopy delivery optics, and to show on radiographic imaging. GVO is usually performed in specialized therapeutic endoscopy centers. Complications include sepsis, embolization of glue, and obstruction from polymerization in the lumen of the stomach.[citation needed]
Other techniques for refractory bleeding include:[5]
- Transjugular intrahepatic portosystemic shunts(TIPS)
- Balloon occluded retrograde transvenous obliteration techniques (BRTO)
- Coil-assisted retrograde transvenous obliteration (CARTO)
- Gastric variceal ligation, although this modality is falling out of favour[citation needed]
- Intra-gastric balloon tamponade as a bridge to further therapy
- a caveat is that a larger balloon is required to occupy the fundusof the stomach where gastric varices commonly occur
- a caveat is that a larger balloon is required to occupy the
- Liver transplantation
See also
References
- ^ PMID 26958057.
- ^ "Cirrhosis". The Lecturio Medical Concept Library. 28 September 2020. Retrieved 9 July 2021.
- PMID 1446890.
- PMID 31277322.
- ^ S2CID 93000660.
- PMID 3512261.)
{{cite journal}}: CS1 maint: multiple names: authors list (link
