Glossitis
| Glossitis [1] | |
|---|---|
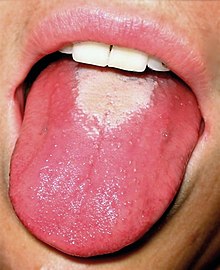 | |
| Glossitis in a person with scarlet fever ("red strawberry tongue"). | |
| Specialty | Gastroenterology |
Glossitis can mean soreness of the tongue, or more usually inflammation with depapillation of the dorsal surface of the tongue (loss of the
Symptoms
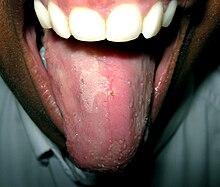
Depending upon what exact meaning of the word glossitis is implied, signs and symptoms might include:
- Smooth, shiny appearance of the tongue, caused by loss of lingual papillae.
- Tongue color changes, usually to a darker red color than the normal white-pink color of a healthy tongue.
- Tongue swelling.
- Difficulty with chewing, swallowing, or speaking (either because of tongue soreness or tongue swelling).
- Burning sensation.[2] Some use the term secondary burning mouth syndrome in cases where a detectable cause, such as glossitis, for an oral burning sensation.[5]
Depending upon the underlying cause, there may be additional signs and symptoms such as pallor, oral ulceration and angular cheilitis.[2]
Causes
Anemias
Pernicious anemia is usually caused by autoimmune destruction of gastric parietal cells. Parietal cells secrete intrinsic factor which is required for the absorption of vitamin B12. Vitamin B12 deficiency results in megaloblastic anemia and may present as glossitis. The appearance of the tongue in vitamin B12 deficiency is described as "beefy" or "fiery red and sore".[6] There may be linear or patchy red lesions.[2]
Vitamin B deficiencies
Infections
Syphilis is now relatively rare, but the tertiary stage can cause diffuse glossitis and atrophy of lingual papillae, termed "syphilitic glossitis",[2] "luetic glossitis" or "atrophic glossitis of tertiary syphilis".[8] It is caused by Treponema pallidum and is a sexually transmitted infection.
Other causes
Many conditions can cause glossitis via malnutrition or malabsorption,[7] which creates the nutritional deficiencies described above, although other mechanisms may be involved in some of those conditions listed.
- Alcoholism[7]
- Crohn's disease[7]
- Whipple disease[7]
- Glucagonoma syndrome[7]
- Cowden disease[7]
- Acquired immunodeficiency syndrome (AIDS)[7]
- Carcinoid syndrome[7]
- Kwashiorkor amyloidosis[7]
- Veganism and other specialized diets, without B12 supplementation.[2]
- Poor hydration and low saliva in the mouth, which allows bacteria to grow more readily
- Mechanical irritation or injury from burns, rough edges of teeth or dental appliances, or other trauma
- Tongue piercing[12] Glossitis can be caused by the constant irritation by the ornament and by colonization of Candida albicans in site and on the ornament[13]
- Exposure to irritants such as tobacco, alcohol, hot foods, or spices
- Allergic reaction to ACE inhibitors)
- Administration of Tubocurarine, Mecamylamine).
- Oral aphthous ulcer, pemphigusvulgaris
- Heredity
- Albuterol(bronchodilator medicine)
A painful tongue may be an indication of an underlying serious medical condition and nearly always merits assessment by a physician or dental surgeon.
Diagnosis
Classification
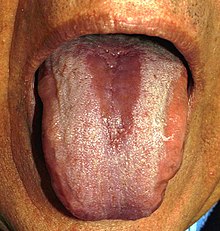
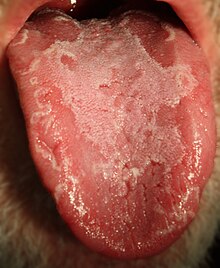
Glossitis could be classified as a group of tongue diseases or gastrointestinal diseases.[4] It may be primary, where there is no underlying cause, or secondary where it is a sign or symptom of another condition.[3] It can be acute or chronic.[4] Generally speaking, there are several clinical patterns of glossitis, some more common than others.
Atrophic glossitis
Atrophic glossitis, also known as bald tongue,
Candidiasis may be a concurrent finding or an alternative cause of erythema, burning, and atrophy.
Median rhomboid glossitis
This condition is characterized by a persistent erythematous, rhomboidal depapillated lesion in the central area of the dorsum of the tongue, just in front of the
Benign migratory glossitis
Geographic tongue, also termed benign migratory glossitis, is a common condition which usually affects the dorsal surface of the tongue. It is characterized by patches of depapillation and erythema bordered by a whitish peripheral zone. These patches give the tongue the appearance of a map, hence the name. Unlike glossitis due to nutritional deficiencies and anemia, the lesions of geographic tongue move around the tongue over time.[20] This is because in geographic tongue, new areas of the tongue become involved with the condition whilst previously affected areas heal, giving the appearance of a moving lesion.[3] The cause is unknown,[21] and there is no curative treatment. Rarely are there any symptoms associated with the lesions, but occasionally a burning sensation may be present, which is exacerbated by eating hot, spicy or acidic foodstuffs. Some consider geographic tongue to be an early stage of fissured tongue, since the two conditions often occur in combination.[22]
Geometric glossitis
Geometric glossitis, also termed herpetic geometric glossitis,[4] is a term used by some to refer to a chronic lesion associated with herpes simplex virus (HSV) type I infection,[23] in which there is a deep fissure in the midline of the tongue, which gives off multiple branches.[8] The lesion is usually very painful, and there may be erosions present in the depths of the fissures. Similar fissured lesions which are not associated with HSV, as may occur in fissured tongue, do not tend to be painful.[23] The name comes from the geometric pattern of the fissures which are longitudinal, crossed or branched.[24] It is described as occurring in immunocompromized persons, e.g. who have leukemia. However, the association between herpes simplex and geometric glossitis is disputed by some due to a lack of gold standard techniques for diagnosis of intraoral herpetic lesions, and the high prevalence of asymptomatic viral shedding in immunocompromized individuals.[8] Treatment is with systemic aciclovir.[23]
Strawberry tongue

Strawberry tongue, or raspberry tongue,
Treatment
The goal of treatment is to reduce inflammation. Treatment usually does not require hospitalization unless tongue swelling is severe. Good oral hygiene is necessary, including thorough tooth brushing at least twice a day, and flossing at least daily. Corticosteroids such as prednisone may be given to reduce the inflammation of glossitis. For mild cases, topical applications (such as a prednisone mouth rinse that is not swallowed) may be recommended to avoid the side effects of swallowed or injected corticosteroids. Antibiotics, antifungal medications, or other antimicrobials may be prescribed if the cause of glossitis is an infection. Anemia and nutritional deficiencies (such as a deficiency in niacin, riboflavin, iron, or Vitamin E) must be treated, often by dietary changes or other supplements. Avoiding irritants (such as hot or spicy foods, alcohol, and tobacco) may minimize the discomfort. In some cases, tongue swelling may threaten the airway, a medical emergency that needs immediate attention.
Epidemiology
One review reported overall prevalence ranges of 0.1–14.3% for geographic tongue, 1.3–9.0% for "atrophy tongue" (atrophic glossitis), and 0.0–3.35% for median rhomboid glossitis.[31]
References
- ^ "Glossitis: MedlinePlus Medical Encyclopedia". medlineplus.gov. Retrieved 26 April 2019.
- ^ ISBN 978-0443068188.
- ^ ISBN 978-1615301317.
- ^ ISBN 978-1451103038.
- ^ PMID 27855478.
- ^ ISBN 978-1-60327-519-4.
- ^ ISBN 978-1-4051-6911-0.
- ^ ISBN 0721690033.
- PMID 21877503. Archived from the original(PDF) on 2014-04-19.
- PMID 26733948.
- S2CID 205776755.
- PMID 17993034.
- PMID 19732353.
- ^ ISBN 3540594523.
- ^ ISBN 0721629210.
- ^ PMID 21121523.
- PMID 21507289.
- ^ "Dental Enamel Defects and Celiac Disease" (PDF). National Institute of Health (NIH). Archived from the original (PDF) on March 5, 2016. Retrieved Mar 7, 2016.
Tooth defects that result from celiac disease may resemble those caused by too much fluoride or a maternal or early childhood illness. Dentists mostly say it's from fluoride, that the mother took tetracycline, or that there was an illness early on
- PMID 20212408.
There are enough evidence making the correlation between CD and oral defects scientifically sustainable. This recognition should lead dentists to play more significant roles in screening for CD, as otherwise, if not properly diagnosed and not treated with a gluten-free diet, may eventually cause some malignancies.
- PMID 22048588.
- PMID 20187599.
- ISBN 978-1550093452.
- ^ PMID 7502116.
- PMID 8247038.
- ISBN 978-0323025102.
- PMID 17719644.
- PMID 15835487.
- PMID 9184977.
- PMID 7106318.
- ^ Gary Williams; Murray Katcher. "Skin Lesions: Strawberry Tongue". Primary Care Dermatology Module (University of Wisconsin Madison). Retrieved 2007-08-14.
- PMID 1291323.
