Gonorrhea
| Gonorrhea | |
|---|---|
| Other names | Gonorrhoea, gonococcal infection, gonococcal urethritis, the clap |
Infectious disease | |
| Symptoms | None, burning with urination, vaginal discharge, discharge from the penis, pelvic pain, testicular pain[1] |
| Complications | Pelvic inflammatory disease, inflammation of the epididymis, septic arthritis, endocarditis[1][2] |
| Causes | Neisseria gonorrhoeae typically sexually transmitted[1] |
| Diagnostic method | Testing the urine, urethra in males, or cervix in females[1] |
| Prevention | Condoms, having sex with only one person who is uninfected, not having sex[1][3] |
| Treatment | Ceftriaxone by injection and azithromycin by mouth[4][5] |
| Frequency | 0.8% (women), 0.6% (men)[6] |
Gonorrhoea or gonorrhea, colloquially known as the clap, is a
Gonorrhea is spread through sexual contact with an infected person.[1] This includes oral, anal, and vaginal sex.[1] It can also spread from a mother to a child during birth.[1] Diagnosis is by testing the urine, urethra in males, or cervix in females.[1] Testing all women who are sexually active and less than 25 years of age each year as well as those with new sexual partners is recommended;[3] the same recommendation applies in men who have sex with men (MSM).[3]
Gonorrhea can be prevented with the use of
Gonorrhea affects about 0.8% of women and 0.6% of men.[6] An estimated 33 to 106 million new cases occur each year, out of the 498 million new cases of curable STI – which also includes syphilis, chlamydia, and trichomoniasis.[8][9] Infections in women most commonly occur when they are young adults.[3] In 2015, it caused about 700 deaths.[10] Descriptions of the disease date back to before the Common Era within the Hebrew Bible/Old Testament (Leviticus 15:2–3).[2] The current name was first used by the Greek physician Galen before AD 200 who referred to it as "an unwanted discharge of semen".[2]
Signs and symptoms
Gonorrhea infections of
Women
Half of women with gonorrhea are
Men
Most infected men with symptoms have inflammation of the penile urethra associated with a burning sensation during urination and discharge from the penis.[17] In men, discharge with or without burning occurs in half of all cases and is the most common symptom of the infection.[20] This pain is caused by a narrowing and stiffening of the urethral lumen.[21] The most common medical complication of gonorrhea in men is inflammation of the epididymis.[19] Gonorrhea is also associated with increased risk of prostate cancer.[22]
Infants
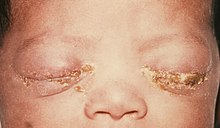
If not treated, gonococcal ophthalmia neonatorum will develop in 28% of infants born to women with gonorrhea.[23]
Spread
If left untreated, gonorrhea can spread from the original site of infection and infect and damage the joints, skin, and other organs. Indications of this can include fever, skin rashes, sores, and joint pain and swelling.
Cause


Gonorrhea is caused by the bacterium Neisseria gonorrhoeae.[17] Previous infection does not confer immunity – a person who has been infected can become infected again by exposure to someone who is infected. Infected persons may be able to infect others repeatedly without having any signs or symptoms of their own.[25]
Spread
The infection is usually spread from one person to another through vaginal, oral, or anal sex.[17][26] Men have a 20% risk of getting the infection from a single act of vaginal intercourse with an infected woman. The risk for men who have sex with men (MSM) is higher.[27] Insertive MSM may get a penile infection from anal intercourse, while receptive MSM may get anorectal gonorrhea. Women have a 60–80% risk of getting the infection from a single act of vaginal intercourse with an infected man.[28]
A mother may transmit gonorrhea to her newborn during childbirth; when affecting the infant's eyes, it is referred to as
Risk factors
It is discovered that sexually active women younger than 25 and men who have sex with men are at increased risk of getting gonorrhea.[31]
Other risk factors include:
- Having a new sex partner
- Having a sex partner who has other partners
- Having more than one sex partner
- Having had gonorrhea or another sexually transmitted infection[32]
Complications
Untreated gonorrhea can lead to major complications, such as:
- Infertility in women. Gonorrhea can spread into the uterus and fallopian tubes, causing pelvic inflammatory disease (PID). PID can result in scarring of the tubes, greater risk of pregnancy complications and infertility, and can be fatal, particularly in the immunocompromised.[citation needed] PID requires immediate treatment.
- Infertility in men. Gonorrhea can cause a small, coiled tube in the rear portion of the testicles where the sperm ducts are located (epididymis) to become inflamed (epididymitis). Untreated epididymitis can lead to infertility.
- Infection that spreads to the joints and other areas of the body. The bacterium that causes gonorrhea can spread through the bloodstream and infect other parts of the body, including the joints. Fever, rash, skin sores, joint pain, swelling and stiffness are possible results.
- Increased risk of HIV/AIDS. Having gonorrhea increases the susceptibility to infection with human immunodeficiency virus (HIV), the virus that leads to AIDS. People who have both gonorrhea and HIV (untreated by anti-retroviral therapy) are able to pass both diseases more readily to their partners.
- Complications in babies. Babies who contract gonorrhea from their mothers during birth can develop blindness, sores on the scalp and infections.[24][25]
Diagnosis
Traditionally, gonorrhea was diagnosed with Gram stain and culture; however, newer polymerase chain reaction (PCR)-based testing methods are becoming more common.[18][33] If initial treatment fails, a culture should be done to determine the sensitivity of the bacteria to antibiotics.[34]
Tests that use PCR (aka nucleic acid amplification) to identify genes unique to N. gonorrhoeae are recommended for screening and diagnosis of gonorrhea infection. These PCR-based tests require a sample of urine, urethral swabs, or cervical/vaginal swabs. Culture (growing colonies of bacteria in order to isolate and identify them) and Gram-stain (staining of bacterial cell walls to reveal morphology) can also be used to detect the presence of N. gonorrhoeae in all specimen types except urine.[35][36] Studies of the swab sample method for gonorrhea infections have not shown any difference in the number of patients treated, whether the sample was collected at home or in the clinic. The implications for number of patients cured, reinfection rates, partner management, and safety are unknown.[37]
If Gram-negative, oxidase-positive diplococci are visualized on direct Gram stain of urethral pus (male genital infection), no further testing is needed to establish the diagnosis of gonorrhea infection.[38][39] However, direct Gram stain of cervical swabs is not useful because the N. gonorrhoeae organisms are less concentrated in these samples. The chance of a false positive test is also higher for a cervical swab, as Gram-negative diplococci native to the normal vaginal flora cannot be distinguished from N. gonorrhoeae in that context. Thus, cervical swabs must be cultured under the conditions described above. If oxidase positive, Gram-negative diplococci are isolated from a culture of a cervical/vaginal swab specimen, then the diagnosis is made. Culture is especially useful for diagnosis of infections of the throat, rectum, eyes, blood, or joints—areas where PCR-based tests are not well established in all labs.[39][40] Culture is also useful for antimicrobial sensitivity testing, analyzing treatment failure, and epidemiological purposes (outbreaks, surveillance).[39]
In patients who may have disseminated gonococcal infection (DGI), all possible mucosal sites should be cultured (e.g., pharynx, cervix, urethra, rectum).[40] Three sets of blood cultures should also be obtained.[41] Synovial fluid should be collected in cases of septic arthritis.[40]
All people testing positive for gonorrhea should be tested for other sexually transmitted infections such as
Screening
The United States Preventive Services Task Force (USPSTF) recommends screening for gonorrhea in women at increased risk of infection, which includes all sexually active women younger than 25 years. Extragenital gonorrhea and chlamydia are highest in men who have sex with men (MSM).[49] Additionally, the USPSTF also recommends routine screening in people who have previously tested positive for gonorrhea or have multiple sexual partners and individuals who use condoms inconsistently, provide sexual favors for money, or have sex while under the influence of alcohol or drugs.[16]
Screening for gonorrhea in women who are (or intend to become) pregnant, and who are found to be at high risk for sexually transmitted infections, is recommended as part of prenatal care in the United States.[50]
Prevention
As with most sexually transmitted infections, the risk of infection can be reduced significantly by the correct use of condoms, not having sex, or can be removed almost entirely by limiting sexual activities to a mutually monogamous relationship with an uninfected person.[51][52]
Those previously infected are encouraged to return for follow up care to make sure that the infection has been eliminated. In addition to the use of phone contact, the use of email and text messaging have been found to improve the re-testing for infection.[53]
Newborn babies coming through the birth canal are given erythromycin ointment in the eyes to prevent blindness from infection. The underlying gonorrhea should be treated; if this is done then usually a good prognosis will follow.[54]
Treatment
Antibiotics

Antibiotics are used to treat gonorrhea infections. As of 2016, both
Adults may have eyes infected with gonorrhoea and require proper personal hygiene and medications.[54] Addition of topical antibiotics have not been shown to improve cure rates compared to oral antibiotics alone in treatment of eye infected gonorrhea.[61] For newborns, erythromycin ointment is recommended as a preventative measure for gonococcal infant conjunctivitis.[62]
Infections of the throat can be especially problematic, as antibiotics have difficulty becoming sufficiently concentrated there to destroy the bacteria. This is amplified by the fact that pharyngeal gonorrhoea is mostly asymptomatic, and gonococci and commensal Neisseria species can coexist for long time periods in the pharynx and share anti-microbial resistance genes. Accordingly, an enhanced focus on early detection (i.e., screening of high-risk populations, such as men who have sex with men, PCR testing should be considered) and appropriate treatment of pharyngeal gonorrhoea is important.[4]
Sexual partners
It is recommended that sexual partners be tested and potentially treated.
The United States' Centers for Disease Control and Prevention (CDC) currently recommend that individuals who have been diagnosed and treated for gonorrhea avoid sexual contact with others until at least one week past the final day of treatment in order to prevent the spread of the bacterium.[64]
Antibiotic resistance
Many antibiotics that were once effective including
Prognosis

| no data <13 13–26 26–39 39–52 52–65 65–78 | 78–91 91–104 104–117 117–130 130–143 >143 |
Gonorrhea if left untreated may last for weeks or months with higher risks of complications.
In men, inflammation of the epididymis, prostate gland, and urethra can result from untreated gonorrhea.[68] In women, the most common result of untreated gonorrhea is pelvic inflammatory disease. Other complications include inflammation of the tissue surrounding the liver,[68] a rare complication associated with Fitz-Hugh–Curtis syndrome; septic arthritis in the fingers, wrists, toes, and ankles; septic abortion; chorioamnionitis during pregnancy; neonatal or adult blindness from conjunctivitis; and infertility. Men who have had a gonorrhea infection have an increased risk of getting prostate cancer.[22]
Epidemiology

About 88 million cases of gonorrhea occur each year, out of the 448 million new cases of curable STI each year – that also includes syphilis, chlamydia and trichomoniasis.[9] The prevalence was highest in the African region, the Americas, and Western Pacific, and lowest in Europe.[69] In 2013, it caused about 3,200 deaths, up from 2,300 in 1990.[70]
In the United Kingdom, 196 per 100,000 males 20 to 24 years old and 133 per 100,000 females 16 to 19 years old were diagnosed in 2005.[17] In 2013, the CDC estimated that more than 820,000 people in the United States get a new gonorrheal infection each year. Fewer than half of these infections are reported to CDC. In 2011, 321,849 cases of gonorrhea were reported to the CDC. After the implementation of a national gonorrhea control program in the mid-1970s, the national gonorrhea rate declined from 1975 to 1997. After a small increase in 1998, the gonorrhea rate has decreased slightly since 1999. In 2004, the rate of reported gonorrheal infections was 113. 5 per 100,000 persons.[71]
In the US, it is the second-most-common bacterial
The World Health Organization warned in 2017 of the spread of untreatable strains of gonorrhea, following analysis of at least three cases in Japan, France and Spain, which survived all antibiotic treatment.[75]
History
Some scholars translate the biblical terms zav (for a male) and zavah (for a female) as gonorrhea.[76]
It has been suggested[by whom?] that mercury was used as a treatment for gonorrhea.[when?] Surgeons' tools on board the recovered English warship the Mary Rose included a syringe that, according to some, was used to inject the mercury via the urinary meatus into crewmen with gonorrhea. The name "the clap", in reference to the disease, is recorded as early as the sixteenth century, referring to a medieval red-light district in Paris, Les Clapiers. Translating to "The rabbit holes", it was so named for the small huts in which prostitutes worked.[77][58]
The exact time of onset of gonorrhea as prevalent disease or epidemic cannot be accurately determined from the historical record. One of the first reliable notations occurs in the Acts of the (English) Parliament. In 1161, this body passed a law to reduce the spread of "... the perilous infirmity of burning".
Coincidental to, or dependent on, the appearance of a gonorrhea epidemic, several changes occurred in European medieval society. Cities hired
Medieval public health physicians in the employ of their cities were required to treat prostitutes infected with the "burning", as well as lepers and other epidemic patients.[83] After Pope Boniface completely secularized the practice of medicine, physicians were more willing to treat a sexually transmitted infection.[82]
Research
A vaccine for gonorrhea has been developed that is effective in mice.[84] It will not be available for human use until further studies have demonstrated that it is both safe and effective in the human population. Development of a vaccine has been complicated by the ongoing evolution of resistant strains and antigenic variation (the ability of N. gonorrhoeae to disguise itself with different surface markers to evade the immune system).[58]
As
References
- ^ a b c d e f g h i j k l m n o p q "Gonorrhea – CDC Fact Sheet (Detailed Version)". CDC. 17 November 2015. Archived from the original on 2 September 2016. Retrieved 27 August 2016.
- ^ PMID 27107780.
- ^ PMID 26042815.
- ^ a b c d e "Antibiotic-Resistant Gonorrhea Basic Information". CDC. 13 June 2016. Archived from the original on 8 September 2016. Retrieved 27 August 2016.
- ^ PMID 26293005.
- ^ PMID 26646541.
- ISBN 978-1-4963-5453-2.
- PMID 26063472.
- ^ a b Emergence of multi-drug resistant Neisseria gonorrhoeae (PDF) (Report). World Health Organisation. 2012. p. 2. Archived from the original (PDF) on 13 June 2013.
- PMID 27733281.
- ^ a b "Gonorrhea - Symptoms and causes". Mayo Clinic. Retrieved 6 August 2019.
- S2CID 207538182.
- ^ ISBN 978-0-8018-8658-4.
- ^ "Detailed STD Facts - Gonorrhea". www.cdc.gov. 5 April 2022. Retrieved 23 April 2022.
- PMID 30398526.
- ^ S2CID 37727850.
- ^ PMID 19454057.
- ^ PMID 25614838.
- ^ a b c "What Complications Can Gonorrhea Cause?". WebMD. 2019.
- ^ ISBN 978-1-4381-0142-2.
- ISBN 978-0-323-08619-6.
- ^ PMID 24986642.
- ^ "Prophylaxis for Gonococcal and Chlamydial Ophthalmia Neonatorum in the Canadian Guide to Clinical Preventative Health Care" (PDF). Public Health Agency of Canada. Archived from the original (PDF) on 10 March 2010.
- ^ a b "Complications from gonorrhea". stanfordhealthcare.org. Retrieved 25 April 2022.
- ^ a b "Gonorrhea - Symptoms and causes". Mayo Clinic. Retrieved 23 April 2022.
- PMID 25868133.
- ^ Howard Brown Health Center: STI Annual Report, 2009
- ^ National Institute of Allergy and Infectious Diseases; National Institutes of Health, Department of Health and Human Services (20 July 2001). "Workshop Summary: Scientific Evidence on Condom Effectiveness for Sexually Transmitted Disease (STD) Prevention". Hyatt Dulles Airport, Herndon, Virginia. pp14
- PMID 17961874.
- ISBN 978-1-4381-0142-2.
- OCLC 644578106.
- ISSN 0148-5717.
- PMID 19284360.
- ^ PMID 20643433.
- ^ a b "Final Recommendation Statement: Chlamydia and Gonorrhea: Screening – US Preventive Services Task Force". uspreventiveservicestaskforce.org. Retrieved 7 December 2017.
- ^ "Gonococcal Infections – 2015 STD Treatment Guidelines". cdc.gov. Retrieved 7 December 2017.
- PMID 26418128.
- )
- ^ PMID 18159523.
- ^ a b c https://www.cdc.gov/std/tg2015/clinical.htm section on prevention methods
- ^ Gonorrhea~overview at eMedicine
- S2CID 20864079.
- S2CID 39361152.
- S2CID 16507728.
- ^ "Gonococcal Infections - 2015 STD Treatment Guidelines". 4 January 2018.
- ISBN 978-0-8385-8529-0.[page needed]
- ^ Department of Reproductive Health and Research (2011). "Emergence of multi-drug resistant Neisseria gonorrhoeae – Threat of global rise in untreatable sexually transmitted infections" (PDF). FactSheet WHO/RHR/11.14. World Health Organization.
- ^ "Gonorrhea – STD information from CDC". cdc.gov. 6 October 2017. Retrieved 5 December 2017.
- PMID 18386598.
- ^ Health Care Guideline: Routine Prenatal Care. Fourteenth Edition. Archived 5 July 2008 at the Wayback Machine By the Institute for Clinical Systems Improvement July 2010.
- ^ section: Prevention Archived 20 July 2013 at the Wayback Machine
- ^ section: How can gonorrhea be prevented? Archived 16 December 2016 at the Wayback Machine
- PMID 25759476.
- ^ PMID 26903179.
- ^ PMID 22874837.
- ^ "Antibiotic-resistant gonorrhoea on the rise, new drugs needed". World Health Organization. 7 July 2017. Archived from the original on 9 July 2017. Retrieved 10 July 2017.
- PMID 31358980.
- ^ PMID 26579097.
- S2CID 246129045.
- ^ "Antibiotic Ertapenem is alternative drug in treatment of gonorrhea". Amsterdam UMC. 20 January 2022. Retrieved 8 July 2022.
- PMID 22348418.
- PMID 30694327.
- ^ "Expedited partner therapy in the management of sexually transmitted diseases" Archived 2 November 2009 at the Wayback Machine. February 2006. Centers for Disease Control and Prevention (CDC).
- ^ "Gonorrhea – CDC Fact Sheet". U.S. Centers for Disease Control and Prevention. 14 July 2014. Archived from the original on 16 December 2016. Retrieved 17 October 2014.
- ^ Groopman J (1 October 2012). "Sex and the Superbug". The New Yorker. Vol. LXXXVIII, no. 30. pp. 26–31. Archived from the original on 9 October 2012. Retrieved 13 October 2012.
...public-health experts [see]...the emergence of a strain of gonorrhea that is resistant to the last drug available against it, and the harbinger of a sexually transmitted global epidemic.
- S2CID 249747652.
- ^ "WHO guidelines for the treatment of Neisseria gonorrhoeae". World Health Organization. 2016. Retrieved 24 September 2020.
- ^ ISBN 978-1-4160-2973-1
- PMID 31505159.
- PMID 25530442.)
{{cite journal}}:|author1=has generic name (help)CS1 maint: numeric names: authors list (link - ^ "Gonorrhea – CDC Fact Sheet". CDC. 29 May 2012. Archived from the original on 16 December 2016. Retrieved 20 December 2013.
- ^ "CDC – STD Surveillance – Gonorrhea". Archived from the original on 6 March 2008. Retrieved 21 August 2008.
- ^ "CDC Fact Sheet – Chlamydia". Archived from the original on 16 December 2016. Retrieved 21 August 2008.
- ^ "STD Trends in the United States: 2010 National Data for Gonorrhea, Chlamydia, and Syphilis". Centers for Disease Control and Prevention (CDC). 22 November 2010. Archived from the original on 24 January 2012.
- ^ "Untreatable gonorrhoea 'superbug' spreading around world, WHO warns". The Daily Telegraph. 7 July 2017. Archived from the original on 7 July 2017.
- ^ "Daf Parashat Hashavua". Archived from the original on 3 October 2012. Retrieved 2 November 2012.
- ^ Higgins J (1587). The Mirror for Magistrates. as cited in the Oxford English Dictionary entry for "clap".
- S2CID 45492365.
- ^ MedlinePlus Encyclopedia: Neonatal Conjunctivitis
- ^ Sanger W (1910). History of Prostitution. New York: Harper.
- ^ LaCroix P (1931). The History of Prostitution. Vol. 2. New Yory: MacMillan.
- ^ ISBN 9789386367570.
- ^ Leiky WE (1926). History of European Morals. New York: MacMillan.
- PMID 24016806.
- PMID 27922851.
- S2CID 4230156.
- ^ "GSK's gonorrhoea vaccine receives FDA's 'fast-track' designation". Reuters. 27 June 2023. Retrieved 20 August 2023.
External links
- Gonorrhea at Curlie
- "Gonorrhea – CDC Fact Sheet"
