Hospital-acquired pneumonia
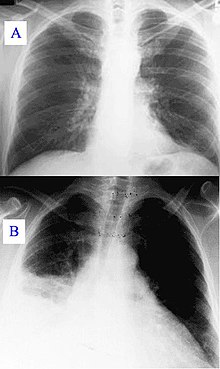
Hospital-acquired pneumonia (HAP) or nosocomial pneumonia refers to any pneumonia contracted by a patient in a hospital at least 48–72 hours after being admitted. It is thus distinguished from community-acquired pneumonia. It is usually caused by a bacterial infection, rather than a virus.[1][2]
Hospital acquired pneumonia is the second most common
Hospital acquired pneumonia typically lengthens a hospital stay by 1–2 weeks.[1][3]
Signs and symptoms
New or progressive infiltrate on the chest X-ray with one of the following:[3]
- Fever > 37.8 °C (100 °F)
- Purulent sputum
- Leukocytosis > 10,000 cells/μl
In an elderly person, the first sign of hospital-acquired pneumonia may be mental changes or confusion. Other symptoms may include:
- A cough with greenish or pus-like phlegm (sputum)
- Fever and chills
- General discomfort, uneasiness, or ill feeling (malaise)
- Loss of appetite
- Nausea and vomiting
- Sharp chest pain that gets worse with deep breathing or coughing
- Shortness of breath
- Decreased blood pressure and fast heart rate[5]
Types
- gram-negative organisms (52%) and Staphylococcus aureus (19%), usually of the MRSA type.[6] Others are Haemophilus spp. (5%). In the ICU results were S. aureus (17.4%), Pseudomonas aeruginosa (17.4%), Klebsiella pneumoniae and Enterobacter spp. (18.1%), and Haemophilus influenzae (4.9%).[1]
- Viral pneumonia: influenza and respiratory syncytial virus and, in the immunocompromised host, cytomegalovirus – cause 10–20% of infections.[2]
Ventilator-associated pneumonia
Ventilator-associated pneumonia (VAP) is a sub-type of hospital-acquired pneumonia (HAP) which occurs in people who are receiving mechanical ventilation. VAP is not characterized by the causative agents; rather, as its name implies, definition of VAP is restricted to patients undergoing mechanical ventilation while in a hospital. A positive culture after intubation is indicative of ventilator-associated pneumonia and is diagnosed as such. In order to appropriately categorize the causative agent or mechanism it is usually recommended to obtain a culture prior to initiating mechanical ventilation as a reference.[citation needed]
Healthcare-associated pneumonia (HCAP)
HCAP is a condition in patients who can come from the community, but have frequent contact with the healthcare environment. Historically, the etiology and prognosis of nursing home pneumonia appeared to differ from other types of community acquired pneumonia, with studies reporting a worse prognosis and higher incidence of multi drug resistant organisms as etiology agents. The definition criteria which has been used is the same as the one which has been previously used to identify bloodstream healthcare associated infections.
HCAP is no longer recognized as a clinically independent entity. This is due to increasing evidence from a growing number of studies that many patients defined as having HCAP are not at high risk for MDR pathogens. As a result, 2016 IDSA guidelines removed consideration of HCAP as a separate clinical entity.[7]
Definition
Healthcare-associated pneumonia can be defined as pneumonia in a patient with at least one of the following risk factors:
- hospitalization in an acute care hospital for two or more days in the last 90 days;
- residence in a nursing home or long-term care facility in the last 30 days
- receiving outpatient antibiotics or chemotherapy) within the past 30 days
- receiving home wound care within the past 30 days
- attending a hospital clinic or dialysis center in the last 30 days
- having a family member with known
Causes
In some studies, the bacteria found in patients with HCAP were more similar to HAP than to CAP; compared to CAP, they could have higher rates of
Treatment
Patients with HCAP are more likely than those with community-acquired pneumonia to receive inappropriate antibiotics that do not target the bacteria causing their disease.[citation needed]
In 2002, an expert panel made recommendations about the evaluation and treatment of probable nursing home-acquired pneumonia.[22] They defined probably pneumonia, emphasized expedite antibiotic treatment (which is known to improve survival) and drafted criteria for the hospitalization of willing patients.
For initial treatment in the nursing home, a
In 2005, the
- cefepime, ceftazidime, imipenem, meropenem or piperacillin–tazobactam; plus
- ciprofloxacin, levofloxacin, amikacin, gentamicin, or tobramycin; plus
- linezolid or vancomycin
In one observational study, empirical antibiotic treatment that was not according to international treatment guidelines was an independent predictor of worse outcome among HCAP patients.[25]
Guidelines from Canada suggest that HCAP can be treated like community-acquired pneumonia with antibiotics targeting Streptococcus pneumoniae, based on studies using blood cultures in different settings which have not found high rates of MRSA or Pseudomonas.[26] For children and neonatal infants, different antibiotic approaches including cefepime, ceftazidime, linezolid, vancomycin, meropenem, cefotaxime, ceftobiprole, or cephalosporin are sometimes used.[4] There is no clear evidence which antibiotic approach is best for both aiding recovery and decreasing harmful effects.[4]
Besides prompt antibiotic treatment, supportive measure for organ failure (such as
Prognosis
Healthcare-associated pneumonia seems to have
Epidemiology
Several studies found that healthcare-associated pneumonia is the second most common type of pneumonia, occurring less commonly than community-acquired pneumonia but more frequently than hospital-acquired pneumonia and ventilator-associated pneumonia. In a recent observational study, the rates for CAP, HCAP and HAP were 60%, 25% and 15% respectively.[25] Patients with HCAP are older and more commonly have simultaneous health problems (such as previous stroke, heart failure and diabetes).[32]
The number of residents in long-term care facilities is expected to rise dramatically over the next 30 years. These older adults are known to develop pneumonia 10 times more than their community-dwelling peers, and hospital admittance rates are 30 times higher.[11][13]
Nursing home-acquired pneumonia
Nursing home-acquired pneumonia is an important subgroup of HCAP. Residents of long-term care facilities may become infected through their contacts with the healthcare system; as such, the
Risk factors
Among the factors contributing to contracting HAP are mechanical ventilation (ventilator-associated pneumonia), old age, decreased filtration of inspired air, intrinsic respiratory, neurologic, or other disease states that result in respiratory tract obstruction, trauma, (abdominal) surgery, medications, diminished lung volumes, or decreased clearance of secretions may diminish the defenses of the lung. Also, poor hand-washing and inadequate disinfection of respiratory devices cause cross-infection and are important factors.[1][3]
Pathogenesis
Most nosocomial respiratory infections are caused by so-called microaspiration of upper airway secretions, through inapparent aspiration, into the lower respiratory tract. Also, "macroaspirations" of esophageal or gastric material is known to result in HAP. Since it results from aspiration either type is called aspiration pneumonia.[1][2][3]
Although
Diagnosis
In hospitalised patients who develop respiratory symptoms and fever, one should consider the diagnosis. The likelihood increases when upon investigation symptoms are found of
Differential diagnosis
- Atelectasis
- Congestive heart failure
- Pulmonary embolism
Treatment
Usually initial therapy is empirical.
A third generation
]References
- ^ a b c d e f g h i j
Mandell's Principles and Practices of Infection Diseases 6th Edition (2004) by Gerald L. Mandell MD, MACP, John E. Bennett MD, Raphael Dolin MD, ISBN 0-443-06643-4· Hardback · 4016 Pages Churchill Livingstone
- ^ ISBN 0-19-262922-0
- ^ ISBN 0-07-140235-7
- ^ PMID 34727368.
- ^ medlineplus.gov
- ISBN 978-1-4160-2973-1. 8th edition.
- ^ "2016 IDSA guidelines" (PDF). Retrieved 1 September 2016.
- ^ "IDSA guidelines" (PDF). Retrieved 3 April 2012.
- S2CID 24129964.
- PMID 24270053.
- ^ PMID 9809694.
- ^ S2CID 39009527.
- ^ PMID 15526736. Archived from the originalon 2008-07-19. Retrieved 2013-08-02.
- PMID 15909270.
- PMID 18261707.
- PMID 17012732.
- S2CID 2422020.
- ^ clevelandcliniceded.com
- ^ Rouille the JL. Ventilator-associated pneumonia: an comprehensive review. Hosp Pract (Minneap) 2012; 40:165–175
- ^ (clevelandclinicmeded.com)
- ^ (Medlineplus.gov)
- PMID 12184969.
- .
- S2CID 14907563.
- ^ PMID 19124816.
- PMID 15993675.
- PMID 18299494.
- PMID 8911243.
- S2CID 25082600.
- PMID 16165074.
- PMID 14871636.
- ^ S2CID 4950173.
- PMID 9789516.
- PMID 11712938.
- S2CID 44467811.
- S2CID 744043.
- S2CID 31882884.
- S2CID 37840890.
Further reading
- Carratalà J, Garcia-Vidal C (2008). "What is healthcare-associated pneumonia and how is it managed?". Curr. Opin. Infect. Dis. 21 (2): 168–173. S2CID 3060658.
- Morrow L. Critical Decisions for the Treatment of Health-care-Associated Pneumonia in the ICU.
External links
- Hospital-Acquired, Health Care Associated, and Ventilator-Associated Pneumonia from the Cleveland Clinic
- Cecil Textbook of Medicine
