Heart valve
| Heart valve | |
|---|---|
 Valves of the heart in motion, the front wall of the heart is removed in this image. | |
| Details | |
| System | Cardiovascular |
| Identifiers | |
| MeSH | D006351 |
| FMA | 7110 |
| Anatomical terminology | |
A heart valve is a biological
The four valves in the mammalian heart are two
The heart also has a
Structure

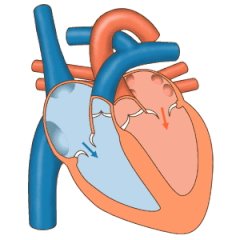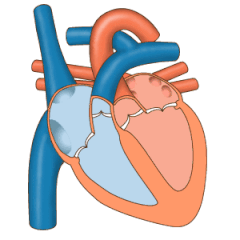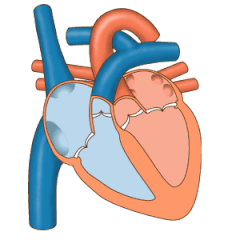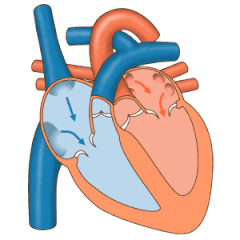
The heart valves and the
The pulmonary valve has left, right, and anterior cusps.[4] The aortic valve has left, right, and posterior cusps.[5] The tricuspid valve has anterior, posterior, and septal cusps; and the mitral valve has just anterior and posterior cusps.
The valves of the human heart can be grouped in two sets:[6]
- Two atrioventricular valves to prevent backflow of blood from the ventricles into the atria:
- Tricuspid valve or right atrioventricular valve, between the right atrium and right ventricle
- Mitral valve or bicuspid valve, between the left atrium and left ventricle
- Two semilunar valves to prevent the backflow of blood into the ventricle:
- Pulmonary valve, located at the opening between the right ventricle and the pulmonary trunk
- Aortic valve, located at the opening between the left ventricle and the aorta.
| Valve | Number of flaps/cusps | location | prevent backflow of blood |
|---|---|---|---|
| Atrioventricular valves | 3 (right), 2 (left) | From the ventricles into the atria | |
| Tricuspid valve | 3 | between the right atrium and right ventricle. | |
| Bicuspid or mitral valve | 2 | between the left atrium and left ventricle. | |
| Semilunar valves | 3 (half-moon shaped) flaps | into the ventricle | |
| Pulmonary semilunar valve | 3 (half-moon shaped) flaps | at the opening between the right ventricle and the pulmonary trunk | |
| Aortic semilunar valve | 3 (half-moon shaped) flaps | at the opening between the left ventricle and the aorta |
Atrioventricular valves
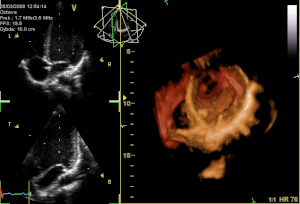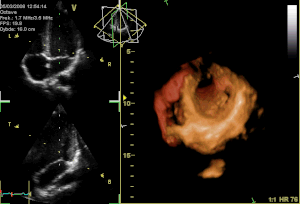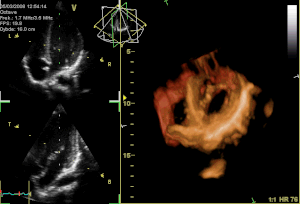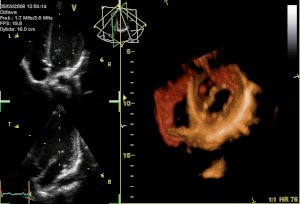
The atrioventricular valves are the mitral valve, and the tricuspid valve, which are situated between the atria and the ventricles, and prevent backflow from the ventricles into the atria during systole. They are anchored to the walls of the ventricles by chordae tendineae, which prevent them from inverting.
The chordae tendineae are attached to papillary muscles that cause tension to better hold the valve. Together, the papillary muscles and the chordae tendineae are known as the subvalvular apparatus. The function of the subvalvular apparatus is to keep the valves from prolapsing into the atria when they close.[7] The subvalvular apparatus has no effect on the opening and closure of the valves, however, which is caused entirely by the pressure gradient across the valve. The peculiar insertion of chords on the leaflet free margin, however, provides systolic stress sharing between chords according to their different thickness.[8]
The closure of the AV valves is heard as lub, the
The mitral valve is also called the bicuspid valve because it contains two leaflets or cusps. The mitral valve gets its name from the resemblance to a
During diastole, a normally-functioning mitral valve opens as a result of increased pressure from the left atrium as it fills with blood (preloading). As atrial pressure increases above that of the left ventricle, the mitral valve opens. Opening facilitates the passive flow of blood into the left ventricle. Diastole ends with atrial contraction, which ejects the final 30% of blood that is transferred from the left atrium to the left ventricle. This amount of blood is known as the end diastolic volume (EDV), and the mitral valve closes at the end of atrial contraction to prevent a reversal of blood flow.
The tricuspid valve has three leaflets or cusps and is on the right side of the heart. It is between the
Semilunar valves
The aortic and pulmonary valves are located at the base of the aorta and the
The
, pressure rises in the left ventricle and when it is greater than the pressure in the aorta, the aortic valve opens, allowing blood to exit the left ventricle into the aorta. When ventricular systole ends, pressure in the left ventricle rapidly drops and the pressure in the aorta forces the aortic valve to close. The closure of the aortic valve contributes the A2 component of the second heart sound.The
Development
In the developing heart, the valves between the atria and ventricles, the bicuspid and the tricuspid valves, develop on either side of the atrioventricular canals.[9] The upward extension of the bases of the ventricles causes the canal to become invaginated into the ventricle cavities. The invaginated margins form the rudiments of the lateral cusps of the AV valves. The middle and septal cusps develop from the downward extension of the septum intermedium.
The semilunar valves (the pulmonary and aortic valves) are formed from four thickenings at the cardiac end of the
Physiology
In general, the motion of the heart valves is determined using the


- Relationship between pressure and flow in open valves
The pressure drop, , across an open heart valve relates to the flow rate, Q, through the valve:
If:
- Inflow energy conserved
- Stagnant region behind leaflets
- Outflow momentum conserved
- Flat velocity profile
- Valves with a single degree of freedom
Usually, the aortic and mitral valves are incorporated in valve studies within a single degree of freedom. These relationships are based on the idea of the valve being a structure with a single degree of freedom. These relationships are based on the Euler equations.
Equations for the aortic valve in this case:
where:
- u = axial velocity
- p = pressure
- A = cross sectional area of valve
- L = axial length of valve
- Λ(t) = single degree of freedom; when
Atrioventricular valve
Clinical significance
Valvular heart disease is a general term referring to dysfunction of the valves, and is primarily in two forms, either regurgitation, (also insufficiency, or incompetence) where a dysfunctional valve lets blood flow in the wrong direction,[10] or stenosis, when a valve is narrow.[11]
Regurgitation occurs when a valve becomes insufficient and malfunctions, allowing some blood to flow in the wrong direction. This insufficiency can affect any of the valves as in
Disease of the heart valves can be congenital, such as
Valvular heart disease is diagnosed by echocardiography, which is a form of ultrasound. Damaged and defective heart valves can be repaired, or replaced with artificial heart valves. Infectious causes may also require treatment with antibiotics.[11]
Congenital heart disease
The most common form of valvular anomaly is a
Less common CHD's are tricuspid and pulmonary atresia, and Ebstein's anomaly. Tricuspid atresia is the complete absence of the tricuspid valve which can lead to an underdeveloped or absent right ventricle. Pulmonary atresia is the complete closure of the pulmonary valve. Ebstein's anomaly is the displacement of the septal leaflet of the tricuspid valve causing a larger atrium and a smaller ventricle than normal.
History
This section needs expansion. You can help by adding to it. (October 2014) |

Function of heart valves
- Artificial heart valve
- Pericardial heart valves
- Bjork–Shiley valve
References
![]() This article incorporates text in the public domain from the 20th edition of Gray's Anatomy (1918)
This article incorporates text in the public domain from the 20th edition of Gray's Anatomy (1918)
- ^ "Heart Valves". American Heart Association, Inc – 10000056 Heart and Stroke Encyclopedia. American Heart Association, Inc. Retrieved 2010-08-05.
- ^ Klabunde, RE (2009-07-02). "Pressure Gradients". Cardiovascular Physiology Concepts. Richard E. Klabunde. Archived from the original on 2015-04-16. Retrieved 2010-08-06.
- ^ Klabunde, RE (2007-04-05). "Cardiac Valve Disease". Cardiovascular Physiology Concepts. Richard E. Klabunde. Retrieved 2010-08-06.
- ^ Anatomy photo:20:21-0102 at the SUNY Downstate Medical Center – "Heart: The Pulmonic Valve"
- ^ Anatomy photo:20:29-0104 at the SUNY Downstate Medical Center – "Heart: The Aortic Valve and Aortic Sinuses"
- ISSN 0008-6363.
- S2CID 4870179.
- ^ S Nazari et al.: Patterns Of Systolic Stress Distribution On Mitral Valve Anterior Leaflet Chordal Apparatus. A Structural Mechanical Theoretical Analysis. J Cardiovasc Surg (Turin) 2000 Apr;41(2):193–202 (video)
- ^ ISBN 978-0-443-06811-9.
- ^ "An Overview of Heart Valve Disease". WebMD. Retrieved 9 May 2021.
- ^ ISBN 978-0-7020-3085-7.)
{{cite book}}:|first=has generic name (help)CS1 maint: multiple names: authors list (link - ^ ISBN 978-1-4160-2973-1.
- ^ Bertazzo, S. et al. Nano-analytical electron microscopy reveals fundamental insights into human cardiovascular tissue calcification. Nature Materials 12, 576–83 (2013).
- ^ Miller, J. D. Cardiovascular calcification: Orbicular origins. Nature Materials 12, 476–78 (2013).






![{\displaystyle A(x,t)=A_{0}\left(1-[1-{\Lambda }(t)]{x \over {L}}\right)^{2}}](https://wikimedia.org/api/rest_v1/media/math/render/svg/d86e8a7cd26aac3833526c8a4a24ace993b9f68f)
![{\displaystyle \int _{0}^{L}p(x,t){{\partial }A \over {\partial }x}\,dx=[A_{0}-A(L,t)]\,p(L,t)}](https://wikimedia.org/api/rest_v1/media/math/render/svg/cd1e3437e71128cc9a0e20f42e2ab4d7dbbc19d8)
