Hemolysis
This article needs more primary sources. (November 2021) |  |
| Hemolysis | |
|---|---|
| Other names | Haemolysis (alternative spelling), hematolysis, erythrolysis, or erythrocytolysis |
 | |
| Specialty | Pathology |
| Complications | Kidney failure, kidney disease |
| Causes | Osmosis |
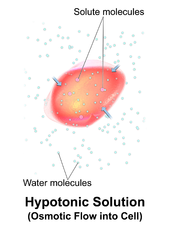

Hemolysis or haemolysis (/hiːˈmɒlɪsɪs/),[1] also known by several other names, is the rupturing (lysis) of red blood cells (erythrocytes) and the release of their contents (cytoplasm) into surrounding fluid (e.g. blood plasma). Hemolysis may occur in vivo or in vitro.
One cause of hemolysis is the action of
Etymology
From hemo- + -lysis, from Ancient Greek αἷμα (haîma, 'blood') + λύσις lúsis, 'loosening').
Inside the body
Hemolysis inside the body can be caused by a large number of medical conditions, including some parasites (e.g.,
Hemolysis can lead to hemoglobinemia due to hemoglobin released into the blood plasma, which plays a significant role in the pathogenesis of sepsis[7] and can lead to increased risk of infection due to its inhibitory effects on the innate immune system.[7]
Parasitic hemolysis
Because the feeding process of the Plasmodium parasites damages red blood cells, malaria is sometimes called "parasitic hemolysis" in medical literature.[citation needed]
HELLP, pre-eclampsia, or eclampsia
- See HELLP syndrome, Pre-eclampsia, and Eclampsia
Hemolytic disease of the newborn
Hemolytic disease of the newborn is an autoimmune disease resulting from the mother's antibodies crossing the placenta to the fetus. This most often occurs when the mother has previously been exposed to blood antigens present on the fetus but foreign to her, through either a blood transfusion or a previous pregnancy.[8]
Hemolytic anemia
Because in vivo hemolysis destroys red blood cells, in uncontrolled, chronic or severe cases it can lead to hemolytic anemia.
Hemolytic crisis
A hemolytic crisis, or hyperhemolytic crisis, is characterized by an accelerated rate of red blood cell destruction leading to
Toxic agent ingestion or poisoning
Paxillus involutus ingestion can cause hemolysis.
Space hemolysis
Spaceflight can cause hemolysis.[10]
Intrinsic causes
Hemolysis may result from intrinsic defects in the red blood cell itself:[11][12]
- Defects of red blood cell membrane production (as in hereditary spherocytosis and hereditary elliptocytosis)
- Defects in hemoglobin production (as in sickle-cell disease and congenital dyserythropoietic anemia)
- Defective red cell metabolism (as in glucose-6-phosphate dehydrogenase deficiency and pyruvate kinase deficiency)
- Paroxysmal nocturnal hemoglobinuria (PNH), sometimes referred to as Marchiafava-Micheli syndrome, is a rare, acquired, potentially life-threatening disease of the blood characterized by complement-induced intravascular hemolytic anemia.
Extrinsic causes
Extrinsic hemolysis is caused by the red blood cell's environment:[5][6]
- Immune-mediated causes could include transient factors as in chronic lymphocytic leukemia).
- Spur cell hemolytic anemia
- Any of the causes of hypersplenism (increased activity of the spleen), such as portal hypertension.
- Acquired hemolytic anemia is also encountered in burns and as a result of certain infections (e.g. malaria).
- Lead poisoning or poisoning by arsine or stibine causes non-immune hemolytic anemia.[6]
- Runners can develop hemolytic anemia due to "footstrike hemolysis", the destruction of red blood cells in feet at foot impact.[13][14]
- Low-grade hemolytic anemia occurs in 70% of prosthetic heart valve recipients, and severe hemolytic anemia occurs in 3%.[15]
Intravascular hemolysis
Intravascular hemolysis describes hemolysis that happens mainly inside the
Intravascular hemolysis may occur when red blood cells are targeted by autoantibodies, leading to complement fixation, or by damage by parasites such as Babesia.[19] Additionally, thrombotic microangiopathy (TMA) can result in hemolysis of red blood cells.[20] TMA is frequently observed in aHUS patients where clots form in the small vessels of the kidney resulting in damaged red blood cells as they attempt to pass through the restricted vessels.[21]
Extravascular hemolysis
Extravascular hemolysis refers to hemolysis taking place in the
If extravascular hemolysis is extensive, hemosiderin can be deposited in the spleen, bone marrow, kidney, liver, and other organs, resulting in hemosiderosis.[18]
Outside the body
In vitro hemolysis can be caused by improper technique during collection of blood specimens, by the effects of mechanical processing of blood, or by bacterial action in cultured blood specimens.
From specimen collection
Most causes of in vitro hemolysis are related to specimen collection. Difficult collections, unsecure line connections, contamination, and incorrect needle size, as well as improper tube mixing and incorrectly filled tubes are all frequent causes of hemolysis.
In vitro hemolysis during specimen collection can cause inaccurate laboratory test results by contaminating the surrounding plasma with the contents of hemolyzed red blood cells. For example, the concentration of potassium inside red blood cells is much higher than in the plasma and so an elevated potassium level is usually found in biochemistry tests of hemolyzed blood.
After the blood collection process, in vitro hemolysis can still occur in a sample due to external factors, such as prolonged storage, incorrect storage conditions and excessive physical forces by dropping or vigorously mixing the tube.
From mechanical blood processing during surgery
In some surgical procedures (especially some heart operations) where substantial blood loss is expected, machinery is used for
From bacteria culture

Visualizing the physical appearance of hemolysis in cultured blood samples may be used as a tool to determine the species of various Gram-positive bacteria infections (e.g., Streptococcus).
Nomenclature
Hemolysis is sometimes called hematolysis, erythrolysis, or erythrocytolysis. The words hemolysis ().
Red blood cells (erythrocytes) have a short lifespan (approximately 120 days), and old (senescent) cells are constantly removed and replaced with new ones via erythropoiesis. This breakdown/replacement process is called erythrocyte turnover. In this sense, erythrolysis or hemolysis is a normal process that happens continually. However, these terms are usually used to indicate that the lysis is pathological.
Complications
Pulmonary hypertension has been gaining recognition as a complication of chronic hereditary and acquired hemolysis.
Chronic hemolysis may also lead to
Complications may also arise from the increased workload for the kidney as it secretes erythropoietin to stimulate the bone marrow to produce more reticulocytes (red blood cell precursors) to compensate for the loss of red blood cells due to hemolysis.[24]
See also
References
- ^ ISBN 978-1-4058-8118-0.
- PMID 28416897.
- ISBN 978-0-321-64963-8.
- ^ "Atypical hemolytic-uremic syndrome". Genetics Home Reference. Retrieved 2020-08-18.
- ^ PMID 26404442.
- ^ PMID 26404441.
- ^ S2CID 49526899.
- ^ "Erythrocyte Alloimmunization and Pregnancy: Overview, Background, Pathophysiology". 2019-02-02.
{{cite journal}}: Cite journal requires|journal=(help) - ^ "Innvista". Archived from the original on 2010-06-24. Retrieved 2010-07-04.
- ^ Guzman, Ana (2022-02-24). "Scientists Find Increased Red Blood Cell Destruction in Space". NASA. Retrieved 2022-06-09.
- PMID 8813716.
- PMID 8813717.
- S2CID 5750453.
- PMID 22682343.
- ]
- ^ a b Stanley L Schrier. William C Mentzer; Jennifer S Tirnauer (eds.). "Diagnosis of hemolytic anemia in the adult". UpToDate. Archived from the original on 2017-12-26. Retrieved 2019-05-04.
- ^ "Intravascular hemolysis". eClinpath. Retrieved 2019-05-08.
- ^ PMID 16793184. Archived from the original(PDF) on 2019-05-03. Retrieved 2019-05-04.
- ^ "Bilirubin and hemolytic anemia". eClinpath. Retrieved 2019-05-08.
- ^ "Thrombotic Microangiopathy (TMA)". UNC Kidney Center. Retrieved 2020-08-19.
- ^ "Atypical Hemolytic Uremic Syndrome". NORD (National Organization for Rare Disorders). Retrieved 2020-08-19.
- PMID 30855920. Retrieved 2019-05-04.
- PMID 6788179.
- ^ a b c d Braunstein, Evan (2019-05-03). "Overview of Hemolytic Anemia – Hematology and Oncology". Merck Manuals Professional Edition (in Latin). Retrieved 2019-05-05.
- ^ "Hypersplenism: MedlinePlus Medical Encyclopedia". MedlinePlus. 2019-04-30. Retrieved 2019-05-08.
- ^ "Capital Health".
- S2CID 753640.
- S2CID 73496695.
- ^ "hematolysis". Merriam-Webster.com Dictionary. Retrieved 8 July 2018.
- ^ "erythrolysis". American Heritage Stedman's Medical Dictionary. Houghton Mifflin. Archived from the original on 8 July 2018. Retrieved 8 July 2018.
- ^ "erythrocytolysis". American Heritage Stedman's Medical Dictionary. Houghton Mifflin. Archived from the original on 8 July 2018. Retrieved 8 July 2018.
- ^ PMID 20522578.
- PMID 15811985.
- ^ S2CID 19878520.
- PMID 15811985.
The systemic removal of nitric oxide has been shown to contribute to clinical morbidities, including severe esophageal spasm and dysphagia, abdominal pain, erectile dysfunction, and thrombosis.16,17,23-26 In addition, systemic release of hemoglobin is associated with pulmonary and systemic hypertension,17,20,53-55 decreased organ perfusion, and increased mortality.53-58 Plasma hemoglobin and its breakdown product heme can also directly activate endothelial cells and further promote inflammation and coagulation.27
- PMID 23264591.
- PMID 26175690.
- PMID 25389409.Material was copied from this source, which is available under a Creative Commons License.

