Herpes simplex keratitis
| Herpes simplex keratitis | |
|---|---|
| Other names | Herpetic keratoconjunctivitis, herpesviral keratitis |
 | |
| Dendritic corneal ulcer after fluorescein staining | |
| Specialty | Ophthalmology |
Herpetic simplex keratitis is a form of keratitis caused by recurrent herpes simplex virus (HSV) infection in the cornea.[1]
It begins with infection of
Subsequent recurrences may be more severe, with infected epithelial cells showing larger dendritic ulceration, and lesions forming white plaques.
HSV infection is very common in humans. It has been estimated that one third of the world population have recurrent infection. Keratitis caused by HSV is the most common cause of cornea-derived
Signs and symptoms
Primary infection

Primary infection most commonly manifests as
Recurrent eye infection
Recurrent herpes of the eye is caused by reactivation of the virus in a latently infected sensory ganglion, transport of the virus down the nerve axon to sensory nerve endings, and subsequent infection of ocular surface. The following classification of herpes simplex keratitis is important for understanding this disease:
Dendritic ulcer (Epithelial keratitis)
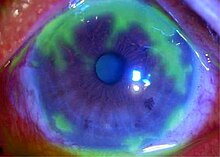
This classic herpetic lesion consists of a linear branching corneal ulcer (dendritic ulcer). During eye exam the defect is examined after staining with fluorescein dye. The underlying cornea has minimal inflammation.
Patients with epithelial keratitis complain of foreign-body sensation, light sensitivity, redness and blurred vision.
Focal or diffuse reduction in corneal sensation develops following recurrent epithelial keratitis.
In immune deficient patients or with the use of corticosteroids the ulcer may become large and in these cases it is called geographic ulcer.[6]
Disciform keratitis (Endothelial keratitis)
Endothelial keratitis manifests a central
Localized endothelitis (localized inflammation of corneal endothelial layer) is the cause of disciform keratitis.
Other forms
- Metaherpetic ulcer : is not due to live virus, results from inability of the corneal surface to heal.
- Necrotizing keratitis
- Keratouveitis : is usually granulomatous uveitis with large keratic precipitates on the corneal endothelium.
Cause
HSV is a double-stranded DNA virus that has icosahedral capsid. HSV-1 infections are found more commonly in the oral area and HSV-2 in the genital area. Ocular herpes simplex is usually caused by HSV-1.[7][8]
Diagnosis

A specific clinical diagnosis of HSV as the cause of dendritic keratitis can usually be made by
- Corneal smears or impression cytology specimens can be analyzed by culture, antigen detection, or fluorescent antibody testing. Tzanck smear, i.e.Papanicolaou staining of corneal smears[further explanation needed], show multinucleated giant cells and intranuclear inclusion bodies, however, the test is low in sensitivity and specificity.
- DNA testing is rapid, sensitive and specific. However, its high cost limits its use to research centers.
- Demonstration of HSV is possible with viral culture.
- Serologic tests may show a rising antibody titer during primary infection but are of no diagnostic assistance during recurrent episodes.
Treatment
Treatment of herpes of the eye is different based on its presentation: epithelial keratitis is caused by live virus while stromal disease is an immune response and metaherpetic ulcer results from inability of the corneal epithelium to heal. But on the viral aciclovir eye ointment q.i.d can be used together a systemic antiviral drug t.d.s for 10/7. :[4][6]
Epithelial keratitis
Epithelial keratitis is treated with topical antivirals, which are very effective with low incidence of resistance. Treatment of the disease with topical antivirals generally should be continued for 10–14 days. Aciclovir ophthalmic ointment and Trifluridine eye drops have similar effectiveness but are more effective than Idoxuridine and Vidarabine eye drops.[9] Oral acyclovir is as effective as topical antivirals for treating epithelial keratitis, and it has the advantage of no eye surface toxicity. For this reason, oral therapy is preferred by some ophthalmologists.
Ganciclovir and brivudine treatments were found to be equally as effective as acyclovir in a systematic review.[9]
Topical
The effect of interferon with an antiviral agent or an antiviral agent with debridement needs further assessment.[9]
Stromal keratitis
Herpetic stromal keratitis is treated initially with prednisolone drops every 2 hours accompanied by a prophylactic antiviral drug: either topical antiviral or an oral agent such as acyclovir or valacyclovir. The prednisolone drops are tapered every 1–2 weeks depending on the degree of clinical improvement. Topical antiviral medications are not absorbed by the cornea through an intact epithelium, but orally administered acyclovir penetrates an intact cornea and anterior chamber. In this context, oral acyclovir might benefit the deep corneal inflammation of disciform keratitis.[6]
Metaherpetic ulcer
Treatment includes artificial tears and eye lubricants, stopping toxic medications, performing punctal occlusion, bandage contact lens and amniotic membrane transplant. These measures intend to improve corneal epithelial healing.
Antiviral medication may reduce the risk of HSV keratitis recurring in people having a graft due to HSV infection and may improve the chances of graft survival.[10]
References
- ISBN 978-0-7216-2921-6.
- S2CID 21409244.
- ^ PMID 10858770.
- ^ ISBN 9780323043328.
- PMID 22542912.
- ^ ISBN 978-1615251155.
- PMID 19445742.
- S2CID 226946434.
- ^ PMID 25879115.
- PMID 27902849.
