Hodgkin lymphoma
| Hodgkin lymphoma | |
|---|---|
| Other names | Hodgkin's lymphoma, Hodgkin's disease[1] |
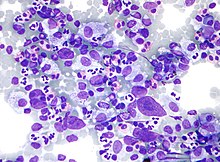 | |
| Micrograph showing Hodgkin lymphoma (Field stain) | |
| Specialty | Hematology and oncology |
| Symptoms | Fever, night sweats, weight loss, nonpainful enlarged lymph nodes[2] |
| Risk factors | Epstein–Barr virus, family history, HIV/AIDS[2][3] |
| Diagnostic method | Lymph node biopsy[2] |
| Treatment | Chemotherapy, radiation therapy, stem-cell transplant,[4] immunotherapy |
| Prognosis | Five-year survival rate 88% (US)[5] |
| Frequency | 574,000 (affected during 2015)[6] |
| Deaths | 23,900 (2015)[7] |
| Named after | Thomas Hodgkin |
Hodgkin lymphoma (HL) is a type of lymphoma in which cancer originates from a specific type of white blood cell called lymphocytes, where multinucleated Reed–Sternberg cells (RS cells) are present in the patient's lymph nodes.[2][8] The condition was named after the English physician Thomas Hodgkin, who first described it in 1832.[9][10] Symptoms may include fever, night sweats, and weight loss.[2] Often, nonpainful enlarged lymph nodes occur in the neck, under the arm, or in the groin.[2] Persons affected may feel tired or be itchy.[2]
The two major types of Hodgkin lymphoma are classic Hodgkin lymphoma and
Hodgkin lymphoma may be treated with
In 2015, about 574,000 people globally had Hodgkin lymphoma, and 23,900 (4.2%) died.[6][7] In the United States, 0.2% of people are affected at some point in their life.[5] Most people are diagnosed with the disease between the ages of 20 and 40.[5]
Signs and symptoms
People with Hodgkin lymphoma may present with these symptoms:
- lymph nodes.[14] The nodes may also feel rubbery and swollen when examined. The nodes of the neck, armpits and groin (cervical and supraclavicular) are most frequently involved (80–90% of the time, on average).[14] The lymph nodes of the chest are often affected, and these may be noticed on a chest radiograph.[14]
- Systemic symptoms: About one-third of people with Hodgkin disease may also present with systemic symptoms, including:[15]
- Itchy skin[15]
- Night sweats[15]
- Unexplained weight loss of at least 10% of the person's total body mass in six months or less[15]
- Low-grade fever.[15]
- Fatigue (lassitude)[15]
- Systemic symptoms such as fever, night sweats, and weight loss are known as B symptoms; thus, presence of these indicate that the person's stage is, for example, 2B instead of 2A.[15]
- Splenomegaly: Enlargement of the spleen is often present in people with Hodgkin lymphoma. The enlargement is seldom massive, and the size of the spleen may fluctuate during the course of treatment.[14]
- Hepatomegaly: Enlargement of the liver, due to liver involvement, is infrequent in people with Hodgkin lymphoma.[14]
- Hepatosplenomegaly: The enlargement of both the liver and spleen can be caused by the same disease.
- Pain following alcohol consumption: Classically, involved nodes are painful after alcohol consumption, though this phenomenon is very uncommon,[16] occurring in only two to three percent of people with Hodgkin lymphoma,[17] thus having a low sensitivity. On the other hand, its positive predictive value is high enough for it to be regarded as a pathognomonic sign of Hodgkin lymphoma.[17] The pain typically has an onset within minutes after ingesting alcohol, and is usually felt as coming from the vicinity where there is an involved lymph node.[17] The pain has been described as either sharp and stabbing or dull and aching.[17]
- Back pain: Nonspecific back pain (pain that cannot be localised or its cause determined by examination or scanning techniques) has been reported in some cases of Hodgkin lymphoma. The lower back is most often affected.[18]
- Cyclical fever: People may also present with a cyclical high-grade fever known as the Pel–Ebstein fever,[19] or more simply "P-E fever". However, there is debate as to whether the P-E fever truly exists.[20]
- Nephrotic syndrome can occur in individuals with Hodgkin lymphoma and is most commonly caused by minimal change disease.[21]
- May present with airway obstruction, pleural/pericardial effusion, hepatocellular dysfunction, or bone-marrow infiltration.
Diagnosis
Hodgkin lymphoma must be distinguished from noncancerous causes of lymph node swelling (such as various infections) and from other types of cancer. Definitive diagnosis is by lymph node biopsy (usually excisional biopsy with microscopic examination). Blood tests are also performed to assess function of major organs and safety for chemotherapy.[22] Positron emission tomography (PET) is used to detect small deposits that do not show on CT scanning. PET scans are also useful in functional imaging (by using a radiolabeled glucose to image tissues of high metabolism). In some cases, a gallium scan may be used instead of a PET scan.[23]
Types
The two main types of Hodgkin lymphoma are classic Hodgkin lymphoma and nodular lymphocyte-predominant Hodgkin lymphoma. The prevalence of classic Hodgkin lymphoma and nodular-lymphocyte Hodgkin lymphoma are about 90 and 10%, respectively.[24][25] The morphology, phenotype, molecular features, and, therefore, the clinical behaviour and presentation of the two types differ.[26]
Classic
Classic Hodgkin lymphoma (excluding nodular lymphocyte predominant Hodgkin lymphoma) can be subclassified into four pathologic subtypes based upon Reed–Sternberg cell morphology and the composition of the reactive cell infiltrate seen in the lymph node biopsy specimen (the cell composition around the Reed–Sternberg cell(s)). Presence of EBV in Reed-Sternberg cells is most commonly found in the subtypes lymphocyte depleted HL (>70%) and mixed cellularity HL (70%), whilst being less prevalent in lymphocyte-rich HL (40%) and relatively uncommon by comparison in nodular sclerosing HL.[27][28]
| Name | Description | ICD-10 | ICD-O
|
|---|---|---|---|
| Nodular sclerosing HL | Is the most common subtype and is composed of large plasma cells with varying degrees of collagen fibrosis/sclerosis. |
C81.1 | M9663/3 |
| Mixed-cellularity subtype | Is a common subtype and is composed of numerous classic RS cells admixed with numerous inflammatory cells including lymphocytes, histiocytes, eosinophils, and plasma cells without sclerosis. This type is most often associated with Epstein-Barr virus infection and may be confused with the early, so-called 'cellular' phase of the nodular sclerosing subtype. This type of Hodgkin lymphoma is most commonly seen in immunocompromised people. |
C81.2 | M9652/3. |
| Lymphocyte-rich | Is a rare subtype, show many features which may cause diagnostic confusion with nodular lymphocyte predominant B-cell non-Hodgkin lymphoma (B-NHL). This form also has the most favorable prognosis. | C81.0 | M9651/3 |
| Lymphocyte depleted | Is a rare subtype, composed of large numbers of often pleomorphic RS cells with only few reactive lymphocytes which may easily be confused with anaplastic large cell lymphoma.[29] |
C81.3 | M9653/3 |
| Unspecified | C81.9 | M9650/3 |


For the other forms, although the traditional
However, this may be an artifact of the ambiguity inherent in the diagnosis.Hodgkin cells produce
Nodular lymphocyte predominant
Nodular lymphocyte predominant Hodgkin lymphoma (NLPHL) is another subtype of Hodgkin lymphoma distinct from classic Hodgkin lymphoma and is characterized by the presence of popcorn cells which express CD20.[25][34] Due to these differences, among others, NLPHL is often treated differently from classic Hodgkin lymphoma, including using rituximab in combination with AVBD chemotherapy, though individual cases vary and clinical trials are ongoing.[25]
Staging
The staging is the same for both Hodgkin and non-Hodgkin lymphomas.
After Hodgkin lymphoma is diagnosed, a person will be
On the basis of this staging, the person will be classified according to a staging classification (the
- Stage I is involvement of a single lymph node region (I) (mostly the cervical region) or single extralymphatic site (Ie);
- Stage II is involvement of two or more lymph node regions on the same side of the diaphragm(II) or of one lymph node region and a contiguous extralymphatic site (IIe);
- Stage III is involvement of lymph node regions on both sides of the diaphragm, which may include the spleen (IIIs) or limited contiguous extralymphatic organ or site (IIIe, IIIes);
- Stage IV is disseminated involvement of one or more extralymphatic organs.
The absence of systemic symptoms is signified by adding "A" to the stage; the presence of systemic symptoms is signified by adding "B" to the stage. For localised extranodal extension from mass of nodes that does not advance the stage, subscript "E" is added. Splenic involvement is signified by adding "S" to the stage. The inclusion of "bulky disease" is signified by "X".[37]
-
Stage 1 Hodgkin lymphoma
-
Stage 2 Hodgkin lymphoma
-
Stage 3 Hodgkin lymphoma
-
Stage 4 Hodgkin lymphoma
Pathology
Macroscopy
Affected lymph nodes (most often, laterocervical lymph nodes) are enlarged, but their shape is preserved because the capsule is not invaded. Usually, the cut surface is white-grey and uniform; in some histological subtypes (e.g. nodular sclerosis) a nodular aspect may appear.[38]
A fibrin ring granuloma may be seen.
Microscopy

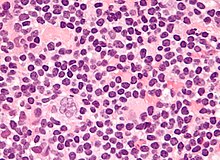
Microscopic examination of the lymph node biopsy reveals complete or partial effacement of the lymph node architecture by scattered large malignant cells known as
Characteristics of classic Reed–Sternberg cells include large size (20–50 micrometres), abundant, amphophilic, finely granular/homogeneous cytoplasm; two mirror-image nuclei (owl eyes) each with an eosinophilic nucleolus and a thick nuclear membrane (chromatin is distributed close to the nuclear membrane). Almost all of these cells have an increased copy number of chromosome 9p/9p24.1.[40]
Variants:
- Hodgkin cell (atypical mononuclear RSC) is a variant of RS cell, which has the same characteristics but is mononucleated.[41]
- Lacunar RSC is large, with a single hyperlobulated nucleus, multiple, small nucleoli and eosinophilic cytoplasm which is retracted around the nucleus, creating an empty space ("lacunae").
- Pleomorphic RSC has multiple irregular nuclei.
- "Popcorn" RSC (lympho-histiocytic variant) is a small cell, with a very lobulated nucleus, small nucleoli.
- "Mummy" RSC has a compact nucleus with no nucleolus and basophilic cytoplasm.
Hodgkin lymphoma can be sub-classified by histological type. The cell histology in Hodgkin lymphoma is not as important as it is in non-Hodgkin lymphoma: the treatment and prognosis in classic Hodgkin lymphoma usually depends on the stage of disease rather than the histotype.[42]
Management
The current approach for treatment aims to reduce the acute and long-term toxicities associated with Hodgkin lymphoma (e.g. cardiac damage and secondary cancers) and increase overall survival.[43]
People with early stage disease (IA or IIA) can be treated effectively with radiation therapy or chemotherapy. The choice of treatment depends on the age, sex, bulk and the histological subtype of the disease.[42] Adding localised radiation therapy after the chemotherapy regimen may provide a longer
| MOPP | ABVD | Stanford V | BEACOPP |
|---|---|---|---|
| The original treatment for Hodgkin's was Oncovin (also known as vincristine), Prednisone and Procarbazine (also known as Matulane). The treatment is usually administered in four week cycles, often for six cycles. MSD and VCR are administered intravenously, while procarbazine and prednisone are pills taken orally. MOPP was the first combination chemotherapy brought in that achieved a high success rate. It was developed at the National Cancer Institute in the 1960s by a team that included Vincent DeVita Jr.
Although no longer the most effective combination, MOPP is still used after relapse or where the person has certain allergies or lung or heart problems which prevents the use of another regimen. |
Currently, the . Developed in Italy in the 1970s, the ABVD treatment typically takes between six and eight months, although longer treatments may be required. | The newer Stanford V regimen is typically only half as long as the ABVD but involves a more intensive chemotherapy schedule and incorporates radiation therapy. In a randomised controlled study in Italy, Stanford V was inferior to ABVD;[46] however, this study has been heavily criticized due to its incorrect administration of radiotherapy, diverging from the original Stanford V protocol.[47] | GCSF to increase production of white blood cells. Currently, the German Hodgkin Study Group tests 8 cycles (8x) BEACOPP esc vs. 6x BEACOPP esc vs. 8x BEACOPP-14 baseline (HD15-trial).[48]
|
| Chlormethine | Doxorubicin | Doxorubicin | Doxorubicin |
Oncovin
|
Bleomycin | Bleomycin | Bleomycin |
| Prednisone | Vinblastine | Vinblastine, Vincristine | Vincristine |
| Procarbazine | Dacarbazine | Chlormethine | Cyclophosphamide, Procarbazine |
| Etoposide | Etoposide | ||
| Prednisone | Prednisone |
The common non-Hodgkin treatment, rituximab (which is a monoclonal antibody against CD20) is not routinely used to treat Hodgkin lymphoma due to the lack of CD20 surface antigens in most cases. The use of rituximab in Hodgkin lymphoma, including the lymphocyte predominant subtype has been recently reviewed.[49] The evidence is very uncertain about the effect of Nivolumab for patients with a Hodgkin's lymphoma e.g. on the overall survival.[50]
Increased age is an adverse risk factor for Hodgkin lymphoma, but in general elderly people (≥ 60 years of age) without major comorbidities are sufficiently fit to tolerate therapy with curative intent. Despite this, treatment outcome in the elderly patient is not comparable to that of younger people and the disease is a different entity in older people where different considerations enter into treatment decisions.[51][52]
Recently, two novel targeted drugs have been developed for relapsing and refractory HL patients; Brentuximab vedotin, a CD30 antibody conjugated with a cytotoxic component MMAE,[53] and the checkpoint inhibitors, Nivolumab and Pembrolizumab.[54][55][56][57] This has been an important step in the treatment for the few, but still existing refractory patients.
For Hodgkin lymphomas, radiation oncologists typically use
For lymphomas, there are a few different ways radiation oncologists target the cancer cells. Involved site radiation is when the radiation oncologists give radiation only to those parts of the person's body known to have the cancer.[58] Very often, this is combined with chemotherapy. Radiation therapy directed above the diaphragm to the neck, chest or underarms is called mantle field radiation. Radiation to below the diaphragm to the abdomen, spleen or pelvis is called inverted-Y field radiation. Total nodal irradiation is when the therapist gives radiation to all the lymph nodes in the body to destroy cells that may have spread.[59]
Adverse effects
The high cure rates and long survival of many people with Hodgkin lymphoma has led to a high concern with late adverse effects of treatment, including cardiovascular disease and second malignancies such as acute
In childhood cases of Hodgkin lymphoma, long-term endocrine adverse effects are a major concern, mainly gonadal dysfunction and
It is possible that patients undergoing a chemotherapy need a platelet transfusion.[62][63] If a stem cell transplantation is necessary for the treatment of a relapse, graft-versus-host diseases might occur.[64]
Supportive treatment
Adding physical exercises to the standard treatment for adult patients with haematological malignancies like Hodgkin lymphoma may result in little to no difference in the mortality, the quality of life and the physical functioning. These exercises may result in a slight reduction in depression. Furthermore, aerobic physical exercises probably reduce fatigue. The evidence is very uncertain about the effect on anxiety and serious adverse events.[65]
Prognosis
Treatment of Hodgkin's disease has been improving over the past few decades. Recent[when?] trials that have made use of new types of chemotherapy have indicated higher survival rates than have previously been seen. In one recent European trial, the five-year survival rate for those people with a favorable prognosis (FFP) was 98%, while that for people with worse outlooks was at least 85%.[66]
In 1998, an international effort[67] identified seven prognostic factors that accurately predict the success rate of conventional treatment in people with locally extensive or advanced-stage Hodgkin lymphoma. Freedom from progression (FFP) at five years was directly related to the number of factors present in a person. The five-year FFP for people with zero factors is 84%. Each additional factor lowers the five-year FFP rate by 7%, such that the five-year FFP for a person with five or more factors is 42%.[68]
The adverse prognostic factors identified in the international study are:
- Age ≥ 45 years
- Stage IV disease
- Hemoglobin < 10.5 g/dl
- Lymphocyte count< 600/µl or < 8%
- Male
- Albumin < 4.0 g/dl
- White blood count≥ 15,000/µl
Other studies have reported the following to be the most important adverse prognostic factors: mixed-cellularity or lymphocyte-depleted histologies, male sex, large number of involved nodal sites, advanced stage, age of 40 years or more, the presence of B symptoms, high erythrocyte sedimentation rate, and bulky disease (widening of the mediastinum by more than one third, or the presence of a nodal mass measuring more than 10 cm in any dimension.)[69]
More recently, the use of positron emission tomography (PET) early after commencing chemotherapy has demonstrated to have powerful prognostic ability.[70] This enables assessment of an individual's response to chemotherapy as the PET activity switches off rapidly in people who are responding. In this study,[70] after two cycles of ABVD chemotherapy, 83% of people were free of disease at 3 years if they had a negative PET versus only 28% in those with positive PET scans. This prognostic method improves on FFP estimates based on the seven conventional factors. Several trials are underway to see if PET-based risk adapted response can be used to improve a person's outcomes by changing chemotherapy early in people who are not responding.
The evidence is very uncertain about the effect of negative (= good prognosis) or positive (= bad prognosis) interim PET scan results for patients with a Hodgkin's lymphoma on the progression-free survival. Negative interim PET scan results may result in an increase in progression-free survival compared if the adjusted result was measured. Negative interim PET scan results probably result in a large increase in the overall survival compared to those with a positive interim PET scan result,[43]
Epidemiology
Unlike some
In 2010, globally it resulted in about 18,000 deaths down from 19,000 in 1990.[1] In 2012, there were an estimated 65,950 cases and 25,469 deaths from Hodgkin lymphoma worldwide, with 28,852 and 37,098 cases occurring in developed and developing countries, respectively.[74] However, the age-standardized rates were higher in developed regions, with the greatest rates in the Americas (1.5 per 100,000), East Mediterranean Region (1.5 per 100,000), and Europe (2.0 per 100,000).[74] The East Mediterranean Region also has the highest age-standardized mortality rate of 1.0 per 100,000, which is mainly attributed to lifestyle and environmental risk factors associated with transitional economies such as smoking, obesity, physical inactivity, and reproductive behaviors, as well as availability of diagnostic practices and awareness of the disease.[74]
The number of cases of Hodgkin lymphoma is increased in people with HIV infection.[75] In contrast to many other lymphomas associated with HIV infection it occurs most commonly in people with higher CD4 T cell counts.
Canada
Hodgkin lymphoma accounts for 0.6% of all male cancer cases, and 0.4% of all female cancer cases in Canada. In 2017, approximately 990 Canadians will be diagnosed with Hodgkin lymphoma, and 140 will die of the disease.[76]
UK
Hodgkin lymphoma accounts for less than 1% of all cancer cases and deaths in the UK. Around 1,800 people were diagnosed with the disease in 2011, and around 330 people died in 2012.[77]
United States
In 2016, there were 8,389 new cases and 1,000 mortalities attributed to Hodgkin lymphoma, a decrease from the 8,625 new cases and 1,120 mortalities in 2015.[78] As of January 1, 2016, the 5-year limited duration prevalence of Hodgkin lymphoma was 37,513 representing 0.71% of all diagnosed cancers in the U.S.[78]
History

Hodgkin lymphoma was first described in an 1832 report by Thomas Hodgkin, although Hodgkin noted that perhaps an earlier reference to the condition was provided by Marcello Malpighi in 1666.[79][10] While occupied as museum curator at Guy's Hospital, London, Hodgkin studied seven people with painless lymph node enlargement. Of the seven cases, two were under the care of Richard Bright, one was of Thomas Addison, and one was of Robert Carswell.[79] Carswell's report of the seventh case was accompanied by numerous illustrations that aided early descriptions of the disease.[80]
Hodgkin's report on the seven cases, entitled "On some morbid appearances of the absorbent glands and spleen", was presented to the Medical and Chirurgical Society of London in January 1832 and was subsequently published in the society's journal, Medical-Chirurgical Society Transactions.[79] Hodgkin's paper went largely unnoticed, however, even though Bright highlighted it in an 1838 publication.[79] Indeed, Hodgkin himself did not view his contribution as particularly significant.[81]
In 1856, Samuel Wilks independently reported on a series of patients with the same disease that Hodgkin had previously described.[81] Wilks, a successor to Hodgkin at Guy's Hospital, was unaware of Hodgkin's prior work on the subject. Bright informed Wilks of Hodgkin's contribution and in 1865, Wilks published a second paper, entitled "Cases of enlargement of the lymphatic glands and spleen", in which he named the illness "Hodgkin's disease" in honor of his predecessor.[81]
Tissue specimens from Hodgkin's seven cases were preserved at Guy's Hospital. Nearly 100 years after Hodgkin's initial publication, histopathologic reexamination confirmed Hodgkin lymphoma in only three of seven of these people.[81] The remaining cases included non-Hodgkin lymphoma, tuberculosis, and syphilis.[81]
Hodgkin lymphoma was one of the first cancers to be treated successfully with
Notable cases
- Paul Allen, co-founder of Microsoft was diagnosed with Hodgkin lymphoma in 1982. He later died from non-Hodgkin lymphoma, on October 15, 2018.[82]
- Eric Berry, All-Pro strong safety for the Kansas City Chiefs of the National Football League, diagnosed in 2014.[83]
- David Brooks, Welsh professional footballer, diagnosed in 2021 while playing for AFC Bournemouth.[84]
- Dale Carnegie, Public Speaker and author of "How to Win Friends and Influence People" (c)1936, Born 1888, Maryville, MO, died 1955, Forrest Hills,NY.[85] [86] [87]
- Howard Carter, Egyptologist and discoverer of the Tomb of Tutankhamun, died in 1939 from Hodgkin's disease.[88][89]
- medical neglect.[90]
- James Conner, running back and 2014 ACC Player of the Year for the Arizona Cardinals.[91]
- Michael Cuccione, Canadian child actor, was diagnosed in 1994 at age 9. Treatments that rendered him cancer-free, including chemotherapy, a bone marrow transplant, and radiation, left him with permanent lung and respiratory problems and he died in 2001 just after turning 16.[92][93][circular reference]
- Victoria Duval, American tennis player, was diagnosed in 2014.[94]
- Gerald Finzi, British composer, was diagnosed in 1951 and died in 1956.[95]
- Mist Edvardsdóttir, Icelandic football player and member of the Icelandic women's national team. Diagnosed in June 2014 at the age of 23. Continued to play until becoming too ill due to chemotherapy. Made recovery in early 2015.[96][97]
- Delta Goodrem, Australian singer, songwriter, and actress. She was diagnosed in July 2003 at the age of 18.[98]
- Hank Green, one of the cofounders of the Vlogbrothers, VidCon and production company Complexly, announced that he was diagnosed with Hodgkin lymphoma in a video he released on 19 May 2023.[99] Green would announce his entrance into remission on 25 August 2023.[100]
- Jiří Grossmann, Czechoslovak theatre actor, poet, and composer[101]
- Michael C. Hall (born February 1, 1971), American actor, best known for his lead role as Dexter Morgan, in Showtime's crime series Dexter. In 2010, aged 38, Hall announced he was undergoing treatment for Hodgkin lymphoma; within two years, the disease was in full remission.[102]
- Richard Harris, Irish actor who portrayed Albus Dumbledore in the first two Harry Potter movies, died on October 25, 2002, after being diagnosed earlier that year.[103]
- Daniel Hauser, whose mother fled with him in 2009 in order to prevent him from undergoing chemotherapy.[104]
- Tessa James, Australian actress, was diagnosed in 2014.[105]
- stand up comedian and actor. Was diagnosed in 2002 while writing on The Best Damn Sports Show Period.[106][107] After three months of chemotherapy and one month of radiation, the cancer went into remission.[107]
- Mario Lemieux, Hall of Fame NHL player, co-owner of the Pittsburgh Penguins and founder of the Mario Lemieux Foundation, diagnosed in 1993.[108]
- Dinu Lipatti (1917–1950), Romanian classical pianist and composer. Diagnosed in 1947, received cortisone treatment in 1949; died from a burst abscess on his one lung.[109]
- Jack Lisowski, English snooker player, diagnosed in 2008 at the age of 16.[110]
- Mamta Mohandas, Indian film actress and producer, diagnosed in 2010.[111][circular reference]
- Nanni Moretti, Italian actor and director.[112]
- Laura Packard, health care activist diagnosed in 2017, spoke at the 2020 Democratic National Convention.[113]
- Nikola Pokrivač, Croatian soccer midfielder, diagnosed in 2015.[114]
- Anthony Rizzo, MLB All-Star first baseman for the New York Yankees, diagnosed in May 2008 while signed as a minor league player for the Boston Red Sox.[115]
- Dave Roberts, MLB outfielder and manager of the Los Angeles Dodgers. Diagnosed in March 2010 while he was a coach for the San Diego Padres.[116]
- Chip Roy, Texas congressman.[117]
- Flip Saunders, head coach of the NBA team Minnesota Timberwolves, announced in August 2015 that he was diagnosed with Hodgkin's disease. He died of the disease in October 2015.[118]
- Arlen Specter, United States Senator from Pennsylvania (1981–2011), diagnosed in 2005. He later died from non-Hodgkin lymphoma in 2012.[119]
- Brandon Tartikoff, American television executive, diagnosed around 1974, died in 1997.[120]
- Bernardo Tengarrinha, Portuguese professional footballer, diagnosed in 2017 Tengarrinha died on October 30, 2021, at the age of 32. Hours later, his former teams FC Porto and Boavista FC paid tribute to him before the local derby. playing for FC Porto.[121]
- Ethan Zohn, American professional soccer player and a winner of the Survivor reality television series. Zohn was diagnosed twice (in 2009 and 2011).[122]
- Richard Holliday, American professional wrestler, reported to be ill with diagnosis from June 2022, completed treatment February 17, 2023[123]
- Rick Czaplewski, Author Better Dirty Than Done, Motivational Speaker, 2009 Boston Marathon Finisher.[124]
References
- ^ S2CID 1541253.
- ^ a b c d e f g h i "Adult Hodgkin Lymphoma Treatment (PDQ) – Patient Version". NCI. August 3, 2016. Archived from the original on 28 July 2016. Retrieved 12 August 2016.
- ^ ISBN 978-928320429-9.
- ^ a b c "Adult Hodgkin Lymphoma Treatment (PDQ) – Patient Version". NCI. August 3, 2016. Archived from the original on 28 July 2016. Retrieved 13 August 2016.
- ^ a b c d e "SEER Stat Fact Sheets: Hodgkin Lymphoma". NCI. April 2016. Archived from the original on 17 October 2012. Retrieved 13 August 2016.
- ^ PMID 27733282.
- ^ PMID 27733281.
- ISBN 978-1118293003. Archivedfrom the original on 2017-09-10.
- ^ PMID 20818856.
- ^ a b Hodgkin T (1832). "On some morbid experiences of the absorbent glands and spleen". Med Chir Trans. 17: 69–97.
- S2CID 46790198.
- S2CID 47010934.
- PMID 24488779.
- ^ PMID 26541251.
- ^ a b c d e f g Portlock CS (July 2008). "Hodgkin Lymphoma". Merck Manual Professional. Archived from the original on June 28, 2009. Retrieved June 18, 2009.
- PMID 6613116.
- ^ ISBN 978-90-5702-215-9.
- ^ a b "Hodgkin Lymphoma". The Lecturio Medical Concept Library. Retrieved 25 July 2021.
- ISBN 978-0-7817-6422-3.
- PMID 7777006.
- PMID 20200355.
- ^ "Hodgkin Lymphoma Diagnosis | Tests for Hodgkin Lymphoma". www.cancer.org. Retrieved 2022-11-09.
- PMID 32345712.
- PMID 26538004.
- ^ OCLC 1011064243.)
{{cite book}}: CS1 maint: location missing publisher (link) CS1 maint: others (link - S2CID 8192701.
- S2CID 27274760.
- S2CID 2355660.
- ^ a b "HMDS: Hodgkin's Lymphoma". Archived from the original on March 4, 2009. Retrieved February 1, 2009.
- PMID 12078890.
- PMID 16385563.
- S2CID 22493125.
- PMID 18684866.
- PMID 26541251.
- S2CID 11505564.
- ^ Board PP (2022-04-08). "[Table], Table 4. Ann Arbor Staging Classification for Hodgkin Lymphomaa". www.ncbi.nlm.nih.gov. Retrieved 2022-11-09.
- PMID 32644754, retrieved 2022-11-09
- ^ Baba AI, Câtoi C (2007). TUMORS OF HEMATOPOIETIC AND LYMPHOID TISSUES. The Publishing House of the Romanian Academy.
- PMID 25418190.)
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link - PMID 31816062.
- PMID 31194473, retrieved 2022-11-09
- ^ a b "Hodgkin lymphoma". NHS. 23 October 2017. Retrieved 25 July 2021.
- ^ PMID 31930780.
- PMID 28447341.
- PMID 23696962.
- S2CID 24367707.
- PMID 19759185.
- ^ "Home | German Hodgkin Study Group". Ghsg.org. Archived from the original on 2011-08-17. Retrieved 2012-08-26.
- PMID 21183282.
- S2CID 16108474.
- ^ Borchmann, S., Engert, A. & Böll, B. (2018). Hodgkin lymphoma in elderly patients. Current Opinion in Oncology, 30 (5), 308-316. doi: 10.1097/CCO.0000000000000464.
- from the original on 2009-05-12.
- S2CID 15815020.
- S2CID 43857382.
- PMID 23023715.
- PMID 25185243.
- PMID 23515511.
- PMID 23790512.
- ^ "RTanswers.com". RTanswers.com. 2010-12-03. Archived from the original on 2012-09-09. Retrieved 2012-08-26.
- PMID 23812271.
- PMID 21896559.
- PMID 22592695.
- PMID 26576687.
- PMID 30697701.
- PMID 30702150.
- S2CID 11153555.
- PMID 9819449.
- PMID 27900988.
- PMID 28083035.
- ^ S2CID 9959867.
- ^ "WHO Disease and injury country estimates". World Health Organisation. 2009. Archived from the original on 2009-11-11. Retrieved Nov 11, 2009.
- ISBN 978-0-7817-1502-7.
- ^ "SEER Stat Fact Sheets: Leukemia". NCI Surveillance, Epidemiology, and End Results Program. Archived from the original on 17 October 2012. Retrieved 18 August 2014.
- ^ PMID 25045456.
- PMID 16917006.
- ^ "Canadian Cancer Statistics". www.cancer.ca. Archived from the original on 2018-01-25. Retrieved 2018-02-08.
- ^ "Hodgkin lymphoma statistics". Cancer Research UK. Archived from the original on 17 October 2014. Retrieved 27 October 2014.
- ^ a b "Lymphoma | CDC". www.cdc.gov. 2019-01-16. Retrieved 2019-11-25.
- ^ ISBN 978-0-7817-6422-3.
- PMID 10594291.
- ^ PMID 6381744.
- ^ "Microsoft co-founder Paul Allen diagnosed with cancer". CNN. Retrieved 2017-12-23.
- ^ "Eric Berry has Hodgkin's lymphoma". ESPN. 2014-12-08. Archived from the original on 2015-03-08.
- ^ "Bournemouth midfielder David Brooks diagnosed with cancer". Sky Sports. 13 October 2021. Retrieved 13 October 2021.
- ^ "Dale Carnagie at Biography.com". 6 February 2024. Retrieved 6 February 2024.
- ^ "Dale Carnagie page: strategies for influence". 6 February 2024. Retrieved 8 February 2024.
- ISBN 978-1-64095-416-8. Retrieved 8 February 2024.
- ISBN 9781845112585. Archivedfrom the original on 2017-09-10.
- doi:10.1093/ref:odnb/32312. (Subscription or UK public library membershiprequired.)
- ^ "Teen, court reach agreement over cancer care". NBC News. Associated Press. September 5, 2006. Retrieved June 18, 2009.
- ^ "James Conner Announces Cancer Diagnosis". Archived from the original on 2016-09-12. Retrieved 2016-09-29.
- ^ "Childhood Cancer Research Program—Michael Cuccione Foundation". www.childhoodcancerresearch.org. Archived from the original on 2016-08-18. Retrieved 2016-07-22.
- ^ Michael Cuccione
- ^ "Victoria Duval battling cancer". 2014-07-04. Archived from the original on 2016-01-12.
- ^ "Gerald Finzi biography". Retrieved 27 November 2017.
- Dagblaðið Vísir(in Icelandic). pp. 30–31. Retrieved 23 April 2021.
- ^ Gunnar Birgisson (11 October 2020). "Ótrúleg endurkoma eftir röð áfalla". RÚV (in Icelandic). Retrieved 23 April 2021.
- ^ "Delta Goodrem Hospitalized With Cancer". Billboard. 2003-07-14.
- ^ vlogbrothers (19 May 2023). "So, I've got cancer". YouTube. Retrieved 19 May 2023.
- ^ vlogbrothers (25 August 2023), Remission, retrieved 2023-08-26
- ISBN 80-902731-7-3.
- ^ Huver S (2010-07-23). "Cancer-Free Michael C. Hall Back to Work on Dexter—Health, Dexter, Michael C. Hall". People. Archived from the original on 2015-02-08. Retrieved 2015-03-04.
- ^ "Lionhearted—Death, Richard Harris". People. Archived from the original on 2015-02-04. Retrieved 2015-03-04.
- ^ "Minnesota: Evaluation Ordered for a 13-Year-Old With Cancer". The New York Times. Associated Press. May 16, 2009. Archived from the original on May 31, 2015. Retrieved June 18, 2009.
- ^ "Tessa James reveals she is in remission". Yahoo! News Australia. Archived from the original on 2015-12-22. Retrieved 2015-12-16.
- ^ "Comedian Sean Kent laughs off hecklers, cancer to stay on road". Columbia Daily Tribune. Retrieved 19 May 2023.
- ^ a b Chandler R (28 November 2007). "Funnyman Sean Kent winning fight vs. cancer". www.tahoedailytribune.com. Retrieved 19 May 2023.
- ^ "Mario Lemieux Foundation". Archived from the original on 3 April 2013. Retrieved 11 April 2013.
- ^ Mark Ainley (2002). "Dinu Lipatti: Prince of Pianists". markainley.com. Archived from the original on 22 October 2015. Retrieved 30 August 2015.
- ^ "Cancer fight gives Lisowski new angle on life". Daily Telegraph. Archived from the original on April 30, 2013.
- ^ Mamta Mohandas
- ^ Laura Winters (2002). "FILM; An Italian Satirist Takes a Very Serious Turn". The New York Times. Retrieved 6 September 2020.
- ^ "Denver health care activist speaking at Democratic convention". Denver Post. 2020-08-18.
- ^ "Nikola Pokrivač: Nema predaje, sve ću podnijeti za ženu i kćer" (in Croatian). 8 June 2017. Retrieved 10 September 2015.[permanent dead link]
- ^ "Emma: Anthony Rizzo's Indelible Impact". CBS Chicago. 8 May 2014. Archived from the original on 14 September 2015. Retrieved 30 August 2015.
- ^ "'04 Red Sox hero Roberts treated for lymphoma". ESPN.com. 2010-05-03. Retrieved 2020-10-28.
- ^ Chasnoff B (May 13, 2018). "Chip Roy's plan to get Washington out of the way includes going there himself". San Antonio Express-News. ExpressNews.com. Retrieved September 18, 2020.
- ^ |"Minnesota Timberwolves Say Head Coach Flip Saunders Has Died". abc.go.com. Archived from the original on 2015-10-26. Retrieved 2015-10-25.
- ^ "Specter diagnosed with Hodgkin's disease". CNN. 16 February 2005. Retrieved 31 August 2021.
- ^ Carter B (1997-08-28). "Brandon Tartikoff, Former NBC Executive Who Transformed TV in the 80's, Dies at 48". The New York Times.
- ^ "Portuguese midfielder Bernardo Tengarrinha diagnosed with linfoma de Hodgkin". Abola. 30 October 2021. Retrieved 30 October 2021.
- ^ "Ethan Zohn is a survivor in more ways than one". Chicago Tribune. 18 June 2014. Archived from the original on 2016-03-17. Retrieved 2016-03-26.
- ^ Thompson A (17 Feb 2023). "Richard Holliday completes cancer treatment". Post Wrestling. Retrieved 23 May 2023.
- ^ Czaplewski R (2023-09-30). "Home". www.rickczaplewski.com. Retrieved 2024-01-18.
Further reading
- Charlotte DeCroes Jacobs. Henry Kaplan and the Story of Hodgkin's Disease (Stanford University Press; 2010) 456 pages; combines a biography of the American radiation oncologist (1918–84) with a history of the lymphatic cancer whose treatment he helped to transform.
External links
- Hodgkin lymphoma at Curlie
- Hodgkin Lymphoma at American Cancer Society
- Hodgkin Lymphoma at the American National Cancer Institute




