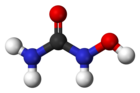
Hydroxycarbamide
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Droxia, Hydrea, Siklos, others |
| Other names | Hydroxyurea (USAN US) |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a682004 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Metabolism | Liver (to CO2 and urea) |
| Elimination half-life | 2–4 hours |
| Excretion | Kidney and lungs |
| Identifiers | |
| |
JSmol) | |
| Melting point | 133 to 136 °C (271 to 277 °F) |
| |
| |
| (verify) | |
Hydroxycarbamide, also known as hydroxyurea, is a medication used in
Common
Hydroxycarbamide was approved for medical use in the United States in 1967.
Medical uses
Hydroxycarbamide is used for the following indications:
- Myeloproliferative disease (primarily essential thrombocythemia and polycythemia vera). It has been found to be superior to anagrelide for the control of ET.[5]
- Sickle-cell disease[6] (increases production of fetal hemoglobinthat then interferes with the hemoglobin polymerisation as well as by reducing white blood cells that contribute to the general inflammatory state in sickle cell patients.)
- Second line treatment for psoriasis[7] (slows down the rapid division of skin cells)
- Systemic mastocytosis[8]
- Chronic myelogenous leukemia (largely replaced by imatinib, but still in use for its cost-effectiveness)[9]
Side effects
Reported side effects are:
Due to its negative effect on the bone marrow, regular monitoring of the
Hydroxycarbamide has been used primarily for the treatment of myeloproliferative diseases, which has an inherent risk of transforming to acute myeloid leukemia. There has been a longstanding concern that hydroxycarbamide itself carries a leukemia risk, but large studies have shown that the risk is either absent or very small. Nevertheless, it has been a barrier for its wider use in patients with sickle-cell disease.[13]
Mechanism of action
Hydroxycarbamide decreases the production of deoxyribonucleotides[14] via inhibition of the enzyme ribonucleotide reductase by scavenging tyrosyl free radicals as they are involved in the reduction of nucleoside diphosphates (NDPs).[13]
In the treatment of
Natural occurrence
Hydroxyurea has been reported as endogenous in human blood plasma at concentrations of approximately 30 to 200 ng/ml.[16]
Chemistry
| Hazards | |
|---|---|
| Occupational safety and health (OHS/OSH): | |
Main hazards
|
Mutagen – Reproductive toxicity |
| GHS labelling: | |

| |
| Danger | |
| H340, H361 | |
| P201, P202, P281, P308+P313, P405, P501 | |
Hydroxyurea has been prepared in many different ways since its initial synthesis in 1869.
One common mechanism for synthesizing hydroxyurea is by the reaction of calcium cyanate with hydroxylamine nitrate in absolute ethanol and by the reaction of a cyanate salt and hydroxylamine hydrochloride in aqueous solution.[19] Hydroxyurea has also been prepared by converting a quaternary ammonium anion exchange resin from the chloride form to the cyanate form with sodium cyanate and reacting the resin in the cyanate form with hydroxylamine hydrochloride. This method of hydroxyurea synthesis was patented by Hussain et al. (2015).[20]
Pharmacology
Hydroxyurea is a monohydroxyl-substituted urea (hydroxycarbamate)
Biochemical research has explored its role as a
Hydroxyurea has many pharmacological applications under the Medical Subject Headings classification system:[21]
- Antineoplastic agents – Substances that inhibit or prevent the proliferation of neoplasms.
- Antisickling agents – Agents used to prevent or reverse the pathological events leading to sickling of erythrocytes in sickle cell conditions.
- Nucleic acid synthesis inhibitors – Compounds that inhibit cell production of DNA or RNA.
- Enzyme inhibitors – Compounds or agents that combine with an enzyme in such a manner as to prevent the normal substrate-enzyme combination and the catalytic reaction.
- Cytochrome P-450 CYP2D6 inhibitors – Agents that inhibit one of the most important enzymes involved in the metabolism of xenobiotics in the body, CYP2D6, a member of the cytochrome P450 mixed oxidase system.
Society and culture
Brand names
Brand names include: Hydrea, Litalir, Droxia, and Siklos.[citation needed]
References
- FDA. Retrieved 22 Oct 2023.
- ^ a b c d e f g h i "Hydroxyurea". The American Society of Health-System Pharmacists. Retrieved 8 December 2016.
- ^ a b "Hydrea 500 mg Hard Capsules – Summary of Product Characteristics (SPC) – (eMC)". www.medicines.org.uk. Archived from the original on 20 December 2016. Retrieved 14 December 2016.
- hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- PMID 16000354.
- PMID 18458272.
- from the original on 2009-07-03.
- PMID 19541349.
- PMID 15245690.
- PMID 17712860.
- ISBN 978-1-4144-0362-5.
- ^ "HYDREA" (PDF). Accessdata.fda.gov. US Food and Drug Administration.
- ^ PMID 18367739.
- ^ "hydroxyurea" at Dorland's Medical Dictionary
- PMID 12531879.
- PMID 19144580.
- ^ .
- PMID 21454878.
- ^ US 2705727, Graham PJ, "Synthesis of Ureas", assigned to E.I. du Pont de Nemours & Co., Wilmington, DE
- .
- ^ a b "Hydroxyurea". PubChem. U.S. National Library of Medicine. Archived from the original on 2017-05-18.
- S2CID 2675195.[permanent dead link]
- PMID 1641648.
