Immune system
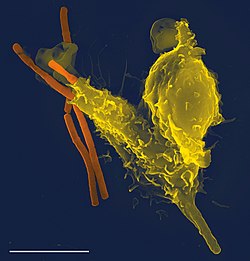
The immune system is a network of
Nearly all organisms have some kind of immune system.
Dysfunction of the immune system can cause
Layered defense
The immune system protects its host from infection with layered defenses of increasing specificity. Physical barriers prevent pathogens such as bacteria and viruses from entering the organism.[1] If a pathogen breaches these barriers, the innate immune system provides an immediate, but non-specific response. Innate immune systems are found in all animals.[2] If pathogens successfully evade the innate response, vertebrates possess a second layer of protection, the adaptive immune system, which is activated by the innate response.[3] Here, the immune system adapts its response during an infection to improve its recognition of the pathogen. This improved response is then retained after the pathogen has been eliminated, in the form of an immunological memory, and allows the adaptive immune system to mount faster and stronger attacks each time this pathogen is encountered.[4][5]
| Innate immune system | Adaptive immune system |
|---|---|
| Response is non-specific | Pathogen and antigen specific response |
| Exposure leads to immediate maximal response | Lag time between exposure and maximal response |
humoral components |
humoral components
|
| No immunological memory | Exposure leads to immunological memory |
| Found in nearly all forms of life | Found only in jawed vertebrates |
Both innate and adaptive immunity depend on the ability of the immune system to distinguish between self and non-self molecules. In immunology, self molecules are components of an organism's body that can be distinguished from foreign substances by the immune system.[6] Conversely, non-self molecules are those recognized as foreign molecules. One class of non-self molecules are called antigens (originally named for being antibody generators) and are defined as substances that bind to specific immune receptors and elicit an immune response.[7]
Surface barriers
Several barriers protect organisms from infection, including mechanical, chemical, and biological barriers. The waxy
Chemical barriers also protect against infection. The skin and respiratory tract secrete antimicrobial peptides such as the β-defensins.[10] Enzymes such as lysozyme and phospholipase A2 in saliva, tears, and breast milk are also antibacterials.[11][12] Vaginal secretions serve as a chemical barrier following menarche, when they become slightly acidic, while semen contains defensins and zinc to kill pathogens.[13][14] In the stomach, gastric acid serves as a chemical defense against ingested pathogens.[15]
Within the genitourinary and gastrointestinal tracts,
Innate immune system
Microorganisms or toxins that successfully enter an organism encounter the cells and mechanisms of the innate immune system. The innate response is usually triggered when microbes are identified by
Immune sensing
Cells in the innate immune system use
Recognition of extracellular or endosomal PAMPs is mediated by transmembrane proteins known as toll-like receptors (TLRs).[24] TLRs share a typical structural motif, the leucine rich repeats (LRRs), which give them a curved shape.[25] Toll-like receptors were first discovered in Drosophila and trigger the synthesis and secretion of cytokines and activation of other host defense programs that are necessary for both innate or adaptive immune responses. Ten toll-like receptors have been described in humans.[26]
Cells in the innate immune system have pattern recognition receptors, which detect infection or cell damage, inside. Three major classes of these "cytosolic" receptors are NOD–like receptors, RIG (retinoic acid-inducible gene)-like receptors, and cytosolic DNA sensors.[27]
Innate immune cells

Some
Neutrophils and macrophages are phagocytes that travel throughout the body in pursuit of invading pathogens.[34] Neutrophils are normally found in the bloodstream and are the most abundant type of phagocyte, representing 50% to 60% of total circulating leukocytes.[35] During the acute phase of inflammation, neutrophils migrate toward the site of inflammation in a process called chemotaxis, and are usually the first cells to arrive at the scene of infection. Macrophages are versatile cells that reside within tissues and produce an array of chemicals including enzymes, complement proteins, and cytokines, while they can also act as scavengers that rid the body of worn-out cells and other debris, and as antigen-presenting cells (APCs) that activate the adaptive immune system.[36]
Dendritic cells are phagocytes in tissues that are in contact with the external environment; therefore, they are located mainly in the skin, nose, lungs, stomach, and intestines.[37] They are named for their resemblance to neuronal dendrites, as both have many spine-like projections. Dendritic cells serve as a link between the bodily tissues and the innate and adaptive immune systems, as they present antigens to T cells, one of the key cell types of the adaptive immune system.[37]
Granulocytes are leukocytes that have granules in their cytoplasm. In this category are neutrophils, mast cells, basophils, and eosinophils. Mast cells reside in connective tissues and mucous membranes, and regulate the inflammatory response.[38] They are most often associated with allergy and anaphylaxis.[35] Basophils and eosinophils are related to neutrophils. They secrete chemical mediators that are involved in defending against parasites and play a role in allergic reactions, such as asthma.[39]
Innate lymphoid cells (ILCs) are a group of
Inflammation
Inflammation is one of the first responses of the immune system to infection.
Humoral defenses
The complement system is a
Adaptive immune system

The adaptive immune system evolved in early vertebrates and allows for a stronger immune response as well as immunological memory, where each pathogen is "remembered" by a signature antigen.[55] The adaptive immune response is antigen-specific and requires the recognition of specific "non-self" antigens during a process called antigen presentation. Antigen specificity allows for the generation of responses that are tailored to specific pathogens or pathogen-infected cells. The ability to mount these tailored responses is maintained in the body by "memory cells". Should a pathogen infect the body more than once, these specific memory cells are used to quickly eliminate it.[56]
Recognition of antigen
The cells of the adaptive immune system are special types of leukocytes, called lymphocytes.
Antigen presentation to T lymphocytes
Both B cells and T cells carry receptor molecules that recognize specific targets. T cells recognize a "non-self" target, such as a pathogen, only after antigens (small fragments of the pathogen) have been processed and presented in combination with a "self" receptor called a major histocompatibility complex (MHC) molecule.[62]
Cell mediated immunity
There are two major subtypes of T cells: the
Killer T cells
Helper T cells

Helper T cells regulate both the innate and adaptive immune responses and help determine which immune responses the body makes to a particular pathogen.[66][67] These cells have no cytotoxic activity and do not kill infected cells or clear pathogens directly. They instead control the immune response by directing other cells to perform these tasks.[68]
Helper T cells express T cell receptors that recognize antigen bound to Class II MHC molecules. The MHC:antigen complex is also recognized by the helper cell's CD4 co-receptor, which recruits molecules inside the T cell (such as Lck) that are responsible for the T cell's activation. Helper T cells have a weaker association with the MHC:antigen complex than observed for killer T cells, meaning many receptors (around 200–300) on the helper T cell must be bound by an MHC:antigen to activate the helper cell, while killer T cells can be activated by engagement of a single MHC:antigen molecule. Helper T cell activation also requires longer duration of engagement with an antigen-presenting cell.[69] The activation of a resting helper T cell causes it to release cytokines that influence the activity of many cell types. Cytokine signals produced by helper T cells enhance the microbicidal function of macrophages and the activity of killer T cells.[70] In addition, helper T cell activation causes an upregulation of molecules expressed on the T cell's surface, such as CD40 ligand (also called CD154), which provide extra stimulatory signals typically required to activate antibody-producing B cells.[71]
Gamma delta T cells
Humoral immune response
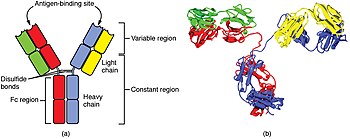
A
Newborn infants have no prior exposure to microbes and are particularly vulnerable to infection. Several layers of passive protection are provided by the mother. During pregnancy, a particular type of antibody, called
Immunological memory
When B cells and T cells are activated and begin to replicate, some of their offspring become long-lived memory cells. Throughout the lifetime of an animal, these memory cells remember each specific pathogen encountered and can mount a strong response if the pathogen is detected again. T-cells recognize pathogens by small protein-based infection signals, called antigens, that bind to directly to T-cell surface receptors.[80] B-cells use the protein, immunoglobulin, to recognize pathogens by their antigens. [81] This is "adaptive" because it occurs during the lifetime of an individual as an adaptation to infection with that pathogen and prepares the immune system for future challenges. Immunological memory can be in the form of either passive short-term memory or active long-term memory.[82]
Physiological regulation

The immune system is involved in many aspects of physiological regulation in the body. The immune system interacts intimately with other systems, such as the
Hormones
Vitamin D
Although cellular studies indicate that vitamin D has receptors and probable functions in the immune system, there is no
Sleep and rest
The immune system is affected by sleep and rest, and
In people with sleep deprivation, active immunizations may have a diminished effect and may result in lower antibody production, and a lower immune response, than would be noted in a well-rested individual.[99] Additionally, proteins such as NFIL3, which have been shown to be closely intertwined with both T-cell differentiation and circadian rhythms, can be affected through the disturbance of natural light and dark cycles through instances of sleep deprivation. These disruptions can lead to an increase in chronic conditions such as heart disease, chronic pain, and asthma.[100]
In addition to the negative consequences of sleep deprivation, sleep and the intertwined circadian system have been shown to have strong regulatory effects on immunological functions affecting both innate and adaptive immunity. First, during the early slow-wave-sleep stage, a sudden drop in blood levels of
During wake periods, differentiated effector cells, such as cytotoxic natural killer cells and cytotoxic T lymphocytes, peak to elicit an effective response against any intruding pathogens. Anti-inflammatory molecules, such as cortisol and catecholamines, also peak during awake active times. Inflammation would cause serious cognitive and physical impairments if it were to occur during wake times, and inflammation may occur during sleep times due to the presence of melatonin. Inflammation causes a great deal of oxidative stress and the presence of melatonin during sleep times could actively counteract free radical production during this time.[101][102]
Physical exercise
Physical exercise has a positive effect on the immune system and depending on the frequency and intensity, the pathogenic effects of diseases caused by bacteria and viruses are moderated.[103] Immediately after intense exercise there is a transient immunodepression, where the number of circulating lymphocytes decreases and antibody production declines. This may give rise to a window of opportunity for infection and reactivation of latent virus infections,[104] but the evidence is inconclusive.[105][106]
Changes at the cellular level

During exercise there is an increase in circulating
The number of circulating
Some monocytes leave the blood circulation and migrate to the muscles where they differentiate and become macrophages.[104] These cells differentiate into two types: proliferative macrophages, which are responsible for increasing the number of stem cells and restorative macrophages, which are involved their maturing to muscle cells.[107]
Repair and regeneration
The immune system, particularly the innate component, plays a decisive role in tissue repair after an insult. Key actors include macrophages and neutrophils, but other cellular actors, including γδ T cells, innate lymphoid cells (ILCs), and regulatory T cells (Tregs), are also important. The plasticity of immune cells and the balance between pro-inflammatory and anti-inflammatory signals are crucial aspects of efficient tissue repair. Immune components and pathways are involved in regeneration as well, for example in amphibians such as in axolotl limb regeneration. According to one hypothesis, organisms that can regenerate (e.g., axolotls) could be less immunocompetent than organisms that cannot regenerate.[108]
Disorders of human immunity
Failures of host defense occur and fall into three broad categories: immunodeficiencies,[109] autoimmunity,[110] and hypersensitivities.[111]
Immunodeficiencies
Autoimmunity
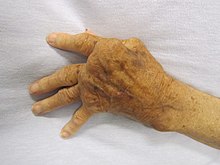
Overactive immune responses form the other end of immune dysfunction, particularly the
Hypersensitivity
Idiopathic inflammation
Inflammation is one of the first responses of the immune system to infection,[44] but it can appear without known cause.
Inflammation is produced by eicosanoids and cytokines, which are released by injured or infected cells. Eicosanoids include prostaglandins that produce fever and the dilation of blood vessels associated with inflammation, and leukotrienes that attract certain white blood cells (leukocytes).[45][46] Common cytokines include interleukins that are responsible for communication between white blood cells; chemokines that promote chemotaxis; and interferons that have anti-viral effects, such as shutting down protein synthesis in the host cell.[47] Growth factors and cytotoxic factors may also be released. These cytokines and other chemicals recruit immune cells to the site of infection and promote healing of any damaged tissue following the removal of pathogens.[48]
Manipulation in medicine
The immune response can be manipulated to suppress unwanted responses resulting from autoimmunity, allergy, and transplant rejection, and to stimulate protective responses against pathogens that largely elude the immune system (see immunization) or cancer.[125]
Immunosuppression
Immunostimulation
Claims made by marketers of various products and alternative health providers, such as chiropractors, homeopaths, and acupuncturists to be able to stimulate or "boost" the immune system generally lack meaningful explanation and evidence of effectiveness.[130]
Vaccination

Long-term active memory is acquired following infection by activation of B and T cells. Active immunity can also be generated artificially, through
Many vaccines are based on acellular components of micro-organisms, including harmless toxin components.[131] Since many antigens derived from acellular vaccines do not strongly induce the adaptive response, most bacterial vaccines are provided with additional adjuvants that activate the antigen-presenting cells of the innate immune system and maximize immunogenicity.[133]
Tumor immunology
Another important role of the immune system is to identify and eliminate

The main response of the immune system to tumors is to destroy the abnormal cells using killer T cells, sometimes with the assistance of helper T cells.[138][142] Tumor antigens are presented on MHC class I molecules in a similar way to viral antigens. This allows killer T cells to recognize the tumor cell as abnormal.[143] NK cells also kill tumorous cells in a similar way, especially if the tumor cells have fewer MHC class I molecules on their surface than normal; this is a common phenomenon with tumors.[144] Sometimes antibodies are generated against tumor cells allowing for their destruction by the complement system.[139]
Some tumors evade the immune system and go on to become cancers.
Paradoxically, macrophages can promote tumor growth
Predicting immunogenicity
Some drugs can cause a neutralizing immune response, meaning that the immune system produces
Evolution and other mechanisms
Evolution of the immune system
It is likely that a multicomponent, adaptive immune system arose with the first vertebrates, as invertebrates do not generate lymphocytes or an antibody-based humoral response.[157] Immune systems evolved in deuterostomes as shown in the cladogram.[157]
| Deuterostomes |
| ||||||
| innate immunity
|
Many species, however, use mechanisms that appear to be precursors of these aspects of vertebrate immunity. Immune systems appear even in the structurally simplest forms of life, with bacteria using a unique defense mechanism, called the
Pattern recognition receptors are proteins used by nearly all organisms to identify molecules associated with pathogens. Antimicrobial peptides called defensins are an evolutionarily conserved component of the innate immune response found in all animals and plants, and represent the main form of invertebrate systemic immunity.[157] The complement system and phagocytic cells are also used by most forms of invertebrate life. Ribonucleases and the RNA interference pathway are conserved across all eukaryotes, and are thought to play a role in the immune response to viruses.[164]
Unlike animals, plants lack phagocytic cells, but many plant immune responses involve systemic chemical signals that are sent through a plant.
Alternative adaptive immune system
Manipulation by pathogens
The success of any pathogen depends on its ability to elude host immune responses. Therefore, pathogens evolved several methods that allow them to successfully infect a host, while evading detection or destruction by the immune system.[169] Bacteria often overcome physical barriers by secreting enzymes that digest the barrier, for example, by using a type II secretion system.[170] Alternatively, using a type III secretion system, they may insert a hollow tube into the host cell, providing a direct route for proteins to move from the pathogen to the host. These proteins are often used to shut down host defenses.[171]
An evasion strategy used by several pathogens to avoid the innate immune system is to hide within the cells of their host (also called
The mechanisms used to evade the adaptive immune system are more complicated. The simplest approach is to rapidly change non-essential epitopes (amino acids and/or sugars) on the surface of the pathogen, while keeping essential epitopes concealed. This is called antigenic variation. An example is HIV, which mutates rapidly, so the proteins on its viral envelope that are essential for entry into its host target cell are constantly changing. These frequent changes in antigens may explain the failures of vaccines directed at this virus.[175] The parasite Trypanosoma brucei uses a similar strategy, constantly switching one type of surface protein for another, allowing it to stay one step ahead of the antibody response.[176] Masking antigens with host molecules is another common strategy for avoiding detection by the immune system. In HIV, the envelope that covers the virion is formed from the outermost membrane of the host cell; such "self-cloaked" viruses make it difficult for the immune system to identify them as "non-self" structures.[177]
History of immunology

These and other observations of acquired immunity were later exploited by
Immunology made a great advance towards the end of the 19th century, through rapid developments in the study of
See also
- Fc receptor
- Immunostimulator
- List of distinct cell types in the adult human body
- Neuroimmune system
- Original antigenic sin – when the immune system uses immunological memory upon encountering a slightly different pathogen
- Plant disease resistance
- Polyclonal response
- Tumor antigens
References
Citations
- ^ Sompayrac 2019, p. 1.
- ^ PMID 16261174.
- ^ Sompayrac 2019, p. 4.
- PMID 24148236.
- S2CID 20825732.
- ^ Sompayrac 2019, p. 11.
- ^ Sompayrac 2019, p. 146.
- ^ Alberts et al. 2002, sec. "Pathogens Cross Protective Barriers to Colonize the Host".
- PMID 11997295.
- PMID 16909918.
- PMID 11527949.
- PMID 4434640.
- PMID 54972.
- PMID 12628001.
- PMID 12870767.
- PMID 2109988.
- S2CID 4392839.
- S2CID 13615808.
- ^ a b Alberts et al. 2002, Chapter: "Innate Immunity".
- ^ Iriti 2019, p. xi.
- S2CID 42000671.
- S2CID 16916572.
- ^ Sompayrac 2019, p. 20.
- S2CID 20991617.
- PMID 21481769.
- PMID 29730580.
- PMID 21994762.
- ^ Sompayrac 2019, pp. 1–4.
- ^ Alberts et al. 2002, sec. "Phagocytic Cells Seek, Engulf, and Destroy Pathogens".
- PMID 3910340.
- PMID 8083520.
- PMID 11228151. Archived from the originalon 31 March 2020. Retrieved 6 November 2009.
- S2CID 28520695. Archived from the original(PDF) on 31 March 2020.
- PMID 14519390.
- ^ a b Stvrtinová, Jakubovský & Hulín 1995, Chapter: Inflammation and Fever.
- PMID 26162402.
- ^ PMID 11861614.
- ^ Krishnaswamy, Ajitawi & Chi 2006, pp. 13–34.
- S2CID 260317790.
- PMID 22224763.
- PMID 28078307.
- ^ Bertok & Chow 2005, p. 17.
- ^ Rajalingam 2012, Chapter: Overview of the killer cell immunoglobulin-like receptor system.
- ^ S2CID 9567407.
- ^ PMID 16887467.
- ^ PMID 17030228.
- ^ PMID 16212895.
- ^ PMID 16202600.
- S2CID 73464235.
- ^ S2CID 46096567.
- PMID 23672641.
- ^ Bertok & Chow 2005, pp. 112–113.
- PMID 8834497.
- S2CID 24505041. Archived from the original(PDF) on 2 March 2019.
- PMID 16551257.
- ^ Sompayrac 2019, p. 38.
- ^ a b c Janeway 2005.
- ^ PMID 15976493.
- PMID 19647627.
- ^ Janeway, Travers & Walport 2001, sec. 12-10.
- ^ Sompayrac 2019, pp. 5–6.
- ^ Sompayrac 2019, pp. 51–53.
- ^ Sompayrac 2019, pp. 7–8.
- PMID 10837060.
- ^ PMID 16928189.
- S2CID 4319699.
- PMID 17048705.
- ^ Sompayrac 2019, p. 8.
- PMID 12419850.
- ^ Alberts et al. 2002, Chapter. "Helper T Cells and Lymphocyte Activation".
- PMID 9597126.
- PMID 16417214.
- ^ "Understanding the Immune System: How it Works" (PDF). National Institute of Allergy and Infectious Diseases (NIAID). Archived from the original (PDF) on 3 January 2007. Retrieved 1 January 2007.
- ^ S2CID 6550357.
- PMID 8476565.
- ^ Murphy & Weaver 2016, Chapter 10: The Humoral Immune Response.
- S2CID 31099552. Archived from the original(PDF) on 30 January 2021.
- PMID 12850343.
- PMID 11023960.
- ^ Sauls RS, McCausland C, Taylor BN. Histology, T-Cell Lymphocyte. In: StatPearls. StatPearls Publishing; 2023. Accessed November 15, 2023. http://www.ncbi.nlm.nih.gov/books/NBK535433/
- ^ Althwaiqeb SA, Bordoni B. Histology, B Cell Lymphocyte. In: StatPearls. StatPearls Publishing; 2023. Accessed November 15, 2023. http://www.ncbi.nlm.nih.gov/books/NBK560905/
- ^ Sompayrac 2019, p. 98.
- PMID 8262005.
- PMID 3256322.
- S2CID 36504684.
- PMID 27153494.
- PMID 28092662.
- PMID 28542262.
- ^ Wira, Crane-Godreau & Grant 2004, Chapter: Endocrine regulation of the mucosal immune system in the female reproductive tract.
- PMID 10655462.
- S2CID 1021367.
- PMID 10857555.
- PMID 15798098.
- ^ "Vitamin D - Fact Sheet for Health Professionals". Office of Dietary Supplements, US National Institutes of Health. 17 August 2021. Retrieved 31 March 2022.
- S2CID 58721779.
- S2CID 29318345.
- S2CID 24508121.
- PMID 16337444.
- PMID 27077395.
- PMID 19075717.
- ^ PMID 22071480.
- ^ "Can Better Sleep Mean Catching fewer Colds?". Archived from the original on 9 May 2014. Retrieved 28 April 2014.
- PMID 32728975.
- ^ S2CID 3521624.
- PMID 29713319.
- PMID 32139352.
- S2CID 244369441.
- PMID 27521522.
- ^ Sompayrac 2019, pp. 120–24.
- ^ Sompayrac 2019, pp. 114–18.
- ^ Sompayrac 2019, pp. 111–14.
- PMID 17313487.
- ^ PMID 9250133.
- S2CID 12108587.
- ^ Reece 2011, p. 967.
- PMID 21479529.
- PMID 16322598.
- PMID 8987361.
- S2CID 32476323.
- ^
 This article incorporates text from this source, which is in the public domain: "Hashimoto's disease". Office on Women's Health, U.S. Department of Health and Human Services. 12 June 2017. Archived from the original on 28 July 2017. Retrieved 17 July 2017.
This article incorporates text from this source, which is in the public domain: "Hashimoto's disease". Office on Women's Health, U.S. Department of Health and Human Services. 12 June 2017. Archived from the original on 28 July 2017. Retrieved 17 July 2017.
- S2CID 37973054.
- S2CID 19872862.
- ^ "Handout on Health: Systemic Lupus Erythematosus". www.niams.nih.gov. February 2015. Archived from the original on 17 June 2016. Retrieved 12 June 2016.
- ^ a b c d Ghaffar A (2006). "Immunology – Chapter Seventeen: Hypersensitivity States". Microbiology and Immunology On-line. University of South Carolina School of Medicine. Retrieved 29 May 2016.
- ^ Sompayrac 2019, pp. 83–85.
- ^ Ciccone 2015, Chapter 37.
- ^ PMID 16039869.
- PMID 16436275.
- PMID 12835079.
- ^ Hall H (July–August 2020). "How You Can Really Boost Your Immune System". Skeptical Inquirer. Amherst, New York: Center for Inquiry. Archived from the original on 21 January 2021. Retrieved 21 January 2021.
- ^ a b Reece 2011, p. 965.
- ^ Death and DALY estimates for 2002 by cause for WHO Member States. Archived 21 October 2008 at the Wayback Machine World Health Organization. Retrieved on 1 January 2007.
- S2CID 21346647.
- ^ PMID 16417215.
- PMID 8642276.
- PMID 24559558.
- S2CID 196590144.
- ^ PMID 17145305.
- ^ PMID 14710950.
- S2CID 42681479.
- PMID 16946036.
- S2CID 25182066.
- ^ S2CID 5655726.
- PMID 16860661.
- ^ PMID 29208439.
- ^ S2CID 1838144.
- PMID 17017974.
- PMID 17695843. Archived from the original(PDF) on 16 July 2011.
- PMID 32555170.
- PMID 26325031.
- PMID 21487506.
- PMID 2411595.
- S2CID 18197810.
- PMID 15921533.
- PMID 15130835.
- S2CID 198982175.
- ^ PMID 19997068.
- PMID 8336674.
- S2CID 3888761.
- PMID 18703739.
- PMID 27672148.
- PMID 28187792.
- PMID 21680436.
- PMID 16732482.
- ^ a b Schneider D. "Innate Immunity – Lecture 4: Plant immune responses" (PDF). Stanford University Department of Microbiology and Immunology. Retrieved 1 January 2007.
- PMID 17108957.
- S2CID 4421274.
- PMID 16373579.
- ^ S2CID 15418509.
- PMID 16216510.
- PMID 11211218.
- PMID 9184008.
- S2CID 31788349.
- S2CID 10322322. Archived from the original(PDF) on 2 March 2019.
- PMID 16219699.
- PMID 16908087.
- PMID 15890896.
- ^ a b "The Nobel Prize in Physiology or Medicine 1908". The Nobel Prize. Retrieved 8 January 2007.
- PMID 9539938.
- .
- PMID 15530829.
- ^ Silverstein 1989, p. 6.
- ^ Silverstein 1989, p. 7.
- PMID 15812490.
- ^ The Nobel Prize in Physiology or Medicine 1905 Archived 10 December 2006 at the Wayback Machine Nobelprize.org Retrieved on 8 January 2009.
- ^ Major Walter Reed, Medical Corps, U.S. Army Walter Reed Army Medical Center. Retrieved on 8 January 2007.
- LCCN 68025143.
history of humoral immunity.
- ^ "Niels K. Jerne". The Nobel Prize. Retrieved 27 November 2020.
- PMC 1326409.
General bibliography
- Alberts B, Johnson A, Lewis J, Raff M, Roberts K, Walters P (2002). Molecular Biology of the Cell (Fourth ed.). New York and London: Garland Science. ISBN 978-0-8153-3218-3.
- Bertok L, Chow D (2005). Bertok L, Chow D (eds.). Natural Immunity. Vol. 5 (1st ed.). Elsevier Science. ISBN 978-0-44451-755-5.
- Iriti M (2019). Plant Innate Immunity 2.0. Basel: MDPI. OCLC 1105775088.
- Ciccone CD (2015). Pharmacology in Rehabilitation (Contemporary Perspectives in Rehabilitation) (5th ed.). F.A. Davis Company. ISBN 978-0-80364-029-0.
- Janeway CA, Travers P, Walport M (2001). Immunobiology (5th ed.). Garland Science.
- ISBN 0-443-07310-4.
- Krishnaswamy G, Ajitawi O, Chi DS (2006). "The human mast cell: an overview". Mast Cells. Methods in Molecular Biology. Vol. 315. pp. 13–34. PMID 16110146.
- Murphy K, Weaver C (2016). Immunobiology (9 ed.). Garland Science. ISBN 978-0-8153-4505-3.
- Rajalingam R (2012). "Overview of the Killer Cell Immunoglobulin-Like Receptor System". Immunogenetics. Methods in Molecular Biology. Vol. 882. pp. 391–414. PMID 22665247.
- Reece J (2011). Campbell biology. Frenchs Forest, N.S.W: Pearson Australia. OCLC 712136178.
- ISBN 978-0-08-092583-7.
- Sompayrac L (2019). How the immune system works. Hoboken, NJ: Wiley-Blackwell. OCLC 1083261548.
- Stvrtinová V, Jakubovský J, Hulín I (1995). Pathophysiology: Principles of Disease. Computing Centre, Slovak Academy of Sciences: Academic Electronic Press.
- Wira CR, Crane-Godreau M, Grant K (2004). Ogra PL, Mestecky J, Lamm ME, Strober W, McGhee JR, Bienenstock J (eds.). Mucosal Immunology. San Francisco: Elsevier. ISBN 0-12-491543-4.
Further reading
- Dettmer P (2021). Immune: A Journey into the Mysterious System that Keeps You Alive. Philip Laibacher (illustrations). New York: Random House. OCLC 1263845194. Archived from the original on 24 November 2021. Retrieved 4 January 2022. (The book's sourcesare only online.) A popular science explanation of the immune system.
