Intramuscular injection
| Intramuscular injection | |
|---|---|
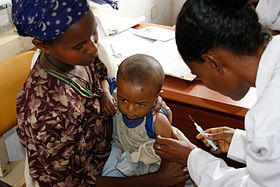 A healthcare worker preparing to administer a vaccine via intramuscular injection | |
| ICD-10-PCS | 3E023 |
| ICD-9-CM | 99.1 |
| MeSH | D007273 |
| CPT | 96372 |
Intramuscular injection, often abbreviated IM, is the
Common sites for intramuscular injections include the
Intramuscular injections commonly result in pain, redness, and swelling or inflammation around the injection site. These side effects are generally mild and last no more than a few days at most. Rarely, nerves or blood vessels around the injection site can be damaged, resulting in severe pain or paralysis. If proper technique is not followed, intramuscular injections can result in localized infections such as abscesses and gangrene. While historically aspiration, or pulling back on the syringe before injection, was recommended to prevent inadvertent administration into a vein, it is no longer recommended for most injection sites by some countries.
Uses
Intramuscular injection is commonly used for medication administration. Medication administered in the muscle is generally quickly absorbed in the bloodstream, and avoids the
Contraindications
Because an intramuscular injection can be used to administer many types of medications, specific contraindications depend in large part on the medication being administered.[8] Injections of medications are necessarily more invasive than other forms of administration such as by mouth or topical and require training to perform appropriately, without which complications can arise regardless of the medication being administered. For this reason, unless there are desired differences in rate of absorption, time to onset, or other pharmacokinetic parameters in the specific situation, a less invasive form of drug administration (usually by mouth) is preferred.[8]
Intramuscular injections are generally avoided in people with low platelet count or clotting problems, to prevent harm due to potential damage to blood vessels during the injection. They are also not recommended in people who are in hypovolemic shock, or have myopathy or muscle atrophy, as these conditions may alter the absorption of the medication.[5] The damage to the muscle caused by an intramuscular injections may interfere with the accuracy of certain cardiac tests for people with suspected myocardial infarction and for this reason other methods of administration are preferred in such instances.[5] In people with an active myocardial infarction, the decrease in circulation may result in slower absorption from an IM injection.[9]: 368–369 Specific sites of administration may also be contraindicated if the desired injection site has an infection, swelling, or inflammation.[9]: 368–369 Within a specific site of administration, the injection should not be given directly over irritation or redness, birthmarks or moles, or areas with scar tissue.[9]: 368–369
Risks and complications
As an injection necessitates piercing the skin, there is a risk of infection from
Site-specific complications
Injections into the deltoid site in the arm can result in unintentional damage to the radial and axillary nerves. In rare cases when not performed properly, the injection may result in shoulder dysfunction.[10] The most frequent complications of a deltoid injection include pain, redness, and inflammation around the injection site, which are almost always mild and last only a few days at most.[11]
The dorsogluteal site of injection is associated with a higher risk of skin and tissue trauma, muscle fibrosis or contracture, hematoma, nerve palsy, paralysis, and infections such as abscesses and gangrene.[12] Furthermore, injection in the gluteal muscle poses a risk for damage to the sciatic nerve, which may cause shooting pain or a sensation of burning. Sciatic nerve damage can also affect a person's ability to move their foot on the affected side, and other parts of the body controlled by the nerve. Damage to the sciatic nerve can be prevented by using the ventrogluteal site instead, and by selecting an appropriate size and length of needle for the injection.[13]
Technique


An intramuscular injection can be administered in multiple different muscles of the body. Common sites for intramuscular injection include:
The injection site is first cleaned using an antimicrobial and allowed to dry. The injection is performed in a quick, darting motion perpendicular to the skin, at an angle between 72 and 90 degrees. The practitioner will stabilize the needle with one hand while using their other hand to depress the plunger to slowly inject the medication – a rapid injection causes more discomfort. The needle is withdrawn at the same angle inserted. Gentle pressure may be applied with gauze if bleeding occurs.[16] Pressure or gentle massage of the muscle following injection may reduce the risk of pain.[17]
Aspiration
Aspirating for blood to rule out injecting into a blood vessel is not recommended by the US CDC, Public Health Agency of Canada, or Norway Institute of Public Health, as the injection sites do not contain large blood vessels and aspiration results in greater pain.[18][19][20] There is no evidence that aspiration is useful to increase safety of intramuscular injections when injecting in a site other than the dorsogluteal site.[6]
Aspiration was recommended by the Danish Health Authority for COVID-19 vaccines for a time to investigate the potential rare risk of blot clotting and bleeding, but it is no longer a recommendation.[21][22]
Z-track method
The Z-track method is a method of administering an IM injection that prevents the medication being tracked through the subcutaneous tissue, sealing the medication in the muscle, and minimizing irritation from the medication. Using the Z-track technique, the skin is pulled laterally, away from the injection site, before the injection; then the medication is injected, the needle is withdrawn, and the skin is released. This method can be used if the overlying tissue can be displaced.[23]
Injection sites
The deltoid muscle in the outer portion of the upper arm is used for injections of small volume, usually equal to or less than 2 mL. This includes most intramuscular vaccinations.
The ventrogluteal site on the hip is used for injections which require a larger volume to be administered, greater than 1 mL, and for medications which are known to be irritating, viscous, or oily. It is also used to administer
The
The dorsogluteal site of the buttock site is not routinely used due to its location near major blood vessels and nerves, as well as having inconsistent depth of adipose tissue.[25] Many injections in this site do not penetrate deep enough under the skin to be correctly administered in the muscle.[12][26] While current evidence-based practice recommends against using this site, many healthcare providers still use this site, often due to a lack of knowledge about alternative sites for injection.[27] This site is located by dividing the buttock into four using a cross shape, and administering the injection in the upper outer quadrant. This is the only intramuscular injection site for which aspiration is recommended of the syringe before injection, due to higher likelihood of accidental
Special populations
Some populations require a different injection site, needle length, or technique. In very young or weak elderly patients, a normal-length needle may be too long to inject properly. In these patients, a shorter needle is indicated to avoid injecting too deeply.[28] It is also recommended to consider using the anterolateral thigh as an injection site in infants under one year old.[28]
To help infants and children cooperate with injection administration, the Advisory Committee on Immunization Practices in the United States recommends using distractions, giving something sweet, and rocking the baby side to side. In people who are overweight, a 1.5-inch needle may be used to ensure the injection is given below the subcutaneous layer of skin, while a 5⁄8-inch needle may be used for people who weigh under 60 kilograms (130 lb). In any case, the skin does not need to be pinched up before injecting when the appropriate length needle is used.[29]
History
Injections into muscular tissue may have taken place as early as the year 500 AD. Beginning in the late 1800s, the procedure began to be described in more detail and techniques began to be developed by physicians. In the early days of intramuscular injections, the procedure was performed almost exclusively by physicians.
Intramuscular injections began to be used for administration of vaccines for
Veterinary medicine
In animals common sites for intramuscular injection include the
See also
- Subcutaneous injection
- Intradermal injection
- Intravenous injection
References
- ISBN 978-0-323-28745-6, retrieved 2020-11-25
- ISBN 978-1-58528-387-3.
- ISBN 978-1-4614-0554-2.
- PMID 15136657.
- ^ PMID 32310581.
- ^ PMID 25871949.
- ^ Mylan Specialty L.P. "EPIPEN®- epinephrine injection, EPIPEN Jr®- epinephrine injection" (PDF). FDA Product Label. Archived (PDF) from the original on 1 February 2014. Retrieved 22 January 2014.
- ^ PMID 12173166.
- ^ ISBN 978-1-4698-5303-1.
- PMID 25868476.
- ^ PMID 28774564.
- ^ a b c d e f g h The Joanna Briggs Institute. Recommended Practice. Injection: Intramuscular. The Joanna Briggs Institute EBP Database, from the JBI@Ovid database, published 2019; JBI2138. Accessed on 12 September 2020.
- PMID 24920643.
- ISBN 978-0-12-801238-3, retrieved 2020-11-25
- ^ ISBN 978-0-7817-9383-4.
- ^ ISBN 978-1-9751-2136-5.
- ^ S2CID 201786789.
- ^ JoEllen Wolicki, Elaine Miller (25 September 2019). "Vaccine Administration". The Pinkbook. CDC. Retrieved 12 September 2020.
Aspiration is not recommended before administering a vaccine.
- ^ "Vaccine administration practices: Canadian Immunization Guide". Public Health Agency of Canada. 2020-12-02. Retrieved 2021-05-25.
Aspiration before injection of vaccine is not recommended, as there are no large blood vessels at the recommended immunization sites and not aspirating before injection has been demonstrated to reduce pain.
- ^ "Praktisk info om vaksinasjon". Folkehelseinstituttet (in Norwegian). 9 April 2008. Retrieved 2021-05-25.
However, it is not recommended to aspirate before intramuscular and subcutaneous vaccine injection provided that the vaccine is placed in the appropriate place … does not involve the risk of injecting intravenously because there are no large blood vessels in these sites. Aspiration can cause the vaccination to be more painful because it takes longer to give the vaccine
- ^ "Covid-19 vacciner skal gives med aspiration før injektion". Politik og nyheder, DSR (in Danish). 2021-03-20. Archived from the original on 2021-03-22. Retrieved 2021-05-25.
The Danish Health and Medicines Authority's guidelines have long recommended this, and now the Statens Serum Institut is following suit.
- ^ name. "Intramuskulær injektion på børn og voksne". Statens Serum Institut (in Danish). Retrieved 2023-10-04.
It has previously been recommended to aspirate before injection with Covid-19 vaccines in relation to investigation of a possible connection between injection with Vaxzevria® and the occurrence of rare and serious side effects. However, this is no longer a recommendation and Covid-19 vaccines can be injected without prior aspiration.
- ^ Doyle GR, McCutcheon JA (2015). "7.4 Intramuscular Injections". Clinical Procedures for Safer Patient Care. BCcampus.
- ^ "Epinephrine Injection". MedlinePlus. Last revised 03/15/2017
- PMID 20107407.
- PMID 3641525.
- PMID 20948472.
- ^ PMID 30091147.
- ^ Centers for Disease Control. 21 June 2019. Retrieved 12 September 2020.
- PMID 22617834.
- PMID 28388718.
- ^ "SOP: Injections in Dogs and Cats" (PDF). Virginia Tech. Dec 12, 2017.
External links
- Injections,+Intramuscular at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
- Prevention and Control of Influenza, Recommendations of ACIP









