Gastrointestinal physiology
Gastrointestinal physiology is the branch of
Motility
The gastrointestinal tract generates
Motility may be overactive (hypermotility), leading to diarrhea or vomiting, or underactive (hypomotility), leading to constipation or vomiting; either may cause abdominal pain.[3]
Stimulation
The stimulation for these contractions likely originates in modified smooth muscle cells called
Contraction patterns
The peristalsis and segmentation, detailed below and pendular movement are famous examples of distinct patterns of GI contraction.[5] Occurring between meals, the migrating motor complex is a series of peristaltic wave cycles in distinct phases starting with relaxation, followed by an increasing level of activity to a peak level of peristaltic activity lasting for 5–15 minutes.[6] This cycle repeats every 1.5–2 hours but is interrupted by food ingestion. The role of this process is likely to clean excess bacteria and food from the digestive system.[7]
Peristalsis
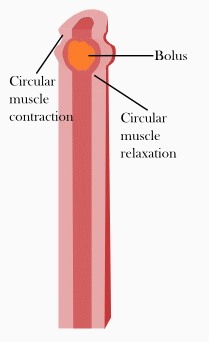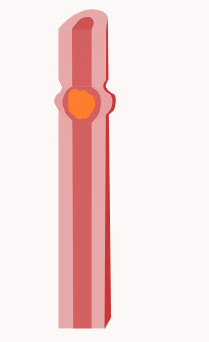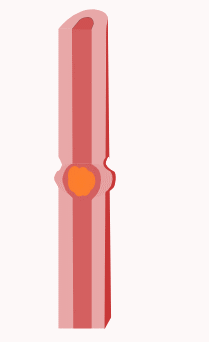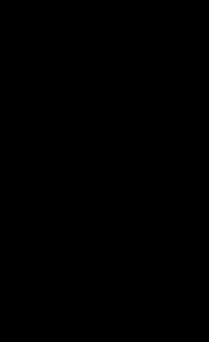
Peristalsis is one of the patterns that occur during and shortly after a meal. The contractions occur in wave patterns traveling down short lengths of the GI tract from one section to the next. The contractions occur directly behind the bolus of food that is in the system, forcing it toward the anus into the next relaxed section of smooth muscle. This relaxed section then contracts, generating smooth forward movement of the bolus at between 2–25 cm per second. This contraction pattern depends upon hormones, paracrine signals, and the autonomic nervous system for proper regulation.[4]
Segmentation
Segmentation contractions also occur during and shortly after a meal within short lengths in segmented or random patterns along the intestine. This process is carried out by the longitudinal muscles relaxing while circular muscles contract at alternating sections thereby mixing the food. This mixing allows food and digestive enzymes to maintain a uniform composition, as well as to ensure contact with the epithelium for proper absorption.[4]
Secretion
Every day, seven liters of fluid are secreted by the digestive system. This fluid is composed of four primary components: ions, digestive enzymes, mucus, and bile. About half of these fluids are secreted by the salivary glands, pancreas, and liver, which compose the accessory organs and glands of the digestive system. The rest of the fluid is secreted by the GI epithelial cells.
Ions
The largest component of secreted fluids is ions and water, which are first secreted and then reabsorbed along the tract. The ions secreted primarily consist of H+, K+, Cl−, HCO3− and Na+. Water follows the movement of these ions. The GI tract accomplishes this ion pumping using a system of proteins that are capable of
H+ and Cl− are secreted by the
HCO3− secretion occurs to neutralize the acid secretions that make their way into the
Digestive enzymes
The second vital secretion of the GI tract is that of digestive enzymes that are secreted in the mouth, stomach and intestines. Some of these enzymes are secreted by accessory digestive organs, while others are secreted by the epithelial cells of the stomach and intestine. While some of these enzymes remain embedded in the wall of the GI tract, others are secreted in an inactive
Mucus
Bile
Bile is secreted into the duodenum of the small intestine via the
Regulation
The digestive system has a complex system of motility and secretion regulation which is vital for proper function. This task is accomplished via a system of long reflexes from the
Long reflexes
Long reflexes to the digestive system involve a sensory neuron sending information to the brain, which integrates the signal and then sends messages to the digestive system. While in some situations, the sensory information comes from the GI tract itself; in others, information is received from sources other than the GI tract. When the latter situation occurs, these reflexes are called feedforward reflexes. This type of reflex includes reactions to food or danger triggering effects in the GI tract. Emotional responses can also trigger GI response such as the butterflies in the stomach feeling when nervous. The feedforward and emotional reflexes of the GI tract are considered
Short reflexes
Control of the digestive system is also maintained by ENS, which can be thought of as a digestive brain that can help to regulate motility, secretion and growth. Sensory information from the digestive system can be received, integrated and acted upon by the enteric system alone. When this occurs, the reflex is called a short reflex.[4] Although this may be the case in several situations, the ENS can also work in conjunction with the CNS; vagal afferents from the viscera are received by the medulla, efferents are affected by the vagus nerve. When this occurs, the reflex is called vagovagal reflex. The myenteric plexus and submucosal plexus are both located in the gut wall and receive sensory signals from the lumen of the gut or the CNS.[6]
Gastrointestinal peptides
For further information see Gastrointestinal hormone
GI peptides are signal molecules that are released into the blood by the GI cells themselves. They act on a variety of tissues including the brain, digestive accessory organs, and the GI tract. The effects range from excitatory or inhibitory effects on motility and secretion to feelings of satiety or hunger when acting on the brain. These hormones fall into three major categories, the gastrin and secretin families, with the third composed of all the other hormones unlike those in the other two families. Further information on the GI peptides is summarized in the table below.[8]
| Secreted by | Target | Effects on endocrine secretion | Effects on exocrine secretion | Effects on motility | Other effects | Stimulus for release | |
|---|---|---|---|---|---|---|---|
| Gastrin | G Cells in stomach | ECL cells; parietal cells | None | Increases acid secretion, increases mucus growth | Stimulates gastric contraction | None | Peptides and amino acids in lumen; gastrin releasing peptide and ACh in nervous reflexes |
| Cholecystokinin (CCK) | Endocrine I cells of the small intestine; neurons of the brain and gut | Gallbladder, pancreas, gastric smooth muscle | None | Stimulates pancreatic enzyme and HCO3- secretion | Stimulates gallbladder contraction; inhibits stomach emptying | Satiety | Fatty acids and some amino acids |
| Secretin | Endocrine S cells of the small intestine | Pancreas, stomach | None | Stimulates pancreatic and hepatic HCO3- secretion; inhibits acid secretion; pancreatic growth | Stimulates gallbladder contraction; Inhibits stomach emptying | None | Acid in small intestine |
| Gastric inhibitory Peptide | Endocrine K cells of the small intestine | Beta cells of the pancreas | Stimulates pancreatic insulin release | Inhibits acid secretion | None | Satiety and lipid metabolism | Glucose, fatty acid, and amino acids in small intestine |
| Motilin | Endocrine M cells in small intestine | Smooth muscle of stomach and duodenum | None | None | Stimulates migrating motor complex | Action in brain, stimulates migratory motor complex | Fasting: cyclic release every 1.5–2 hours by neural stimulus |
| Glucagon-like peptide-1 | Endocrine cells in small intestine | Endocrine pancreas | Stimulates insulin release; inhibits glucagon release | Possibly inhibits acid secretion | Slows gastric emptying | Satiety; various CNS functions | Mixed meals of fats and carbohydrates |
Digestion
- carbohydrates (monosaccharide, disaccharide)
- proteins
- lipids
Splanchnic circulation
External links
- Notes at University of Bristol
- Digestive+Physiology at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
Notes and references
- ISBN 9783319071640.
- ^ "Human Physiology/The gastrointestinal system - Wikibooks, open books for an open world". en.wikibooks.org. Retrieved 2016-09-05.
- PMID 27144617.
- ^ ISBN 0-8053-6851-5.
- PMID 10446098.
- ^ a b c d Bowen DVM PhD, R (July 5, 2006). "Pathophysiology of the Digestive System". Retrieved 2008-03-19.
- ^ Nosek PhD, T.M. "Essentials Of Human Physiology". Archived from the original on 2008-04-01. Retrieved 2008-03-19.
- ^ "Overview of Gastrointestinal Hormones". www.vivo.colostate.edu. Archived from the original on 2018-08-14. Retrieved 2016-09-16.
