Intestinal parasite infection
This article needs more primary sources. (December 2017) |  |
| Intestinal parasite | |
|---|---|
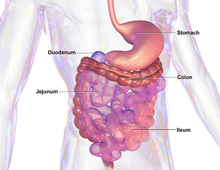 | |
| Human gastro-intestinal system | |
| Specialty | Infectious disease |
An intestinal parasite infection is a condition in which a
Routes of exposure and infection include ingestion of undercooked meat, drinking infected water,
Some types of
Signs and symptoms
Signs and symptoms depend on the type of infection. Intestinal parasites produce a variety of symptoms in those affected, most of which manifest themselves in gastrointestinal complications and general weakness.
Cause
The prevalence of intestinal parasites is the highest among children that are living in the poorest communities in developing nations.[1] The most common causes of intestinal parasites are through consumption of contaminated water, infected soil, inadequate sanitation and hygiene, and improper hygiene.[3] Specifically, lack of access to facilities for safe disposal of human waste can result in intestinal parasites and disease. Poor hygiene habits or lacking available hygiene resources, such as hand washing facilities, also negatively impact rates of disease.[4] Parasitic contamination can also occur from eating raw produce,[5] soil-eating behaviour,[6] and low availability of safe drinking water.[6]
Parasites can get into the intestines by going through the mouth from uncooked or unwashed food, contaminated water or hands, or by skin contact with larva infected soil; they can also be transferred by the sexual act of anilingus in some cases. When the organisms are swallowed, they move into the intestines, where they can reproduce and cause symptoms. Children are particularly susceptible if they are not thoroughly cleaned after coming into contact with infected soil that is present in environments that they may frequently visit such as sandboxes and school playgrounds. People in developing countries are also at particular risk due to drinking water from sources that may be contaminated with parasites that colonize the gastrointestinal tract.[citation needed]
Diagnosis

Due to the wide variety of intestinal parasites, a description of the symptoms rarely is sufficient for diagnosis. Instead, medical personnel use one of two common tests: they search stool samples for the parasites, or apply an adhesive to the anus to search for eggs.
Types
Major groups of parasites include
Prevention
Good hygiene is necessary to avoid reinfection.
Intestinal parasite prevention methods are not isolated to specific geographical areas; however, many of the research-based interventions have primarily taken place in underdeveloped countries and regions, where sanitation is a large concern for spreading disease.[citation needed]Current best practice behaviors that prevent intestinal parasites include: using proper hand washing practices, using correctly-built latrines with ample ventilation, having a piped water source, and wearing shoes.[8][9] Currently, in some parts of Ethiopia where disease prevalence is high, up to 80% of people in a population lack access to washing facilities. While this is high, 93% did have access to a latrine, but only 29.2% of those latrines had proper construction to decrease parasitic infections.[9] Behavioral interventions have focused on promoting washing, sometimes with soap, in context of education at schools and child care facilities.[10] In recent studies, the best interventions follow a multidisciplinary approach by:
- Increasing environmental sanitation to promote hand washing and shoe wearing habits
- Educating children at young ages at school and at home
Specific evidence-based interventions that may lower disease prevalence include:
- Interventions at schools, focusing on the construction of pit latrines (ventilated and improved), providing clean drinking water and educating the students about hygiene[11]
- The SAFE (surgery, antibiotics, facial cleanliness, environmental sanitation) strategy to address trachoma, primarily the facial cleanliness and the environmental sanitation components[12]
- Hand-washing with soap at critical times and nail clipping to decrease reinfection rates, although further research is needed to develop and implement similar interventions at scale[citation needed]
- Programs combining anthelmintic drug administration with interventions to increase environmental sanitation (such as decreasing fecal contamination)[13]
Treatment
Drugs are frequently used to kill parasites in the host. In earlier times, turpentine was often used for this, but modern drugs do not poison intestinal worms directly. Rather, anthelmintic drugs now inhibit an enzyme that is necessary for the worm to make the substance that prevents the worm from being digested.[citation needed]
For example,
References
- ^ a b "Intestinal worms". World Health Organization. Archived from the original on October 18, 2014. Retrieved 2017-03-28.
- PMID 22185945.
- PMID 22291577.
- PMID 21125019.
- PMID 28264707.
- ^ PMID 26248869.
- PMID 10501641.
- PMID 23560704.
- ^ PMID 24528627.
- PMID 26346329.
- PMID 25859318.
- PMID 23755308.
- PMID 25308524.
- ^ "WHO Model Prescribing Information: Drugs Used in Parasitic Diseases - Second Edition: Helminths: Cestode (tapeworm) infection". apps.who.int. Archived from the original on July 15, 2010. Retrieved 9 December 2017.
External links
- Feary, J.; Britton, J.; Leonardi-Bee, J. (April 2011). "Atopy and current intestinal parasite infection: a systematic review and meta-analysis". Allergy. 66 (4): 569–578. S2CID 205405288.
