Ketogenic diet
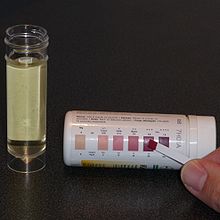
The ketogenic diet is a high-fat, adequate-protein, low-carbohydrate dietary therapy that in conventional medicine is used mainly to treat hard-to-control (refractory) epilepsy in children. The diet forces the body to burn fats rather than carbohydrates.
Normally, carbohydrates in food are converted into
The original therapeutic diet for
In 1994, Hollywood producer
Possible therapeutic uses for the ketogenic diet have been studied for many additional
Epilepsy
History
The ketogenic diet is a
Fasting

Physicians of ancient Greece treated diseases, including epilepsy, by altering their patients' diet. An early treatise in the Hippocratic Corpus, On the Sacred Disease, covers the disease; it dates from c. 400 BC. Its author argued against the prevailing view that epilepsy was supernatural in origin and cure, and proposed that dietary therapy had a rational and physical basis.[Note 3] In the same collection, the author of Epidemics describes the case of a man whose epilepsy is cured as quickly as it had appeared, through complete abstinence of food and drink.[Note 4] The royal physician Erasistratus declared, "One inclining to epilepsy should be made to fast without mercy and be put on short rations."[Note 5] Galen believed an "attenuating diet"[Note 6] might afford a cure in mild cases and be helpful in others.[11]
The first modern study of fasting as a treatment for epilepsy was in France in 1911.[12] Twenty epilepsy patients of all ages were "detoxified" by consuming a low-calorie vegetarian diet, combined with periods of fasting and purging. Two benefited enormously, but most failed to maintain compliance with the imposed restrictions. The diet improved the patients' mental capabilities, in contrast to their medication, potassium bromide, which dulled the mind.[13]
Around this time,
Conklin's fasting therapy was adopted by
Diet
In 1921,
Wilder's colleague, paediatrician Mynie Gustav Peterman, later formulated the classic diet, with a ratio of one gram of protein per kilogram of body weight in children, 10–15 g of carbohydrate per day, and the remainder of calories from fat. Peterman's work in the 1920s established the techniques for induction and maintenance of the diet. Peterman documented positive effects (improved alertness, behaviour, and sleep) and adverse effects (nausea and vomiting due to excess ketosis). The diet proved to be very successful in children: Peterman reported in 1925 that 95% of 37 young patients had improved seizure control on the diet and 60% became seizure-free. By 1930, the diet had also been studied in 100 teenagers and adults. Clifford Joseph Barborka Sr., also from the Mayo Clinic, reported that 56% of those older patients improved on the diet and 12% became seizure-free. Although the adult results are similar to modern studies of children, they did not compare as well to contemporary studies. Barborka concluded that adults were least likely to benefit from the diet, and the use of the ketogenic diet in adults was not studied again until 1999.[10][14]
Anticonvulsants and decline
During the 1920s and 1930s, when the only anticonvulsant drugs were the sedative
MCT diet

In the 1960s, medium-chain triglycerides (MCTs) were found to produce more ketone bodies per unit of energy than normal dietary fats (which are mostly long-chain triglycerides).[15] MCTs are more efficiently absorbed and are rapidly transported to the liver via the hepatic portal system rather than the lymphatic system.[16] The severe carbohydrate restrictions of the classic ketogenic diet made it difficult for parents to produce palatable meals that their children would tolerate. In 1971, Peter Huttenlocher devised a ketogenic diet where about 60% of the calories came from the MCT oil, and this allowed more protein and up to three times as much carbohydrate as the classic ketogenic diet. The oil was mixed with at least twice its volume of skimmed milk, chilled, and sipped during the meal or incorporated into food. He tested it on 12 children and adolescents with intractable seizures. Most children improved in both seizure control and alertness, results that were similar to the classic ketogenic diet. Gastrointestinal upset was a problem, which led one patient to abandon the diet, but meals were easier to prepare and better accepted by the children.[15] The MCT diet replaced the classic ketogenic diet in many hospitals, though some devised diets that were a combination of the two.[10]
Revival
The ketogenic diet achieved national media exposure in the US in October 1994, when NBC's
By 2007, the ketogenic diet was available from around 75 centres in 45 countries, and less restrictive variants, such as the modified Atkins diet, were in use, particularly among older children and adults. The ketogenic diet was also under investigation for the treatment of a wide variety of disorders other than epilepsy.[1]
Efficacy
The ketogenic diet reduces seizure frequency by more than 50% in half of the patients who try it and by more than 90% in a third of patients.[18] Three-quarters of children who respond do so within two weeks, though experts recommend a trial of at least three months before assuming it has been ineffective.[19] Children with refractory epilepsy are more likely to benefit from the ketogenic diet than from trying another anticonvulsant drug.[1] Adolescents and adults may also benefit from the diet, though compliance with oral diet (vs tube fed) remains a problem.[20]
Trial design
Early studies reported high success rates; in one study in 1925, 60% of patients became seizure-free, and another 35% of patients had a 50% reduction in seizure frequency. These studies generally examined a
Another difference between older and newer studies is that the type of patients treated with the ketogenic diet has changed over time. When first developed and used, the ketogenic diet was not a treatment of last resort; in contrast, the children in modern studies have already tried and failed a number of anticonvulsant drugs, so may be assumed to have more difficult-to-treat epilepsy. Early and modern studies also differ because the treatment
Outcomes
A study with an intent-to-treat prospective design was published in 1998 by a team from the
It is possible to combine the results of several small studies to produce evidence that is stronger than that available from each study alone—a statistical method known as meta-analysis. One of four such analyses, conducted in 2006, looked at 19 studies on a total of 1,084 patients.[25] It concluded that a third achieved an excellent reduction in seizure frequency and half the patients achieved a good reduction.[18]
A Cochrane systematic review in 2018 found and analysed eleven randomized controlled trials of ketogenic diet in people with epilepsy for whom drugs failed to control their seizures.[2] Six of the trials compared a group assigned to a ketogenic diet with a group not assigned to one. The other trials compared types of diets or ways of introducing them to make them more tolerable.[2] In the largest trial of the ketogenic diet with a non-diet control,[16] nearly 38% of the children and young people had half or fewer seizures with the diet compared 6% with the group not assigned to the diet. Two large trials of the Modified Atkins Diet compared to a non-diet control had similar results, with over 50% of children having half or fewer seizures with the diet compared to around 10% in the control group.[2]
A systematic review in 2018 looked at 16 studies on the ketogenic diet in adults. It concluded that the treatment was becoming more popular for that group of patients, that the efficacy in adults was similar to children, the side effects relatively mild. However, many patients gave up the diet, for various reasons, and the quality of evidence was inferior to studies on children. Health issues include high levels of low-density lipoprotein, high total cholesterol, and weight loss.[26]
Indications and contraindications
The ketogenic diet is indicated as an adjunctive (additional) treatment in children and young people with
Advocates for the diet recommend that it be seriously considered after two medications have failed, as the chance of other drugs succeeding is only 10%.
A survey in 2005 of 88 paediatric neurologists in the US found that 36% regularly prescribed the diet after three or more drugs had failed, 24% occasionally prescribed the diet as a last resort, 24% had only prescribed the diet in a few rare cases, and 16% had never prescribed the diet. Several possible explanations exist for this gap between evidence and clinical practice.[36] One major factor may be the lack of adequately trained dietitians who are needed to administer a ketogenic diet programme.[33]
Because the ketogenic diet alters the body's metabolism, it is a
Interactions
The ketogenic diet is usually initiated in combination with the patient's existing anticonvulsant regimen, though patients may be weaned off anticonvulsants if the diet is successful. Some evidence of synergistic benefits is seen when the diet is combined with the vagus nerve stimulator or with the drug zonisamide, and that the diet may be less successful in children receiving phenobarbital.[18]
Adverse effects
The ketogenic diet is not considered a
Long-term use of the ketogenic diet in children increases the risk of slowed or stunted growth, bone fractures, and
- Excess calcium in the urine (hypercalciuria) occurs due to increased bone demineralisation with acidosis. Bones are mainly composed of calcium phosphate. The phosphate reacts with the acid, and the calcium is excreted by the kidneys.[41]
- Hypocitraturia: the urine has an abnormally low concentration of citrate, which normally helps to dissolve free calcium.[41]
- The urine has a low pH, which stops uric acid from dissolving, leading to crystals that act as a nidus for calcium stone formation.[41]
- Many institutions traditionally restricted the water intake of patients on the diet to 80% of normal daily needs;[41] this practice is no longer encouraged.[18]
In adolescent and adults, common side effects reported include weight loss, constipation, dyslipidemia, and in women, dysmenorrhea.[42]
Implementation
The ketogenic diet is a
Implementing the diet can present difficulties for caregivers and the patient due to the time commitment involved in measuring and planning meals. Since any unplanned eating can potentially break the nutritional balance required, some people find the discipline needed to maintain the diet challenging and unpleasant. Some people terminate the diet or switch to a less demanding diet, like the modified Atkins diet or the low-glycaemic index treatment diet, because they find the difficulties too great.[43]
Initiation
The Johns Hopkins Hospital protocol for initiating the classic ketogenic diet has been widely adopted.[44] It involves a consultation with the patient and their caregivers and, later, a short hospital admission.[21] Because of the risk of complications during ketogenic diet initiation, most centres begin the diet under close medical supervision in the hospital.[19]
At the initial consultation, patients are
The day before admission to hospital, the proportion of carbohydrate in the diet may be decreased and the patient begins fasting after his or her evening meal.[21] On admission, only calorie- and caffeine-free fluids[39] are allowed until dinner, which consists of "eggnog"[Note 9] restricted to one-third of the typical calories for a meal. The following breakfast and lunch are similar, and on the second day, the "eggnog" dinner is increased to two-thirds of a typical meal's caloric content. By the third day, dinner contains the full calorie quota and is a standard ketogenic meal (not "eggnog"). After a ketogenic breakfast on the fourth day, the patient is discharged. Where possible, the patient's current medicines are changed to carbohydrate-free formulations.[21]
When in the hospital,
Variations on the Johns Hopkins protocol are common. The initiation can be performed using
For patients who benefit, half achieve a seizure reduction within five days (if the diet starts with an initial fast of one to two days), three-quarters achieve a reduction within two weeks, and 90% achieve a reduction within 23 days. If the diet does not begin with a fast, the time for half of the patients to achieve an improvement is longer (two weeks), but the long-term seizure reduction rates are unaffected.[45] Parents are encouraged to persist with the diet for at least three months before any final consideration is made regarding efficacy.[19]
Maintenance
After initiation, the child regularly visits the hospital outpatient clinic where they are seen by the dietitian and neurologist, and various tests and examinations are performed. These are held every three months for the first year and then every six months thereafter. Infants under one year old are seen more frequently, with the initial visit held after just two to four weeks.
A short-lived increase in seizure frequency may occur during illness or if ketone levels fluctuate. The diet may be modified if seizure frequency remains high, or the child is losing weight.[21] Loss of seizure-control may come from unexpected sources. Even "sugar-free" food can contain carbohydrates such as maltodextrin, sorbitol, starch, and fructose. The sorbitol content of suntan lotion and other skincare products may be high enough for some to be absorbed through the skin and thus negate ketosis.[33]
Discontinuation
About 20% of children on the ketogenic diet achieve freedom from seizures, and many are able to reduce the use of anticonvulsant drugs or eliminate them altogether.[18] Commonly, at around two years on the diet, or after six months of being seizure-free, the diet may be gradually discontinued over two or three months. This is done by lowering the ketogenic ratio until urinary ketosis is no longer detected, and then lifting all calorie restrictions.[48] This timing and method of discontinuation mimics that of anticonvulsant drug therapy in children, where the child has become seizure-free. When the diet is required to treat certain metabolic diseases, the duration will be longer. The total diet duration is up to the treating ketogenic diet team and parents; durations up to 12 years have been studied and found beneficial.[46]
Children who discontinue the diet after achieving seizure freedom have about a 20% risk of seizures returning. The length of time until recurrence is highly variable, but averages two years. This risk of recurrence compares with 10% for resective surgery (where part of the brain is removed) and 30–50% for anticonvulsant therapy. Of those who have a recurrence, just over half can regain freedom from seizures either with anticonvulsants or by returning to the ketogenic diet. Recurrence is more likely if, despite seizure freedom, an
Variants
Classic

The ketogenic diet is calculated by a dietitian for each child. Age, weight, activity levels, culture, and food preferences all affect the meal plan. First, the energy requirements are set at 80–90% of the recommended daily amounts (RDA) for the child's age (the high-fat diet requires less energy to process than a typical high-carbohydrate diet). Highly active children or those with muscle spasticity require more food energy than this; immobile children require less. The ketogenic ratio of the diet compares the weight of fat to the combined weight of carbohydrate and protein. This is typically 4:1, but children who are younger than 18 months, older than 12 years, or who are obese may be started on a 3:1 ratio. Fat is energy-rich, with 9 kcal/g (38 kJ/g) compared to 4 kcal/g (17 kJ/g) for carbohydrate or protein, so portions on the ketogenic diet are smaller than normal. The quantity of fat in the diet can be calculated from the overall energy requirements and the chosen ketogenic ratio. Next, the protein levels are set to allow for growth and body maintenance, and are around 1 g protein for each kg of body weight. Lastly, the amount of carbohydrate is set according to what allowance is left while maintaining the chosen ratio. Any carbohydrate in medications or supplements must be subtracted from this allowance. The total daily amount of fat, protein, and carbohydrate is then evenly divided across the meals.[39]
A computer program such as KetoCalculator may be used to help generate recipes.[49] The meals often have four components: heavy whipping cream, a protein-rich food (typically meat), a fruit or vegetable and a fat such as butter, vegetable oil, or mayonnaise. Only low-carbohydrate fruits and vegetables are allowed, which excludes bananas, potatoes, peas, and corn. Suitable fruits are divided into two groups based on the amount of carbohydrate they contain, and vegetables are similarly divided into two groups. Foods within each of these four groups may be freely substituted to allow for variation without needing to recalculate portion sizes. For example, cooked broccoli, Brussels sprouts, cauliflower, and green beans are all equivalent. Fresh, canned, or frozen foods are equivalent, but raw and cooked vegetables differ, and processed foods are an additional complication. Parents are required to be precise when measuring food quantities on an electronic scale accurate to 1 g. The child must eat the whole meal and cannot have extra portions; any snacks must be incorporated into the meal plan. A small amount of MCT oil may be used to help with constipation or to increase ketosis.[39]
The classic ketogenic diet is not a
| Meal | Menu idea | Ingredients |
|---|---|---|
| Breakfast | Egg with bacon |
|
| Morning snack | Peanut butter ball
(serving size: 0.5 ounce) |
|
| Lunch | Tuna salad |
|
| Afternoon snack | Keto yogurt
(serving size: 1.3 ounces) |
|
| Dinner | Cheeseburger (no bun) |
|
| Evening snack | Keto custard
(serving size: 1.2 ounces) |
|
MCT oil
Normal dietary fat contains mostly long-chain triglycerides (LCTs).
Modified Atkins
First reported in 2003, the idea of using a form of the Atkins diet to treat epilepsy came about after parents and patients discovered that the induction phase of the Atkins diet controlled seizures. The ketogenic diet team at Johns Hopkins Hospital modified the Atkins diet by removing the aim of achieving weight loss, extending the induction phase indefinitely, and specifically encouraging fat consumption. Compared with the ketogenic diet, the modified Atkins diet (MAD) places no limit on calories or protein, and the lower overall ketogenic ratio (about 1:1) does not need to be consistently maintained by all meals of the day. The MAD does not begin with a fast or with a stay in hospital and requires less dietitian support than the ketogenic diet. Carbohydrates are initially limited to 10 g per day in children or 20 g per day in adults, and are increased to 20–30 g per day after a month or so, depending on the effect on seizure control or tolerance of the restrictions. Like the ketogenic diet, the MAD requires vitamin and mineral supplements and children are carefully and periodically monitored at outpatient clinics.[50]
The modified Atkins diet reduces seizure frequency by more than 50% in 43% of patients who try it and by more than 90% in 27% of patients.[18] While the strength of evidence is low for the modified Atkins, it has been known to show seizure freedom in some infants.[51] Few adverse effects have been reported, though cholesterol is increased and the diet has not been studied long term.[50] Although based on a smaller data set (126 adults and children from 11 studies over five centres), these results from 2009 compare favorably with the traditional ketogenic diet.[18]
Low glycemic index treatment
The low glycemic index treatment (LGIT)
Short-term results for the LGIT indicate that at one month approximately half of the patients experience a greater than 50% reduction in seizure frequency, with overall figures approaching that of the ketogenic diet. The data (coming from one centre's experience with 76 children up to the year 2009) also indicate fewer side effects than the ketogenic diet and that it is better tolerated, with more palatable meals.[18][53]
Prescribed formulations

Infants and patients fed via a
Worldwide
In theory, there are no restrictions on where the ketogenic diet might be used, and it can cost less than modern anticonvulsants. However, fasting and dietary changes are affected by religious and cultural issues. A culture where food is often prepared by grandparents or hired help means more people must be educated about the diet. When families dine together, sharing the same meal, it can be difficult to separate the child's meal. In many countries, food labelling is not mandatory, so calculating macronutrients such as fat, protein and carbohydrates can be difficult. In some countries, it may be hard to find sugar-free forms of medicines and supplements, to purchase an accurate electronic scale, or to afford MCT oils.[57]
In Asia, the traditional diet includes rice and noodles as the main source of energy, making their elimination difficult. Therefore, the MCT-oil form of the diet, which allows more carbohydrate, has proved useful. In India, religious beliefs commonly affect the diet: for instance, Hindus consider cows sacred animals not to be killed and eaten, Islam forbids consumption of pork, and strict vegetarians of the Jain faith do not eat root vegetables. The Indian ketogenic diet is started without a fast due to cultural opposition towards fasting in children. The low-fat, high-carbohydrate nature of the normal Indian and Asian diet means that their ketogenic diets typically have a lower ketogenic ratio (1:1) than in America and Europe. However, they appear to be just as effective.[57]
In many developing countries, the ketogenic diet is expensive because dairy fats and meat are more expensive than grain, fruit, and vegetables. The modified Atkins diet has been proposed as a lower-cost alternative for those countries; the slightly more expensive food bill can be offset by a reduction in pharmaceutical costs if the diet is successful. The modified Atkins diet is less complex to explain and prepare and requires less support from a dietitian.[58]
Mechanism of action
Seizure pathology
The brain is composed of a network of
The nerve impulse is characterised by a great influx of sodium ions through channels in the neuron's cell membrane followed by an efflux of potassium ions through other channels. The neuron is unable to fire again for a short time (known as the refractory period), which is mediated by another potassium channel. The flow through these ion channels is governed by a "gate" which is opened by either a voltage change or a chemical messenger known as a ligand (such as a neurotransmitter). These channels are another target for anticonvulsant drugs.[7]
There are many ways in which epilepsy occurs. Examples of pathological physiology include: unusual excitatory connections within the neuronal network of the brain; abnormal neuron structure leading to altered current flow; decreased inhibitory neurotransmitter synthesis; ineffective receptors for inhibitory neurotransmitters; insufficient breakdown of excitatory neurotransmitters leading to excess; immature synapse development; and impaired function of ionic channels.[7]
Seizure control
Although many hypotheses have been put forward to explain how the ketogenic diet works, it remains a mystery. Disproven hypotheses include
On the ketogenic diet, carbohydrates are restricted and so cannot provide for all the metabolic needs of the body. Instead, fatty acids are used as the major source of fuel. These are used through
The ketone bodies are possibly
The ketogenic diet has been studied in at least 14 rodent animal models of seizures. It is protective in many of these models and has a different protection profile than any known anticonvulsant. Conversely, fenofibrate, not used clinically as an antiepileptic, exhibits experimental anticonvulsant properties in adult rats comparable to the ketogenic diet.[61] This, together with studies showing its efficacy in patients who have failed to achieve seizure control on half a dozen drugs, suggests a unique mechanism of action.[59]
Anticonvulsants suppress epileptic seizures, but they neither cure nor prevent the development of seizure susceptibility. The development of epilepsy (epileptogenesis) is a process that is poorly understood. A few anticonvulsants (valproate, levetiracetam and benzodiazepines) have shown antiepileptogenic properties in animal models of epileptogenesis. However, no anticonvulsant has ever achieved this in a clinical trial in humans. The ketogenic diet has been found to have antiepileptogenic properties in rats.[59]
Other medical applications
The ketogenic diet has been studied for potential therapeutic use in various neurological disorders other than epilepsy:
See also
Explanatory notes
- ^ In this article, kcal stands for calories as a unit of measure (4.1868 kJ), and calories stands for "energy" from food.
- ^ Unless otherwise stated, the term fasting in this article refers to going without food while maintaining calorie-free fluid intake.
- ^ Hippocrates, On the Sacred Disease, ch. 18; vol. 6.
- ^ Hippocrates, Epidemics, VII, 46; vol. 5.
- ^ Galen, De venae sect. adv. Erasistrateos Romae degentes, c. 8; vol. 11.
- ^ Galen, De victu attenuante, c. 1.
- ^ A good reduction is defined here to mean a 50–90% decrease in seizure frequency. An excellent reduction is a 90–99% decrease.
- ^ a b The ketogenic ratio k can be converted to the portion of calories from fat f using the Atwater coefficients of 9 and 4 kcal/g for fat and combined carbohydrate and water respectively. The equation is: f = 9 k/9 k + 4. For example, a 4:1 diet derives 90% of calories from fat. The inverse equation is k = 4 f/9 (1 - f).
- ^ Ketogenic "eggnog" is used during induction and is a drink with the required ketogenic ratio. For example, a 4:1 ratio eggnog would contain 60 g of 36% heavy whipping cream, 25 g pasteurised raw egg, saccharin and vanilla flavour. This contains 245 kcal (1,025 kJ), 4 g protein, 2 g carbohydrate and 24 g fat (24:6 = 4:1).[17] The eggnog may also be cooked to make a custard, or frozen to make ice cream.[39]
References
- ^ PMID 17332207
- ^ PMID 30403286
- PMID 23515147
- ^ PMID 19049583
- ^ PMID 19033218
- ^ PMID 24847102.
- ^ ISBN 1588292959.
- PMID 18280210
- PMID 28702868.
- ^ ISBN 1588292959.
- ISBN 0801848490.
- ^ Guelpa G, Marie A. La lutte contre l'epilepsie par la desintoxication et par la reeducation alimentaire. Rev Ther med-Chirurg. 1911; 78: 8–13. As cited by Bailey (2005).
- PMID 15652725
- ^ Kossoff EH. Do ketogenic diets work for adults with epilepsy? Yes! Archived 27 April 2018 at the Wayback Machine epilepsy.com. 2007, March. Cited 24 October 2009.
- ^ PMID 5166216
- ^ PMID 18456557
- ^ PMID 9823827
- ^ PMID 19535814
- ^ PMID 29881797.
- PMID 32199222.
- ^ PMID 17241206
- PMID 9832569. Lay summary– JHMI Office of Communications and Public Affairs. Updated 7 December 1998. Cited 6 March 2008.
- ^ PMID 11581442
- PMID 19332337.
- PMID 16901419
- PMID 29588983.
- ISBN 1588292959.
- ^ ISBN 978-1473117907.
- ^ ISBN 1899893245.
- ^ a b c d Turner Z, Kossoff EH. The ketogenic and Atkins diets: recipes for seizure control Archived 11 December 2019 at the Wayback Machine (PDF). Pract Gastroenterol. 2006 Jun;29(6):53, 56, 58, 61–62, 64.
- PMID 17544706
- PMID 15329084.
- ^ ISBN 1588292959.
- ^ Spendiff S. The diet that can treat epilepsy. Archived 1 April 2018 at the Wayback Machine Guardian. 2008 Aug 15;Sect. Health & wellbeing.
- PMID 25364257
- PMID 18281618
- PMID 20301603.
- PMID 16822355
- ^ ISBN 1588292959.
- ^ PMID 21855296.
- ^ PMID 17621514
- PMID 16523530
- ^ Vogelstein F. Epilepsy's Big, Fat Miracle. Archived 1 April 2018 at the Wayback Machine The New York Times. 2010 Nov 17.
- PMID 18301085
- ^ PMID 18028405
- ^ PMID 18823325
- ISBN 1588292959.
- ^ PMID 17241227
- PMID 19049577
- ^ PMID 19049584
- from the original on 5 July 2023. Retrieved 30 September 2023.
- ^ Pfeifer, Heidi H. Low glycemic index treatment Archived 27 April 2018 at the Wayback Machine. Epilepsy Foundation. 22 August 2013. Cited 31 March 2018.
- PMID 19220406
- ^ KetoCal Product Information Archived 12 June 2018 at the Wayback Machine. Nutricia North America. Cited 8 June 2018.
- ^ KetoVOLVE: 4:1 Ratio Powder. Solace Nutrition. Cited 17 June 2013.
- ^ a b Kossoff EH. The Ketogenic Diet ... in a bottle?. Keto News. Epilepsy.com. Updated July 2009. Cited 29 November 2009.
- ^ PMID 15679509.
- PMID 18782218
- ^ PMID 17509459
- PMID 6758355
- PMID 19054409.
- PMID 30554068
- PMID 33813635
Further reading
- Freeman JM, Kossoff EH, Freeman JB, Kelly MT. The Ketogenic Diet: A Treatment for Children and Others with Epilepsy. 4th ed. New York: Demos; 2007. ISBN 1932603182.
- Lowery R, Wilson J. The Ketogenic Bible: The Authoritative Guide to Ketosis. 1st ed. Victory Belt Publishing; 2017. ISBN 978-1628601046.
External links
- Diet Review: Ketogenic Diet for Weight Loss, from the Harvard University School of Public Health
- Ketogenic diet at Curlie
- Matthew's Friends, a UK charity and information resource
- The Charlie Foundation, a US charity and information resource
- Epilepsy.com: Dietary Therapies & Ketogenic News, information and regular research news updates