Kupffer cell
| Kupffer cell | |
|---|---|
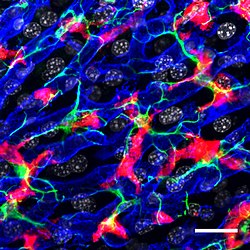 Confocal microscopy picture showing the steady-state location and interactions between Kupffer cells (Red), hepatic stellate cells (green) and liver sinusoidal endothelial cells (blue). Cell nuclei are in grey.[1] | |
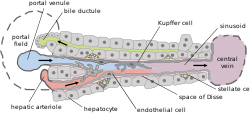 Basic liver structure | |
| Details | |
| Location | Liver |
| Function | Macrophage |
| Identifiers | |
| Latin | macrophagocytus stellatus |
| MeSH | D007728 |
| TH | H3.04.05.0.00016 |
| FMA | 14656 |
| Anatomical terms of microanatomy | |
Kupffer cells, also known as stellate macrophages and Kupffer–Browicz cells, are specialized cells localized in the liver within the lumen of the liver sinusoids and are adhesive to their endothelial cells which make up the blood vessel walls. Kupffer cells comprise the largest population of tissue-resident macrophages in the body. Gut bacteria, bacterial endotoxins, and microbial debris transported to the liver from the gastrointestinal tract via the portal vein will first come in contact with Kupffer cells, the first immune cells in the liver. It is because of this that any change to Kupffer cell functions can be connected to various liver diseases such as alcoholic liver disease, viral hepatitis, intrahepatic cholestasis, steatohepatitis, activation or rejection of the liver during liver transplantation and liver fibrosis.[2][3] They form part of the mononuclear phagocyte system.
Location and structure
Kupffer cells can be found attached to
Kupffer cells are amoeboid in character, with surface features including
The nucleus is indented and ovoid, and can be lobulated.
Notable cytoplasmic elements include
Importantly, Kupffer cells express the SR-AI/II scavenger receptor. This receptor is involved in recognising and binding the lipid A domain of lipopolysaccharide (LPS) and lipoteichoic acid. (Lipopolysaccharide (LPS) is a bacterial endotoxin which is found in the cell wall gram-negative bacteria, whereas lipoteichoic acid is present in gram-positive bacteria.) Because of this detection system, Kupffer cells play a critical role in initiating and mediating immune responses to bacterial infection of the liver.[4]
Development
Development of an initial population of Kupffer cells begins in the embryonic
However, if resident Kupffer cell populations are depleted, monocytes derived from hematopoietic stem cells in the bone marrow and transported through blood circulation to the liver can also fully differentiate into true Kupffer cells. Unlike other tissue macrophages, which must be continually renewed by circulating monocytes, these monocyte-derived Kupffer cells are capable of self-renewal once a population is established.[6]
Development of mature Kupffer cells is regulated by numerous growth factors, with macrophage colony-stimulating factor (
Function
The primary function of the Kupffer cell is to remove foreign debris and particles that have come from the hepatic portal system when passing through the liver. It is possible for the Kupffer cells to take in large particles by phagocytosis and smaller particles via pinocytosis.[4] Kupffer cells are integral in the innate responses of the immune system. They are important for host defense and play a role in the metabolism of many different compounds including, lipids, protein complexes and small particles. They are also useful in removing apoptotic cells from circulation.[2][3]
The amount of Kupffer cells in the liver is held constant. Kupffer cells have a proliferative capacity, allowing for cell populations to replenish themselves: this is in complete contrast to monocyte-derived macrophages that have no proliferative potential. Old or defective cells are removed through apoptosis, as well as through being phagocytized by neighbouring Kupffer cells.
Kupffer cells are heterogeneous in their function, dependent on their location in the
In response to infection or irritation, Kupffer cells can produce
Apart from
Helmy et al. identified a receptor present in Kupffer cells, the complement receptor of the immunoglobulin family (CRIg). Mice without CRIg could not clear complement system-coated pathogens. CRIg is conserved in mice and humans and is a critical component of the innate immune system.[8]
Clinical significance
Kupffer cells are incredibly plastic cells that have the capability to polarize specific activation states and can perform different functions in different microenvironments. M1 (classical activation) and M2 (alternative activation) designate the two extremes of
Kupffer cells play a role in the pathogenesis of a damaged liver in response to sepsis. The macrophages in the liver activate and release both IL-1 and TNF-alpha. In turn, this activates leukocytes and sinusoidal endothelial cells to express ICAM-1. This results in tissue damage to the endothelium because of proteases, oxygen radicals, prostanoids and other substances from leukocytes.
Kupffer cell activation contributes to pathogenesis of both chronic and acute alcoholic liver disease in response to ethanol-induced liver injury, common in chronic alcoholics. Chronic alcoholism and liver injury deal with a two-hit system. While the first hit is direct, mediated by the direct toxicity of ethanol and its metabolic byproducts, the second hit is indirect, mediated by increased uptake of lipopolysaccharide (endotoxin) from the intestine.
Ethanol increases permeability of the intestinal epithelium, resulting in endotoxin produced by the
The cascade begins with endotoxin-mediated activation of the Toll-like receptor 4 (
Cytokines and superoxides go on to cause inflammation and oxidizing damage respectively, while TNFα triggers the
History
The cells were first observed by Karl Wilhelm von Kupffer in 1876.[11] The scientist called them "Sternzellen" (star cells or hepatic stellate cell) but thought, inaccurately, that they were an integral part of the endothelium of the liver blood vessels and that they originated from it. In 1898, after several years of research, Tadeusz Browicz identified them, correctly, as macrophages.[12][13][14][15]
References
External links
- Anatomy photo: digestive/mammal/liver5/liver4 - Comparative Organology at University of California, Davis - "Mammal, liver (EM, Low)"
- Histology image: 15508loa – Histology Learning System at Boston University
