Lactation


Lactation describes the secretion of
In most species, lactation is a sign that the female has been pregnant at some point in her life, although in humans and goats, it can happen without pregnancy.
Galactopoiesis is the maintenance of milk production. This stage requires
Purpose
The chief function of a lactation is to provide nutrition and immune protection to the young after birth. Due to lactation, the mother-young pair can survive even if food is scarce or too hard for the young to attain, expanding the environmental conditions the species can withstand. The costly investment of energy and resources into milk is outweighed by the benefit to offspring survival.[4] In almost all mammals, lactation induces a period of infertility (in humans, lactational amenorrhea), which serves to provide the optimal birth spacing for survival of the offspring.[5]
Human
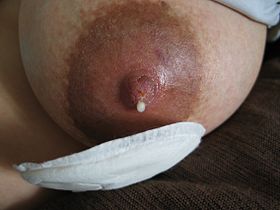
Hormonal influences
From the eighteenth week of
- Progesterone influences the growth in size of alveoli and lobes; high levels of progesterone inhibit lactation before birth. Progesterone levels drop after birth; this triggers the onset of copious milk production.[6]
- Estrogen stimulates the milk duct system to grow and differentiate. Like progesterone, high levels of estrogen also inhibit lactation. Estrogen levels also drop at delivery and remain low for the first several months of breastfeeding.[6] Breastfeeding mothers should avoid estrogen-based birth control methods, as a spike in estrogen levels may reduce a mother's milk supply.
- Prolactin contributes to the increased growth and differentiation of the alveoli, and also influences differentiation of ductal structures. High levels of prolactin during pregnancy and breastfeeding also increase insulin resistance, increase growth factor levels (IGF-1) and modify lipid metabolism in preparation for breastfeeding. During lactation, prolactin is the main factor maintaining tight junctions of the ductal epithelium and regulating milk production through osmotic balance.
- Human placental lactogen (HPL) – from the second month of pregnancy, the placenta releases large amounts of HPL. This hormone is closely associated with prolactin and appears to be instrumental in breast, nipple, and areola growth before birth.
- Follicle stimulating hormone (FSH), luteinizing hormone (LH), and human chorionic gonadotropin(hCG), through control of estrogen and progesterone production, and also, by extension, prolactin and growth hormone production, are essential.
- Growth hormone (GH) is structurally very similar to prolactin and independently contributes to its galactopoiesis.
- Adrenocorticotropic hormone (ACTH) and glucocorticoids such as cortisol have an important lactation inducing function in several animal species, including humans. Glucocorticoids play a complex regulating role in the maintenance of tight junctions.
- Thyroid-stimulating hormone (TSH) and thyrotropin-releasing hormone (TRH) are very important galactopoietic hormones whose levels are naturally increased during pregnancy.
- Oxytocin contracts the smooth muscle of the uterus during and after birth, and during orgasm(s). After birth, oxytocin contracts the smooth muscle layer of band-like cells surrounding the alveoli to squeeze the newly produced milk into the duct system. Oxytocin is necessary for the milk ejection reflex, or let-down, in response to suckling, to occur.
It is also possible to induce lactation without pregnancy through combinations of birth control pills, galactagogues, and milk expression using a breast pump.



Secretory differentiation
During the latter part of pregnancy, the woman's breasts enter into the Secretory Differentiation stage. This is when the breasts make colostrum (see below), a thick, sometimes yellowish fluid. At this stage, high levels of progesterone inhibit most milk production. It is not a medical concern if a pregnant woman leaks any colostrum before her baby's birth, nor is it an indication of future milk production.
Secretory activation
At birth, prolactin levels remain high, while the delivery of the placenta results in a sudden drop in progesterone, estrogen, and HPL levels. This abrupt withdrawal of progesterone in the presence of high prolactin levels stimulates the copious milk production of Secretory Activation.
When the breast is stimulated, prolactin levels in the blood rise, peak in about 45 minutes, and return to the pre-breastfeeding state about three hours later. The release of prolactin triggers the cells in the alveoli to make milk. Prolactin also transfers to the breast milk. Some research indicates that prolactin in milk is greater at times of higher milk production, and lower when breasts are fuller, and that the highest levels tend to occur between 2 a.m. and 6 a.m.[7]
Other hormones—notably insulin, thyroxine, and cortisol—are also involved, but their roles are not yet well understood. Although biochemical markers indicate that Secretory Activation begins about 30–40 hours after birth, mothers do not typically begin feeling increased breast fullness (the sensation of milk "coming in the breast") until 50–73 hours (2–3 days) after birth.
Colostrum is the first milk a breastfed baby receives. It contains higher amounts of white blood cells and antibodies than mature milk, and is especially high in immunoglobulin A (IgA), which coats the lining of the baby's immature intestines, and helps to prevent pathogens from invading the baby's system. Secretory IgA also helps prevent food allergies.[8] Over the first two weeks after the birth, colostrum production slowly gives way to mature breast milk.[6]
Autocrine control - Galactopoiesis
The hormonal
During this stage, the more that milk is removed from the breasts, the more the breast will produce milk.[9][10] Research also suggests that draining the breasts more fully also increases the rate of milk production.[11] Thus the milk supply is strongly influenced by how often the baby feeds and how well it is able to transfer milk from the breast. Low supply can often be traced to:
- not feeding or pumping often enough
- inability of the infant to transfer milk effectively caused by, among other things:
- jaw or mouth structure deficits
- poor latching technique
- premature birth
- drowsiness in the baby, due to illness, medication or recovery from medical procedures
- rare maternal endocrine disorders
- hypoplastic breast tissue
- inadequate calorie intake or malnutrition of the mother
Milk ejection reflex

This is the mechanism by which milk is transported from the breast alveoli to the nipple. Suckling by the baby stimulates the
Milk ejection is initiated in the mother's breast by the act of suckling by the baby. The milk ejection reflex (also called let-down reflex) is not always consistent, especially at first. Once a woman is conditioned to nursing, let-down can be triggered by a variety of stimuli, including the sound of any baby. Even thinking about breastfeeding can stimulate this reflex, causing unwanted leakage, or both breasts may give out milk when an infant is feeding from one breast. However, this and other problems often settle after two weeks of feeding.
A poor milk ejection reflex can be due to sore or cracked nipples, separation from the infant, a history of breast surgery, or tissue damage from prior breast trauma. If a mother has trouble breastfeeding, different methods of assisting the milk ejection reflex may help. These include feeding in a familiar and comfortable location, massage of the breast or back, or warming the breast with a cloth or shower.
Milk ejection reflex mechanism
This is the mechanism by which milk is transported from the breast alveoli to the nipple. Suckling by the baby innervates slowly adapting
Following the electrical impulse, oxytocin is released into the bloodstream. Through the bloodstream, oxytocin makes its way to
Afterpains
A surge of oxytocin also causes the uterus to contract. During breastfeeding, mothers may feel these contractions as afterpains. These may range from period-like cramps to strong labour-like contractions and can be more severe with second and subsequent babies.[15][16]
Without pregnancy, induced lactation, relactation
In humans, induced lactation and relactation have been observed frequently in some cultures, and demonstrated with varying success in adoptive mothers and wet nurses.[17][18] It appears plausible that the possibility of lactation in women (or females of other species) who are not biological mothers does confer an evolutionary advantage, especially in groups with high maternal mortality and tight social bonds.[19][20] The phenomenon has been also observed in most primates, in some lemurs, and in dwarf mongooses.[21][22]
Lactation can be induced in humans by a combination of physical and psychological stimulation, by drugs, or by a combination of those methods.[23] Several protocols for inducing lactation were developed by Dr. Jack Newman and Lenore Goldfarb and are commonly called the Newman-Goldfarb protocols. The "regular protocol" involves the use of birth control pills to mimic the hormone levels of pregnancy with domperidone to stimulate milk production, followed by discontinuing the birth control and the introducing use of a double electric breast pump to induce milk production.[24] Additional protocols exist to support an accelerated timeline and to support induced lactation in menopausal parents.
Some couples may stimulate lactation outside of pregnancy for sexual purposes.
Rare accounts of male lactation (as distinct from galactorrhea) exist in historical medical and anthropological literature.[25] Most recently a subject of transgender health care, multiple case reports have described patients assigned male at birth successfully inducing lactation.[26][27] Research has indicated that such breast milk is nutritionally comparible to both the milk of naturally lactating and induced lactating women.[28]
Domperidone is a drug that can induce lactation.[29][30]
Evolution
As all mammals lactate, lactation must have evolved before the last common ancestor of all mammals, which places it at a minimum in the Middle or Late Triassic when monotremes diverged from therians.[32] O. T. Oftedal has argued that therapsids evolved a proto-lacteal fluid in order to keep eggs moist, an adaptation necessitated due to synapsids’ parchment shelled eggs which are more vulnerable to evaporation and dehydration than the mineralized eggs produced by some sauropsids.[31][33] This protolacteal fluid became a complex, nutrient-rich milk which then allowed a decline in egg size by reducing the dependence on a large yolk in the egg.[20] The evolution of lactation is also believed to have resulted in the more complex dentition seen in mammals, as lactation would have allowed the prolonged development of the jaw before the eruption of teeth.[31]
Oftedal also proposed that the protolacteal fluid was initially secreted through pilosebaceous glands on mammary patches, analogous to the areola, and that hairs on this patch transported the fluid to the hatchlings as is seen in monotremes. This would have occurred in the mammal lineages that diverged after monotremes, metatheria and eutheria. In this scenario, some genes and signaling pathways involved in lactation evolved from ancient precursors which facilitated secretions from spiny structures, which themselves evolved from odontodes.[34]
Occurrence outside Mammalia
Another well known example of nourishing young with secretions of glands is the
The
Lactation is also the hallmark of
Toxeus magnus, an ant-mimicking jumping spider species of Southeast Asia, also lactates. It nurses its offspring for about 38 days, although they are able to forage on their own after 21 days. Blocking nursing immediately after birth resulted in complete mortality of the offspring, whereas blocking it 20 days after birth resulted in increased foraging and reduced survival. This form of lactation may have evolved from production of trophic eggs.[42]
See also
- Lactation room
- Galactogogue
- Milk line
- Male lactation
- Udder
- Breastfeeding
- Lactation failure
- Lactation suppression
- Erotic lactation
- Hypothalamic–pituitary–prolactin axis
- Roman charity
- Pregnancy
- Crop milk
References
- ^ PMID 19439024.
- ^ "Lactating Without Pregnancy". sites.google.com. Archived from the original on 14 January 2021.[unreliable source?]
- ^ "Goats with Precocious Udder Syndrome". berryemporium.com. Archived from the original on January 14, 2021.
- ISBN 978-1-4214-2042-4.
- S2CID 30817565.
- ^ ISBN 978-0-912500-92-8.
- PMID 11856965.
- ISBN 978-0-316-77924-1.
- PMID 3984973.
- S2CID 36906244.
- PMID 8471241.
- PMID 863036.
- PMID 1010088.
- PMID 15960763.
- ISBN 978-0-9845039-0-2.
- ISBN 978-1-86941-713-0.
- ISBN 978-0-323-04414-1.
- ^ Wilson-Clay B (1996). Induced Lactation. The American Surrogacy Center. Archived from the original on 9 February 2010.
- S2CID 1335211.
- ^ S2CID 12991397.
- S2CID 23240724.
- S2CID 4336672.
- PMID 9283123.
- ^ Goldfarb L, Newman J. "The Newman Goldfarb Protocols for Induced Lactation". www.asklenore.info.
- ^ Swaminathan N. "Strange but True: Males Can Lactate". Scientific American.
- PMID 29372185.
- S2CID 231755160.
- S2CID 258485541.
- TheGuardian.com.
- PMID 29372185.
- ^ S2CID 25806501.
- PMID 16291999.
- S2CID 8319185.
- S2CID 6608975.
- PMID 8527218.
- ^ "Bird Milk". web.stanford.edu.
- ^ PMID 21037057.
- S2CID 37973363.
- PMID 19272315.
- PMID 18647605.
- S2CID 31048064.
- PMID 30498127.
Further reading
- CBarras C (18 March 2008). "How mammals lost their egg yolks]—Did mammals develop nutritional milk before or after they abandoned yolky eggs?". New Scientist.

