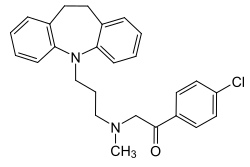
Lofepramine
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Gamanil, Lomont, Tymelyt, others |
| Other names | Lopramine; DB-2182; Leo-460; WHR-2908A[1][2][3][4] |
| AHFS/Drugs.com | International Drug Names |
| Routes of administration | Oral |
| ATC code | |
| Legal status | |
| Legal status |
|
| Metabolites | Desipramine (major) |
| Elimination half-life | Up to 5 hours;[1] 12–24 hours (active metabolites) |
| Excretion | Urine, feces (mostly as metabolites) |
| Identifiers | |
| |
JSmol) | |
| |
| |
| | |
Lofepramine, sold under the brand names Gamanil, Lomont, and Tymelyt among others, is a tricyclic antidepressant (TCA) which is used to treat depression.[7][3][8] The TCAs are so named as they share the common property of having three rings in their chemical structure. Like most TCAs lofepramine is believed to work in relieving depression by increasing concentrations of the neurotransmitters norepinephrine and serotonin in the synapse, by inhibiting their reuptake.[7] It is usually considered a third-generation TCA, as unlike the first- and second-generation TCAs it is relatively safe in overdose and has milder and less frequent side effects.[9]
Lofepramine is not available in the United States, Canada, Australia or New Zealand, although it is available in Ireland, Japan, South Africa and the United Kingdom, among other countries.[1]
Depression
In the United Kingdom, lofepramine is licensed for the treatment of depression which is its primary use in medicine.[6][10]
Lofepramine is an efficacious antidepressant with about 64% patients responding to it.[11]
Contraindications
To be used with caution, or not at all, for people with the following conditions:[7]
- Heart disease
- Impaired kidney or liver function
- Narrow angle glaucoma
- In the immediate recovery period after myocardial infarction
- In arrhythmias (particularly heart block)
- Mania
- In severe liver and/or severe renal impairment[12]
And in those being treated with amiodarone or terfenadine.[7]
Pregnancy and lactation
Lofepramine use during pregnancy is advised against unless the benefits clearly outweigh the risks.
Side effects
The most common adverse effects (occurring in at least 1% of those taking the drug) include agitation, anxiety, confusion, dizziness, irritability,
Dropout incidence due to side effects is about 20%.[11]
Side effects with unknown frequency include (but are not limited to):[13]
- Digestive effects:
- Constipation
- Diarrhoea
- Dry mouth
- Nausea
- Taste disturbances
- Vomiting
- Effects on the heart:
- Arrhythmia
- ECGchanges
- Abnormal heart rhythm
- Heart block
- Sudden cardiac death
- High heart rate
- Blood abnormalities:
- Abnormal blood cell counts
- Blood sugar changes
- Low blood sodium levels
- Breast effects:
- Breast enlargement, including in males.
- Spontaneous breast milk secretion that is unrelated to breastfeeding or pregnancy
- Effects on the skin:
- Abnormal sweating
- Hair loss
- Hives
- Increased light sensitivity
- Itching
- Rash
- Mental / neurologic effects:
- Delusions
- Hallucinations
- Headache
- Hypomania/mania
- Seizures
- Suicidal behaviour
- Other effects:
- Appetite changes
- Blurred vision
- Difficulty emptying the bladder
- Difficulty talking due to difficulties in moving the required muscles
- Liver problems
- Ringing in the ears
- impotence
- Swelling
- Weight changes
Withdrawal
If abruptly stopped after regular use it can cause withdrawal effects such as sleeplessness, irritability and excessive sweating.[7]
Overdose
Compared to other TCAs, lofepramine is considered to be less toxic in overdose.[13] Its treatment is mostly a matter of trying to reduce absorption of the drug, if possible, using gastric lavage and monitoring for adverse effects on the heart.[7]
Interactions
Lofepramine is known to interact with:[13][7]
- Alcohol. Increased sedative effect.
- drop in blood pressure upon standing.
- ventricular arrhythmias.
- Anticoagulants(blood thinners). Lofepramine may inhibit the metabolism of certain anticoagulants leading to a potentially increased risk of bleeding.
- Anticonvulsants. Possibly reduce the anticonvulsanteffect of antiepileptics by lowering the seizure threshold.
- paralytic ileus, among other effects) and sedative effects.
- antimuscarinicside-effects.
- hypnotics. Increased sedative effect.
- Apraclonidine. Avoidance advised by manufacturer of apraclonidine.
- Brimonidine. Avoidance advised by manufacturer of brimonidine.
- antihypertensiveeffects of clonidine.
- Diazoxide. Enhanced hypotensive (blood pressure-lowering) effect.
- irregular heart rate.
- Disulfiram. May require a reduction of lofepramine dose.
- reduced blood pressure on standing.
- Cimetidine, diltiazem, verapamil. May increase concentration of lofepramine in the blood plasma.
- Hydralazine. Enhanced hypotensive effect.
- MAOIs). Advised not to be started until at least 2 weeks after stopping MAOIs. MAOIs are advised not to be started until at least 1–2 weeks after stopping TCAs like lofepramine.
- Moclobemide. Moclobemide is advised not to be started until at least one week after treatment with TCAs is discontinued.
- Nitrates. Could possibly reduce the effects of sublingual tablets of nitrates (failure to dissolve under tongue owing to dry mouth).
- Rifampicin. May accelerate lofepramine metabolism thereby decreasing plasma concentrations of lofepramine.
- Ritonavir. May increase lofepramine concentration in the blood plasma.
- Sodium nitroprusside. Enhanced hypotensive effect.
- Thyroid hormones. Effects on the heart of lofepramine may be exacerbated.
Pharmacology
Pharmacodynamics
| Site | LPA | DSI | Species | Ref |
|---|---|---|---|---|
| SERT | 70 | 17.6–163 | Human | [16][17] |
| NET | 5.4 | 0.63–3.5 | Human | [16][17] |
| DAT | >10,000 | 3,190 | Human | [16] |
| 5-HT1A | 4,600 | ≥6,400 | Human | [18][19] |
| 5-HT2A | 200 | 115–350 | Human | [18][19] |
| 5-HT2C | ND | 244–748 | Rat | [20][21] |
| 5-HT3 | ND | 4,402 | Mouse | [21] |
| 5-HT7 | ND | >1,000 | Rat | [22] |
| α1 | 100 | 23–130 | Human | [18][23][17] |
| α2 | 2,700 | ≥1,379 | Human | [18][23][17] |
β |
>10,000 | ≥1,700 | Rat | [24][25] |
D1 |
500 | 5,460 | Human/rat | [26] |
D2 |
2,000 | 3,400 | Human | [18][23] |
| H1 | 245–360 | 60–110 | Human | [27] |
| H2 | 4,270 | 1,550 | Human | [27] |
| H3 | 79,400 | >100,000 | Human | [27] |
| H4 | 36,300 | 9,550 | Human | [27] |
| mACh | 67 | 66–198 | Human | [18][23] |
| M1 | 67 | 110 | Human | [28] |
| M2 | 330 | 540 | Human | [28] |
| M3 | 130 | 210 | Human | [28] |
| M4 | 340 | 160 | Human | [28] |
| M5 | 460 | 143 | Human | [28] |
| σ1 | 2,520 | 4,000 | Rodent | [29][14] |
| σ2 | ND | 1,611 | Rat | [14] |
| Values are Ki (nM). The smaller the value, the more strongly the drug binds to the site. | ||||
Lofepramine is a strong inhibitor of norepinephrine reuptake and a moderate inhibitor of serotonin reuptake.[14] It is a weak-intermediate level antagonist of the muscarinic acetylcholine receptors.[14]
Lofepramine has been said to be a prodrug of desipramine,[30] although there is also evidence against this notion.[8]
Pharmacokinetics
Lofepramine is extensively metabolized, via cleavage of the p-chlorophenacyl group, to the TCA, desipramine, in humans.[7][8][1] However, it is unlikely this property plays a substantial role in its overall effects as lofepramine exhibits lower toxicity and anticholinergic side effects relative to desipramine while retaining equivalent antidepressant efficacy.[8] The p-chlorophenacyl group is metabolized to p-chlorobenzoic acid which is then conjugated with glycine and excreted in the urine.[7] The desipramine metabolite is partly secreted in the faeces.[7] Other routes of metabolism include hydroxylation, glucuronidation, N-dealkylation and N-oxidation.[7][1]
Chemistry
Lofepramine is a
History
Lofepramine was developed by Leo Läkemedel AB.[36] It first appeared in the literature in 1969 and was patented in 1970.[36] The drug was first introduced for the treatment of depression in either 1980 or 1983.[36][37]
Society and culture
Generic names
Lofepramine is the
Brand names
Brand names of lofepramine include Amplit, Deftan, Deprimil, Emdalen, Gamanil, Gamonil, Lomont, Tymelet, and Tymelyt.[1][2][3][4]
Availability
In the United Kingdom, lofepramine is marketed (as the hydrochloride salt) in the form of 70 mg tablets [12] and 70 mg/5 mL oral suspension.[39]
Research
Fatigue
A formulation containing lofepramine and the
References
- ^ a b c d e f "Lofepramine Hydrochloride". Martindale: The Complete Drug Reference. The Pharmaceutical Press. Retrieved 3 August 2017.
- ^ ISBN 978-1-4757-2085-3.
- ^ ISBN 978-3-88763-075-1.
- ^ a b c d "Lofepramine". Drugs.com. Archived from the original on 2017-08-14. Retrieved 2017-08-14.
- S2CID 195693275.
- ^ a b "Lofepramine 70mg tablets - Summary of Product Characteristics (SPC)". electronic Medicines Compendium. Merck Serono. 18 November 2010. Archived from the original on 2 December 2013. Retrieved 21 November 2013.
- ^ a b c d e f g h i j k l m n o p "Lofepramine 70 mg Film-coated Tablets - Summary of Product Characteristics (SPC) - (eMC)". electronic Medicines Compendium (eMC). Datapharm. April 2016. Archived from the original on 3 August 2017. Retrieved 3 August 2017.
- ^ PMID 2891742.
- ^ "SAFC Commercial Life Science Products & Services | Sigma-Aldrich". Safcglobal.com. 2015-05-12. Retrieved 2016-02-24.
- ISBN 978-0-85711-084-8.
- ^ S2CID 22873432.
- ^ a b "Lofepramine 70mg Tablets". Archived from the original on 2015-10-25. Retrieved 2014-08-07.
- ^ ISBN 978-0-85711-276-7.
- ^ a b c d e Roth BL, Driscol J. "PDSP Ki Database". Psychoactive Drug Screening Program (PDSP). University of North Carolina at Chapel Hill and the United States National Institute of Mental Health. Retrieved 7 May 2022.
- ^ Roth BL, Driscol J. "PDSP Ki Database". Psychoactive Drug Screening Program (PDSP). University of North Carolina at Chapel Hill and the United States National Institute of Mental Health. Retrieved 7 May 2022.
- ^ PMID 9537821.
- ^ PMID 9400006.
- ^ S2CID 21236268.
- ^ PMID 3816971.
- S2CID 24889381.
- ^ PMID 9686407.
- PMID 8394362.
- ^ PMID 6086881.
- PMID 3790168.
- S2CID 19490821.
- PMID 17850785.
- ^ S2CID 14274150.
- ^ PMID 8100134.
- PMID 2877462.
- ^ ISBN 978-3-527-64632-6.
- ^ ISBN 978-94-007-5805-6.
- ^ ISBN 978-0-7817-6879-5.
- ISBN 978-0-471-95052-3.
- ^ ISBN 978-0-19-162675-3.
- ISBN 978-1-56053-470-9.
- ^ PMID 19557250.
- ISBN 978-0-7817-2845-4.
- ISBN 978-94-011-4439-1.
- ^ "Lofepramine Rosemont 70mg/5ml Oral Suspension - Summary of Product Characteristics (SPC) - (eMC)". 26 January 2016. Retrieved 3 August 2017.
- ^ "Lofepramine/phenylalanine - MultiCell Technologies". AdisInsight. Springer International Publishing AG. Retrieved 3 August 2017.
