Lymphadenopathy
| Lymphadenopathy | |
|---|---|
| Other names | Adenopathy, swollen lymph nodes, swollen glands |
MRI scan; ultrasound | |
Lymphadenopathy or adenopathy is a
Lymphadenopathy is a common and nonspecific
Causes

Lymph node enlargement is recognized as a common sign of infectious, autoimmune, or malignant disease. Examples may include:
- Reactive: acute ).
- The most distinctive sign of bubonic plague is extreme swelling of one or more lymph nodes that bulge out of the skin as "buboes." The buboes often become necrotic and may even rupture.[5]
- Epstein-Barr virus and may be characterized by a marked enlargement of the cervical lymph nodes.[6]
- It is also a sign of
- Toxoplasmosis, a parasitic disease, gives a generalized lymphadenopathy (Piringer-Kuchinka lymphadenopathy).[9]
- Mesenteric lymphadenitis after viral systemic infection (particularly in the GALT in the appendix) can commonly present like appendicitis.[12][13]
Infectious causes of lymphadenopathy may include bacterial infections such as
- Tumoral:
- Primary: Hodgkin lymphoma[16] and non-Hodgkin lymphoma give lymphadenopathy in all or a few lymph nodes.[9]
- Secondary: metastasis, Virchow's node, neuroblastoma,[17] and chronic lymphocytic leukemia.[18]
- systemic lupus erythematosus[19] and rheumatoid arthritis may have a generalized lymphadenopathy.[9]
- Immunocompromised: progression, preceding a diagnosis of AIDS.
- Bites from certain venomous snakes such as the pit viper[21]
- Unknown: Kimura disease[25]
Benign (reactive) lymphadenopathy
Benign lymphadenopathy is a common biopsy finding, and may often be confused with
- Follicular hyperplasia: This is the most common type of reactive lymphadenopathy.[6]
- Paracortical hyperplasia/Interfollicular hyperplasia: It is seen in viral infections, skin diseases, and nonspecific reactions.
- Sinus histiocytosis: It is seen in lymph nodes draining limbs, inflammatory lesions, and malignancies.
- Nodal extensive necrosis
- Nodal granulomatous inflammation
- Nodal extensive fibrosis (Connective tissue framework)
- Nodal deposition of interstitial substance
These morphological patterns are never pure. Thus, reactive follicular hyperplasia can have a component of paracortical hyperplasia. However, this distinction is important for the differential diagnosis of the cause.
Diagnosis
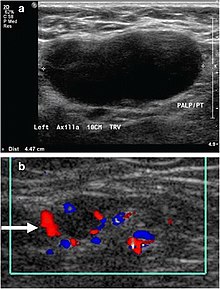
- Absence of the fatty hilum
- Increased focal cortical thickness greater than 3 cm
- Doppler ultrasonography that shows hyperaemic blood flow in the hilum and central cortex and/or abnormal (non-hilar cortical) blood flow.[26]
In
On
Fine-needle aspiration cytology (FNAC) has sensitivity and specificity percentages of 81% and 100%, respectively, in the histopathology of malignant cervical lymphadenopathy.[27] PET-CT has proven to be helpful in identifying occult primary carcinomas of the head and neck, especially when applied as a guiding tool prior to panendoscopy, and may induce treatment related clinical decisions in up to 60% of cases.[27]
Classification
Lymphadenopathy may be classified by:
- Size, where lymphadenopathy in adults is often defined as a short axis of one or more lymph nodes is greater than 10mm.[29]
- By extent:
- Localized lymphadenopathy: due to localized spot of infection; e.g., an infected spot on the scalp will cause lymph nodes in the neck on that same side to swell up

- Generalized lymphadenopathy: due to a systemic infection of the body; e.g., influenza or secondary syphilis
- Persistent generalized lymphadenopathy (PGL): persisting for a long time, possibly without an apparent cause
- Generalized lymphadenopathy: due to a systemic infection of the body; e.g., influenza or secondary syphilis
- By localization:
- Dermatopathic lymphadenopathy: lymphadenopathy associated with skin disease.
- By malignancy: Benign lymphadenopathy is distinguished from malignant types which mainly refer to lymphomas or lymph node metastasis.
Size


- By size, where lymphadenopathy in adults is often defined as a short axis of one or more lymph nodes is greater than 10mm.[29][30] However, there is regional variation as detailed in this table:
| Generally | 10 mm[29][30] |
| Inguinal | 10[31] – 20 mm[32] |
| Pelvis | 10 mm for ovoid lymph nodes, 8 mm for rounded[31] |
| Neck | |
|---|---|
| Generally (non-retropharyngeal) | 10 mm[31][33] |
| Jugulodigastric lymph nodes | 11mm[31] or 15 mm[33] |
| Retropharyngeal | 8 mm[33]
|
| Mediastinum | |
| Mediastinum, generally | 10 mm[31] |
| Superior mediastinum and high paratracheal | 7mm[34] |
| Low paratracheal and subcarinal | 11 mm[34] |
| Upper abdominal | |
| Retrocrural space | 6 mm[35] |
| Paracardiac | 8 mm[35] |
| Gastrohepatic ligament | 8 mm[35] |
| Upper paraaortic region | 9 mm[35] |
| Portacaval space | 10 mm[35] |
| Porta hepatis | 7 mm[35] |
| Lower paraaortic region | 11 mm[35] |
Lymphadenopathy of the
In children, a short axis of 8 mm can be used.[37] However, inguinal lymph nodes of up to 15 mm and cervical lymph nodes of up to 20 mm are generally normal in children up to age 8–12.[38]
Lymphadenopathy of more than 1.5–2 cm increases the risk of
See also
References
- ^ "lymphadenitis" at Dorland's Medical Dictionary
- ^ "lymphangitis" at Dorland's Medical Dictionary
- PMID 21865192.
- PMID 21243990.
- PMID 19606935.
- ^ PMID 23281438.
- PMID 21852539.
- S2CID 8688394.
- ^ a b c Status and anamnesis, Anders Albinsson. Page 12
- PMID 22977337.
- PMID 22728487.
- PMID 23618562.
- PMID 12800960.
- PMID 33085335.
- PMID 23068148.
- PMID 18788239.
- PMID 21736987.
- PMID 22143059.
- PMID 19107085.
- PMID 18620868.
- PMID 22998994.
- PMID 23020225.
- PMID 22789970.
- PMID 22560577.
- PMID 23154725.
- ^ PMID 25534139. Creative Commons attribution license
- ^ PMID 22312490.
- ^ PMID 18390388.
- ^ PMID 20080453.
- ^ PMID 17724531.
- ^ PMID 15347718.
- ^ "Assessment of lymphadenopathy". BMJ Best Practice. Retrieved 2017-03-04. Last updated: Last updated: Feb 16, 2017
- ^ ISBN 9781482216202.
- ^ S2CID 7434544.
- ^ PMID 2068292.
- ^ ISBN 9781609139438.
- ISBN 9781455711444.
- ^ Laurence Knott. "Generalised Lymphadenopathy". Patient UK. Retrieved 2017-03-04. Last checked: 24 March 2014
- PMID 12484692.
External links
- HPC:13820 Archived 2012-06-02 at the Wayback Machine on humpath.com (Digital slides)
