Maprotiline
 | |
 | |
| Clinical data | |
|---|---|
| Trade names | Ludiomil, others |
| Other names | Maprotiline hydrochloride; Maprotiline methanesulfonate; Ba 34276[1][2][3] |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a682158 |
| Routes of administration | Oral, intramuscular, intravenous |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 66–70% |
| Protein binding | 88% |
| Metabolism | hepatic |
| Onset of action | 6 hours |
| Elimination half-life | 27–58 hours |
| Excretion | Urine (57%) and bile (30%) as glucuronides, 3–4% as unchanged drug |
| Identifiers | |
| |
JSmol) | |
| |
| |
| | |
Maprotiline, sold under the brand name Ludiomil among others, is a
Medical uses
Maprotiline is used in the treatment of depression, such as depression associated with agitation or anxiety and has similar efficacy to the antidepressant drug moclobemide.[12] This finding has also been validated by a group of general practitioners who compared the respective efficacy and tolerability of maprotiline and moclobemide.[13]
- Treatment of neurotic), especially depression associated with agitation or anxiety
- Panic disorder
- Neuropathic pain, including painful polyneuropathy in diabetics and non-diabetics alike.[14]
- Treatment of the depressive phase of bipolar affective disorder
- For the symptomatic relief of tension or insomnia
The use of maprotiline in the treatment of
A very small body of research has also explored the potential of maprotiline in treating diabetic kidney disease[16] and it has been measured against amitriptyline in this regard.[17]
Maprotiline and fluoxetine have also been found, among certain lines of research, to have quite potent anti-profilerative effects against certain forms of cancer of the Burkitt lymphoma type.[18][19] One study also bore ought a certain level of evidence regarding maprotiline’s ability to suppress both cholesterol biosynthesis and hepatocellular carcinoma liver-cancer progression.
Maprotiline was also measured against imipramine, fluoxetine and ketamine in an experiment-model involving two different kinds of chicken differently-conditioned against stress, including (black) Australorps in the proposed treatment of treatment-resistant depression in humans.[20]
In general, lower dosages are recommended for patients over 60 years of age. Dosages of 50 mg to 75 mg daily are usually satisfactory as maintenance therapy for elderly patients who do not tolerate higher amounts.[21][22] In any case, 225 m.g./d. is the absolute-maximum highest recommended dose for this drug, as any more can predispose more significantly to seizures. 150 m.g. is the average optimal daily dose for otherwise-healthy patients who can tolerate a full dose.
Available forms
- Coated tablets: 10 mg, 25 mg, 50 mg, and 75 mg
- Injectable concentrate, 25 mg
Contraindications
In generalised theory, maprotiline (as with other tricyclic antidepressants, besides trimipramine[23][24][25] and possibly clomipramine) may somewhat worsen certain features of schizophrenia, necessitating caution in prescribing them to someone with it and continuation of the antipsychotic treatment (e.g., with risperidone or olanzapine). However, certain bodies of evidence have found maprotiline a useful augment in treating some of the negative, or "anaesthetic", symptoms of schizophrenia and in probable extension pronounced schizoidia (including the characteristic deterioration in personal grooming/appearance).[26][27] It has also been weighed against fluvoxamine in this overall regard (i.e., treating the negative symptoms of schizophrenia),[28] with fluvoxamine evidencing clear superiority therein. Maprotiline, however, may be specifically useful for the "negative symptom" of alogia (poverty of thought and/or speech) and in this regard was found demonstrably superior to the other control-drugs (alprazolam, bromocriptine, citalopram, fluoxetine, fluvoxamine, nortriptyline) in one study.[29] Citalopram, clomipramine and fluvoxamine appeared particularly useful in the study for reducing affective blunting, with alprazolam (Xanax) and maprotiline ranking joint-next.
Patients with
They (
Absolute
- Hypersensitivity to maprotiline or to other TCAs and TeCAs
- prostate glandwith urine hesitancy
- Closed angle glaucoma
Special caution needed
- Concomitant treatment with a MAO inhibitor
- Serious impairment of liver and kidney function
- alcohol withdrawal, other medications)
- Serious cardiovascular conditions (arrhythmias, heart insufficiency, state after myocardial infarctionetc.)
- Treatment of patients under age 18[38]
Suicidal patients
As with other antidepressants, maprotiline increased the risk compared to placebo of suicidal thinking and behavior (suicidality) in children, adolescents and young adults in short-term studies of major depressive disorder (MDD) and other psychiatric disorders. Anyone considering the use of maprotiline or any other antidepressant in a child, adolescent, or young adult must balance this risk with the clinical need. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a reduction in risk with antidepressants compared to placebo in adults aged 65 and older. Depression and certain other psychiatric disorders are themselves associated with increases in the risk of suicide. Patients of all ages who are started on antidepressant therapy should be monitored appropriately and observed closely for clinical worsening, suicidality, or unusual changes in behavior. Families and caregivers should be advised of the need for close observation and communication with the prescriber. Maprotiline is not approved for use in pediatric patients.[39]
Pregnancy and lactation
Reproduction studies have been performed in female laboratory rabbits, mice, and rats at doses up to 1.3, 7, and 9 times the maximum daily human dose respectively and have revealed no evidence of impaired fertility or harm to the fetus due to maprotiline. There are, however, no adequate and well controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Maprotiline is excreted in breast milk. At steady-state, the concentrations in milk correspond closely to the concentrations in whole blood. Caution should be exercised when maprotiline hydrochloride is administered to a nursing woman.
Side effects
The side-effect profile is comparable to other TCAs and TeCAS and many of the following are due to anticholinergic (which are less prominent than those of most TCAs) and antihistamine effects.[15] Most often seen are:
- Dizziness
- Drowsiness
- Somnolence
- Fatigue
- dental caries)
- Constipation
- Vertigo
- Nausea (rare, incidence of ~2%) and vomiting
- Increased appetite and weight gain
- arrhythmiasand other cardiac effects
- decreased libido
- Sexual dysfunction in women: decreased libido, vaginal dryness, painful sexual intercourse, anorgasmia
- Allergic skin reactions such as urticaria (more often than with other antidepressants). Rarely, severe skin reactions such as erythema multiformecan occur.
- Photosensitivity
- Agitation, confusion
- Induction of bipolar affective disorder
- Psychoticsymptoms
- Tremor
- Extrapyramidal symptoms
- Headache
- Seizures (at high doses)
- Rare haematological complications: leukopenia and agranulocytosis (dangerous fall in white blood cells)
- Fever
- Urinary retention
Maprotiline causes a strong initial sedation (first 2 to 3 weeks of therapy) and is therefore indicated to treat agitated patients or those with suicidal risks. It causes
Maprotiline has no known potential for abuse and psychological dependence.
Withdrawal
Withdrawal symptoms frequently seen when treatment with maprotiline is stopped abruptly (agitation, anxiety, insomnia, sometimes activation of mania or rebound depression) can be avoided by reducing the daily dose of maprotiline gradually by approximately 25% each week. If treatment has to be stopped at once due to medical reasons, the use of a benzodiazepine (e.g., lorazepam, clonazepam, diazepam) for a maximum of 4 weeks as needed will usually suppress withdrawal symptoms.
Interactions
Maprotiline does have a wide range of possible interactions. Some are typical for TCAs and TeCAs, others are caused by specific metabolic effects (e.g., high plasma-protein-binding) of maprotiline:
Increased drug actions:
- Other antidepressants, barbiturates, narcotics, sedating antihistamines, anticonvulsive drugs, alcohol – resulting in increased central depression and necessitating some caution when using any of these drugs alongside maprotiline
- Drugs with potential anti-muscarinic/anti-cholinergic activity (antiparkinsonian agents, tricyclic antidepressantsbesides maprotiline) – resulting in increased anti-muscarinic effects (dry mouth, constipation, etc.)
- Sympathomimetics (also those used in local anesthetics like noradrenaline) – sympathomimetic effects increased (increased blood-pressure, pulse-rate, paleness of skin, etc.)
- Nitrates and antihypertensives (e.g., beta-blockers) – increased antihypertensive action with pronounced fall in blood pressure
Although concurrent administration of tricyclic antidepressants (likewise with
In any case, however, it is very-strongly advised that an MAOI is added to the (compatible) tricyclic and not the other way around, as adding a tricyclic to an existing treatment-regime involving an MAOI may significantly increase the risk of going into hypertensive crisis.
Decreased drug actions:
- Guanethidine, reserpine, guanfacine: anti-hypertensive effects decreased
- Clonidine: anti-hypertensive effects decreased and risk of (massive) rebound hypertension.
Other types of interaction:
- Drugs which induce certain enzymes in the liver, e.g., barbiturates, phenytoin, carbamazepine and oral anti-conceptive drugs, enhance the elimination of maprotiline and decrease its antidepressant effects. Additionally the blood-concentrations of phenytoin or carbamazepine may be increased, leading to a higher incidents of side effects.
- The concomitant use of maprotiline and neurolepticscan lead to increased maprotiline blood-levels and to seizures. Combining maprotiline and thioridazine could induce severe arrhythmias.
- Additionally, increased blood-levels of maprotiline are possible, if certain beta-blocking agents (e.g., propranolol) are given concomitantly.
- Maprotiline may amplify the actions of coumarin-type anticoagulants (e.g., warfarin, phenprocoumon). The plasma-prothrombin-activity must be assessed closely in order to avoid overt bleedings.
- Maprotiline can increase the actions of oral antidiabetic drugs (sulfonylureas) and insulin. Diabetic patients should have regular assessments of their blood-glucose-levels.
- The concomitant application with fluoxetine or fluvoxamine may lead to significantly increased plasma-levels of maprotiline, with a correspondingly (and substantially) incidence of maprotiline side effects. Owing to the long half-lives of fluoxetine and fluvoxamine, this effect may persist for quite-some time.
Pharmacology
Pharmacodynamics
| Site | Ki (nM) | Species | Ref | |
|---|---|---|---|---|
| SERT | 5,800 | Human | [46] | |
| NET | 11–12 | Human | [46][47] | |
| DAT | 1,000 | Human | [46] | |
| 5-HT2A | 51 | Rat | [48] | |
| 5-HT2C | 122 | Rat | [48] | |
| 5-HT6 | ND | ND | ND | |
| 5-HT7 | 50 | Guinea pig | [49] | |
| α1 | 90 | Human | [50] | |
| α2 | 9,400 | Human | [50] | |
| D1 | 402 | Human | [51] | |
| D2 | 350–665 | Human | [51][50] | |
| D3 | 504 | Human | [51] | |
| D4 | ND | ND | ND | |
| D5 | 429 | Human | [51] | |
| H1 | 0.79–2.0 | Human | [52][51][53][50] | |
| H2 | 776 | Human | [52] | |
| H3 | 66,100 | Human | [51] | |
| H4 | 85,100 | Human | [52] | |
| mACh | 570 | Human | [54][50] | |
| Values are Ki (nM). The smaller the value, the more strongly the drug binds to the site. | ||||
Maprotiline exhibits strong effects as a
The pharmacological profile of maprotiline explains its
The postulated mechanism of maprotiline is that it acts primarily by potentiation of central adrenergic synapses by blocking reuptake of norepinephrine at nerve endings. This pharmacological action is thought to be primarily responsible for the drug's antidepressant and anxiolytic effects. It is a strong norepinephrine reuptake inhibitor with only weak effects on serotonin and dopamine reuptake. At higher doses, however, maprotiline increases serotonergic transmission and increases the level of serotonin available.[58]
Pharmacokinetics
After oral use absorption is good. It binds to plasma proteins 80–90%. Maximal plasma concentration is reached 6 hours after use. The mean time to peak is 12 hours. The
Chemistry


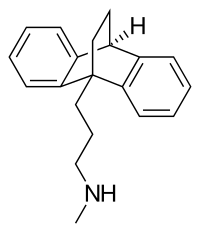
Maprotiline is a
Maprotiline is very similar in structure to the anxiolytic, sedative, and muscle relaxant drug benzoctamine (Tacitin).[6][60] The only structural difference between the two compounds is in the length of their side chain.[6][60] However, this modification results in considerable differences in their pharmacological and therapeutic effects.[6][60]
History
Maprotiline was developed by
Society and culture

Generic names
Maprotiline is the
Brand names
Maprotiline is marketed throughout the world, mainly under the brand name Ludiomil.[2][3] It is also available under a variety of other brand names including Deprilept, Maprolu, and Psymion among others.[2][3]
Although it remains widely available across the world, it was discontinued in the
References
- ^ ISBN 978-1-4757-2085-3.
- ^ ISBN 978-3-88763-075-1.
- ^ a b c d e f "Maprotiline - Drugs.com". drugs.com. Retrieved 28 March 2018.
- ^ Anvisa (2023-03-31). "RDC Nº 784 - Listas de Substâncias Entorpecentes, Psicotrópicas, Precursoras e Outras sob Controle Especial" [Collegiate Board Resolution No. 784 - Lists of Narcotic, Psychotropic, Precursor, and Other Substances under Special Control] (in Brazilian Portuguese). Diário Oficial da União (published 2023-04-04). Archived from the original on 2023-08-03. Retrieved 2023-08-16.
- ^ ISBN 978-1-60913-345-0.
- ^ ISBN 978-1-4831-9193-5.
- S2CID 8444656.
- PMID 16617674.
- PMID 2859273.
- PMID 6360257.
- S2CID 41977086.
- PMID 8557884.
- S2CID 260560762.
- PMID 9430812.
- ^ a b c "DRUGDEX Evaluations - Maprotiline". Retrieved 25 April 2013.
- ^ Zhou, Z. and Liu, S., 2022. Maprotiline Ameliorates High Glucose-Induced Dysfunction in Renal Glomerular Endothelial Cells. Experimental and Clinical Endocrinology & Diabetes, 130(09), pp.596-603.
- S2CID 6097534.
- S2CID 33104465.
- S2CID 24955263.
- S2CID 23648185.
- ^ "Maprotiline: MedlinePlus Drug Information". www.nlm.nih.gov. Retrieved 29 September 2013.
- ^ "Maprotiline - FDA prescribing information, side effects and uses". www.drugs.com. Archived from the original on 30 December 2019. Retrieved 29 September 2013.
- S2CID 29596291.
- S2CID 5719177.
- S2CID 41564511.
- PMID 2570687.
- S2CID 40809634.
- PMID 9617979.
- ^ Shafti SS, Rey A, Abad A (2005). "Drug – Specific Responsiveness of Negative Symptoms". International Journal of Psychosocial Rehabilitation. pp. 10 (1), 43–51. Archived from the original on 2012-07-12. Retrieved 2012-04-29.
- S2CID 260253520.
- PMID 3314536.
- PMID 28503107.
- PMID 22706421.
- PMID 24359859.
- S2CID 201125145.
- PMID 15898959.
- PMID 23789317.
- ^ Simeon J, Maguire J, Lawrence S (1981). Maprotiline effects in children with enuresis and behavioural disorders. Progress in Neuro-Psychopharmacology 5 ( 5–6), 495–8
- ^ U.S. National Library of Medicine. Last Reviewed 1 Sept. 2010 Medline Plus entry for Maprotiline
- PMID 6421394.
- S2CID 206312818.
- PMID 2677241.
- PMID 8006248.
- S2CID 35570626.
- ^ Roth BL, Driscol J. "PDSP Ki Database". Psychoactive Drug Screening Program (PDSP). University of North Carolina at Chapel Hill and the United States National Institute of Mental Health. Retrieved 7 May 2022.
- ^ PMID 9537821.
- PMID 19836247.
- ^ S2CID 24889381.
- S2CID 24189673.
- ^ PMID 6086881.
- ^ PMID 19091563.
- ^ S2CID 14274150.
- S2CID 45303586.
- PMID 6297650.
- PMID 17804020.
- S2CID 25515856.
- ISBN 978-1-58562-309-9.
- PMID 1815068.
- ^ ISBN 978-0-08-046212-7.
- ^ ISBN 978-0-471-04392-8.
- ^ PMID 19557250.
- ^ ISBN 978-0-7817-2845-4.
- ISBN 978-0-7514-0499-9.
- ^ Jensen L. "Drug Shortage Detail: Maprotiline Tablets". www.ashp.org. American Society of Health-System Pharmacists. Retrieved 22 October 2023.
