Mitral regurgitation
| Mitral regurgitation | |
|---|---|
| Other names | Mitral incompetence, mitral insufficiency |
 | |
| Mitral regurgitation (schematic drawing) During systole, contraction of the left ventricle causes abnormal backflow (arrow) into the left atrium. 1 Mitral valve 2 Left ventricle 3 Left atrium 4 Aorta | |
| Specialty | Cardiology |
| Symptoms | Heart murmur, shortness of breath during exercise or lying down, fatigue, palpitations, swollen feet or ankles[1] |
| Complications | In severe cases: congestive heart failure, arrhythmias (atrial fibrillation), pulmonary hypertension[1] |
| Types | Acute mitral regurgitation, chronic compensated mitral regurgitation, chronic decompensated mitral regurgitation[2] |
| Causes | mitral valve prolapse, ageing, rheumatic fever, mitral annular calcification, infective endocarditis, hypertrophic cardiomyopathy[2] |
| Treatment | Medication, Mitral valve repair, Mitral valve replacement, MitraClip |
Mitral regurgitation (MR), also known as mitral insufficiency or mitral incompetence, is a form of
Definition
Mitral regurgitation, also known as mitral insufficiency or mitral incompetence, is the backward flow of blood from the
Signs and symptoms
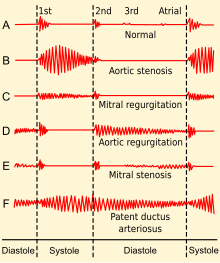
Mitral regurgitation may be present for many years before any symptoms appear.
Individuals with chronic compensated MR may be asymptomatic for long periods of time, with a normal exercise tolerance and no evidence of heart failure. Over time, however, there may be decompensation and patients can develop volume overload (congestive heart failure). Symptoms of entry into a decompensated phase may include fatigue, shortness of breath particularly on exertion, and leg swelling. Also, there may be development of an irregular heart rhythm known as atrial fibrillation.[6]
Findings on clinical examination depend on the severity and duration of MR. The mitral component of the
Patients with mitral valve prolapse may have a holosystolic murmur or often a mid-to-late systolic click and a late systolic murmur. Cases with a late systolic regurgitant murmur may still be associated with significant hemodynamic consequences.[8]
Mitral regurgitation as a result of papillary muscle damage or rupture may be a complication of a
Cause

The mitral valve apparatus comprises two valve leaflets, the
The most common cause of MR in developed countries is mitral valve prolapse.[10] It is the most common cause of primary mitral regurgitation in the United States, causing about 50% of cases. Myxomatous degeneration of the mitral valve is more common in women as well as with advancing age, which causes a stretching of the leaflets of the valve and the chordae tendineae. Such elongation prevents the valve leaflets from fully coming together when the valve closes, causing the valve leaflets to prolapse into the left atrium, thereby causing MR.[citation needed]
Secondary mitral regurgitation is due to the dilatation of the
Acute MR is most often caused by endocarditis, mainly S. aureus.[6] Rupture or dysfunction of the papillary muscle are also common causes in acute cases,[6] dysfunction, which can include mitral valve prolapse.[7]
Pathophysiology
The pathophysiology of MR can be broken into three phases of the disease process: the acute phase, the chronic compensated phase, and the chronic decompensated phase.[citation needed]

Acute phase
Acute MR (as may occur due to the sudden rupture of the
In the acute setting, the stroke volume of the left ventricle is increased (increased
The regurgitant volume causes a volume overload and a
Chronic phase
Compensated
If the MR develops slowly over months to years or if the acute phase cannot be managed with medical therapy, the individual will enter the chronic compensated phase of the disease. In this phase, the left ventricle develops eccentric hypertrophy in order to better manage the larger than normal stroke volume. The eccentric hypertrophy and the increased diastolic volume combine to increase the stroke volume (to levels well above normal) so that the forward stroke volume (forward cardiac output) approaches the normal levels.In the left atrium, the volume overload causes enlargement of the left atrium, allowing the filling pressure in the left atrium to decrease. This improves the drainage from the pulmonary veins, and signs and symptoms of pulmonary congestion will decrease.[citation needed]
These changes in the left ventricle and left atrium improve the low forward cardiac output state and the pulmonary congestion that occur in the acute phase of the disease. Individuals in the chronic compensated phase may be asymptomatic and have normal exercise tolerances.[15]
Decompensated
An individual may be in the compensated phase of MR for years, but will eventually develop left ventricular dysfunction, the hallmark for the chronic decompensated phase of MR. It is currently unclear what causes an individual to enter the decompensated phase of this disease. However, the decompensated phase is characterized by calcium overload within the cardiac
In this phase, the ventricular myocardium is no longer able to contract adequately to compensate for the volume overload of mitral regurgitation, and the stroke volume of the left ventricle will decrease. The decreased stroke volume causes a decreased forward cardiac output and an increase in the
The left ventricle begins to dilate during this phase. This causes a dilatation of the mitral valve annulus, which may worsen the degree of MR. The dilated left ventricle causes an increase in the wall stress of the cardiac chamber as well.While the ejection fraction is less in the chronic decompensated phase than in the acute phase or the chronic compensated phase, it may still be in the normal range (i.e.: > 50 percent), and may not decrease until late in the disease course. A decreased ejection fraction in an individual with MR and no other cardiac abnormality should alert the physician that the disease may be in its decompensated phase.[citation needed]
Diagnosis
There are many diagnostic tests that have abnormal results in the presence of MR. These tests suggest the diagnosis of MR and may indicate to the physician that further testing is warranted. For instance, the
| Acute | Chronic | |
|---|---|---|
Electrocardiogram
|
Normal | P mitrale, Atrial fibrillation, left ventricular hypertrophy |
| Heart size | Normal | Cardiomegaly, left atrial enlargement |
| Systolic murmur | Heard at the base, radiates to the neck, spine, or top of head | Heard at the apex, radiates to the axilla |
| Apical thrill | May be absent | Present |
| Jugular venous distension | Present | Absent |
The quantification of MR usually employs
Chest X-ray
The chest X-ray in individuals with chronic MR is characterized by enlargement of the left atrium and the left ventricle, and then maybe calcification of the mitral valve.[16]
Echocardiogram


|

|
| Severe MR | Legend |
| 1 Left atrium (LA) – 2 MR Jet, LV Left ventricle – RV Right ventricle – RA Right atrium | |
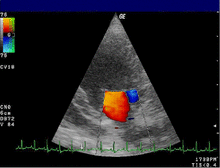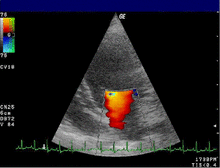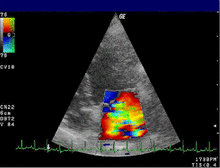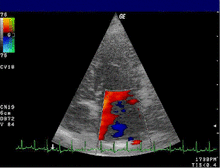
An
Electrocardiography
P mitrale is a broad, bifid notched P wave in several or many leads with a prominent late negative component to the P wave in lead V1, and may be seen in MR, but also in mitral stenosis, and, potentially, any cause of overload of the left atrium.[18]
Quantification of mitral regurgitation
The degree of severity of MR can be quantified by the
- regurgitant fraction =
where Vmitral and Vaortic are, respectively, the volumes of blood that flow forward through the mitral valve and aortic valve during a cardiac cycle. Methods that have been used to assess the regurgitant fraction in mitral regurgitation include echocardiography, cardiac catheterization, fast CT scan, and cardiac MRI.The echocardiographic technique to measure the regurgitant fraction is to determine the forward flow through the mitral valve (from the left atrium to the left ventricle) during ventricular
Another way to quantify the degree of MR is to determine the area of the regurgitant flow at the level of the valve. This is known as the regurgitant orifice area and correlates with the size of the defect in the mitral valve. One particular echocardiographic technique used to measure the orifice area is measurement of the proximal isovelocity surface area (PISA). The flaw of using PISA to determine the mitral valve regurgitant orifice area is that it measures the flow at one moment in time in the cardiac cycle, which may not reflect the average performance of the regurgitant jet.[citation needed]

| Grade[19] | Degree of mitral regurgitation | Regurgitant fraction | Regurgitant Orifice area |
|---|---|---|---|
| 1 | Mild | < 20 percent | |
| 2 | Moderate | 20 - 40 percent | |
| 3 | Moderate to severe | 40 - 60 percent | |
| 4 | Severe | > 60 percent | > 0.4 cm2 |
Treatment
The treatment of MR depends on the acuteness of the disease and whether there are associated signs of hemodynamic compromise. In general, medical therapy is non-curative and is used for mild-to-moderate regurgitation or in patients unable to tolerate surgery.[15]
In acute MR secondary to a mechanical defect in the heart (i.e., rupture of a papillary muscle or chordae tendineae), the treatment of choice is mitral valve surgery. If the patient is hypotensive prior to the surgical procedure, an intra-aortic balloon pump may be placed in order to improve perfusion of the organs and to decrease the degree of MR.[6]
Medicine
If the individual with acute MR is normotensive,
Individuals with chronic MR can be treated with vasodilators as well to decrease afterload.
Surgery
Surgery is curative of mitral valve regurgitation. There are two surgical options for the treatment of MR: mitral valve replacement and mitral valve repair.[6] Mitral valve repair is preferred to mitral valve replacement where a repair is feasible as bioprosthetic replacement valves have a limited lifespan of 10 to 15 years, whereas synthetic replacement valves require ongoing use of blood thinners to reduce the risk of stroke. There are two general categories of approaches to mitral valve repair: resection of the prolapsed valvular segment (sometimes referred to as the "Carpentier" approach) and installation of artificial chordae to "anchor" the prolapsed segment to the papillary muscle (sometimes referred to as the "David" approach). With the resection approach, any prolapsing tissue is resected, in effect removing the hole through which the blood is leaking. In the artificial chordae approach, ePTFE (expanded polytetrafluoroethylene, or Gore-Tex) sutures are used to replace the broken or stretched chordae tendonae, bringing the natural tissue back into the physiological position, thus restoring the natural anatomy of the valve. With both techniques, an annuloplasty ring is typically secured to the annulus, or opening of the mitral valve, to provide additional structural support. In some cases, the "double orifice" (or 'Alfieri') technique for mitral valve repair, the opening of the mitral valve is sewn closed in the middle, leaving the two ends still able to open. This ensures that the mitral valve closes when the left ventricle pumps blood, yet allows the mitral valve to open at the two ends to fill the left ventricle with blood before it pumps. In general, mitral valve surgery requires "open-heart" surgery in which the heart is arrested and the patient is placed on a heart-lung machine (cardiopulmonary bypass). This allows the complex surgery to proceed in a still environment.[citation needed]
Due to the physiological stress associated with open-heart surgery, elderly and very sick patients may be subject to increased risk, and may not be candidates for this type of surgery. As a consequence, there are attempts to identify means of correcting MR on a beating heart. The Alfieri technique for instance, has been replicated using a percutaneous catheter technique, which installs a "MitraClip" device to hold the middle of the mitral valve closed.[23][24]
Indications for surgery for chronic MR include signs of left ventricular dysfunction with ejection fraction less than 60%, severe pulmonary hypertension with pulmonary artery systolic pressure greater than 50 mmHg at rest or 60 mmHg during activity, and new-onset atrial fibrillation.[citation needed]
| Symptoms | LV EF | LVESD |
|---|---|---|
| NYHA II | > 30 percent | < 55 mm |
| NYHA III-IV | < 30 percent | > 55 mm |
| Asymptomatic | 30 - 60 percent | ≥ 40 mm |
| Asymptomatic with pulmonary hypertension | LV EF > 60 percent and pulmonary artery systolic pressure >50-60 mmHg | |
| Asymptomatic and chance for a repair without residual MR is >90% | > 60 percent | < 40 mm |
Epidemiology
Significant mitral valve regurgitation has a
In a study of 595 male elite football players aged 18–38 and 47 sedentary non-athletes, mitral regurgitation was found in 20% football players and 15% in control group. Football players with mitral regurgitation were found to have larger mitral annulus diameter compared to athletes without regurgitation, and left atrium diameter was larger in athletes with MR.[28]
See also
- Tricuspid regurgitation
- Aortic regurgitation
- Pulmonary insufficiency
References
- ^ a b c "Mitral valve regurgitation - Symptoms and causes". Mayo Clinic. Retrieved 2021-12-01.
- ^ a b "Mitral Regurgitation: Practice Essentials, Background, Pathophysiology". 2021-11-05.
{{cite journal}}: Cite journal requires|journal=(help) - ^ PMID 31985928. Retrieved 19 December 2021.
- ^ Mount Sinai Hospital
- ^ a b "What is mitral regurgitation? | Heart Disease". patient.info. Retrieved 15 February 2021.
- ^ ISBN 978-0-7817-7153-5. Chapter 1: Diseases of the Cardiovascular system > Section: Valvular Heart Disease
- ^ a b c d e f g VOC=VITIUM ORGANICUM CORDIS, a compendium of the Department of Cardiology at Uppsala Academic Hospital. By Per Kvidal September 1999, with revision by Erik Björklund May 2008
- S2CID 44385990.
- ISBN 9780071748872.
- ^ Kulick, Daniel. "Mitral Valve Prolapse (MVP)". MedicineNet.com. MedicineNet, Inc. Retrieved 2010-01-18.
- ^ [1] NIH US National Library of Medicine, A.D.A.M. Medical Encyclopedia, Ehlers Danlos Syndrome- PMH0002439
- ^ Functional mitral regurgitation Archived 2010-08-22 at the Wayback Machine By William H Gaasch, MD. Retrieved on Jul 8, 2010
- ^ a b "Aortic Regurgitation". The Lecturio Medical Concept Library. October 2020. Retrieved 29 June 2021.
- ^ Harrison's Internal Medicine 17th edition
- ^ a b c "Mitral Regurgitation". The Lecturio Medical Concept Library. Retrieved 11 August 2021.
- ^ ISBN 0-702-02579-8.
- ^ "Transoesophageal echocardiogram (TOE) | Royal Brompton & Harefield hospitals". www.rbht.nhs.uk. Retrieved 19 December 2021.
- ^ medilexicon.com < P mitrale Archived 2011-11-03 at the Wayback Machine Citing. Stedman's Medical Dictionary. Copyright 2006
- PMID 28314623.
- ^ "Sodium Nitroprusside". The American Society of Health-System Pharmacists. Archived from the original on 21 December 2016. Retrieved 8 December 2016.
- PMID 668075.
- S2CID 40731762.
- PMID 18262841.
- S2CID 205092586.
- PMID 18820172.
- ^ The Cleveland Clinic Center for Continuing Education > Mitral Valve Disease: Stenosis and Regurgitation Authors: Ronan J. Curtin and Brian P. Griffin. Retrieved September 2010
- ^ Valvular heart disease in elderly adults Authors: Dania Mohty, Maurice Enriquez-Sarano. Section Editors:Catherine M Otto, Kenneth E Schmader. Deputy Editor: Susan B Yeon. This topic last updated: April 20, 2007. Last literature review version 18.2: May 2010
- S2CID 2631112.


