Mitral stenosis
| Mitral stenosis | |
|---|---|
hypertrophy. Superior view. Autopsy preparation. | |
| Specialty | Cardiology |
| Symptoms |
Late Stage:
|
| Causes | mitral valvuloplasty |
Mitral stenosis is a
Signs and symptoms

Signs and symptoms of mitral stenosis include the following:
- paroxysmal nocturnal dyspnea (PND)[3]
- Palpitations[3]
- Chest pain[3]
- Hemoptysis[3]
- Thromboembolism[3] in later stages when the left atrial volume is increased (i.e., dilation). The latter leads to increase risk of atrial fibrillation, which increases the risk of blood stasis (motionless). This increases the risk of coagulation.
- Ascites and edema and hepatomegaly (if right-side heart failure develops)[3]
Fatigue and weakness increase with exercise and pregnancy.[3]
Natural history
The natural history of mitral stenosis secondary to rheumatic fever (the most common cause) is an asymptomatic latent phase following the initial episode of rheumatic fever. This latent period lasts an average of 16.3 ± 5.2 years. Once symptoms of mitral stenosis begin to develop, progression to severe disability takes 9.2 ± 4.3 years.[citation needed]
In individuals having been offered mitral valve surgery but refused, survival with medical therapy alone was 44 ± 6% at 5 years, and 32 ± 8% at 10 years after they were offered correction.[4]
Cause
Almost all cases of mitral stenosis are due to disease in the heart secondary to
Other causes include infective endocarditis where the vegetations may favor increase risk of stenosis. Other rare causes include mitral annular calcification, endomyocardial fibroelastosis, malignant carcinoid syndrome, systemic lupus erythematosus, whipple disease, fabry disease, and rheumatoid arthritis.[9] hurler' disease, hunter's disease, amyloidosis.
Pathophysiology

The normal area of the mitral valve orifice is about 4 to 6 cm2. In normal cardiac physiology, the
When the mitral valve area goes below 2 cm2, the valve causes an impediment to the flow of blood into the left ventricle, creating a pressure gradient across the mitral valve. This gradient may be increased by increases in the heart rate or cardiac output. As the gradient across the mitral valve increases, the amount of time necessary to fill the left ventricle with blood increases. Eventually, the left ventricle requires the atrial kick to fill with blood. As the heart rate increases, the amount of time that the ventricle is in diastole and can fill up with blood (called the diastolic filling period) decreases. When the heart rate goes above a certain point, the diastolic filling period is insufficient to fill the ventricle with blood and pressure builds up in the left atrium, leading to pulmonary congestion.[citation needed]
When the mitral valve area goes less than 1 cm2, there will be an increase in the left atrial pressures (required to push blood through the stenotic valve). Since the normal left ventricular diastolic pressures is about 5 mmHg, a pressure gradient across the mitral valve of 20 mmHg due to severe mitral stenosis will cause a left atrial pressure of about 25 mmHg. This left atrial pressure is transmitted to the pulmonary vasculature and causes
The constant pressure overload of the left atrium will cause the left atrium to increase in size. As the left atrium increases in size, it becomes more prone to develop atrial fibrillation (AF).
In individuals with severe mitral stenosis, the left ventricular filling is dependent on the atrial kick. The loss of the atrial kick due to atrial fibrillation (i.e., blood cannot flow into the left ventricle thus accumulating in the left atrium ) can cause a precipitous decrease in cardiac output and sudden congestive heart failure.[citation needed]
Patients with mitral stenosis prompts a series of hemodynamic changes that frequently cause deterioration of the patient's clinical status. A reduction in cardiac output, associated with acceleration of heart rate and shortening of the diastolic time, frequently leads to congestive heart failure. In addition, when AF sets in, systemic embolization becomes a real danger.[10]
Mitral stenosis typically progresses slowly (over decades) from the initial signs of mitral stenosis to NYHA functional class II symptoms to the development of atrial fibrillation to the development of NYHA functional class III or IV symptoms. Once an individual develops NYHA class III or IV symptoms, the progression of the disease accelerates and the patient's condition deteriorates.[citation needed]
Diagnosis
Physical examination
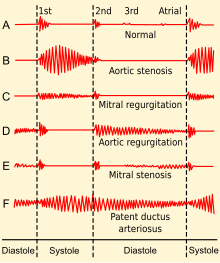
Upon
If
An opening snap that is a high-pitch additional sound may be heard after the A2 (aortic) component of the second heart sound (S2), which correlates to the forceful opening of the mitral valve. The mitral valve opens when the pressure in the left atrium is greater than the pressure in the left ventricle. This happens in ventricular diastole (after closure of the aortic valve), when the pressure in the ventricle precipitously drops. In individuals with mitral stenosis, the pressure in the left atrium correlates with the severity of the mitral stenosis. As the severity of the mitral stenosis increases, the pressure in the left atrium increases, and the mitral valve opens earlier in ventricular diastole.[3]
A mid-diastolic rumbling
Advanced disease may present with signs of
Almost all signs increase with exercise and pregnancy.[3]
Other peripheral signs include:
- Malar flush - due to back pressure and buildup of carbon dioxide (CO2). CO2 is a natural vasodilator.[12]
- Atrial fibrillation - irregular pulse and loss of 'a' wave in jugular venous pressure
- Left parasternal heave - presence of right ventricular hypertrophy due to pulmonary hypertension
- Tapping apex beat that is not displaced
Heart rate is about 100-150/min. Irregularly irregular pulse with a pulse deficit>10. Varying first heart sound intensity. Opening snap is not heard sometimes. Absent a waves in the neck veins. Presystolic accentuation of diastolic murmur disappears. Embolic manifestations may appear.[citation needed]
Associated lesions
With severe pulmonary hypertension, a pansystolic murmur produced by functional tricuspid regurgitation may be audible along the left sternal border. This murmur is usually louder during inspiration and diminishes during forced expiration (Carvallo's sign). When the cardiac output is markedly reduced in MS, the typical auscultatory findings, including the diastolic rumbling murmur, may not be detectable (silent MS), but they may reappear as compensation is restored. The Graham Steell murmur of pulmonary regurgitation, a high-pitched, diastolic, decrescendo blowing murmur along the left sternal border, results from dilation of the pulmonary valve ring and occurs in patients with mitral valve disease and severe pulmonary hypertension. This murmur may be indistinguishable from the more common murmur produced by aortic regurgitation (AR), although it may increase in intensity with inspiration and is accompanied by a loud and often palpable P2. [13]
Echocardiography
| Degree of mitral stenosis | Mean gradient | Mitral valve area |
|---|---|---|
| Progressive mitral stenosis | <5 mmHg | >1.5 cm2 |
| Severe mitral stenosis | 5–10 mmHg | 1.0–1.5 cm2 |
| Very severe mitral stenosis | > 10 mmHg | < 1.0 cm2 |
In most cases, the diagnosis of mitral stenosis is most easily made by
Cardiac chamber catheterization
Another method of measuring the severity of mitral stenosis is the simultaneous left and right
Other techniques
Electrocardiography may show P mitrale, that is, broad, notched P waves in several or many leads with a prominent late negative component to the P wave in lead V1, and may also be seen in mitral regurgitation, and, potentially, any cause of overload of the left atrium.[14] Thus, P-sinistrocardiale may be a more appropriate term.[14]
Treatment
Treatment is not necessary in asymptomatic patients.[3]
The treatment options for mitral stenosis include mitral valve replacement by surgery, and percutaneous mitral valvuloplasty by balloon catheter.[15]
The indication for invasive treatment with either a mitral valve replacement or valvuloplasty is NYHA functional class III or IV symptoms.[citation needed]
Another option is balloon dilatation.
Treatment also focuses on concomitant conditions often seen in mitral stenosis:
- Any angina is treated with short-acting calcium blockers[11]
- Any beta-blockers[11]
- Any heart failure is treated with digoxin, diuretics, nitrovasodilators and, if not contraindicated, cautious inpatient administration of ACE inhibitors[11]

Mitral valvuloplasty
Mitral valvuloplasty is a minimally invasive therapeutic procedure to correct an uncomplicated mitral stenosis by dilating the valve using a balloon. Under
With careful patient pre-selection, percutaneous balloon mitral valvuloplasty (PBMV) is associated with good success rates and a low rate of complications. By far the most serious adverse event is the occurrence of acute severe mitral regurgitation. Severe mitral regurgitation usually results from a tear in one of the valve leaflets or the subvalvular apparatus. It can lead to pulmonary edema and hemodynamic compromise, necessitating urgent surgical mitral valve replacement.[citation needed]
Other serious complications with PBMV usually relate to the technique of trans-septal puncture (TSP). The ideal site for TSP is the region of the fossa ovalis in the inter-atrial septum. Occasionally, however, the sharp needle used for TSP may inadvertently traumatize other cardiac structures, leading to cardiac tamponade or serious blood loss.[citation needed]
Although the immediate results of PBMV are often quite gratifying, the procedure does not provide permanent relief from mitral stenosis. Regular follow-up is mandatory, to detect restenosis. Long-term follow-up data from patients undergoing PBMV indicates that up to 70–75% individuals can be free of restenosis 10 years following the procedure. The number falls to about 40% 15 years post-PBMV.[18]
References
- PMID 16027271.
- ISBN 9780702050473.
- ^ ISBN 978-0-7817-7153-5.
- ^ "Los 13 mejores consejos para dejar de fumar". cursoenarm.net. Archived from the original on 2016-11-13.
- ^ "Mitral Stenosis: Heart Valve Disorders: Merck Manual Home Edition". Archived from the original on 2009-03-02. Retrieved 2009-03-14.
- ^ Bertazzo, S. et al. Nano-analytical electron microscopy reveals fundamental insights into human cardiovascular tissue calcification. Nature Materials 12, 576-583 (2013).
- ^ Miller, J. D. Cardiovascular calcification: Orbicular origins. Nature Materials 12, 476-478 (2013).
- PMID 18007005.
- ISBN 978-1-4377-0398-6.
- ^ American Heart Journal[full citation needed]
- ^ a b c d VOC=VITIUM ORGANICUM CORDIS, a compendium of the Department of Cardiology at Uppsala Academic Hospital. By Per Kvidal September 1999, with revision by Erik Björklund May 2008
- ^ "Mitral Stenosis: Valvular Disorders: Merck Manual Professional". Merckmanuals.com. Archived from the original on 2014-08-19. Retrieved 2013-02-21.
- ISBN 978-1-25-964404-7.
- ^ a b medilexicon.com < P mitrale Archived 2011-11-03 at the Wayback Machine Citing. Stedman's Medical Dictionary. Copyright 2006
- ^ "Mitral Stenosis". The Lecturio Medical Concept Library. Retrieved 11 August 2021.
- PMID 3190958.
- PMID 2372892.
- PMID 17944115.
