Multiple myeloma
| Multiple myeloma | |
|---|---|
| Other names | Plasma cell myeloma, myelomatosis, Kahler's disease, myeloma |
| Prognosis | Five-year survival rate 54% / life expectancy 6 years (USA)[7] |
| Frequency | 488,200 (affected during 2015)[8] |
| Deaths | 101,100 (2015)[9] |
Multiple myeloma (MM), also known as plasma cell myeloma and simply myeloma, is a
The cause of multiple myeloma is unknown.
Multiple myeloma is considered treatable, but generally incurable.
Globally, about 175,000 people were diagnosed with the disease in 2020, while about 117,000 people died from the disease that year. In the U.S., forecasts suggest about 35,000 people will be diagnosed with the disease in 2023, and about 12,000 people will die from the disease that year.[16] In 2020, there were an estimated 170,405 people living with myeloma in the U.S.[17]
It is difficult to judge mortality statistics because treatments for the disease are advancing rapidly. Based on data concerning people diagnosed with the disease between 2013 and 2019, about 60% lived five years or more post-diagnosis, with about 34% living ten years or more.[17] People newly diagnosed with the disease now have a better outlook, due to improved treatments.[18]
The disease usually occurs around the age of 60 and is more common in men than women.[6] It is uncommon before the age of 40.[6] The word myeloma is from Greek myelo- 'marrow' and -oma 'tumor'.[19]
Signs and symptoms
Because many organs can be affected by myeloma, the symptoms and signs vary greatly. Fatigue and bone pain are the most common symptoms at presentation. The CRAB criteria were formerly the benchmark used to establish presence of active multiple myeloma (as opposed to an earlier, generally asymptomatic, "smoldering" form of the disease). The CRAB criteria are:[20][2][21]
- Calcium: serum calcium >0.25 mmol/L (>1 mg/dL) higher than the upper limit of normal or >2.75 mmol/L (>11 mg/dL)
- Renal insufficiency: creatinine clearance <40 mL per minute or serum creatinine >1.77 mol/L (>2 mg/dL)
- Anemia: hemoglobin value of >2g/dL below the lowest limit of normal, or a hemoglobin value <10g/dL
- Bone lesions: osteolytic lesions on skeletal radiography, CT, or PET/CT
As of 2014[update] the diagnostic criteria were expanded and updated by the IMWG (International Myeloma Working Group) to add three myeloma defining events, any one of which indicates presence of active multiple myeloma. Each of these three events may occur before any of the CRAB criteria appears, thereby making more people eligible for treatment with myeloma drugs earlier.[21]
Bone pain

Bone pain affects almost 70% of people with multiple myeloma and is one of the most common symptoms.
Anemia
The anemia found in myeloma is usually
Impaired kidney function
Impaired
The most common cause of kidney failure in multiple myeloma is due toLight chains produce myriad effects that can manifest as the Fanconi syndrome (type II kidney tubular acidosis).[27]
Infection
Collateral infections are common with multiple myeloma, since the disease impairs functioning of blood components that normally resist pathogens. The most common infections are pneumonias, urinary tract infections, and sepsis.[29] The greatest risk period for the occurrence of infection is in the initial few months after the start of a new drug therapy, since many drug therapies further suppress the normal immune response.[30]
Infections (and "adverse events" for all diseases) are graded by a standardized scale.[31] With some myeloma drug therapies, over 30% of people experience a "Grade 3" or higher infection (many people experience multiple such infections),[32] calling for intervention at least by antibiotics.[31] Of people who die within 6 months of their myeloma diagnosis, between 20% and 50% die from collateral infections.[29]
Clinical evaluation of a person's immune response is typically performed by a lab test that measures the levels of different
Neurological symptoms
Some symptoms (e.g.,
When the disease is well-controlled, neurological symptoms may result from current treatments, some of which may cause peripheral neuropathy, manifesting itself as numbness or pain in the hands, feet, and lower legs.[citation needed]
Mouth
The initial symptoms may involve pain, numbness, swelling, expansion of the jaw, tooth mobility, and
Cause
The cause of multiple myeloma is generally unknown.[4]
Risk factors
- Monoclonal gammopathy of undetermined significance (MGUS) increases the risk of developing multiple myeloma. MGUS transforms to multiple myeloma at the rate of 1% to 2% per year, and almost all cases of multiple myeloma are preceded by MGUS.[38]
- Obesity is related to multiple myeloma with each increase of body mass index by five increasing the relative risk by 11%. In addition, studies have shown a positive correlation between BMI and adhesion of multiple myeloma cells.[41]
Studies have reported a familial predisposition to myeloma.[42][43] Hyperphosphorylation of a number of proteins—the paratarg proteins—a tendency that is inherited in an autosomal dominant manner, appears a common mechanism in these families. This tendency is more common in African-American with myeloma and may contribute to the higher rates of myeloma in this group.[42]
Occupations
In a study to investigate the association between occupational exposure to aromatic hydrocarbon solvents (Benzene and its many derivatives), evidence has shown that these solvents have a role in causation of multiple myeloma.[14] The occurrence of multiple myeloma may occur more in certain occupations. The risk of multiple myeloma occurring is greater in occupations as a firefighter, as a hairdresser, and in agricultural and industrial occupations.[44] The risk in certain occupations is due to the exposure of different chemicals. Repeated exposure to chemicals increases risk of multiple myeloma. The use of pesticides and hazardous chemicals in occupations, like firefighting and agriculture have been seen to cause an increase of risk for multiple myeloma.[13] Other occupations, such as the industrial occupations, are also at increased risk for multiple myeloma. Industrial workers are exposed to chemicals that have aromatic hydrocarbon solvents in them.[14][13]
Exposure to aromatic hydrocarbon solvents, benzene, toluene, and xylene, can increase risk of multiple myeloma. Increased duration, high intensity of exposure, or repeated exposure was associated with an increased risk of multiple myeloma by up to 63%.[14] The time from exposure to diagnosis was studied, and diagnosis after exposure lagged at least 20 years.[14] When exposure to one chemical was identified, there was usually exposure to another hydrocarbon solvent identified.[14] Multiple myeloma affects more men, older adults, and African Americans. These populations also have higher exposure frequencies than their female counterparts.[14]
Epstein–Barr virus
Rarely,
Pathophysiology
Multiple myeloma develops in B lymphocytes after they have left the part of the lymph node known as the
The immune system keeps the proliferation of B cells and the secretion of antibodies under tight control. When chromosomes and genes are damaged, often through rearrangement, this control is lost. Often, a promoter gene moves (or translocates) to a chromosome, where it stimulates an antibody gene to overproduction.[citation needed]
A chromosomal translocation between the immunoglobulin heavy chain gene (on chromosome 14, locus q32) and an oncogene (often 11q13, 4p16.3, 6p21, 16q23 and 20q11[50]) is frequently observed in people with multiple myeloma. This mutation results in dysregulation of the oncogene which is thought to be an important initiating event in the pathogenesis of myeloma.[51] The result is a proliferation of a plasma cell clone and genomic instability that leads to further mutations and translocations. The chromosome 14 abnormality is observed in about 50% of all cases of myeloma. Deletion of (parts of) chromosome 13 is also observed in about 50% of cases.
Production of cytokines[52] (especially IL-6) by the plasma cells causes much of their localized damage, such as osteoporosis, and creates a microenvironment in which the malignant cells thrive. Angiogenesis (the generation of new blood vessels) is increased.[citation needed]
The produced antibodies are deposited in various organs, leading to kidney failure, polyneuropathy, and various other myeloma-associated symptoms.
Epigenetics
In a study that investigated the DNA methylation profile of multiple myeloma cells and normal plasma cells, a gradual demethylation from stem cells to plasma cells was observed. The observed methylation pattern of CpG within intronic regions with enhancer-related chromatin marks in multiple myeloma is similar to undifferentiated precursor and stem cells. These results may represent a de novo epigenetic reprogramming in multiple myeloma, leading to the acquisition of a methylation pattern related to stemness.[53] Other studies have identified a multiple myeloma specific gene silencing pattern associated with the polycomb repressive complex 2 (PRC2).[54][55] Increased expression of the PRC2 subunit, EZH2 have been described to be a common feature in multiple myeloma, resulting in an accumulation and redistribution of histone H3 lysine 27 trimethylation which advances with disease severity.[56]
Genetics
Chromosomal abnormalities commonly found in this disease, like trisomy of multiple odd-numbered chromosomes, t(11;14), and del(13q), are not associated with a worse prognosis. However, about 25% of patients with newly diagnosed disease have abnormalities associated with a worse prognosis, like t(4;14), t(14;16), and del(17p). Other less common abnormalities associated with a worse prognosis include t(14;20) and ≥4 copies of 1q.[57]: 1730–1
Associated genetic mutations include
Development
The genetic and epigenetic changes occur progressively. The initial change, often involving one chromosome 14 translocation, establishes a clone of bone marrow plasma cells that causes the asymptomatic disorder
Subsequent genetic and epigenetic changes lead to a new, more aggressive clone of plasma cells, which cause further rises in the level of the circulating myeloma protein, further rises in the number of bone marrow plasma cells, or the development of one or more of a specific set of "CRAB" symptoms, which are the basis for diagnosing malignant multiple myeloma and treating the disease.[citation needed]
In a small percentage of multiple myeloma cases, further genetic and epigenetic changes lead to the development of a plasma cell clone that moves from the bone marrow into the
Monoclonal gammopathy of undetermined significance → smoldering multiple myeloma → multiple myeloma → plasma cell leukemia
Being asymptomatic, monoclonal gammopathy of undetermined significance and smoldering multiple myeloma are typically diagnosed fortuitously by detecting a myeloma protein on serum protein electrophoresis tests done for other purposes. MGUS is a relatively stable condition afflicting 3% of people aged 50 and 5% of people aged 70; it progresses to multiple myeloma at a rate of 0.5–1% cases per year; smoldering multiple myeloma does so at a rate of 10% per year for the first 5 years, but then falls off sharply to 3% per year for the next 5 years and thereafter to 1% per year.[39][40]
Overall, some 2–4% of multiple myeloma cases eventually progress to plasma cell leukemia.[59]
Diagnosis
Blood tests
The globulin level may be normal in established disease. A doctor may request
In theory, multiple myeloma can produce all classes of immunoglobulin, but
Additional findings may include a raised calcium level (when
Other useful laboratory tests include quantitative measurement of IgA, IgG, and IgM to look for immune paresis, and beta-2 microglobulin, which provides prognostic information. On peripheral blood smear, the
The recent introduction of a commercial immunoassay for measurement of free light chains potentially offers an improvement in monitoring disease progression and response to treatment, particularly where the paraprotein is difficult to measure accurately by electrophoresis (for example in light chain myeloma, or where the paraprotein level is very low). Initial research also suggests that measurement of free light chains may also be used, in conjunction with other markers, for assessment of the risk of progression from MGUS to multiple myeloma.[63]
This assay, the serum free light chain assay, has recently been recommended by the
-
Bone marrow aspirate showing the histologic correlate of multiple myeloma under the microscope, H&E stain
-
Plasmacytoma, H&E stain
-
PAS stain.
-
Atypical plasma cell infiltrate with both Russell (cytoplasmic) and Dutcher (nuclear) bodies (H&E, 50x)
Histopathology
A
The plasma cells seen in multiple myeloma have several possible morphologies. First, they could have the appearance of a normal plasma cell, a large cell two or three times the size of a peripheral lymphocyte. Because they are actively producing antibodies, the Golgi apparatus typically produces a light-colored area adjacent to the nucleus, called a perinuclear halo. The single nucleus (with inside a single nucleolus with vesicular nuclear chromatin) is eccentric, displaced by an abundant cytoplasm. Other common morphologies seen, but which are not usual in normal plasma cells, include:
- Bizarre cells, which are multinucleated
- Mott cells, containing multiple clustered cytoplasmic droplets or other inclusions (sometimes confused with Auer rods, commonly seen in myeloid blasts)
- Flame cells, having a fiery red cytoplasm[65][66]
Historically, the CD138 has been used to isolate myeloma cells for diagnostic purposes. However, this antigen disappears rapidly ex vivo. Recently, however, the surface antigen
The prognosis varies widely depending upon various risk factors. The Mayo Clinic has developed a risk-stratification model termed Mayo Stratification for Myeloma and Risk-adapted Therapy (mSMART), which divides people into high-risk and standard-risk categories.
Medical imaging
The diagnostic examination of a person with suspected multiple myeloma typically includes a
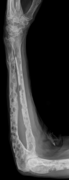
-
X-ray of the forearm, with lytic lesions
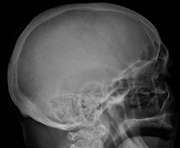
-
Skull X-ray showing multiple lucencies due to multiple myeloma
-
Multiple myeloma in the upper arm
-
Pathological fracture of the lumbar spine due to multiple myeloma
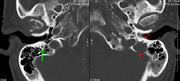
-
Apetrous temporal bones involving the mastoid segment of the facial nervecanal. Red arrows: lesion; green arrow: normal contralateral facial nerve canal. The lesions are consistent with a myeloma deposit.
-
CT scan of the lower vertebral column in a man with multiple myeloma, showing multiple osteoblastic lesions: These are morecancellous bone, in contrast to osteolytic lesions, which are less radiodense.
-
Femur with multiple myeloma lesions
-
Same femur before myeloma lesions for comparison
-
Humerus with multiple myeloma lesions
-
Same humerus before, with just subtle lesions
Diagnostic criteria
In 2003, the IMG[20] agreed on diagnostic criteria for symptomatic myeloma, asymptomatic myeloma, and MGUS, which was subsequently updated in 2009:[72]
- Symptomatic myeloma (all three criteria must be met):
- Clonal plasma cells >10% on bone marrow biopsy or (in any quantity) in a biopsy from other tissues (plasmacytoma)
- A monoclonalprotein (myeloma protein) in either serum or urine and it has to be more than 3g/dL (except in cases of true nonsecretory myeloma)
- Evidence of end-organ damage felt related to the plasma cell disorder (related organ or tissue impairment, CRAB):
- HyperCalcemia(corrected calcium >2.75 mmol/L, >11 mg/dL)
- Renal failure(kidney insufficiency) attributable to myeloma
- Anemia (hemoglobin <10 g/dL)
- Bone lesions(lytic lesions or osteoporosis with compression fractures)
Note: Recurrent infections alone in a person who has none of the CRAB features is not sufficient to make the diagnosis of myeloma. People who lack CRAB features, but have evidence of amyloidosis, should be considered as amyloidosis and not myeloma. CRAB-like abnormalities are common with numerous diseases, and these abnormalities must be felt to be directly attributable to the related plasma cell disorder and every attempt made to rule out other underlying causes of anemia, kidney failure, etc.
In 2014, the IMWG updated their criteria further to include biomarkers of malignancy.[64][73] These biomarkers are >60% clonal plasma cells, a serum involved / uninvolved free light chain ratio ≥ 100 (the concentration of the involved free light chain must be ≥ 100 mg/L) and more than one focal lesion ≥ 5 mm by MRI.[64][73] Together, these biomarkers and the CRAB criteria are known as myeloma-defining events (MDEs). A person must have >10 % clonal plasma cells and any MDE to be diagnosed with myeloma.[64] The biomarker criteria were added so that smouldering people with multiple myeloma at high risk of developing multiple myeloma could be diagnosed before organ damage occurred, so they would therefore have a better prognosis.[73]
- Asymptomatic/smoldering myeloma:
- Serum M protein >30 g/L (3 g/dL) or
- Clonal plasma cells >10% on bone marrow biopsy and
- No myeloma-related organ or tissue impairment
- Monoclonal gammopathy of undetermined significance (MGUS):
- Serum paraprotein <30 g/L (3 g/dL) and
- Clonal plasma cells <10% on bone marrow biopsy and
- No myeloma-related organ or tissue impairment or a related B-cell lymphoproliferative disorder
Related conditions include solitary plasmacytoma (a single tumor of plasma cells, typically treated with irradiation), plasma cell dyscrasia (where only the antibodies produce symptoms, e.g., AL amyloidosis), and peripheral neuropathy, organomegaly, endocrinopathy, monoclonal plasma cell disorder, and skin changes.
Staging
In multiple myeloma, staging helps with prognostication but does not guide treatment decisions. The Durie-Salmon staging system was used historically and was replaced by the International Staging System (ISS), published by the
- Stage I: β2 microglobulin (β2M) < 3.5 mg/L, albumin ≥ 3.5 g/dL, normal cytogenetics, no elevated LDH
- Stage II: Not classified under Stage I or Stage III
- Stage III: β2M ≥ 5.5 mg/L and either elevated LDH or high-risk cytogenetics [t(4,14), t(14,16), and/or del(17p)]
Prevention
The risk of multiple myeloma can be reduced slightly by maintaining a normal body weight.[77]
Treatment
Most drug therapies employ multiple agents, e.g., so-called "triplet" or "quadruplet" therapies. Many such groupings include one or more of a monoclonal antibody (e.g., isatuximab or daratumumab), an immunomodulatory agent (e.g., lenalidomide or pomalidomide), and a proteasome inhibitor (e.g., or bortezomib, carfilzomib or ixazomib), in combination with a steroid (e.g., dexamethasone).[78]
While triplet therapies were the standard of care for many years, current practice more commonly applies quadruplets of drugs.[78] Such combination therapies are commonly referenced by initials, employing upper-case letters for drug brandnames and lower-case letters for generic drug names, e.g., VRd for Velcade (brandname for bortezomib), Revlimid (brandname for lenalidomide) and dexamethasone. Similarly with DKRd, with the D representing Darzalex (brandname for daratumumab), and K representing Kyprolis (brandname for carfilzomib).[79] (Emerging practice is not to call such drugs "chemotherapy" because they are not the traditional non-specific intracellular poisons that operate in the classic "chemo" fashion of inhibiting mitosis or inducing DNA damage.[80][81])
Commonly, the efficacy of each drug diminishes over time, as the cancer develops drug resistance mechanisms, such as by clonal evolution or genetic mutations. In part for this reason, multiple myeloma has not historically been treated when in its "smoldering" stage, since the drug(s) utilized may then be of diminished efficacy if the disease progresses to a symptomatic stage. Thus, the standard of care was "watchful waiting" while the disease smoldered.[82] Increasingly, however, efforts are underway to study whether drug therapies applied during the smoldering stage might prevent the disease from ever advancing to the active stage. Exemplary are the GEM-CESAR,[83] ASCENT[84] and Immuno-PRISM[85] clinical trials.
After drug therapy has reduced a patient's cancer burden, some patients undergo a bone marrow transplant (more properly termed a autologous hematopoietic stem cell transplant, or ASCT) to further suppress the disease. However, this procedure is not available for frail patients,[86] as it essentially resets aspects of the immune system and requires redevelopment of natural defenses, such as by administering childhood vaccines.[87]
Increasingly, precision medicine therapies are being explored, with research indicating that certain variants and genetic sub-types of the disease respond more favorably to some drug therapies than others.[88] For example, some research indicates that patients with the t(11,14) genetic translocation (present in about 15-20% of multiple myeloma patients) may particularly benefit from Venetoclax therapy (which is FDA approved for other blood cancers but not yet available for multiple myeloma patients except through clinical trials).[88][89]
While drug therapies commonly entail months or years of treatment, CAR-T therapy offers the alternative of a single treatment (albeit involving a prolonged hospital stay). Moreover, CAR-T treatment seems to provide a deeper, longer lasting disease remission than existing drugs.[90] Presently, however, such therapy is FDA-approved only for patients in later stages of the disease, and is available only at certain medical centers.[91]
An upcoming therapy that also leverages
Some patients seek out clinical drug trials, as these provide a degree of medical oversight not present in most other clinical settings – not to mention access to new drugs that seem to hold promise over existing therapies. Some patients temporarily relocate to urban areas where such trials are available.
The major cancer research institutes offer the most clinical trials, but some trials (particularly later-stage, Phase 3, trials) are available at satellite networks that extend to hundreds of hospitals. The U.S. National Institutes of Health maintains a directory of clinical trials.[94] In the U.S., cities such as New York, Boston, Houston and Rochester host leading multiple myeloma research efforts; globally, other top-tier myeloma research programs are found at the University of Salamanca, Spain, and at Vrije Universiteit Brussels, amongst others.
Medical information soon becomes outdated in fast-moving medical arenas, such as therapies for multiple myeloma, so oncologists at smaller medical centers may not be able to stay up-to-date with the literature in all relevant disciplines. This has given rise to organizations that work to educate patients on latest developments in the disease, e.g., by offering webinars featuring prominent researchers and practitioners who focus on multiple myeloma; examples of such organisations are the International Myeloma Foundation and the Multiple Myeloma Research Foundation. Some patients interested in following latest developments review proceedings from major hematologic cancer conferences, such as the American Society of Hematologists (ASH) Conference,[95] the American Society of Clinical Oncology (ASCO) Conference,[96] the IMF IMWG Summit, and the European Hematology Association (EHA) Annual Conference.[97]
Treatment is indicated in myeloma with symptoms. If there are no symptoms, but a paraprotein typical of myeloma and diagnostic bone marrow is present without end-organ damage, treatment is usually deferred or restricted to clinical trials.[98] Treatment for multiple myeloma is focused on decreasing the clonal plasma cell population and consequently decrease the symptoms of disease.
Chemotherapy
Initial
The preferred treatment for those under the age of 65 is high-dose chemotherapy, commonly with bortezomib-based regimens, and lenalidomide–dexamethasone,[99] to be followed by a stem cell transplant. A 2016 study concluded that stem cell transplant is the preferred treatment of multiple myeloma.[100] There are two types of stem cell transplants to treat multiple myeloma.[101] In autologous hematopoietic stem-cell transplantation (ASCT) – the patient's own stem cells are collected from the patient's own blood. The patient is given high-dose chemotherapy, and the patient's stem cells are then transplanted back into the patient. The process is not curative, but does prolong overall survival and complete remission. In allogeneic stem-cell transplantation, a healthy donor's stem cells are transplanted into the affected person. Allogenic stem-cell transplantation has the potential for a cure, but is used in a very small percentage of people (and in the relapsed setting, not as part of initial treatment).[50] Furthermore, a 5–10% treatment-associated mortality rate is associated with allogeneic stem-cell transplant.
People over age 65 and people with significant concurrent illnesses often cannot tolerate stem-cell transplantation. For these people, the standard of care has been chemotherapy with melphalan and prednisone. Recent studies among this population suggest improved outcomes with new chemotherapy regimens, e.g., with bortezomib.[102][103] Treatment with bortezomib, melphalan, and prednisone had an estimated overall survival of 83% at 30 months, lenalidomide plus low-dose dexamethasone an 82% survival at 2 years, and melphalan, prednisone, and lenalidomide had a 90% survival at 2 years. Head-to-head studies comparing these regimens have not been performed as of 2008[update].[104]
There is support for continuous therapies with multiple drug combinations of antimyeloma drugs bortezomib, lenalidomide, and thalidomide as initial treatment for transplant-ineligible multiple myeloma.[105] Further clinical studies are required to determine the potential harms of these drugs and the effect on the person's quality of life.[105] A 2009 review noted, "Deep venous thrombosis and pulmonary embolism are the major side effects of thalidomide and lenalidomide. Lenalidomide causes more myelosuppression, and thalidomide causes more sedation. Chemotherapy-induced peripheral neuropathy and thrombocytopenia are major side effects of bortezomib."[106] The addition of subcutaneous daratumumab to induction and consolidation therapy with bortezomib, lenalidomide, and dexamethasone, and to lenalidomide maintenance therapy, conferred improved progression-free survival among transplantation-eligible patients with newly diagnosed multiple myeloma.[107]
Treatment of related hyperviscosity syndrome may be required to prevent neurologic symptoms or kidney failure.[108][109]
Maintenance
Most people, including those treated with ASCT, relapse after initial treatment. Maintenance therapy using a prolonged course of low-toxicity medications is often used to prevent relapse. A 2017 meta-analysis showed that post-ASCT maintenance therapy with lenalidomide improved progression-free survival and overall survival in people at standard risk.[110] A 2012 clinical trial showed that people with intermediate- and high-risk disease benefit from a bortezomib-based maintenance regimen.[111]
Relapse
Reasons for relapse include disease evolution, either from the selective pressure applied by treatment or by de novo mutations and/or if disease was inadequately represented in the initial biopsy.[57] Relapse within the first 18 months of diagnosis is considered as functional high-risk multiple myeloma.[57] Depending on the person's condition, the prior treatment modalities used and the duration of remission, options for relapsed disease include retreatment with the original agent, use of other agents (such as melphalan, cyclophosphamide, thalidomide, or dexamethasone, alone or in combination), and a second ASCT.
Later in the course of the disease, it becomes refractory (resistant) to formerly effective treatment. This stage is referred to as relapsed/refractory multiple myeloma (RRMM). Treatment modalities that are commonly use to treat RRMM include dexamethasone,
Kidney failure in multiple myeloma can be
Several newer options are approved for the management of advanced disease:
- belantamab mafodotin: a monoclonal antibody against B-cell maturation antigen (BCMA), also known as CD269, indicated for the treatment of adults with relapsed or refractory multiple myeloma who have received at least four prior therapies including an anti-CD38 monoclonal antibody, a proteasome inhibitor, and an immunomodulatory agent.[113][114]
- carfilzomib: a proteasome inhibitor that is indicated:
- as a single agent in people who have received one or more lines of therapy
- in combination with dexamethasone or with lenalidomide and dexamethasone in people who have received one to three lines of therapy[115]
- daratumumab: a monoclonal antibody against CD38 indicated in people who have received at least three prior lines of therapy including a proteasome inhibitor and an immunomodulatory agent or who are double refractory to a proteasome inhibitor and an immunomodulatory agent[116]
- elotuzumab: an immunostimulatory humanized monoclonal antibody against SLAMF7 (also known as CD319) indicated in combination with lenalidomide and dexamethasone in people who have received one to three prior therapies[117]
- isatuximab: a monoclonal antibody against CD38 indicated in combination with pomalidomide and dexamethasone for the treatment of adults with multiple myeloma who have received at least two prior therapies including lenalidomide and a proteasome inhibitor.[118][119]
- ixazomib: an orally available proteasome inhibitor indicated in combination with lenalidomide and dexamethasone in people who have received at least one prior therapy[120]
- panobinostat: an orally available histone deacetylase inhibitor used in combination with bortezomib and dexamethasone in people who have received at least two prior chemotherapy regimens, including bortezomib and an immunomodulatory agent[121]
- selinexor: an orally available selective inhibitor of nuclear export indicated in combination with dexamethasone in people who have received at least four prior therapies and whose disease does not respond to at least two proteasome inhibitors, two immunomodulatory agents and an anti-CD38 monoclonal antibody[122]
- FDA in 2021 for the treatment of adults with relapsed or refractory multiple myeloma who have received at least four prior therapies[123]
Talquetamab (Talvey) and elranatamab (Elrexfio) were approved for medical use in the United States in August 2023.[124][125][126][127]
Stem cell transplant
Bone marrow transplant
Plerixafor (Mozobil) was approved for medical use in the United States in 2008.[129]
Motixafortide (Aphexda) was approved for medical use in the United States in September 2023.[130]
Gene therapy
- FDA in 2021 for the treatment of adults with relapsed or refractory multiple myeloma who have received at least four prior therapies[123]
- indicated for the treatment of adults with relapsed or refractory multiple myeloma after four or more prior lines of therapy, including a proteasome inhibitor, an immunomodulatory agent, and an anti-CD38 monoclonal antibody.[131]
Other measures
In addition to direct treatment of the plasma cell proliferation,
Side effects
Supportive treatment
Adding physical exercises to the standard treatment for adult patients with haematological malignancies like multiple myeloma may result in little to no difference in the mortality, in the quality of life and in the physical functioning.[134] These exercises may result in a slight reduction in depression.[134] Furthermore, aerobic physical exercises probably reduce fatigue. The evidence is very uncertain about the effect and serious adverse events [134]
Palliative care
Multiple national cancer treatment guidelines recommend early palliative care for people with advanced multiple myeloma at the time of diagnosis and for anyone who has significant symptoms.[135][136]
Palliative care is appropriate at any stage of multiple myeloma and can be provided alongside curative treatment. In addition to addressing symptoms of cancer, palliative care helps manage unwanted side effects, such as pain and nausea related to treatments.[137][138]
Teeth
Oral prophylaxis, hygiene instruction and elimination of sources of infection within the mouth before beginning cancer treatment, can reduce the risk of infectious complications. Before starting bisphosphonates therapy, the person's dental health should be evaluated to assess the risk factors to prevent the development of
Prognosis
Overall the 5-year survival rate is around 54% in the United States.[140] With high-dose therapy followed by ASCT, the median survival has been estimated in 2003 to be about 4.5 years, compared to a median around 3.5 years with "standard" therapy.[141]
The international staging system can help to predict survival, with a median survival (in 2005) of 62 months for stage-1 disease, 45 months for stage-2 disease, and 29 months for stage-3 disease.[74] The median age at diagnosis is 69 years.[140]
Genetic testing
The following table outlines the prognostic effect of various genetic findings in multiple myeloma, with chromosomal translocations designated t, followed by standard nomenclature thereof:[143]
| Genetic abnormality | Gene(s) | Incidence among myelomas | Prognostic impact |
|---|---|---|---|
Deletion/isolated monosomy 13
|
RB1, DIS3 | 45–50% | Effect on prognosis is unclear |
Trisomies
|
40–50% | Median overall survival: 7–10 years | |
| 1q21 gain, as an addition to another abnormality | CKS1B, ANP32E | 35–40% | Median overall survival: 5 years |
| t(11;14)(q13;q32) | IgH and CCND1 | 15–20% | Median overall survival: 7–10 years |
| Trisomies plus any one IgH translocation | 15% | May neutralize high risk IgH and del 17p translocations | |
| Hypodiploidy | 13–20% | Unfavorable prognosis, high risk of progression | |
| t(4:14)(p16;q32) | IgH and FGFR3/MMSET | 10–15% | Median overall survival: 5 years |
| 17p deletion, as an addition to another abnormality | TP53 | 10% | Median overall survival: 5 years |
| t(14;16) | IgH and C-MAF | 2–5% | Median overall survival: 5 years |
| t(6;14)(p21;q32) | IgH and CCND3 | 2% | Median overall survival: 7–10 years |
| t(14;20)(q32;q12) | MAFB | 1% | Median overall survival: 5 years |
Epidemiology

Globally, multiple myeloma affected 488,000 people and resulted in 101,100 deaths in 2015.[8][9] This is up from 49,000 in 1990.[145]
United States
In the United States in 2016, an estimated 30,330 new cases and 12,650 deaths were reported.[7] These numbers are based on assumptions made using data from 2011, which estimated the number of people affected as 83,367 people, the number of new cases as 6.1 per 100,000 people per year, and the mortality as 3.4 per 100,000 people per year.
Multiple myeloma is the second-most prevalent blood cancer (10%) after
Multiple myeloma affects slightly more men than women. African Americans and native Pacific Islanders have the highest reported number of new cases of this disease in the United States and Asians the lowest. Results of one study found the number of new cases of myeloma to be 9.5 cases per 100,000 African Americans and 4.1 cases per 100,000 Caucasian Americans.[147] Among African Americans, myeloma is one of the top-10 causes of cancer death.[148]
UK
Myeloma is the 17th-most common cancer in the UK: around 4,800 people were diagnosed with the disease in 2011. It is the 16th-most common cause of cancer death: around 2,700 people died of it in 2012.[149]
Other animals
Multiple myeloma has been diagnosed in dogs,[150] cats, and horses.[151]
In dogs, multiple myeloma accounts for around 8% of all haemopoietic tumors. Multiple myeloma occurs in older dogs and is not particularly associated with either males or females. No breeds appear overrepresented in case reviews that have been conducted.
See also
- Development of analogs of thalidomide
References
- ^ "Myeloma Canada | What is Multiple Myeloma?". www.myelomacanada.ca. Archived from the original on 13 May 2020. Retrieved 17 April 2020.
- ^ OCLC 1080368315.
- ^ a b c d e f g h "Plasma Cell Neoplasms (Including Multiple Myeloma) Treatment (PDQ®)–Health Professional Version". NCI. 29 July 2016. Archived from the original on 4 July 2016. Retrieved 8 August 2016.
- ^ ISBN 978-92-832-0429-9.
- ^ ISBN 978-92-832-0429-9.
- ^ S2CID 12906881.
- ^ a b c "SEER Stat Fact Sheets: Myeloma". NCI Surveillance, Epidemiology, and End Results Program. Archived from the original on 27 July 2016. Retrieved 8 August 2016.
- ^ PMID 27733282.
- ^ PMID 27733281.
- ^ a b c d e "Plasma Cell Neoplasms (Including Multiple Myeloma)—Patient Version". NCI. 1 January 1980. Archived from the original on 27 July 2016. Retrieved 8 August 2016.
- ^ "Plasma Cell Neoplasms (Including Multiple Myeloma) Treatment". National Cancer Institute. 1 January 1980. Archived from the original on 9 January 2021. Retrieved 28 November 2017.
- ISBN 978-0-323-08431-4. Archivedfrom the original on 18 August 2023. Retrieved 23 August 2020.
- ^ PMID 34575290.
- ^ PMID 30121582.
- PMID 27161311.
- ^ "Multiple Myeloma: Statistics". ASCO Cancer.net. March 2023. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ^ a b "Cancer Stat Facts: Myeloma". National Cancer Institute. Archived from the original on 7 May 2020. Retrieved 10 June 2023.
- ^ "Survival Rates for Multiple Myeloma". American Cancer Society. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ISBN 978-1-60831-464-5. Archivedfrom the original on 21 August 2016.
- ^ S2CID 3195084.
- ^ a b "International Myeloma Working Group (IMWG) criteria for the diagnosis of multiple myeloma". International Myeloma Foundation. 26 October 2014. Archived from the original on 7 December 2022. Retrieved 11 June 2023.
- ISBN 978-0-07-174889-6.
- ^ "Hypercalcemia". The Lecturio Medical Concept Library. Archived from the original on 25 July 2021. Retrieved 11 August 2021.
- PMID 22517906.
- PMID 9759684.
- S2CID 2861880.
- ^ PMID 23302715.
- PMID 27866585.
- ^ PMID 25344526.
- PMID 8033429.
- ^ a b "Common Terminology Criteria for Adverse Events (CTCAE), Version 5.0" (PDF). U.S. Dept. of Health and Human Services. 27 November 2017. Archived (PDF) from the original on 19 May 2023. Retrieved 12 June 2023.
- ^ a b Lancman G (15 November 2022). "Infections and Severe Hypogammaglobulinemia in Multiple Myeloma Patients Treated with Anti-BCMA Bispecific Antibodies". Archived from the original on 11 June 2023. Retrieved 11 June 2023.
- ^ a b "Diagnosis of multiple myeloma". Canadian Cancer Society. Archived from the original on 11 June 2023. Retrieved 11 June 2023.
- PMID 7730490.
- ^ "Rudhiram Hematology Clinic—Google Search". www.google.com. Archived from the original on 1 April 2023. Retrieved 4 February 2022.
- OCLC 888026338.
- PMID 22190790.
- PMID 19179464.
- ^ PMID 28466550.
- ^ PMID 28479151.
- PMID 19824817.
- ^ PMID 23926460.
- PMID 27330041.
- PMID 26294217.
- PMID 25973110.
- ^ S2CID 47010934.
- ^ PMID 28325354.
- PMID 29518976.
- ISBN 978-3-8055-6460-1. Archivedfrom the original on 27 May 2016.
- ^ PMID 15509819.
- S2CID 22325904.
- S2CID 41876106.
- PMID 25644835.
- PMID 20634887.
- PMID 26755663.
- S2CID 24588617.
- ^ PMID 33285523.
- from the original on 18 July 2020. Retrieved 13 July 2019.
- ^ PMID 23288300.
- PMID 26263974.
- PMID 24282993. Archived from the originalon 12 January 2018.
- ISBN 978-1-4160-2973-1.
- PMID 16304401.
- ^ S2CID 36384542.
- ^ "Robbins & Cotran Pathologic Basis of Disease – 9781455726134 | US Elsevier Health Bookshop". www.us.elsevierhealth.com. Archived from the original on 27 April 2021. Retrieved 26 October 2016.
- ISBN 978-1-4557-2683-7. Archivedfrom the original on 10 September 2017.
- PMID 24385542.
- ^ "Mayo Stratification for Myeloma And Risk-adapted Therapy". nebula.wsimg.com. Archived from the original on 28 August 2021. Retrieved 29 September 2017.
- PMID 27002115.
- PMID 14990813.
- PMID 29018236.
- PMID 18971951.
- ^ a b c "International Myeloma Working Group (IMWG) Criteria for the Diagnosis of Multiple Myeloma". International Myeloma Working Group. 29 October 2015. Archived from the original on 7 November 2017. Retrieved 5 August 2018.
- ^ PMID 15809451.
- PMID 26240224.
- ISBN 978-0-9789212-4-8.
- PMID 27557308.
- ^ from the original on 11 June 2023. Retrieved 10 June 2023.
- PMID 31990580.
- ^ "Drug Therapy for Multiple Myeloma". American Cancer Society. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ^ "What Is DARZALEX®?". 9 April 2021. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ^ "Watchful waiting for multiple myeloma". Canadian Cancer Society. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ^ "Triplet and Quadruplet Regimens in Smoldering Multiple Myeloma". 10 March 2023. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ^ "Aggressive Smoldering Curative Approach Evaluating Novel Therapies and Transplant (ASCENT)". Archived from the original on 3 June 2023. Retrieved 3 June 2023.
- ^ a b "Immuno-PRISM (PRecision Intervention Smoldering Myeloma)". Archived from the original on 3 June 2023. Retrieved 3 June 2023.
- ^ "Getting a Stem Cell or Bone Marrow Transplant". American Cancer Society. Archived from the original on 10 June 2023. Retrieved 10 June 2023.
- PMID 31005140.
- ^ PMID 35127532.
- from the original on 18 August 2023. Retrieved 3 June 2023.
- ^ "FDA Approves BCMA-Targeted CAR T-Cell Therapy for Multiple Myeloma". National Cancer Institute. 14 April 2021. Archived from the original on 11 June 2023. Retrieved 10 June 2023.
- ^ "Carvykti Approval Marks Second CAR T-Cell Therapy for Multiple Myeloma". National Cancer Institute. 30 March 2022. Archived from the original on 10 June 2023. Retrieved 10 June 2023.
- ^ "FDA approves teclistamab-cqyv for relapsed or refractory multiple myeloma". U.S. Food and Drug Administration. 25 October 2022. Archived from the original on 27 October 2022. Retrieved 10 June 2023.
- S2CID 254560960.
- ^ "Clinical Trials". Archived from the original on 18 December 2020. Retrieved 3 June 2023.
- ^ "American Society of Hematology". Archived from the original on 3 June 2023. Retrieved 3 June 2023.
- ^ "American Society of Clinical Oncology". Archived from the original on 23 August 2020. Retrieved 3 June 2023.
- ^ "European Hematology Association". Archived from the original on 3 June 2023. Retrieved 3 June 2023.
- PMID 21441462.
- PMID 18332230.
- S2CID 78285186.
- ^ "Stem Cell Transplant for Multiple Myeloma". www.cancer.org. Archived from the original on 13 October 2019. Retrieved 13 October 2019.
- PMID 18753647.
- PMID 19441872.
- PMID 18753654.
- ^ PMID 31765002.
- .
- S2CID 266217426.
- PMID 2183734.
- PMID 7139441.
- PMID 28742454.
- from the original on 18 August 2023. Retrieved 23 December 2022.
- PMID 31187526.
- ^ "FDA granted accelerated approval to belantamab mafodotin-blmf for multiple myeloma". U.S. Food and Drug Administration (FDA). 5 August 2020. Archived from the original on 6 August 2020. Retrieved 6 August 2020.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "FDA Approves GSK's BLENREP (belantamab mafodotin-blmf) for the Treatment of Patients with Relapsed or Refractory Multiple Myeloma" (Press release). GlaxoSmithKline. 6 August 2020. Retrieved 6 August 2020 – via Business Wire.
- ^ "Kyprolis (carfilzomib) for Injection, for Intravenous Use. Full Prescribing Information" (PDF). Thousand Oaks, CA: Onyx Pharmaceuticals. Archived from the original (PDF) on 23 October 2016. Retrieved 20 August 2016.
- ^ "Darzalex (daratumumab) Injection, for Intravenous Use. Full Prescribing Information" (PDF). Horsham, PA: Janssen Biotech. Archived from the original (PDF) on 18 August 2016. Retrieved 18 August 2016.
- ^ "Empliciti (elotuzumab) for Injection, for Intravenous Use. Full Prescribing Information" (PDF). Princeton, NJ: Bristol-Myers Squibb Company. Archived from the original (PDF) on 8 December 2015. Retrieved 18 August 2016.
- ^ "FDA approves isatuximab-irfc for multiple myeloma". U.S. Food and Drug Administration (FDA). 2 March 2020. Archived from the original on 5 March 2020. Retrieved 2 March 2020.
- PMID 31779273.
- ^ "Ninlaro (ixazomib) Capsules, for Oral Use. Full Prescribing Information" (PDF). Millennium Pharmaceuticals, Inc. Archived from the original (PDF) on 19 August 2016. Retrieved 18 August 2016.
- ^ "Farydak (panobinostat) Capsules, for Oral Use. Full Prescribing Information" (PDF). East Hanover, New Jersey: Novartis Pharmaceuticals Corporation. Archived from the original (PDF) on 22 October 2016. Retrieved 18 August 2016.
- ^ "Xpovio (selinexor) Tablets, for Oral Use. Full Prescribing Information" (PDF). Newton, MA: Karyopharm Therapeutics. Archived from the original (PDF) on 3 August 2019. Retrieved 3 August 2019.
- ^ FDA. 27 March 2021.
- ^ "FDA grants accelerated approval to talquetamab-tgvs for relapsed or refractory multiple myeloma". U.S. Food and Drug Administration (FDA). 9 August 2023. Archived from the original on 11 August 2023. Retrieved 10 August 2023.
- ^ "U.S. FDA Approves Talvey (talquetamab-tgvs), a First-in-Class Bispecific Therapy for the Treatment of Patients with Heavily Pretreated Multiple Myeloma" (Press release). Janssen. 10 August 2023. Retrieved 17 August 2023 – via PR Newswire.
- ^ "FDA grants accelerated approval to elranatamab-bcmm for multiple myeloma". U.S. Food and Drug Administration (FDA) (Press release). 14 August 2023. Retrieved 14 August 2023.
- ^ "Pfizer's Elrexfio Receives U.S. FDA Accelerated Approval for Relapsed or Refractory Multiple Myeloma" (Press release). Pfizer. 14 August 2023. Retrieved 17 August 2023 – via Business Wire.
- ^ PMID 30697701.
- ^ "Mozobil- plerixafor injection, solution". DailyMed. 26 June 2023. Retrieved 13 September 2023.
- ^ "BioLineRx Announces FDA Approval of Aphexda (motixafortide) in Combination with Filgrastim (G-CSF) to Mobilize Hematopoietic Stem Cells for Collection and Subsequent Autologous Transplantation in Patients with Multiple Myeloma" (Press release). BioLineRx Ltd. 11 September 2023. Retrieved 13 September 2023 – via PR Newswire.
- ^ a b "FDA approves ciltacabtagene autoleucel for relapsed or refractory multiple myeloma". U.S. Food and Drug Administration (FDA). 7 March 2022. Archived from the original on 17 March 2022. Retrieved 16 March 2022.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- PMID 22592695.
- PMID 26576687.
- ^ PMID 30702150.
- ABIM Foundation, American Society of Clinical Oncology, archived from the original(PDF) on 31 July 2012, retrieved 14 August 2012
- ^ Snowden JA, Ahmedzai S, Ashcroft J, et al. (2010). "Guidelines for Supportive Care in Myeloma" (PDF). British Committee for Standards in Haematology. Archived from the original (PDF) on 23 September 2015. Retrieved 21 August 2014.
- S2CID 39881122.
- PMID 18195339.
- PMID 32166015.
- ^ a b "Myeloma—Cancer Stat Facts". SEER. Archived from the original on 7 May 2020. Retrieved 17 April 2020.
- S2CID 41048909.
- PMID 19687334.
- PMID 32166015.
- ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 11 November 2009. Retrieved 11 November 2009.
- PMID 25530442.)
{{cite journal}}:|author1=has generic name (help)CS1 maint: numeric names: authors list (link - PMID 16361127.
- S2CID 41616510.
- PMID 32166015.
- ^ "Myeloma statistics". Cancer Research UK. Archived from the original on 28 October 2014. Retrieved 28 October 2014.
- ISBN 978-0-7216-7257-1.
- PMID 3654300.
- ^ PMID 3721983.
- PMID 403649.
External links
- Multiple myeloma at Curlie