Mycosis fungoides
| Mycosis fungoides | |
|---|---|
| Other names | Alibert-Bazin syndrome |
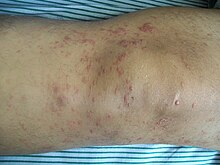 | |
| Skin lesions on the knee of a 52-year-old male patient with mycosis fungoides | |
| Specialty | Dermatology, Hematology, Oncology |
Mycosis fungoides, also known as Alibert-Bazin syndrome or granuloma fungoides,[1] is the most common form of cutaneous T-cell lymphoma. It generally affects the skin, but may progress internally over time. Symptoms include rash, tumors, skin lesions, and itchy skin.
While the cause remains unclear, most cases are not hereditary. Most cases are in people over 20 years of age, and it is more common in men than women. Treatment options include sunlight exposure,
History
Mycosis fungoides was first described in 1806 by French dermatologist
Signs and symptoms


The symptoms of mycosis fungoides are categorized into three clinical stages: the patch stage, the plaque stage, and the tumour stage.[5] The patch stage is defined by flat, reddish patches of varying sizes that may have a wrinkled appearance. They can also look yellowish in people with darker skin.[5] The plaque stage follows the patch stage of mycosis fungoides.[6] It is characterized by the presence of raised lesions that appear reddish-brown; in darker skin tones, plaques may have a greyish or silver appearance.[7] Both patch and plaque stages are considered early-stage mycosis fungoides.[6] The tumour stage typically shows large irregular lumps. Tumours can develop from plaques or normal skin in any region of the body, including the face and head regions.[8]
The symptoms displayed are progressive, with early stages consisting of lesions presented as scaly patches. Lesions often initially develop on the trunk of the body in places that are rarely exposed to the sun, such as the buttocks.[5] These lesions can start as insignificant patches and may remain undiagnosed for up to a decade.[9] Hypopigmentation (when the skin is lighter than normal) of lesions are less common but can be found in children, adolescents and/or dark-skinned individuals.[10]
The advanced stage of mycosis fungoides is characterized by generalized
Mycosis fungoides (MF) and
Cause
Mycosis fungoides is caused by abnormal white blood cells (
Additionally, the disease is an unusual expression of
Diagnosis
Diagnosis often requires a combination of clinical and pathological studies. Diagnosis is sometimes difficult because the early phases of the disease often resemble inflammatory dermatoses (such as
Histology

The criteria for the disease are established on the skin biopsy by the presence of the following:[18]
- Presence of cancer cells with twisted contours (cerebriform nuclei)
- In the patch and plaque stages, the cancer cells are seen in the epidermis (the most superficial layer of skin).[19] This is referred to as epidermotropism.
- Pautrier's microabcesses, aggregates of four or more atypical lymphocytes arranged in the epidermis. Pautrier microabcesses are characteristic of mycosis fungoides but are generally absent.
- In the tumour stage, the cancer cells move into the dermis (the deeper layer of skin)[19]
- Large cell transformation, where clonally identical lymphocytes in the lesion exhibit hypertrophy. In transformed cells, presence of the CD30 receptor is associated with improved survival[20]
To
Peripheral smear will often show
Staging
Traditionally, mycosis fungoides has been divided into three stages: premycotic, mycotic and tumorous. The premycotic stage clinically presents as an erythematous (red), itchy, scaly lesion. Microscopic appearance is non-diagnostic and represented by chronic nonspecific dermatosis associated with psoriasiform changes in epidermis.[medical citation needed]
In the mycotic stage, infiltrative plaques appear and biopsy shows a polymorphous inflammatory infiltrate in the dermis that contains small numbers of frankly atypical lymphoid cells. These cells may line up individually along the epidermal basal layer. The latter finding if unaccompanied by spongiosis is highly suggestive of mycosis fungoides. In the tumorous stage a dense infiltrate of medium-sized lymphocytes with
Accurate staging of mycosis fungoides is essential to determine appropriate treatment and prognosis.[22] Staging is based on the tumor, node, metastasis, blood (TNMB) classification proposed by the Mycosis Fungoides Cooperative Group and revised by the International Society for Cutaneous Lymphomas/European Organization of Research and Treatment of Cancer.[22] This staging system examines the extent of skin involvement (T), presence of lymph node (N), visceral disease (M), and presence of Sezary cells in the peripheral blood (B).[22]
Most patients with mycosis fungoides have early-stage disease (Stage IA-IIA) at the time of their initial diagnosis.[22] People with early stage disease that is primarily confined to the skin have a favorable prognosis.[22] People with advanced stage (Stage IIB-IVB) are often refractory to treatment and have an unfavorable prognosis.[22] Treatment options for people with advanced stage disease are designed to reduce tumor burden, delay disease progression, and preserve quality of life.[22]
Treatment
The most commonly recommended first-line treatment for mycosis fungoides is psoralen plus ultraviolet A (PUVA therapy).[8] PUVA is a photochemotherapy that involves topical or oral administration of the photosensitizing drug psoralen followed by skin exposure to ultraviolet radiation.[23] Systemic treatments of mycosis fungoides often lead to resistance; as such, additional treatment options are often necessary in advanced disease.[24]
Other treatments have been suggested, however, larger and more extensive research is needed to identify effective treatment strategies for this disease.
There is no evidence to support the use of acitretin or
Children
Treatment for adults and children with mycosis fungoides often differs because of the safety profiles of modalities.
Prognosis
A 1999 US-based study of people with CLL's medical records observed a 5-year relative survival rate of 77%, and a 10-year relative survival rate of 69%.[28] After 11 years, the observed relative survival rate remained around 66%.[28] Poorer survival is correlated with advanced age and black race. Superior survival was observed for married women compared with other gender and marital-status groups.[28] The complete remission rate in children is nearly 30%.[27]
Epidemiology
It is rare for mycosis fungoides to appear before age 20; the average age of onset is between 45 and 55 years of age for people with patch and plaque disease only, but is over 60 for people who present with
Culture and society
Notable cases
In 1995 actor Mr. T was diagnosed with a cutaneous T-cell lymphoma, or mycosis fungoides.[32] Once in remission, he joked about the coincidence: "Can you imagine that? Cancer with my name on it — personalized cancer![33]"
Popular British television actor Paul Eddington died of mycosis fungoides after living with the condition for four decades.[34]
See also
- Cutaneous T-cell lymphoma
- Pagetoid reticulosis
- Premycotic phase
- Sézary's disease
- Secondary cutaneous CD30+ large cell lymphoma
- Angiocentric lymphoma
- List of cutaneous conditions
References
- Who Named It?
- ISBN 978-1-4160-2999-1.
- ^ Alibert JL (1806). Descriptions des maladies de la peau observées a l'Hôpital Saint-Louis, et exposition des meilleures méthodes suivies pour leur traitement (in French). Paris: Barrois l’ainé. p. 286. Archived from the original on 2012-12-12.
- ^ Cerroni, 2007, p.13
- ^ ISSN 1865-5785.
- ^ PMID 31313347.
- ^ PMID 29719014.
- ^ PMID 32632956.
- ^ Shinkai K, Fox LP (2022), Papadakis MA, McPhee SJ, Rabow MW, McQuaid KR (eds.), "Cutaneous T-Cell Lymphoma (Mycosis Fungoides)", Current Medical Diagnosis & Treatment 2022, New York, NY: McGraw-Hill Education, retrieved 2021-11-29
- ^ Ipenburg NA, Aird W (eds.). "Mycosis Fungoides/Sezary Syndrome". DynaMed. Retrieved 2021-11-29.
- S2CID 236637083.
- PMID 32965972, retrieved 2021-11-29
- ^ "Mycosis Fungoides (Including Sézary Syndrome) Treatment (PDQ)–Patient Version - National Cancer Institute". www.cancer.gov. 2021-09-03. Retrieved 2021-11-29.
- S2CID 81927761.
- PMID 27782301.
- S2CID 24447286.
- ^ S2CID 232103411.
- ISBN 978-1451172683.
- ^ PMID 30137856. Retrieved 2021-11-29.
- PMID 33769436.
- ISBN 9780323225021.
- ^ PMID 24438970.
- PMID 29067616.
- ^ PMID 32982179.
- ^ "Elorac, Inc. announces orphan drug designation for novel topical treatment for pruritus in cutaneous T-cell lymphoma (CTCL)". Archived from the original on 2010-12-30. Retrieved 2010-11-30.
- PMID 20465602.
- ^ S2CID 232103411.
- ^ PMID 9921994.
- PMID 32141115.
- PMID 33690948.
- PMID 24005876.
- ^ "Mr. T, T cell lymphoma survivor". YouTube. 2013-05-30. Archived from the original on 2021-12-13.
- ^ "Mr. T - The Ultimate Tough Guy goes Head-to-Head with Cancer". copingmag.com. March 2000. Archived from the original on 2010-01-02.
- Independent.co.uk. 23 October 2011. Archivedfrom the original on 2022-06-18.
Further reading
- Knowles DM (2000). Neoplastic Hematopathology. Lippincott Williams Wilkins. p. 1957. ISBN 978-0-683-30246-2.
- Hwang ST, Janik JE, Jaffe ES, Wilson WH (March 2008). "Mycosis fungoides and Sézary syndrome". Lancet. 371 (9616): 945–957. S2CID 205950255.
- Duvic M, Foss FM (December 2007). "Mycosis fungoides: pathophysiology and emerging therapies". Seminars in Oncology. 34 (6 Suppl 5): S21–S28. PMID 18086343.
- Olsen E, Vonderheid E, Pimpinelli N, Willemze R, Kim Y, Knobler R, et al. (September 2007). "Revisions to the staging and classification of mycosis fungoides and Sezary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the cutaneous lymphoma task force of the European Organization of Research and Treatment of Cancer (EORTC)". Blood. 110 (6): 1713–1722. PMID 17540844.
